Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.11 no.2 Centurion abr. 2012
CLINICAL ARTICLE
Musculoskeletal burden of disease: do we have any idea?
RN Dunn MBChB(UCT)I; MMed(UCT)OrthII; FCS(SA)OrthIII
IConsultant Spine and Orthopaedic Surgeon. Professor and Head of the Department of Orthopaedics, University of Cape Town
IIHead: Orthopaedic Spinal Services, Groote Schuur Hospital
IIISpine Deformity, Service Red Cross Children's Hospital
ABSTRACT
Planning an orthopaedic surgical service is extremely difficult as we are faced with competing demands. Our teaching hospitals are expected to provide a comprehensive training yet the service is dominated by trauma-related patient care.
In the past, elective orthopaedic surgery was often ring-fenced in separate hospitals but due to many reasons this has changed. All sub-specialities are competing for resources.
Due to political imperatives and the nature of emergency care, trauma and infective pathology dominate the state workload. This creates a self-perpetuating cycle. Initially the emergency work excludes the elective care of the degenerative/congenital and oncological pathologies due to competition for beds and theatre time. There is a change of the staff profile, with those interested and skilled in elective reconstructive procedures drifting into the private sector where they can continue their work. Then, as the managers and doctors only see trauma/infective conditions being serviced, this becomes perceived as the need. The quiet suffering of the functionally impaired arthritis patient is ignored in the face of the emergency work.
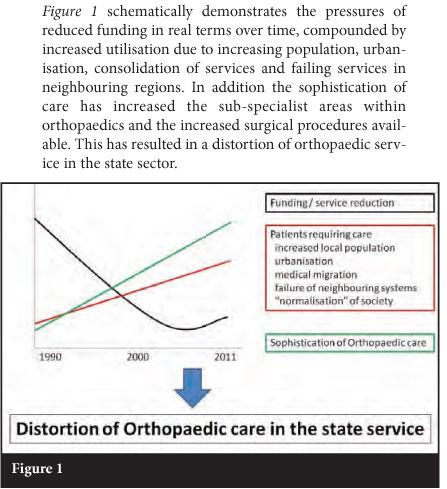
This cycle feeds the misperception and impacts planning. We thus end up with a much skewed orthopaedic service (Figure 2).
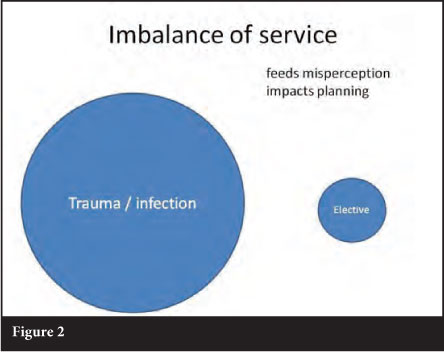
The starting point of any service planning is to understand the burden of disease. Once this is achieved, priorities can be set and resources allocated as seen fit.
Where is the data?
It seems very simple, but finding this data is extremely difficult.
The local MRC Burden of Disease Research unit deals with such data but it is grouped in a manner that hides the pathologies managed in elective orthopaedic surgery. This data is usually grouped into HIV/Aids; Other communicable diseases; Non-communicable diseases; and Injuries. They concentrate on causes of mortality with HIV, violence, road traffic accidents and tuberculosis leading the table. Orthopaedic surgery is involved with many patients falling into these categories but this is not clear from the way the data is usually presented. This data is often used to procure funding for the primary care of these conditions without the realisation of the secondary and tertiary care management involved.1
Not only is the grouping a problem but so is the use of 'mortality' as an outcome measure. Orthopaedic surgery is of course about life not death, and more specifically quality of life.
Unfortunately this perception that infection and trauma are all important comes through in governmental planning. In a Western Cape Provincial treasury working paper in 2010, only two aspects are listed under the burden of disease section, viz. retroviral treatment and TB clinics!2
The WHO web site offers a little more SA data indicating South Africa's relationship to the world's best and worse countries, specifically musculoskeletal diseases and road traffic accidents.
International findings
Due to this paucity of data we are forced to look at the international literature. Vavken reviewed 14 507 European subjects and calculated the prevalence of spine conditions to be greater than 40% in 35-year-olds and older.
The arthritis prevalence was in excess of 20% in greater than 40-year-olds.3
Musculoskeletal pathology is classically under-reported as many simply accept their lot, yet it is one of the most commonly encountered pathologies in general practice.
In a French study of 8 559 patients attending 825 general practitioners, musculoskeletal diseases were the reason for the contact in 29% of cases. This was the commonest cause of consultation, followed by cardiothoracic then psychiatric pathology. In addition, they found that musculoskeletal pathology had the most pronounced effect on physical function. When prevalence and quality of life were combined, musculoskeletal diseases represented the heaviest burden in general practice.4
Geographical differences
Some may think that the incidence of disease may be different between different geographical regions, but this does not appear to be the case. Woolf researched the incidence of knee arthritis by age group, sex and region. Sub-Saharan Africa followed the same incidence when plotted against age as other more developed regions.5
As previously stated, death is not a good measure of musculoskeletal pathology. It is equally poor when measuring the impact of orthopaedic surgical intervention. The increasing use of the Disability Adjusted Life Year (DALY) brings our science to the fore. DALY is an incidence-based measure quantifying the health gap between a population's actual health status and a specified norm. It measures both years lost by premature death as well as years lived with a disability, corrected for the severity of that functional impairment.
Sub-Saharan Africa has a far greater total DALY that the rest of the developing and developed world.1
Impact on surgical service
It is thus quite clear that musculoskeletal pathology is highly prevalent at general practitioner level but how does this impact our surgical service? The numbers of elective procedures we currently perform are based on historical theatre allocations, staffing levels and interest, and available finance for consumables/prosthesis. There is little scientific planning behind resource allocation with historically powerful disciplines/personalities dominating theatre access.
The total hip replacement is synonymous with orthopaedic surgery. I have used Total Hip replacement (THR) for 1° arthritis to make the point. At Groote Schuur Hospital (GSH) around 90 THRs are done per annum for this indication, but what is the need? The problem is we do not know. There are long waiting lists, and presently this is all one can go on. Waiting lists are unreliable indicators, especially when not actively managed.
Lohmander6 looked at the incidence of THR for this specific indication in Scandinavia. Averaging their results for the region, an incidence of 81.5 THRs per 100 000 population can be calculated. Using this incidence in the Western Cape, one can calculate the need based on this incidence.
Assuming a population of 4 500 000 and an 80:20 split between state and private practice, one can calculate that 2 924 THRs should be done in the province per annum. This would be shared between the East and West Metropolitan areas, thus and one would expect GSH and its satellite hospitals to perform 1 462 THR for 1° arthritis per annum.
Clearly one could argue (correctly) that the Western Cape age demographics differ from that of Scandinavia. However one can repeat the calculation to correct for this. Lohmander's6 average THR incidence for 50 to 89-year-olds is 263/100 000. From the Western Cape census (2007) there appears to be in the region of 580 000 people older than 50 years.
Repeating the calculation suggests that GSH (and its two smaller satellite hospitals) should be performing 610 THR for 1° arthritis per annum. This is still seven times more than we are currently doing. In addition this does not take the backlog; other pathologies (inflammatory arthritis/hip fractures); medical tourism from other provinces; and population growth since 2007 into account.
Another basic orthopaedic procedure is knee arthroscopy. In an audit of knee arthroscopy surgery in the United Kingdom National Health system between 2005 and 2010, an incidence of 9.9/10 000 population was calculated.7
With similar assumptions as in the THR exercise, i.e. 4 500 000 Western Cape population, 80:20 state-private split and 50% to be done at GSH, 1 782 knee scopes should be done per annum.
This translates to 34 scopes per week, if all 52 weeks allow elective work (which is unlikely). In the United Kingdom audit, 6% of the cases were ligament reconstruction and 35% meniscal surgery. This would translate to 12 meniscal surgery cases and two ligament reconstruction cases a week at GSH. At present GSH has only one morning soft tissue knee list a week.
Unfortunately other common orthopaedic procedure incident rates were not found in the literature.
However it is quite clear that there is a high burden of musculoskeletal disease in the community. One would thus expect a great need for reconstructive orthopaedic surgery.
By looking at two commonly practised orthopaedic procedures (THR and knee arthroscopy), it is clear that our state service is not satisfying that demand.
We require more local research into the musculoskeletal disease burden of the South African community in an effort to motivate for expansion of our Orthopaedic services and improve care. This research needs to specifically look at disability utilising DALY calculations to identify the burden of orthopaedic-related pathology.
References
1. Bradshaw D, Groenewald P, Laubscher R, Nannan N, Nojilana B, Norman R, Pieterse D, Schneider M. Initial burden of disease estimates for South Africa, 2000. Cape Town: South African Medical Research Council, 2003. [ Links ]
2. Provincial Government Western Cape Provincial Treasury Regional Development Profile: City of Cape Town 2010 Working paper http://www.capegateway.gov.za [ Links ]
3. Vavken P, Dorot R. Burden of musculoskeletal disease and its determination by urbanicity, socioeconomic status, age, and sex: results from 14,507 subjects. Arthritis Care & Research Vol. 63, No. 11, November 2011, pp 1558-64 DOI 10.1002/acr.20558 [ Links ]
4. Grimaldi-Bensouda L, Begaud B, Lert F, et al. Benchmarking the burden of 100 diseases: results of a nationwide representative survey within general practices. BMJ Open 2011;1: e000215. doi:10.1136/bmjopen-2011- 000215 [ Links ]
5. Woolf AD, Pfleger B. Special theme - Bone and Joint Decade 2000-2010 Bulletin of the World Health Organization 2003;81:646-56. [ Links ]
6. Lohmander LS, Engesster LB, Herberts P, Ingvarsson T, Lucht U, Puolakka TJ. Standardized incidence rates of total hip replacement for primary hip osteoarthritis in the 5 Nordic countries: similarities and differences Acta Orthopaedica 2006;77(5):733-40,733. [ Links ]
7. Jameson SS, Dowen D, James P, Serrano-Pedraza D, Reed MR, Deehan DJ. The burden of arthroscopy of the knee: a contemporary analysis of data from the English NHS. J Bone Joint Surg Br. 2011 Oct;93(10):1327-33. [ Links ]
 Reprint requests:
Reprint requests:
Prof Robert Dunn
Email: info@spinesurgery.co.za














