Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.10 n.4 Centurion Jan. 2011
CLINICAL ARTICLE
Intramedullary locked fixation of clavicle shaft fractures : review of early results
Dr PR King MBChB(Stell); Dr A Ikram MBBS, FCS(Orth)SA
Registrar,Orthopaedic Surgery, Advanced Orthopaedic Training Centre, Tygerberg Academic Hospital, Cape Town, South Africa
Consultant, Orthopaedic Surgery, Advanced Orthopaedic Training Centre, Tygerberg Academic Hospital, Cape Town, South Africa
ABSTRACT
Background
To assess the effectiveness of a novel locked intramedullary device in the treatment of acute clavicle shaft fractures.
Description of methods
Patients admitted with midshaft clavicle fractures were assessed to determine whether operative fixation of the fracture was required. Indications for surgery were: midshaft clavicle fractures with 100% displacement; more than 1.5 cm of shortening; presence of a displaced butterfly segment; bilateral clavicle fractures; ipsilateral displaced glenoid neck fractures; skin and neurovascular compromise. Patients who matched the criteria for surgery were treated operatively with an intramedullary locked device by the author. Postoperatively, patients were kept in a shoulder immobiliser for a period of 6 weeks. Patients were invited to attend a scheduled followup visit where the data was collected that comprised the review. All patients were assessed on the same day by the surgeon, a radiologist, a physiotherapist and an occupational therapist. Scar size and quality, Dash score, Constant Shoulder score, complications and the radiological picture were assessed.
Summary of results
Twentynine patients (31 clavicle fractures - two patients sustained bilateral fractures), 18 males and 11 females with a mean age of 28 years attended the schedule data collection visit and were included in the study. Twentynine clavicles achieved complete union with the remaining two fractures progressing normally to union at 10 and 13 weeks post surgery. Three patients developed postoperative complications - two nail failures and one hardware sepsis. All three fractures achieved union despite the respective complications and achieved union in an acceptable position. Two of the patients were noncompliant with the postoperative regimen and one sustained secondary trauma to the affected shoulder. These factors are believed to have caused the nail breakages in the two cases but implant failure could not be excluded.
Conclusion
Locked intramedullary fixation of clavicle shaft fractures that matches the criteria for operative fixation was found to be a reliable method of achieving fracture reduction and fracture union. This operation is moderately demanding with a short learning curve.
Level of evidence
Case series; level IV evidence
Key words: Clavicle, fracture, intramedullary, locked, nailing
BACKGROUND
The clavicle is a bone frequently fractured through a number of mechanisms. Although most fractures are benign and heal with minimal attention to give excellent results, some clavicle fractures need extra attention for satisfactory results to be achieved. These fractures have historically been overlooked and it has only recently come to the attention of clinicians and researchers that patient satisfaction is not what is expected.
The treatment of these special fractures has been a point of controversy and debate. The type of fracture that needs to be treated surgically has been well researched and seems to be resolved. The debate on which type of operative treatment is appropriate for each type of fracture is less well resolved with numerous treatment options available with various positive and negative aspects attached to each of them.1
Numerous fixation devices are available on the market with new technology becoming available on a regular basis. The development of a locked intramedullary device that can be inserted with minimal surgical exposure to restore the anatomy of the clavicle, while giving enough fracture stability to allow fracture healing, has been an exciting new acquisition.
No literature exists reviewing the results of patients treated with this device as it has only recently become available and is not widely used yet. This study was conducted to assess the effectiveness of this novel device in achieving fracture union with minimum complications to allow patients to return to their previous level of functioning.
Clavicle fractures are common fractures comprising 2.6%-4% of all adult fractures and account for 35% of injuries to the shoulder girdle.1 Sixtyeight per cent of fractures occur in men with the left clavicle being affected in 61%.2 Fractures of the middle third of the clavicle account for 69% of fractures of the clavicle.1 Fractures occurring in the middle third of the clavicle are displaced in 48% and comminuted in 19% of cases.2
Various treatment modalities exist for the treatment of middle third clavicle fractures. Treatment options include nonoperative treatment, mostly with a sling or figure-of-8 bandage, and operative treatment.
However, the optimal treatment for displaced middle third clavicle fractures remains controversial and widely debated.3
Recent studies have indicated significantly higher complication rates in certain fracture types treated conservatively.35 Nonrandomised, noncomparative, pooled data across all studies comparing conservative treatment with plating of middle third clavicle fractures have shown a nonunion rate of 2.5% in the operatively treated fractures compared to a nonunion rate of 5.9% in the conservatively treated group.3 When the displaced group of fractures is looked at separately the nonunion rate increases to 15.1%.3
Hill, McGuire and Crosby showed in 1997 in a retrospective study of 52 nonoperatively treated middle third clavicle fractures that displaced fractures with initial shortening of >20 mm was associated with a higher risk of nonunion and a poor clinical outcome.4
A recent multicentre study comparing nonoperative treatment with primary plate fixation for displaced fractures in 132 middle third clavicle fractures showed superior functional outcomes, lower rates of malunion and nonunion and a shorter time to union in the operative group.5
Escola, Vainionpaa, Myllynen, Patiala and Rokhanen demonstrated that malunion of a middle third clavicle fracture with shortening of the clavicle may alter the position of the glenoid fossa which in turn may affect glenohumeral mobility and scapular rotation.6 This may lead to unsatisfactory results and loss of function. Lazarides and Zafiropoulos looked at 132 patients with united fractures of the middle third of the clavicle after conservative treatment. Residual symptoms and overall patient satisfaction after treatment were assessed through a questionnaire. In this study 25.8% of patients were dissatisfied with their treatment result. Final clavicle shortening of more than 18 mm in males and 14 mm in females was associated with an unsatisfactory result.7
Operative treatment of displaced middle third clavicle fractures are associated with significantly improved Constant Shoulder and Dash scores when compared to fractures in patients treated conservatively.5
It is widely accepted in the literature that undisplaced or minimally displaced middle third clavicle fractures can and should be treated conservatively either in a sling or a figure-of-8 bandage.1,8
Indications for surgical treatment of middle third clavicle fractures using either open reduction and a plate and screws or an intramedullary device can be divided into absolute and relative indications. Absolute indications include open fractures, overlying skin compromise, neurological deficit or associated vascular injury.8 Relative indications include multisystem traumatised patients, painful malunions and nonunions and a floating shoulder. Relative indications have also been expanded to include fractures with shortening of 15-20 mm, complete displacement and comminution.8 These indications are expanded as suggested by Zenni, Krieg and Rosen to include patients who cannot tolerate prolonged immobilisation of the upper limb, for example patients with Parkinson's disease and neuromuscular disorders.8
Operative treatment consists of open reduction and internal fixation using locked or nonlocked plates and screws or open or closed reduction with internal fixation using intramedullary rods, wires or nails.3
Numerous intramedullary fixation devices for the treatment of middle third clavicle fractures are available on the market and are commonly used. These include Knowles pins, Hagie pins, Rockwood pins and minimally invasive titanium nails.9 Techniques include antegrade insertion through an entry point on the anteromedial surface of the clavicle or through a posterolateral entry point in the lateral fragment. Both of these techniques make it necessary to open the fracture site to reduce the fracture.
Intramedullary fixation of displaced middle third clavicle fractures are associated with a significantly reduced nonunion rate compared to conservative treatment.3 Thyagarajan recommended intramedullary fixation of displaced middle third clavicle fractures over plating and conservative treatment.10 He reported no nonunions and reported scarrelated complications and prominent hardware in the plating group in 42% (8 out of 17 patients).
In a randomised controlled trial using the Rockwood pin by Ferran et al where the Rockwood pin was compared to plating of displaced middle third clavicle fractures there was no difference between the union rates, Constant Shoulder score or the Oxford Shoulder score between the two groups.11
However, in this study all the Rockwood pins had to be removed and 53% of the plates had to be removed due to infection or soft tissue irritation.12
Boehme et al reported successful treatment of middle third clavicle fracture nonunions with the Hagie intramedullary pin. Twenty of their 21 patients achieved union.12
Intramedullary nailing of the clavicle holds considerable advantages over other forms of fixation of clavicle fractures. Due to the percutaneous operative technique with no periosteal stripping and no bone/plate compression interface, the periosteal blood supply is preserved and thus union is promoted.12 Intramedullary fixation of a middle third clavicle fracture requires a small skin incision with minimal soft tissue dissection. This leads to a cosmetically acceptable scar and much higher patient satisfaction.13 As previously discussed a very high proportion (± 50%) of fractures treated with plate fixation requires a second operation to remove the plate. This has to be done through the original skin incision with further scarring and soft tissue compromise. Traditional intramedullary devices also necessitated implant removal after fracture union, but removal can be facilitated via a small skin incision and be done percutaneously.
Materials and methods
The study was designed as a case series reviewing the outcome of patients with a middle third clavicle fracture treated with an intramedullary device. Institutional approval was obtained from the relevant review board prior to the study commencing. A total of 29 patients (31 fractured clavicles) admitted to a tertiary hospital with midshaft clavicle fractures fulfilling the inclusion criteria were included in the study after being treated surgically with a locked intramedullary device by the author.
Inclusion criteria
• Minimum of 15 years of age
• Fracture of the middle third of the clavicle as determined by the Allman classification with one of the following characteristics:
- Minimum of 15 mm shortened- Presence of a significantly displaced butterfly segment at the fracture site
- 100% fracture displacement
- Skin tenting or tethering
- Threatening skin breakdown
- Neurovascular structure injury as a result of the fracture
- Open fractures
- Associated scapula fracture causing a 'floating shoulder'
- Bilateral clavicle fractures
• Patients who attended the data collection visit.
• Patient at least 10 weeks post surgery.
Device description
The Sonoma Clavicle fracture repair system (CRx System) is based on WaviBodyTM and ActivelocTM technology, a patented new approach that transforms a flexible intramedullary device at insertion into a rigid fixation system after placement. The stainless steel device consists of a solid straight hub, a flexible tubular midsection, and an internal fixation system.
The CRx device is inserted into the intramedullary canal following reduction of the fracture. Once properly seated in the intramedullary canal, the internal WaviBodyTM assembly is activated. Upon activation, the flexible WaviBodyTM section is transformed into a rigid nail and ActivelocTM grippers at the end of the WaviBodyTM are deployed. The ActivelocTM grippers provide additional stability to the implant eliminating the need for a second incision at the medial end of the device.
The Sonoma CRx clavicle repair devices are intended to be used to repair an acute middle third clavicle fracture, middle third clavicle fracture malunion or non-union.
Management
Patients were selected for surgery according to the inclusion criteria and kept in a shoulder immobiliser until they were operated on a suitable trauma slate within 1 week of presentation.
Patients were given 2 g of intravenous Kefzol preop and a general anaesthetic. Patients were positioned in the beach chair position and prepped and draped. A ± 5 cm incision is made over the fracture site and the medial and lateral fragments prepared while taking care that minimal soft tissue is stripped off the clavicle. The fracture is reduced and the intramedullary nail applied from lateral to medial. The medial aspect of the device is activated and the device locked with a screw on the lateral aspect. Adjuvant fixation of the butterfly segments are performed using cerclage wire or nonabsorbable braided sutures while avoiding periosteal stripping.
The wound is closed in layers with meticulous care taken to approximate the deltopectoral fascia and the platysma muscle. Subcutaneous absorbable sutures are placed and the surgical wound sealed with a plastic surgical dressing. Patients are kept in a shoulder immobiliser for a period of 6 weeks postop (Figures 1, 2 and 3).
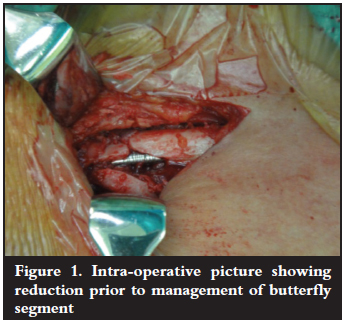
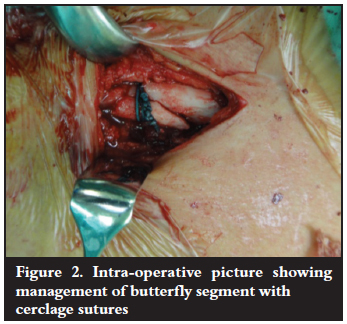
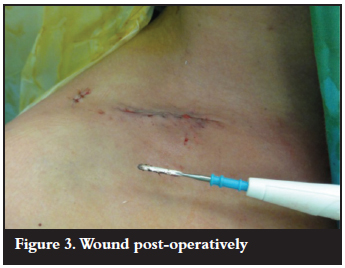
Patients were instructed to perform pendular exercises of the shoulder and range of movement exercises of the ipsilateral elbow six times a day for a period of 6 weeks. Patients were kept in the shoulder immobiliser for an extended period due to general patient unreliability and noncompliance with activity restriction. The use of the shoulder immobiliser served as a reminder that normal activity of the affected limb should be restricted. Once radiological evidence of progression to union (callus at the fracture site) was seen, full range of movement of the affected shoulder was commenced with the help of a physiotherapist. Full range of movement exercises of the shoulder were normally commenced at 6 weeks. Full return to activity and sport were advised at 3 months postop - although most patients returned to full activity prior to this date due to non-compliance.
Patients were followed up at 7 days postop for a wound assessment and then at 6 weeks and 3 months for radiological evaluation.
Assessment
Patients gave informed consent prior to surgical treatment and prior to enrolling in the study. All patients reviewed were seen on the same day ranging from a period of 10 weeks to 47 weeks postop.
Fifteen degree cephalad tilt radiographs taken at admission preoperatively of each fractured clavicle were used to classify fractures according to their degree of comminution and to measure displacement in the coronal plane and shortening.
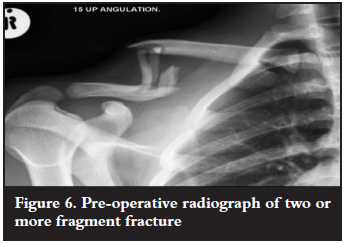
The fracture is described as simple if the fracture is transverse or oblique with a single fracture line. Single fragment fractures have a large, single fragment complicating the fracture. Two or more fragment fractures have substantial comminution of the fracture with two or more major fragments forming part of the fracture (Figures 4, 5 and 6).

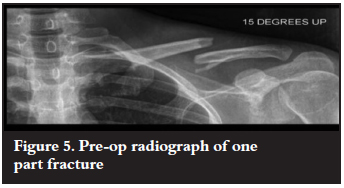
Anaesthetic notes were used to determine the time each patient spent in theatre and to determine any anaesthetic complications. The surgical notes were examined to determine any surgical complications.
The assessment comprised a clinical examination of the surgical scar for size and cosmetic result. The cosmetic result was graded as excellent if the wound was linear and only noticeable on close inspection. The scar was graded as good if it is slightly wider and more noticeable. Fair scars were wounds that were more than 0.5 cm wide and easily noticeable. Scars were judged as poor if there were any keloid formation.
An occupational therapist assessed each patient separately and facilitated the completion of the Dash and Constant Shoulder scores. Section D (power of affected limb) of the Constant Shoulder score was not included and the score was calculated out of 75 instead of the normal 100. The power assessment was disregarded because of inconsistencies in the method of testing from patient to patient. The power score was deemed as unreliable because of this.
The range of movement assessment of the affected limb was done by a physiotherapist individually with each patient. The range of movement assessment was done and scored according to the range of movement section of the Constant Shoulder score.
Intramedullary nailing of the clavicle holds considerable advantages over other forms of fixation of clavicle fractures
The score is calculated out of 40 and tests forward flexion, abduction, internal and external rotation. Full range of motion in each plane is scored as 10 and thus full range of movement is deemed as 40/40.
Standard anteriorposterior, 15º and 45º cephalad tilt radiographs of the affected clavicle was taken and evaluated by a radiologist for progression to union and quality of reduction. A 15º cephalad view of the contralateral clavicle was used to assess the restoration of length of the injured clavicle.
Patient notes were reviewed to assess any complications and adverse events experienced.
Statistical analysis
The primary objectives of the study were an analysis of:
• union rates
• quality of restoration of anatomy of the clavicle
• functional outcome
• complication rates
• surgical scar size and quality
Functional outcome was measured by means of Dash scores and Constant Shoulder scores. These scores, the surgical scars measurements and restoration of anatomy data were analysed using appropriate descriptive statistics, including the following: means, standard deviations, confidence intervals, medians and quartiles, etc. Scores were also grouped according to categories and were analysed using frequency distributions, proportions and 95% confidence intervals.
For all further analyses the following general analysis guidelines were followed: Summary statistics were used to describe the variables. Distributions of variables were presented with histograms and or frequency tables. Medians or means were used as the measures of central location for ordinal and continuous responses and standard deviations and quartiles as indicators of spread.
Results (Table I)
During the study period 45 clavicle fractures were treated by intramedullary nailing. Of these 29 patients with 31 clavicle fractures treated by locked intramedullary nailing were reviewed - 18 male and 11 female. Ten patients failed to attend the scheduled data collection visit and four patients were less than 10 weeks postoperative, and thus not included. The mean age of the patients was 28 years (15-44). Fifteen right clavicles and 16 left clavicle fractures were reviewed with mechanisms of injury ranging from motor vehicle accidents (12; 38%), a fall on the point of the shoulder (10; 32%), motorbike accidents (7; 23%) and rugby injuries (2; 7%).
Nine fractures were classified as simple, nine as single fragment fractures and 13 as two or more fragment fractures. Average coronal displacement of the lateral portion of the clavicle in relation to the medial portion was 18.8 mm (6-44) inferiorly. Average shortening of the affected clavicle was found to be 18.2 mm (0-39) preoperatively.
Patients spent an average of 77 minutes (50-110) in theatre from induction to leaving the theatre post surgery. No anaesthetic or surgical complications were encountered intraoperatively.
The average time patients seen at the scheduled data collection review visit after surgery was 27 weeks (10-47).
Constant Shoulder scores
The average Constant Shoulder score was 68 (32-75) for the group assessed at the specific followup date. The average score for patients 10 weeks postop was 55 (51-64). This score should not be compared to Constant Shoulder scores calculated for patients treated by other means as the full score was not used. The score does however give a reflection of the recovery of the patient after trauma.
Dash scores
The average Disabilities of the Arm, Shoulder and Hand (Dash) score was 17.5 (0 to 70). The average Dash score for patients at 10 weeks postop was 38 (2.5-70). The two patients with clavicle fractures with ipsilateral glenoid neck fractures had Dash scores of 63 and 70 respectively. This underlines the severity of this type of injury.
Shoulder range of movement
The average range of movement score of affected shoulders, according to the ROM section of the Constant Shoulder score, was 38 (8-40).
Surgical scar
The average length of surgical scar was 51 mm (30-100) with 14 patients (46%) achieving an excellent cosmetic result and 15 patients (48%) achieving a good cosmetic outcome. One (3%) wound was judged as having a fair result and one (3%) wound was assessed as having a poor result secondary to keloid formation.
Radiographic assessment
The average length difference postoperatively between the fractured clavicle and the contralateral normal clavicle was 5.1 mm (0-11). The patient who sustained bilateral clavicle fractures during the same trauma event was not included in the length difference review as no control was available. The average residual angulation of the injured clavicles postoperatively was 6º (0-32). The residual angulation was measured along the AP axis of the clavicle with the medial fragment taken as reference.
Fracture union
All fractures (29) had achieved union when reviewed at the data collection visit at 14 weeks or longer post surgery. Two fractures at 13 and 10 weeks post surgery were assessed as showing signs of incomplete union (Figures 7 and 8).
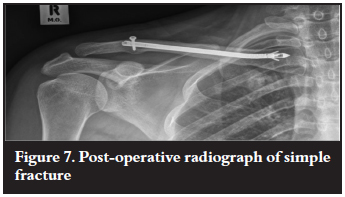
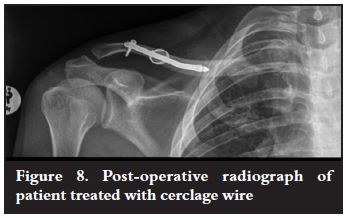
Complications
Three postoperative complications were encountered. One patient developed a deep infection that necessitated removal of the implant. The fracture was partially united when the implant was removed.
Two patients had failure of the implant. Both implants failed at the junction of the flexible and nonflexible portion of the implant.
Discussion
This series indicates that locked intramedullary fixation of middle third clavicle fractures, which fit the criteria for operative fixation, is an effective modality of treatment.
Functional outcome of the affected shoulder is comparable to that reported to be achieved with plating of the clavicle. It is uncertain whether longer periods of postoperative immobilisation are needed to protect the fracture than with conventional locked plating. In this series a period of 6 weeks' immobilisation was used, but this may be unnecessarily conservative. The prolonged immobilisation does not seem to affect the functional outcome of the affected shoulder.
The shoulder range of motion recovered to normal in a short period of time once mobilisation was started. Concomitant ipsilateral glenoid neck fractures seem to be an exception to the rule as both these patients achieved poor functional outcomes despite anatomical reduction and fixation being achieved.
Fixation of the fracture can be achieved through a much smaller incision than that needed for fixation using a plate and screws. There is also no prominent hardware under the skin necessitating removal of the implant. A very good cosmetic result is achieved using this modality making the device particularly useful in the treatment of women and young adults.
The complications encountered could be managed successfully. In the patient who became septic the sepsis cleared up with intravenous antibiotics and the fracture united uneventfully in an acceptable position.
Both implants failed at the junction of the flexible and nonflexible portion of the implant. In the first case the implant failed secondary to additional trauma to the affected shoulder ± 1 month post surgery. The patient failed to seek medical attention and presented 6 weeks later with the fracture united in an acceptable position. The implant was left in situ as it was viewed as stable in its current position. In the second case the patient failed to adhere to the prescribed postoperative regimen and resumed normal duty at a building site as a heavy labourer 1 week after surgery. The patient did not report for followup and the failure was only discovered 7 months after surgery. His fracture united in an acceptable position and the implant was left in situ.
While it is assumed that the implant failure was due to noncompliance with the immobilisation regimen and secondary trauma, failure secondary to failure of the fixation device could not be completely excluded. Further review with a larger sample size is desirable to further prove the effectiveness of the device.
Failure of the device in a nonunited fracture may prove problematic as removal of the medial end of the device can be difficult. The authors advocate early intervention if normal progression to union is absent.
The limited sample size and diverse time spans postop of the data collection visit are limiting factors to this study.
The patients were all operated by the same surgeon leading to a consistent surgical technique. The postoperative followup was conducted by the same surgeon who did the operations.
The union rate achieved with this device compared to conventional plating is of particular interest to the authors. Initial results are encouraging with no nonunions found during this review, but further review with a larger sample size is needed.
Further study is needed to determine the fracture configurations that are optimally treated by locked intramedullary nailing as well as fracture types where the device is less effective.
The authors have received institutional approval to conduct a randomised controlled trial comparing the device to conventional plating using an anatomically contoured locking plate. This study will commence shortly. No benefits of any form have been received by the authors from a commercial party related directly or indirectly to the subject of this article.
Source of funding: Funding was made available by Silvamed (Pty) Ltd, the company distributing the device. The company provided R200 for each patient who attended the specified data collection visit. The funds provided to patients were to cover their respective travel expenses as most patients live some distance away from the institution where the review was conducted. Total funding supplied was R5 800.
References
1. Kashif Khan L.A, Bradnock TJ, Scott Caroline, Robinson Michael. Fractures of the clavicle. The Journal of Bone & Joint Surgery Am. 2009;91:447-60. [ Links ]
2. Postacchini Franco, Gumina Stefano, De Santis P, Albo Francesco. Epidemiology of clavicle fractures. Journal of Shoulder and Elbow Surgery. 2002;11(5):452-56. [ Links ]
3. Zlowodzki M, Zelle B, Cole P, Jeray K, McKee M. Treatment of acute midshaft clavicle fractures: Systematic review of 2144 fractures. Journal of Orthopedic Trauma. 2005;19(7). [ Links ]
4. Hill JM, McGuire MH, Crosby LA. Closed treatment of displaced middlethird fractures of the clavicle gives poor results. J Bone Joint Surg Br. 1997;79:537-39. [ Links ]
5. Canadian Orthopedic Trauma Society. Nonoperative treatment compared with plate fixation of displaced midshaft clavicular fractures. A multicenter randomized clinical trial. J Bone Joint Surg Am. 2007;89:1-10. [ Links ]
6. Escola A, Vainionpaa S, Myllynen P, Patiala H, Rokhanen P. Outcome of clavicular fracture in 89 patients. Arch Orthop Trauma Surg 1986;105:337-38. [ Links ]
7. Lazarides S, Zafiropoulos G. Conservative treatment of fractures at the middle third of the clavicle: The relevance of shortening and clinical outcome. J Shoulder Elbow Surg 2006;15:191-94. [ Links ]
8. Zenni EJ, Krieg JK, Rosen M. Open reduction and internal fixation of clavicle fractures. Journal of Bone and Joint Surgery 1981;63A(1). [ Links ]
9. Jubel A, Andemahr J, Schiffer G, Tsironis K, Rehm KE. Elastic stable intramedullary nailing of middclavicular fractures with a titanium nail. Clin Orthop Relat Res. 2003;408:279-85. [ Links ]
10. Thyagarajan DS. Treatment of displaced midclavicle fractures with Rockwood pin: a comparative study. Proceedings from the 72nd Annual Meeting of the American Academy of Orthopedic Surgeons. 2005. [ Links ]
11. Ferran N, Hodgson P, Vannet N, Williams R, Evans R. Locked intramedullary fixation versus plating for displaced and shortened midshaft clavicle fractures: A randomized clinical trial. Journal of Shoulder and Elbow Surgery. 2010;19:783-89. [ Links ]
12. Boehme D, Curtis R, De Haan J, Kay S, Young D, Rockwood D. Nonunion of fractures of the midshaft of the clavicle: Treatment with a modified Hagie intramedullary pin and autogenou bone grafting. The Jounal of Bone and Joint Surgery. 1991;73A(8):1219-26. [ Links ]
13. Wang K, Dowrick A, Choi J, Rahim R, Edwards E. Postoperative numbness and patient satisfaction following plate fixation of clavicular fractures. Injury, Int J Care of Injured. 2010;41:1002-1005. [ Links ]
 Reprint requests:
Reprint requests:
Dr PR King
Advanced Orthopaedic Training Centre Tygerberg Academic Hospital
Cape Town, South Africa
Cell: +27 83 364 8470
Email: Docreg10@gmail.com














