Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.11 n.2 Centurion Apr. 2012
CLINICAL ARTICLE
CD White MBChBI; S Dix-Peek MBChBII; AL van Huyssteen MBChBIII; EB Hoffman MBChBIV
IFCS(SA)Orth, MMed Registrar From The Maitland Cottage Paediatric Orthopaedic Hospital and Groote Schuur Hospital, Department of Orthopaedics, University of Cape Town
IIFCS(SA)Orth, MMed Consultant From The Maitland Cottage Paediatric Orthopaedic Hospital and Groote Schuur Hospital, Department of Orthopaedics, University of Cape Town
IIIFCS(SA)Orth Orthopaedic surgeon in private practice, Panorama Medi-Clinic Cape Town
IVFCS(SA)Orth Associate Professor From The Maitland Cottage Paediatric Orthopaedic Hospital and Groote Schuur Hospital, Department of Orthopaedics, University of Cape Town
ABSTRACT
BACKGROUND: Late-onset Blount's disease is subdivided by age at onset into juvenile (4-10 years) and adolescent (≥ llyears). Recent literature recommends the use of external fixation with gradual correction of tibial varus and simultaneous correction of associated femoral varus.
METHODS: We retrospectively reviewed 36 patients (43 knees) treated from 1990-2005. Of the 36 patients, 22 were female and 61.1% were obese. Seventeen knees were in juvenile and 26 in adolescent patients. Pre-operatively and at follow-up patients were assessed clinically and radiographically. Pre-operative mechanical axis ranged from 8-55° varus. Seventeen of the 43 knees (39.5%) had femoral varus (lateral distal femoral angle >90°, range 94°-102°). Surgery involved a tibial barrel-vault osteotomy, acutely correcting the overall mechanical axis, internal tibial torsion and procurvatum. Fixation was with Steinmann pins and plaster.
RESULTS: At a mean follow-up of 4 years (38 knees to maturity), 33 knees (76.7%) had a good result. In three juvenile knees the varus recurred after initial correction to 0-4° valgus. Joint line obliquity ranged from 4°-12°.
CONCLUSION: Tibial osteotomy alone with limited internal fixation can achieve good results in late-onset Blount's. In juvenile knees overcorrection to 5-10° mechanical valgus accommodates recurrence secondary to persistent growth inhibition.
Key words: Late-onset Blount's, limited internal fixation
Introduction
Proximal tibia vara in childhood is due to growth disturbance of the proximal medial tibial physis. The condition was critically analysed by WP Blount1 in 1937 who was the first to sub-classify the condition into two broad groups: an infantile form with onset of bowing in infancy which was later sub-classified by Langenskiöld,2 and an adolescent form with onset between 6 and 12 years.
This late-onset form of the disease was later sub-classified by Thompson et al3 into a juvenile form with onset at 4-10 years and an adolescent form with an onset at or after 11 years of age. Both differed from the infantile form in radiological appearance. In late-onset Blount's the physis was irregular; there was less medial epiphyseal wedging; and minimal increased prominence or 'beaking' of the proximal medial tibial metaphysis. The juvenile group was categorised as a separate entity due to the high rate of recurrence of the varus deformity following surgical correction.
Late-onset Blount's disease classically occurs in obese patients with characteristically wide thighs, with a male:female ratio of 4:1 and over 90% of patients obese and black.3-11 There is a well-documented association with slipped upper femoral epiphysis (SUFE).4,12,13
Late-onset Blount's disease has been noted to have an association with concomitant distal femoral varus with a reported incidence of 19%-60%.10,13-18 It is postulated that the medial femoral physis also suffers growth inhibition due to the high loads through the medial knee joint particularly in older obese patients with a 'fat thigh gait'.10,17-20
The treatment of late-onset tibia vara has evolved over time, although the mainstay remains high tibial osteotomy as it was when Blount published his review in 1937.1 Methods of fixation of the osteotomy however have changed, from plaster alone1 to include limited internal fixation with Steinmann pins5,14,21 or stable internal fixation with compression plates.22 Due to the difficulties associated with obesity in late-onset Blount's disease, external fixators have become a popular fixation method, including monolateral8,23 and circular fixators.7,9,24,25 The deformity correction using external fixation can be done either acutely or gradually. Gradual correction with a circular fixator has become increasingly popular and authors report that a more accurate correction is achieved than with acute correction.24,25 Lateral tibial hemi-epiphyseal stapling has also been used but does not address the associated internal rotation or procurvatum deformities.26,27,28
Recently authors have recommended simultaneous correction of distal femoral varus if >5° outside the reference range. This is achieved by simultaneous distal femoral valgus osteotomy (held with a blade plate or external fixator) or lateral distal femoral hemi-epiphyseal stapling.16,23 This is done to prevent knee joint line obliquity which occurs when both the tibial and femoral mechanical varus are corrected by tibial osteotomy alone.29 In some advanced cases distal tibial valgus also occurs.7,16
The authors recommend that this deformity be simultaneously corrected by hemi-epiphyseal stapling or distal tibial osteotomy which is held with an extension of the tibial circular external fixator.
We have treated all patients with late-onset Blount's between 1990 and 2005 with acute correction by means of a high tibial barrel vault osteotomy alone held with Steinmann pins and plaster. We did not correct concomitant femoral varus, but corrected the overall mechanical varus by overcorrecting the tibia.
Materials and methods
We retrospectively reviewed 36 patients (43 knees) treated for late-onset Blount's disease from 1990-2005. Of the 36 patients, 31 (86%) were black and 22 were female (M:F ratio 2:3). Of the 36 patients 15 (17 knees) were juvenile (4-10 years old at presentation) and 19 (26 knees) were adolescent (11 years or older). Twenty-two patients (61.1%) were obese (weight for age >95th percentile). Eight of the15 juvenile patients (53.3%) were obese and 14 (73.6%) of the adolescent patients were obese.
All patients were assessed clinically at presentation and at final follow-up. Presenting symptoms were bowing with or without pain (Figure 1a). Twenty-two (61.1%) of the 36 patients had some form of bilateral genu varum: seven patients had bilateral late-onset Blount's disease, seven patients had contralateral late presenting infantile Blount's and a further eight patients had contralateral genu varum <5° which did not warrant corrective osteotomy. All patients had intoeing due to internal tibial torsion (Figure 1b). The mean thigh-foot angle was 10° internal rotation (range 0°-25°). All patients were Siffert-Katz negative (no increased deformity demonstrated with varus stress in 20° flexion as is found in late presenting infantile Blount's).30
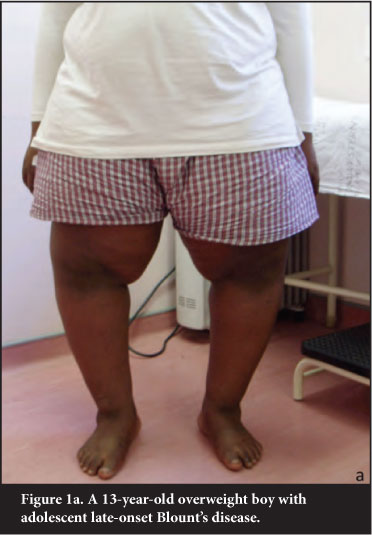
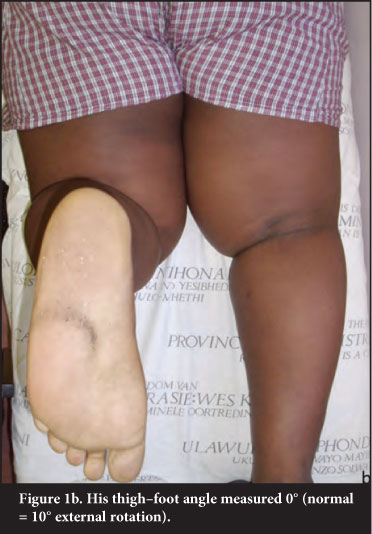
Ten patients had associated pathologies: seven contralateral late presenting infantile Blount's, two peroneal spastic flat feet and one SUFE.
Radiographs taken pre-operatively and at final follow-up included a mechanical axis antero-posterior (AP) standing radiograph with the patella pointing forward and a lateral radiograph of the tibia. These were measured using the methods of Paley and Tetsworth.29 On the AP mechanical axis (MA), lateral distal femoral angle (LDFA normal = 87°, range of 85°-90°), medial proximal tibial angle (MPTA normal = 87°, range 85°-90) and lateral distal tibial angle (LDTA normal = 89°, range 86°-92°) were measured. On the lateral the posterior proximal tibial angle (PPTA normal = 81°, range 77°-84°) quantified the procurvatum. Post-operatively mechanical axis AP views and lateral tibial views were taken. At removal of the plaster AP and lateral tibial views were done to confirm union.
Pre-operative mechanical varus ranged from 8° to 55°. All patients had tibial varus.
Femoral varus was defined as an LDTA >90°. Distal femoral varus occurred in 17 (39.5%) of the 43 knees. Femoral varus ranged from 4° (LDFA 94°) to 12° (LDTA 102°). This quantifies the potential joint line obliquity in these knees as the mechanical varus was corrected with a tibial osteotomy only.
Of the knees with distal femoral varus 88% were in obese patients, compared to 42% obesity in those patients who did not have femoral varus. Distal femoral varus occurred in 50% of adolescent knees and in 23.5% of juvenile knees.
There was no pre-operative ankle valgus in this study.
The surgical technique was the same in all cases. Preoperatively the centre of the femoral head is determined with fluoroscopy and marked with an ECG electrode. Through a mid-fibular incision a lateral compartment fasciotomy and an oblique osteotomy of the fibula was done. Through a second incision below the tibial apoph-ysis and after anterior compartment fasciotomy, a low energy tibial barrel vault osteotomy was performed just below the apophysis. To achieve a comfortable correction 1 cm of shortening was done. Through this osteotomy the mechanical axis of the limb was corrected to 0°-5° valgus in adolescents and 5°-10° in juveniles.
This was done with intra-operative fluoroscopy using the electrocautery cord from the centre of the femoral head represented by the ECG electrode. The internal tibial torsion was corrected to 10° external tibial torsion and the procurvatum to a PPTA of 80°. No patient had a distal femoral or distal tibial osteotomy. The corrected barrel vault osteotomy was held with two to three crossed 2.4 mm Steinmann pins and the leg immobilised in an above-knee plaster for 6 weeks. The patients were then weaned of crutches and partial weightbearing over 4 weeks.
There were no cases of compartment syndrome, infection, delayed or non-union or peroneal nerve palsy.
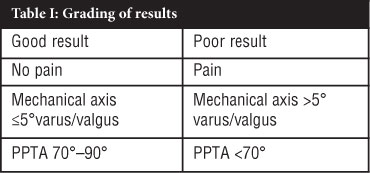
Patients were followed up for 2-8 years (mean 4 years) and 38 of the 43 knees were followed up to physeal closure (either secondary to maturity or epiphysiodesis in the case of the seven patients with contralateral late presenting infantile Blount's). Results were graded clinically and radiologically using a modification of the criteria described by Schoenecker et al.21 A good result had no pain, a mechanical axis ≤5° varus or valgus and a procurvatum deformity <10° (PPTA ≥70°).
Results
Thirty-three (76.7%) knees had a good result (Figure 2) and ten (23.3%) a poor result (Table I).
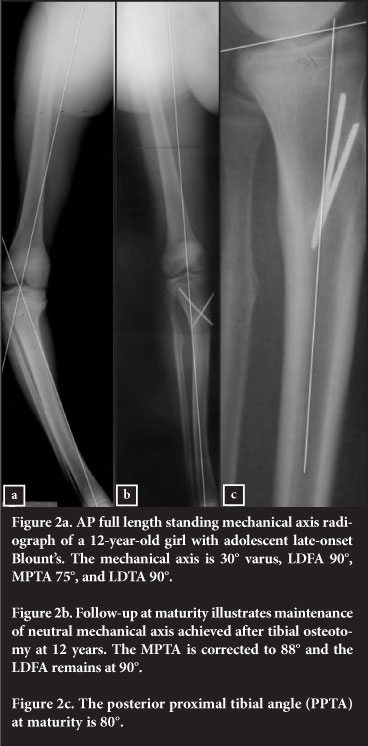
All patients had adequate correction of the internal tibial torsion to thigh foot angles 10° to 15° external rotation. No patient had ankle valgus clinically or radiologically (LDTA 86°-90°). No patient had a leg length discrepancy of >2 cm.
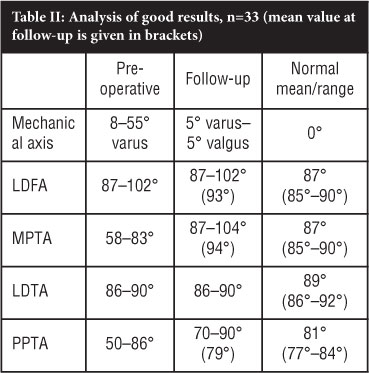
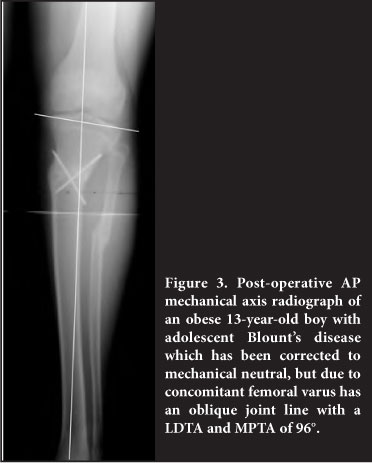
Analysis of the radiological measurements of the 33 knees with good results (Table II) showed that although the overall mechanical varus of 8-55° had been corrected to within 5° of neutral, the average MPTA was 94°, reflecting tibial valgus. This is because both the femoral and tibial contributions to the overall mechanical varus were corrected by a tibial osteotomy alone, and is a reflection of the mean distal femoral varus (LDFA 93°) (Figure 3).
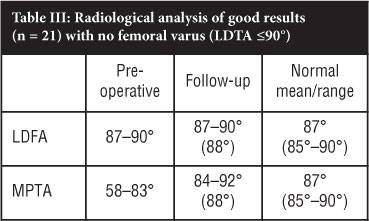
When the 12 knees with femoral varus are excluded, the mean post-operative MPTA is normal at 88° (Table III; Figure 2).
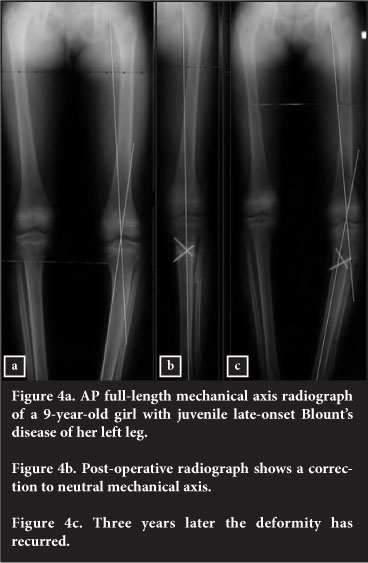
Eight of the ten poor results were attributable to not obtaining accurate deformity correction at surgery. Five knees required re-operation: two knees for over-correction to >10° mechanical valgus and three juvenile knees which were initially only corrected to between 0°-4° valgus and recurred to >5° varus, due to ongoing growth disturbance of the proximal medial tibial physis (Figure 4).
The five knees with poor results who did not have further surgery included four knees with under-correction to between 6° and 10° mechanical varus and one with under-correction of procurvatum (PPTA 60°). These five patients were satisfied with their cosmetic outcome and refused further corrective surgery.
Discussion
The pathology of Blount's disease is due to abnormal endochondral ossification with resultant growth inhibition of the medial proximal tibial physis. This growth plate abnormality manifests histologically as column disorganisation with clefts and fissures.4,12,14
The aetiology however remains unknown and is probably multifactorial.11 Davids et al19 postulated that obese adolescents had a 'fat thigh gait' with resultant difficulty adducting the hip in stance, which together with swing limb circumduction results in increased forces across the medial side of the knee causing physeal growth inhibition.
Demographics
Demographic data from the USA show that 80% are black, 75% male and >90% obese patients.3-11 Although 86% of the patients in our study were black, the male:female ratio was 2:3 and only 61.1% of the patients were obese. The 'fat thigh gait' alone does not explain late-onset Blount's disease in patients of normal weight and in the 39% of patients in our study who did not have any form of bilateral involvement. The theory however, is supported by the distribution of the femoral varus which occurred in 39.5% of the knees in our study. Older or adolescent patients (50% femoral varus) and overweight patients (88% femoral varus) were twice as likely to develop femoral varus when compared to juvenile (25%) or normal weight (42%) patients.
Three orthopaedic conditions that occur in overweight children are Blount's disease, SUFE and idiopathic peroneal spastic flat foot. SUFE has a similar histopathology of the growth plate as Blount's.12 Idiopathic peroneal spastic flat foot which occurred in two patients in this study has not previously been described in Blount's.
Treatment
Over the last 20 years the treatment of late-onset Blount's disease has evolved away from the more traditional high tibial osteotomy alone held with limited internal fixation. This is due to difficulties with managing the very obese patient in plaster and achieving exact correction of the deformity under fluoroscopy. The literature reflects an evolution of the surgical technique towards more complicated techniques such as internal fixation with a plate and external fixation with monolateral and ring fixators.
Acute correction and compression plate fixation was used by Martin et al.22 It was never widely used because it required greater soft tissue stripping and did not allow lateral translation at the osteotomy site. Monolateral external fixation with an Orthofix fixator was described by Gaudinez et al8 and Stanitsky et al.23
It allows for simultaneous lengthening although in our study leg length discrepancy was not a problem. Similarly circular external fixation allowed simultaneous lengthening and weightbearing throughout treatment. Coogan et al and Stanitsky et al described gradual correction with a hinged Ilizarov-type external fixator. The fixator was on for an average of 19 weeks.
More recently the Taylor Spatial Frame (TSF) has allowed correction with a circular fixator and six-axis deformity analysis. Feldman et al21 used the TSF in chronic mode for gradual correction and reported 100% good results. They also published a comparative study where they compared the patients treated with gradual correction in a TSF to a group treated by acute correction. They concluded that the gradual correction was more accurate.25
Advantages of our technique are that it is relatively simple to perform and that the equipment is much cheaper than the external fixator devices. The surgical time is less and bilateral cases can be done at the same sitting. The plaster is removed at 6 weeks, compared to a mean of 19 weeks for gradual correction in an external fixator.
The maximum weight in our study was 114 kg. The study by Gordon et al16 reported a mean weight of 112 kg with a maximum of 178 kg! Since the completion of our study in 2005 the degree and the incidence of severe obesity in mainly adolescent patients has increased significantly. These severely obese patients are difficult to manage in plaster and we are now utilising a monolateral Orthofix fixator. The juvenile patients and the adolescent patients who are not severely obese are managed as described in this study.
Intra-operative assessment of mechanical axis and alignment
All our poor results not due to juvenile recurrence were due to inaccuracy of correction at the time of surgery. Using the electrocautery cord for alignment in an obese patient is a crude instrument at best. Sabharwal et al31 have shown that this method is accurate only in patients with a normal body mass index, <2 cm of mechanical axis deviation and <3° of joint line convergence angle on the standing AP radiograph. Saleh et al32 developed a grid with wires to accurately align the tibial mechanical axis. A longer grid has since been made with a wire from the hip to the ankle but still has to be verified.
Distal femoral varus
Distal femoral varus occurred in 17 (39.5%) of all the knees and in 12 (36.3%) of the good results. The adolescent (50% vs 23.5%) and obese patients (88% vs 42%) were twice as likely to develop femoral varus, lending weight to the theory that increased forces across the medial femoral physis in an overloaded varus knee contribute to this secondary deformity.10,17-20 This is different from late-presenting infantile Blount's. In late-presenting infantile Blount's the more pliable epiphysis of the medial joint line becomes depressed, necessitating an elevating osteotomy while the femur is unaffected.4
Gordon et al16 describe a comprehensive approach to late-onset Blount's disease. They simultaneously corrected the femoral varus by means of lateral distal hemi-epiphyseal stapling (if there was enough growth remaining) or with an osteotomy and blade plate, in order to avoid residual distal joint line obliquity which could possibly lead to degenerative joint disease. They corrected the femoral varus if it exceeded 5° (LDFA >95°).Twelve of the 33 knees with good results in our study had residual joint line obliquity between 4° and 12°, due to residual femoral varus with a LDTA >90° (the upper limit of normal). There are to our knowledge no long-term studies into adulthood to assess whether this amount of joint line obliquity results in significant degeneration. It may well be that in these obese patients who cannot normally adduct in the stance phase, the joint line is parallel to the floor in stance although not perpendicular to the mechanical axis. We currently will correct the femoral varus if it exceeds 10° (LDFA >100°).
Ankle valgus
There was no ankle valgus (LDTA <86°) pre- or post-operatively in our study. Myers et al18 also found no ankle valgus. This is difficult to explain especially in those limbs where the tibia was overcorrected into valgus to correct the tibial and femoral varus. Gordon et al16 in their comprehensive approach corrected ankle valgus with a varus osteotomy or medial distal hemi-epiphyseal stapling if the LDTA was<86°.
Since the completion of this study we follow the osteotomy rule of Paley and Tetsworth29 to lateralise the tibia after the proximal tibial osteotomy. The osteotomy is distal to the centre of the deformity which occurs at the growth plate, and translation of the tibia laterally limits overcorrection into valgus and prevents a 'dog leg' deformity.
Recurrence in juvenile knees
Juvenile recurrence due to ongoing abnormal endochondral ossification is a well-recognised problem with reported rates between 25% and 50%.3,13,14 Our study was no exception. Three (17.6%) of the 17 juvenile knees required re-operation due to recurrence following initial correction to <5° valgus (Figure 4). No juvenile knees that were corrected to between 5° and 10° valgus recurred into varus. We therefore recommend that patients <11 years old at surgery be corrected to 5°-10° valgus to allow for this recurrence.
Limitations of this study are that the follow-up was relatively short and the long-term effects on the knee could not be assessed; five knees were not followed to maturity; and it has the bias of a retrospective study.
Conclusions
Tibial osteotomy alone held with Steinmann pins and plaster is a simple and cheap option and can give good results in the treatment of all juvenile patients and adolescent patients that are not severely obese. In juvenile knees overcorrection to 5°-10° mechanical valgus accommodates recurrence secondary to persistent growth inhibition.
The content of this article is the sole work of the authors. No benefits of any form have been or are to be received from a commercial party related directly or indirectly to the subject of this article. The research has been approved by the Research Ethics Committee, Health Sciences Faculty, University of Cape Town (ref: 349/2008).
References
1. Blount WP. Tibia vara. Osteochondrosis deformans tibiae. J Bone Joint Surg 1937;19:1-29. [ Links ]
2. Langenskiöld A, Riska EB. Tibia vara (osteochondrosis deformans tibiae). A survey of 21 cases. J Bone Joint Surg (Am)1964;46-A:1405-20. [ Links ]
3. Thompson GH, Carter JR, Smith CW. Late-onset tibia vara: A comparative analysis. J Pediatr Orthop 1984;4:185-94. [ Links ]
4. Wenger DR, Mickelson M, Maynard JA. The evolution and histopathology of adolescent tibia vara. J Pediatr Orthop 1984;4:78-88. [ Links ]
5. Loder RT, Schaffer JJ, Bardstein MB. Late-onset tibia vara. J Pediatr Orthop 1991;11:162-67. [ Links ]
6. Henderson RC, Kemp GJ, Greene WB. Adolescent tibia vara: Alternatives for operative treatment. J Bone Joint Surg (Am) 1992:74-A:342-50. [ Links ]
7. Coogan PG, Fox JA, Fitch RD. Treatment of adolescent Blount's disease with the circular external fixation device and distraction osteogenesis. J Pediatr Orthop 1996;16:455-60. [ Links ]
8. Gaudinez R, Adar U. Use of Orthofix T-Garche fixator in late-onset tibia vara. J Pediatr Orthop 1996;16:455-60. [ Links ]
9. Stanitsky DF, Dahl M, Louie K, Grayhack J. Management of late-onset tibia vara in the obese patient by using circular external fixation. J Pediatr Orthop 1997;17:691-94. [ Links ]
10. Sabharwal S, Zhao C, McClemens E. Correlation of boby mass index and radiographic deformities in children with Blount disease. J Bone Joint Surgery (Am) 2007;89-A:1275- 83. [ Links ]
11. Sabharwal S. Current concepts review. Blount disease. J Bone Joint Surg (Am) 2009; 91-A:1758-76. [ Links ]
12. Carter JR, Leeson MC, Thompson GH, Kalamchi A, Kelly CM, Makley JT. Late-onset tibia vara: A histopathological analysis. A comparative evaluation with infantile tibia vara and slipped capital femoral epiphysis. J Pediatr Orthop 1988;8:187-95. [ Links ]
13. Thompson GH, Carter JR. Late-onset tibia vara (Blount's disease). Current Concepts. Clin Orthop 1990;225:24-35. [ Links ]
14. Van Huyssteen AL, Davies JQ, Hastings CJ, Roche SJL, Hoffman EB. Late-onset Blount's disease: an epidemiological, radiological and histological study. J Bone Joint Surg (Br) 2001;83-B (Suppl 1):4. [ Links ]
15. Kline SC, Bostrum M, Griffin PP. Femoral varus: An important component in late-onset Blount's disease. J Pediatr Orthop 1992;12:197-206. [ Links ]
16. Gordon JE, Heidenreich FP, Carpenter CJ, Kelly-Hahn J, Schoenecker PL. Comprehensive treatment of late-onset Blount's. J Bone Joint Surgery (Am) 2005;87-A:1561-70. [ Links ]
17. Gordon JE, King DJ, Luhmann SJ, Dobbs MB, Schoenecker PL. Femoral deformity in tibia vara. J Bone Joint Surg (Am) 2006;88-A:380-86. [ Links ]
18. Myers TG, Fishman MK, McCarthy JJ, Davidson RS, Gaughan J. Incidence of distal femoral and distal tibial deformities in infantile and adolescent Blount's disease. J Pediatr Orthop 2005;25:215-18. [ Links ]
19. Davids JR, Huskamp M, Baglett AM. A dynamic biome-chanical analysis of the etiology of adolescent tibia vara. J Pediatr Orthop 1996;16:461-68. [ Links ]
20. Gushue DL, Houck J, Lerner AL. Effects of childhood obesity on three dimensional knee joint biomechanics during walking. J Pediatr Orthop 2005;25:763-68. [ Links ]
21. Schoenecker PL, Meade WC, Pierron RL, Sheridan JJ, Capelli AM. Blount's disease: A retrospective review and recommendation for treatment. J Pediatr Orthop 1985;5:181-86. [ Links ]
22. Martin SD, Moran MC, Martin TL, Burke SW. Proximal tibial osteotomy with compression plate fixation for tibia vara. J Pediatr Orthop 1994;14:619-22.
23. Stanitsky DF, Srivastava P, Stanitsky CL. Correction of proximal tibial deformities in adolescents with the T-Garches external fixator. J Pediatr Orthop 1998;18:512-17. [ Links ]
24. Feldman DS, Madan SS, Koval KJ, van Bosse HJ, Bazzi J, Lehman WB. Correction of tibia vara with six axis deformity analysis and the Taylor Spatial Frame. J Pediatr Orthop 2003;23:387-91. [ Links ]
25. Feldman DS, Madan SS, Ruchelsman DE, Sala DA, Lehman WB. Accuracy of correction of tibia vara: Acute versus gradual correction. J Pediatr Orthop 2006;26:794-98. [ Links ]
26. Blount WP, Clarke GR. Control of bone growth by epiphyseal stapling. A preliminary report. J Bone Joint Surg (Am)1949;31-A:464-78. [ Links ]
27. Mielke CH, Stevens PM. Hemiepiphyseal stapling for knee deformities in children younger than 10 years: A preliminary report. J Pediatr Orthop 1996;16:423-29. [ Links ]
28. Park SS, Gordon JE, Luhmann SJ, Dodds MB, Schoenecker PL. Outcome of hemiepiphyseal stapling for late-onset tibia vara. J Bone Joint Surg (Am) 2005;87-A:2259-66. [ Links ]
29. Paley D, Tetsworth K. Mechanical axis deviation of the lower limbs. Preoperative planning of uniapical angular deformities of the tibia or femur. Clin Orthop 1992;280:48-64. [ Links ]
30. Siffert RS, Katz JF. The intra-artricular deformity in osteochondrosis deformans tibiae. J Bone Joint Surg (Am) 1970;52-A:800-804. [ Links ]
31. Sabharwal SW, Zhao C. Assessment of lower limb alignment: supine fluoroscopy compared with a standing full length radiograph. J Bone Joint Surg(Am) 2008;90-A:43-51. [ Links ]
32. Saleh M, HarrimanP, EdwardsDJ. A radiological method for producing precise limb alignment. J Bone Joint Surg (Br) 1991;73-B:515-16. [ Links ]
 Reprint requests:
Reprint requests:
EB Hoffman
7 Marne Avenue
Newlands 7700 Cape Town
Tel: +27 21 6742090
Email: teddie@absamail.co.za














