Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.11 n.1 Centurion Jan. 2012
CLINICAL ARTICLE
Greater trochanteric pain syndrome
D Hugo MBChB USI; MPhil(Sports Med)UCTI; HR de Jongh MBChB USII; Dip Anaest CMSAII; MMed(Ortho)USII
IRegistrar, Department of Orthopaedics, Tygerberg Hospital/University of Stellenbosch
IISenior Consultant, Department of Orthopaedics, Tygerberg Hospital/University of Stellenbosch
ABSTRACT
Greater trochanteric pain syndrome is a common, but often misdiagnosed cause of lateral hip pain. Recent advances in the imaging of the hip has improved the understanding of the causative mechanisms of greater trochanteric pain syndrome (GTPS). The syndrome encompasses a wide spectrum of causes including tendinosis, muscle tears, iliotibial band (ITB) disorders and surrounding soft tissue pathology. Clinically GTPS presents with lateral hip tenderness and pain with resisted abduction. A positive Trendelenburg test is the most sensitive predictor of a gluteal tear. Altered lower limb biomechanics is proposed as an important predisposing factor for gluteal muscle pathology. Many conditions are associated with GTPS: some of them may predispose to GTPS, while others may mimic the symptoms. Although plain radiographs are still important for ruling out other causes of hip pain, MRI has become the imaging modality of choice in GTPS. Most cases of GTPS can be regarded as self-limiting. Conservative modalities (rest, NSAIDs, physiotherapy) are still the mainstay of treatment. Corticosteroid injections are still widely used and reported to be successful. Proven gluteal muscle tears are treated with surgical repair and bursectomy. Endoscopic techniques have become increasingly popular.
Key words: trochanteric, bursitis, hip, gluteus medius, tendinopathy
Introduction
Greater trochanteric pain syndrome (GTPS) is a clinical condition that primary care physicians, sports physicians, rheumatologists and orthopaedic surgeons are commonly faced with.1 Yet, it is an often underdiagnosed and misunderstood condition.2 In an attempt to further the understanding of the GTPS, we reviewed the literature by searching via Pubmed/Medline using the terms 'greater trochanteric pain syndrome, 'trochanteric bursitis' and 'lateral hip pain.
GTPS is a regional pain syndrome that is characterised by chronic pain of the lateral hip area, involving the greater trochanter, buttock and lateral thigh.3,4 Clinically it presents with tenderness on palpation of the greater trochanter area with the patient in the side-lying position.2,5 The nature of this syndrome, previously referred to as 'trochanteric bursitis', has classically been poorly understood, as it is often difficult to demonstrate the exact aetiology of the symptoms.2,3,6
Therefore GTPS has become the preferred term for lateral hip pain.3 Recent advances in the imaging of the lateral hip area has improved the understanding of the causative mechanisms of GTPS. The syndrome encompasses a wide spectrum of causes including tendinosis, muscle tears, ITB disorders and surrounding soft tissue pathology.1,3,4,7,8
Classically the cause of lateral hip pain was described as a bursitis. Several orthopaedic text books described trochanteric or subgluteal bursitis.9 'Trochanteric bursitis' was first described in 1923 by Stegemann for symptoms of lateral hip pain.10 In 1958 Leonard suggested the term trochanteric syndrome for pain in the lateral hip region.
He described bursitis, calcareous and non-calcareous tendonitis.11 Gordon suggested in 1961 that gluteal tendinopathy, similar to rotator cuff tendinopathy, could cause fluid accumulation in the bursae.12 Karpinski and Piggott also noted the similarities between GTPS and tendinopathies like tennis and golfer's elbow, policeman's heel and coccydynia.6
'Trochanteric bursitis' is still widely used despite the fact that of the four classic signs of inflammation, only pain was present.3,5
GTPS has been described as a 'great mimicker' and can mimic pain from other causes like osteoarthritis (hip), spinal pathology (L4/5 level) and pain of myofascial origin. Several associated conditions can also simulate the symptoms of GTPS.2,3,13 A comprehensive understanding of the complexities of lateral hip pain is vital in making an accurate diagnosis.
Anatomy (Table I)
The greater trochanter is a large quadrilateral process found on the lateral aspect of the upper shaft of the femur where it meets the neck of the femur. The upper and anterior borders are marked by a tubercle and a depression respectively. The posterior and lower borders are roughened for musculotendinous attachment.14

The fan-shaped gluteus medius muscle originates from the lateral surface of the ilium and inserts on the superolateral surface of the greater trochanter. The gluteus minimus muscle is triangular in shape and runs from the lateral surface of the ilium to the anterosuperior aspect of the greater trochanter. The gluteal muscles (including gluteus maximus) together with tensor fascia lata are the main abductors of the hip joint. Gluteus medius is especially important in walking, running and bearing weight on one limb.3,14 When the muscle is paralysed the pelvis drops on the opposite, unaffected, side. This is known as the Trendelenburg sign.7,14 Many authors refer to the abductor muscle insertion as the 'rotator cuff' of the hip.8,15,16
The fluid-filled sacs between bony prominences and surrounding soft tissues are known as bursae. These bursae have a cushioning or padding function.3,5 Although up to 21 bursae have been described around the greater trochanter, only three of these are present in most individuals.5,8 These are the gluteus minimus bursa, located anterosuperior to the greater trochanter; the subgluteus maximus bursa between the gluteus medius tendon and the gluteus maximus muscle; and the subgluteus medius bursa found deep to the gluteus medius tendon.3 Many secondary bursae can be present and this, together with variable locations of the bursae, add to the misdiagnosis and varied response to steroid injections.3,8
GTPS has been described as a 'great mimicker' and can mimic pain from other causes like osteoarthritis (hip), spinal pathology (L4/5 level) and pain of myofascial origin
Epidemiology and associated conditions (Table II)
GTPS affects between 10% and 25% of people living in industrialised countries, with a lifetime incidence of more than 20%.3,17 It has been shown that in the primary setting around 1.8 per 1 000 patients per year report greater trochanteric pain.3,18 Hip pain is prevalent in all age groups, but more so in the fourth and sixth decades of life.3,5 There is controversy in the literature over the trend towards greater incidence of GTPS in females: the majority of studies suggest a ratio of 3 to 4:1,2,4,19,20 whereas other studies failed to show any gender predominance.12
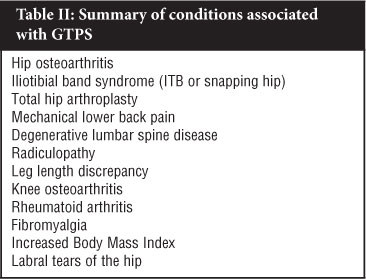
Segal et al, using a strict definition of GTPS, found that the prevalence of GTPS in a non-clinic based population of older adults (mean age 62.4 ± 8 yr) was 17.6%. There was a significantly higher incidence of GTPS in females. In the same study they showed that iliotibial band (ITB) tenderness, knee OA or pain and lower back pain was associated with GTPS. No significant association with Body Mass Index (BMI) could be proven, but there was a tendency towards higher incidence with increased BMI.2 Raman and Haslock showed a GTPS incidence of 15% in a group of rheumatoid arthritis patients.21
Tortolani et al found that 20% of patients referred to their spinal clinic for lower back pain had GTPS.4
Although an association with leg length discrepancy is mentioned in several articles,3,5 Segal et al22 could not find an association of leg length inequality (>1 cm) with GTPS. Associated labral tears and hypertrophy was reported by Voos et al in patients undergoing endoscopic gluteus medius tendon repair.23
Walker et al13 found a higher incidence of GTPS in patients with degenerative spine disease. They postulated that compromised function of the superior gluteal nerve, which supplies the gluteus medius and minimus muscles, would lead to weakened abductor function and ultimately altered lower limb biomechanics. This, in turn, would predispose to gluteal muscle pathology.
Many of the conditions that predispose to GTPS, like spinal pathology, ITB abnormalities and fibromyalgia, can also simulate the symptoms and clinical picture of GTPS. This not only makes the diagnosis of GTPS very challenging, but also confounds prevalence estimates.3
Diagnostic criteria
The diagnosis of trochanteric bursitis has always been viewed as a clinical diagnosis. Rasmussen and Fano proposed clinical criteria for the diagnosis of trochanteric bursitis.24 The criteria requires lateral hip pain and greater trochanter tenderness together with either pain at the extreme of hip rotation, abduction or adduction (especially positive Patrick-FABERE* test); pseudoradiculopathy (extending to lateral thigh) or pain on forced hip abduction. These criteria are frequently quoted, but have not been validated. *(FABERE = flexion, abduction, external rotation, extension)
With greater understanding of the causes of lateral hip pain came the term 'greater trochanteric pain syndrome'.3 GTPS encompasses a myriad of causes and associated conditions. The clinical criteria for trochanteric bursitis could still be applicable to GTPS, but the emphasis of diagnosis now falls on elucidating the cause of the lateral hip, buttock or thigh pain. An integrated approach involving thorough clinical examination, carefully selected special investigations and imaging studies is indicated.1,3,23
Aetiology and pathology
The risk factors and associated conditions of GTPS have been discussed under epidemiology. Schapira et al. demonstrated associated pathological conditions in 91.6% of patients with a diagnosis of trochanteric bursitis.25 True bursitis (inflammation) can be secondary to acute injury (trauma), overuse (chronic microtrauma) or muscle dysfunction.1,3,5 The pain generators in GTPS could be the bursae, ITB or the gluteal muscle insertions.2 Recent MRI-based studies show that radiological evidence of bursal inflammation is uncommon (<10%) in patients with lateral hip pain, but that gluteal muscle abnormalities is a constant finding. Isolated bursal distension could not be indicated in any cases.1,7,23
Inflammation, tendinoses and tears of the gluteus medius and minimus muscles or their tendons can be caused by frictional mechanisms (overuse) or tension from the ITB. Tears at the insertion of the muscle can be complete, partial or intrasubstance.15 Altered lower limb biomechanics predispose to gluteal muscle abnormalities, which is a major cause of GTPS.1,3,17,23
Domb et al26 reported that most partial gluteus medius tears are tears of the under surface of the tendon similar to PASTA (partial articular supraspinatus tendon avulsion) lesions at the shoulder. In contrast with the shoulder, at the hip this lesion is extremely difficult to visualise with endoscopy.
In a recent, small histopathological study, Silva et al could not find any histological evidence of acute or chronic inflammation in bursal specimens of patients who met the criteria for trochanteric bursitis. They challenged the view that true bursitis is a cause of GTPS.17
Other conditions that need to be considered as a cause for lateral hip pain include ITB syndrome, knee OA, lumbar spine pathology, meralgia paraesthetica, crystal deposition and infection such as tuberculosis.1-3 With a history of acute trauma, extreme caution should be taken not to miss a femoral neck fracture or avascular necrosis of the femoral head.3,23,27
Clinical setting
In the clinical setting patients will present with complaints of a chronic, intermittent lateral hip pain. The onset of the pain can be acute or subacute, ranging from an aching to a sharp, intense quality.3,5 Pain can radiate to the lateral aspect of the thigh or buttock (pseudoradiculopathy), but not often to the posterior thigh. Initially patients can experience lower back or knee pain. The pain can also be associated with hip movements, especially external rotation and abduction. Activities like prolonged standing, running, climbing or lying on the affected side can precipitate or exacerbate symptoms. A history of activities that may cause overuse injuries is important.1,3,5
Pain radiating to the lateral thigh area can be confusing. There is anatomical overlap of the ITB and the L2-L4 dermatomes. Pain radiating from lumbar facet joints, sacroiliac joints and intervertebral discs can cause symptoms similar to that of GTPS. Damage to the superior and inferior gluteal nerves can lead to neuropathic-type symptoms in the lateral thigh.3,4 The distinction between these entities lies in the fact that pain from GTPS does not radiate beyond the proximal thigh; ITB abnormalities should give tenderness over Gerdy's tubercle and a positive Ober's test and true nerve root compression gives symptoms in the lower leg and foot.4
Palpation of the affected area should reveal tenderness over the greater trochanter, especially at the insertion of the gluteus medius tendon. Palpation of this trigger point can elicit a 'jump sign' (patient pulls away forcefully on contact of the particular area).3,4,27
It is important to palpate the area 2 cm proximal to the medial joint line of the knee, the proximal trapezius and the extensor mass distal to the lateral epicondyle of the elbow as well, as this could indicate generalised myofascial tenderness.22 When assessing the range of motion of the hip, external rotation and abduction can produce symptoms. Internal rotation occasionally and extension rarely give pain. The typical pain can be reproduced with resisted active abduction. Painful flexion and extension may indicate intra-articular hip pathology. The Patrick-FABERE test should be positive in GTPS and OA.2-4,27 In a study correlating clinical presentation with MRI diagnosis, Bird et al1 found that the Trendelenburg test was the most reliable test to predict gluteal tears (sensitivity 72.2% and specificity 76.9%).
As mentioned before, other potential origins of the symptoms need to be ruled out. Limited range of motion of the hip may point to osteoarthritis or advanced avascular necrosis of the femoral head. Tenderness with deep palpation of the femoral triangle is associated with iliopsoas bursitis. Spinal deformity or lower back tenderness with loss of sensation or muscle weakness corresponding to specific nerve roots and a positive straight leg raise test could be indicative of spinal pathology and radiculopathy. Sacroiliac joint dysfunction can be assessed with provocative manoeuvres like the shear test, Yeoman's test and Gillet's test.2-4,27
Imaging studies
In earlier literature trochanteric bursitis was regarded as a clinical diagnosis. With the advancement of medical imaging, the spectrum of causes and associated conditions of lateral hip pain has broadened considerably. In the quest for accurate diagnosis, appropriate treatment and ultimately ridding patients of their symptoms, imaging studies have become an integral modality.1-3,7,23
Plain radiographs of the affected hip and whole pelvis are still relevant in the work up of patients with lateral hip pain. They are effective in screening for associated conditions like hip osteoarthritis, avascular necrosis of the femoral head, neck of femur fractures, and sacroiliac pathology. Studies mention femoro-acetabular impingement, acetabular protrusion and trochanteric exostosis as associated findings in patients with gluteal muscle pathology1,6,27 Older literature also mention calcifications around the greater trochanter although several newer studies could not identify any calcifications associated with GTPS.1,5,6
Scintigraphic findings in GTPS are mostly non-specific. Increased uptake is confined to the lateral aspect of the greater trochanter, but could indicate either bursitis or tendinosis.1
Ultrasound can be helpful in demonstrating facetal trochanteric anatomy. A so-called 'bald' facet is suggestive of a complete tear of the tendon. Tendinosis may manifest as tendon thickening and heterogeneous, decreased echogenicity. Muscle wasting with fatty infiltration and bursal fluid accumulation can also be appreciated on ultrasound.
In calcific tendinosis ultrasound is superior to MRI with better visualisation and the advantage of sonar-guided aspiration and injection.7
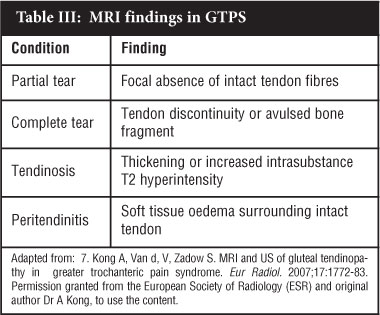
Magnetic resonance imaging (MRI) is now regarded as the gold standard investigation for recalcitrant lateral hip pain. New insight has been gained by the use of MRI in musculoskeletal imaging. It has several advantages over X-rays, ultrasound and scintigraphy, one of which is that deep and superficial soft tissue structures can be evaluated.1,28 MRI has the ability to evaluate direct signs (peritendinitis, tendinosis and partial or complete tears) and indirect signs (bursal fluid, muscular fatty atrophy, bony changes or calcification of tendon the insertion) of abductor tendon pathology and can also evaluate other structures associated with lateral hip pain,7 though Voos et al reported difficulty in distinguishing high-grade partial tears from full thickness tears on MRI.23 A summary of the most pertinent findings on MRI is given in Table III.
Treatment
Most cases of GTPS can be regarded as self-limiting.3 The initial or acute treatment of GTPS involves conservative modalities like non-steroidal anti-inflammatory drugs (NSAIDS), ice and rest. As the pain decreases, the subacute management includes modalities like ultrasound and massage. Rehabilitative and preventative measures like weight loss, behavioural modification and physiotherapy to improve muscle strength, flexibility and joint mechanics are part of many treatment regimens.3,29 The true efficacy of these 'conservative' treatments has not been reported in controlled studies.
When symptoms are unresponsive or recurrent, local injections with corticosteroids and/or local anaesthetics have been shown to be effective in relieving pain. Varied results have been published with efficacy rates varying from 60% to 100%; with recurrence rates as high as 25% within 1 year.3,12,20,24,29 Gordon reported comparable success rates of local anaesthetic and corticosteroid injection.12
No studies looking at the placebo effect of the injections have been published. A recent epidemiological study has shown that in a primary setting the long-term recovery rate is 2.7 times higher in patients who had been treated with corticosteroid injections.18 Cohen et al29 found no difference in the efficacy of landmark-guided injections and fluoroscopic-guided injections. Failed response to local injections can be ascribed to several reasons ranging from misdiagnosis, underlying gluteus medius tendinopathy or inaccurate needle placement.
Shbeeb et al describe their injection technique as using 40-80 mg of methylprednisolone combined with 4-6 ml of 1% lignocaine. Half of the mixture is injected at the point of maximal tenderness with the rest infiltrated in the surrounding tissues. Complications, although rare, include sterile abscess, nerve injury, granulomatous reaction and skin atrophy.5
When conservative management and local injections fail to alleviate symptoms, surgical intervention is the next step. Several surgical modalities have been described.5,6,8,23
Classically, open bursectomy with debridement and removal of calcifications was used for the surgical treatment of persistent GTPS. The results were relatively good on long-term follow-up.5
Craig et al described a new ITB Z-lengthening procedure specifically for recalcitrant GTPS. His results were good to excellent in 16 of the 17 hips in 15 patients. These results are comparable to other techniques like fenestration, T-shaped incision or longitudinal excision with bursectomy of the ITB.8
Endoscopy/arthroscopy has emerged as a useful adjunctive diagnostic as well as a therapeutic modality. Voos et al reported ten cases of gluteus medius tendon tears (proven on MRI). On MRI eight of the ten patients had anterior labral tears. All ten patients were treated with endoscopic gluteus medius tendon repair with suture anchors and bursectomy. Eight of the patients had a labral debridement and one had a labral repair. Other abnormalities that were addressed endoscopically were pincer-type impingement between acetabulum and head of the femur (1), trochanteric exostosis (1), tight ITB (1). On two-year follow-up all ten patients had resolution of pain, full abductor strength and full range of motion of the hip. They do mention that total gluteus medius tendon avulsions from the greater trochanter are better managed with open repair.23 Baker et al reported a series of 25 patients treated with endoscopic bursectomy without tendon repair with significant improvement in all patients.30 Trochanteric bursectomy could be enough to alleviate symptoms, but in conjunction with gluteus medius tendon repair, pain could be relieved and muscle strength regained.23 Recently, Domb et al described a novel trans-tendinous repair technique for partial tears of the undersurface (articular side) of the gluteus medius.26
Endoscopic treatment of resistant GTPS with gluteus medius tears/tendinopathy and bursitis has been shown to be an effective modality of treatment, although long-term follow-up studies are still lacking.23,31,32
Modalities used in other tendinoses (tennis/golf elbow, Achilles tendinopathy) such as autologous blood injection33 and eccentric loading and stretch exercises34,35 have not been reported on in the treatment of gluteus tendinopathy.
Conclusion
Greater trochanteric pain syndrome is a common, often underdiagnosed condition that is characterised by lateral hip pain that may radiate to the buttock or lateral thigh. The consensus in the latest literature is that gluteus medius tendon pathology is the underlying cause, but that trochanteric bursitis may play an important role in causing pain. Several conditions are associated with GTPS: some of them may predispose to GTPS, while others may mimic the symptoms. Clinically patients have tenderness over the greater trochanter in the side-lying position and pain with resisted abduction. MRI has become the imaging study of choice and provides accurate detail of the relevant soft tissue structures. The mainstay of treatment still involves conservative measures including lifestyle changes, physiotherapy, NSAIDs and corticosteroid injections. In resistant cases or cases with proven gluteus medius tendon tears, endoscopic bursectomy with tendon repair has been shown to be effective.
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article. The content of this article is the sole work of the authors.
References
1. Bird PA, Oakley SP, Shnier R, Kirkham BW. Prospective evaluation of magnetic resonance imaging and physical examination findings in patients with greater trochanteric pain syndrome. Arthritis Rheum 2001;44(9):2138-45. [ Links ]
2. Segal NA, Felson DT, Torner JC, Zhu Y, Curtis JR, Niu J, et al. Greater trochanteric pain syndrome: epidemiology and associated factors. Arch Phys Med Rehabil 2007;88(8):988-92. [ Links ]
3. Williams BS, Cohen SP. Greater trochanteric pain syndrome: a review of anatomy, diagnosis and treatment. Anesth Analg 2009;108(5):1662-70. [ Links ]
4. Tortolani PJ, Carbone JJ, Quartararo LG. Greater trochanteric pain syndrome in patients referred to orthopedic spine specialists. Spine J 2002;2(4):251-54. [ Links ]
5. Shbeeb MI, Matteson EL. Trochanteric bursitis (greater trochanter pain syndrome). Mayo Clin Proc 1996;71(6):565-69. [ Links ]
6. Karpinski MR, Piggott H. Greater trochanteric pain syndrome. A report of 15 cases. J Bone Joint Surg Br 1985;67(5):762-63. [ Links ]
7. Kong A, Van d, V, Zadow S. MRI and US of gluteal tendinopathy in greater trochanteric pain syndrome. Eur Radiol 2007;17(7):1772-83. [ Links ]
8. Craig RA, Jones DP, Oakley AP, Dunbar JD. Iliotibial band Z-lengthening for refractory trochanteric bursitis (greater trochanteric pain syndrome). ANZ J Surg 2007;77(ll):996-98. [ Links ]
9. Apley AG, Solomon L. Apley's system of orthopaedics and fractures. 6th ed. London: Butterworth Scientific. 1982. [ Links ]
10. Stegeman H. Die chirurgische Bedeutung paratkularer Kalkablagerungen. Arch Klin Chir 1923;125:718-38. [ Links ]
11. Leonard MH. Trochanteric syndrome; calcareous and noncalcareous tendonitis and bursitis about the trochanter major. J Am Med Assoc 1958;168(2):175-77. [ Links ]
12. Gordon EJ. Trochanteric bursitis and tendinitis. Clin Orthop 1961;20:193-202. [ Links ]
13. Walker P, Kannangara S, Bruce WJ, Michael D, Van der Wall H. Lateral hip pain: does imaging predict response to localized injection? Clin Orthop Relat Res 2007;457:144-49. [ Links ]
14. Palastanga N, Field D, Soames R. Anatomy and Human Movement. 4th ed. London: Butterworth, Heinemann. 1989. [ Links ]
15. Bunker TD, Esler CN, Leach WJ. Rotator-cuff tear of the hip. J Bone Joint Surg Br 1997;79(4):618-20. [ Links ]
16. Kagan A. Rotator cuff tears of the hip. Clin Orthop Relat Res 1999;368:135-40. [ Links ]
17. Silva F, Adams T, Feinstein J, Arroyo RA. Trochanteric bursitis: refuting the myth of inflammation. J Clin Rheumatol 2008;14(2):82-86. [ Links ]
18. Lievense A, Bierma-Zeinstra S, Schouten B, Bohnen A, Verhaar J, Koes B. Prognosis of trochanteric pain in primary care. Br J Gen Pract 2005;55(512):199-204. [ Links ]
19. Anderson TP. Trochanteric bursitis: diagnostic criteria and clinical significance. Arch Phys Med Rehabil 1958;39(10):617-22. [ Links ]
20. Krout RM, Anderson TP. Trochanteric bursitis: management. Arch Phys Med Rehabil 1959;40(1):8-14. [ Links ]
21. Raman D, Haslock I. Trochanteric bursitis—a frequent cause of 'hip' pain in rheumatoid arthritis. Ann Rheum Dis 1982;41(6):602-603. [ Links ]
22. Segal NA, Harvey W, Felson DT, Yang M, Torner JC, Curtis JR, et al. Leg-length inequality is not associated with greater trochanteric pain syndrome. Arthritis Res Ther 2008;10(3):R62. [ Links ]
23. Voos JE, Shindle MK, Pruett A, Asnis PD, Kelly BT. Endoscopic repair of gluteus medius tendon tears of the hip. Am J Sports Med 2009;37(4):743-47. [ Links ]
24. Ege Rasmussen KJ, Fano N. Trochanteric bursitis. Treatment by corticosteroid injection. Scand J Rheumatol 1985;14(4):417-20. [ Links ]
25. Schapira D, Nahir M, Scharf Y. Trochanteric bursitis: a common clinical problem. Arch Phys Med Rehabil 1986;67(11):815-17. [ Links ]
26. Domb BG, Nasser RM, Botser IB. Partial-thickness tears of the gluteus medius: rationale and technique for transtendinous endoscopic repair. Arthroscopy 2010;26(12):1697-705. [ Links ]
27. Margo K, Drezner J, Motzkin D. Evaluation and management of hip pain: an algorithmic approach. J Fam Pract 2003;52(8):607-17. [ Links ]
28. Kingzett-Taylor A, Tirman PF, Feller J, McGann W, Prieto V, Wischer T, et al. Tendinosis and tears of gluteus medius and minimus muscles as a cause of hip pain: MR imaging findings. AJR Am J Roentgenol 1999;173(4):1123-26. [ Links ]
29. Cohen SP, Strassels SA, Foster L, Marvel J, Williams K, Crooks M, et al. Comparison of fluoroscopically guided and blind corticosteroid injections for greater trochanteric pain syndrome: multicentre randomised controlled trial. BMJ2009;338:b1088. [ Links ]
30. Baker CL, Jr., Massie RV, Hurt WG, Savory CG. Arthroscopic bursectomy for recalcitrant trochanteric bursitis. Arthroscopy2007;23(8):827-32. [ Links ]
31. Voos JE, Ranawat AS, Kelly BT. The peritrochanteric space of the hip. Instr Course Lect 2009;58:193-201. [ Links ]
32. Voos JE, Rudzki JR, Shindle MK, Martin H, Kelly BT. Arthroscopic anatomy and surgical techniques for peritrochanteric space disorders in the hip. Arthroscopy 2007;23(11):1246-45. [ Links ]
33. Kazemi M, Azma K, Tavana B, Rezaiee MF, Panahi A. Autologous blood versus corticosteroid local injection in the short-term treatment of lateral elbow tendinopathy: a randomized clinical trial of efficacy. Am J Phys Med Rehabil 2010;89(8):660-67. [ Links ]
34. Alfredson H, Pietila T, Jonsson P, Lorentzon R. Heavyload eccentric calf muscle training for the treatment of chronic Achilles tendinosis. Am J Sports Med 1998;26(3):360-66. [ Links ]
35. Jonsson P, Alfredson H, Sunding K, Fahlstrom M, Cook J. New regimen for eccentric calf-muscle training in patients with chronic insertional Achilles tendinopathy: results of a pilot study. Br J Sports Med 2008;42(9):746-49. [ Links ]
 Reprint requests:
Reprint requests:
Dr Danie Hugo
Email: danie.hugo1@gmail.com














