Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.10 n.4 Centurion Jan. 2011
CLINICAL ARTICLE
Role of ultrasound as a non-invasive method of diagnosis of chronic exertional compartment syndrome
D WassermannI; Z OschmanII
IMBChB, MSc Student, Section Sports Medicine, University of Pretoria
IIMBChB DCH MSc Sports Section Sports Medicine, University of Pretoria
ABSTRACT
Chronic exertional compartment syndrome (CECS) is a well-recognised condition, which can result in significant morbidity and limitation of activity in athletes and non-athletes alike. At present invasive intramuscular pressure (IMP) measurements are still considered the gold standard for diagnosing CECS. The non-invasive nature of ultrasound makes it an attractive alternative to direct IMP measurement.
This retrospective study is a literature and case review of 34 subjects with exerciseinduced leg pain who underwent ultrasound compartment measurement for CECS. Eighteen (group P) of 34 were found to be positive. Fifteen of group P demonstrated calf increases of >15 mm and an additional three with increases of <15 mm failed to return to the resting state at 10 mins after exercise. Sixteen subjects demonstrated a normal ultrasound after exercise.
At follow-up (1-2 years) a telephonic interview of 25 participants showed that 15 of the 18 with a positive confirmation of CECS had responded well to surgical decompression and 10 of the 16 negative cases had responded well to conservative treatment.
This study suggests that ultrasound may be a useful tool for the assessment of CECS.
Keywords: ultrasound, exertional, chronic compartment syndrome, non-invasive, intramuscular pressure
INTRODUCTION
Chronic exertional compartment syndrome (CECS) is a well-recognised condition which can result in significant morbidity and limitation of activity in athletes and nonathletes alike. It is defined as an activity-related, reversible, myofascial intramuscular pressure increase, resulting in decreased tissue perfusion and abnormalities in neuromuscular function.1
It typically affects young people who are engaged in sports and usually results from overuse, poor technique or rapidly increased muscle mass following rigorous athletic training. Muscle mass is increased significantly in a short period of time, resulting in a pathological increase in the intramuscular pressure, as the compartment cannot accommodate the transient increase in volume required secondary to increased blood flow.
The pain is intermittent and might be sharp, cramp-like or burning, occurring predominantly during exercise. The level of exercise that precipitates the symptoms may vary considerably, from running a 'four minute mile' to walking around the block. The patients can often continue with the exercise but at a reduced level. At the end of the exercise the pain usually resolves quickly but could persist for hours or even days. CECS symptoms are bilateral in 70% of patients. Pain is most commonly associated with plantar flexion and dorsiflexion of the foot, as the anterior and posterior compartments of the lower leg are most often involved. Sensation in the distal portion of the extremity may be altered, but this is not a consistent finding. Distal arterial pulses are always normal.24
Although most patients presented with activity-related pain, some complained mainly of ankle weakness at fatigue. The effort needed to produce pain may be quite consistent for one patient, and yet differ greatly for another. Swelling during exercise of a runner's already hypertrophied muscles may produce prolonged muscle ischaemia in the affected compartment. It is also conceivable that the muscular swelling could stretch the compartment fascia and stimulate its contained sensory receptors to provoke pain. Displacement or mild pressure on inflamed compartment structures, e.g. tendons, muscle origins or periosteum, could also produce pain following exercise-induced muscle swelling. Hence, leg pain caused by these other conditions could present with similar symptoms and signs found in compartment syndrome, with the exception of the presence of elevated compartment pressure. Muscle hernias were noted in 30% of patients.5,6
Direct intramuscular pressure measurement
The current gold standard for diagnosing compartment syndrome is direct measurement of invasive intramuscular pressure (IMP) and is the primary investigation used to decide on whether to proceed with surgical intervention.1 IMP is measured by insertion of a slit catheter or a similar pressuretransducing device directly into the muscle compartment at risk. This technique is usually accurate and reproducible but is invasive, painful and has an infection risk particularly when measurements at multiple locations are required. Both non-invasive ultrasound (NIUS) and IMP measurement are userdependent investigations, where the method in which the test is performed affects the result.1,7
The classic reference for exertional compartment testing can be credited to Pedowitz and colleagues. The normal resting compartment pressure is between 0 and 8 mmHg. Exercise results in an increase in muscle volume of 8-20%, which results in increased pressure. Following exercise, volume and pressure will return to preexercise levels usually within 5 minutes in a normal compartment. The persistence of increased pressure post exercise is felt to be suggestive of CECS and these pressures may remain abnormal for 20 minutes or longer after exercise.1 Pedowitz et al. also provided the definitions of a positive test for exertional compartment syndromes, which have been the reference for over two decades: resting pressures of >15 mmHg, post exertion pressures of >30 mmHg and delayed pressure measurements of >20 mmHg. Most clinicians also base their diagnoses on an increase of >10 mmHg compared to the resting pressure.8
Despite the fact that IMP measurement is the gold standard for diagnosing CECS, a standard reproducible protocol for IMP testing has not been described. This results in confusion regarding interpretation of results and reduces the tests' reliability.1,8 Key questions remain: Should both legs be tested? Should all compartments be routinely tested or only symptomatic compartment? Are resting, immediate post exertion and delayed post exertion tests required? What resting pressure defines true rest; how long does the patient need to abstain from exercise before the test; and could even walking before the examination affect the pressure results?9
Non-invasive estimations of IMP
The use of peripheral pulse oximetry failed to show reliable decreases in haemoglobin oxygen saturation in the onset of increased IMP and inadequate tissue perfusion.10 The use of near infrared spectroscopy (NIRS) to measure tissue ischaemia shows some promise in the diagnosis of CECS. These studies demonstrated a significant inverse correlation between IMP and oxyhaemoglobin level, and a correlation between oxyhaemoglobin level and perfusion pressure. However, NIRS has trouble measuring oxygen saturation in deep muscle compartments, as the infrared signal can only penetrate tissue approximately 2-3 cm deep, and the instrumentation for NIRS is relatively expensive.10,11
In studies of CECS, magnetic resonance imaging (MRI) has shown increased T2 signal intensity with elevated anterior compartment pressures, but inconsistent T1 abnormalities in the setting of increased IMP. However, due to its large size and cost MRI is infrequently used and limited to radiology departments.10,11
Lynch et al used a non-invasive ultrasonic pulsed phase locked loop (PPLL) device to measure sub-micrometer displacements of the fascia wall. The PPLL device is a low power ultrasound instrument designed to detect and continuously monitor very small displacements between the ultrasound transducer on the skin surface and any subdermal tissue that is capable of reflecting the ultrasound pulse. These displacements occur as a result of volume expansion of the muscle compartment and are related to changes in intramuscular pressure (IMP). The initial experiments were conducted on human cadaver legs, with promising results as a low-cost non-invasive, alternative diagnostic modality but transition from laboratory studies to clinical use will require further development.12
Wieman e$ a# used the PPLL in a human subject experiment. When a thigh tourniquet was inflated in a stepwise fashion to increase the IMP pressure the PPLL was able to detect fascial displacement waveforms corresponding to arterial pulsation and furthermore could distinguish between normal and elevated IMP. There was a linear correlation between PPLL measurements and invasive IMP. In this study the PPLL also showed potential as a non-invasive device for the measurement of IMP.10
Garabekyan et al 7 used a next generation digital non-invasive ultrasound device (NIUD), in comparison to the analogue model used by Wieman et al .10 The analogue model provided indirect estimates of fascial displacement through post acquisition correlation analysis. In contrast, the digital model calculates displacement directly, thereby providing an instantaneous assessment of the output of the position of the muscle fascia. They hypothesised that fascial displacement in experimental compartments with impaired perfusion pressure (PP) would be significantly greater than fascial displacements in control compartments with a normal baseline PP. Acute compartment syndrome (ACS) was generated in the anterior compartments of anaesthetised pigs; the contralateral leg was used as control. IMP was monitored in all compartments with slit catheters; the IMP in experimental compartments was elevated by 10 mmHg increments by infusing 0.045% albumin in saline. Their results proved that fascial displacement in experimental compartments with impaired PP was significantly greater than fascial displacement in control compartments with a normal baseline. One limitation of their study was the use of an animal model. They felt that the most important point to be addressed in future studies was whether the relationship between PP and amplitude of fascial displacement is consistent among different limbs, different compartments, different injuries, and in different animal models including humans.7
Non-invasive ultrasound
Ultrasound, a non-invasive instrument, has had wide application in medicine. It also has the ability to exclude other entities that have to be considered in the differential diagnosis of CECS: shin splints, stress fractures, periostitis, popliteal entrapment and claudication. It also excludes haematomas, abscesses, deep venous thromboses, ruptured Baker's cysts and other masses. Other advantages include safety with no radiation, portability, accessibility, high resolution and a relatively lower cost. More importantly it allows dynamic imaging. Additionally, direct imaging correlation with patient symptoms provides important information to the referring clinicians.4,5,11
Gershuni et al 5 and Brahim and Zaccardelli11 were the first to evaluate the anterior muscle compartment with ultrasound following exercise. They measured the depth (anteroposterior dimension) of the anterior compartment of the lower leg of healthy joggers and nonjoggers before and after exercise. The anterior compartment was exercised on an isokinetic exerciser until the subject complained of pain. The average increase in depth was 8.6%, the increase in joggers 10.1% and in nonjoggers 7.4%. They suggested that measuring the depth increase with ultrasound might complement IMP measurements. Gershuni et al stated that a definite relationship exists between pressure and volume within the leg compartments. Hence, changes in initial volume of the muscle compartment relative to the capacity of the osseofascial compartment boundaries will be reflected in IMP changes. In addition fascial compliance and permeability are involved in the pressurevolume relationship. However studies have already proved that little if any, fluid permeates through the osseofascial boundaries, and unless anatomic or adventitious defects in the boundaries are present, an increase of IMP would be expected for each unit of volume increase. The anterior compartment allows for changes in only one direction depth, which is an indicator of volume changes.5,11
Van Holsbeeck et al 2 examined the lower leg compartments of a group of normal young people, normal athletes and athletes with the clinical diagnoses of CECS with ultrasound. The ultrasound probe position was marked on the skin, depending on the compartment that was evaluated; this was done so that all the repeat measurements were taken at the same level. The depth or anteroposterior dimension of the compartment was measured from the outer border of the superficial fascia of the compartment perpendicular to the outer border of the interosseous membrane or bone surface in millimetres. The measurements of the compartment were obtained at rest, immediately following exercise, and after a 10minute rest period. The exercise consisted of plantar and dorsiflexion of the foot with a 4 kg load at a rate of 60 cycles/min; this was performed for 15 minutes or until symptoms forced the patient to stop. IMP measurements were obtained at the same time that the ultrasound measurements were taken; however, the method used was not described. In their study the normal group demonstrated normal IMP measurements and an increase of dimension ranging between 10% and 15%. After the 10minute recovery period the dimensions returned to that of preexercise. The patients with the clinical diagnoses of CECS all showed abnormal IMP measurements. Onethird of these patients did not show any increase in compartment dimension after exercise, but thickening and rigidity of the interosseous membrane were evident. The other twothirds showed a normal increase in dimension of 10%-15%, which was unexpected with the clearly abnormal compartment pressures. However the return to preexercise dimension was delayed up to six times the upper limit of normal.2
The aim of this review was to determine the role of NIUS in the diagnoses of CECS.
Materials and methods
The ultrasound records of 34 patients (23 males) between the ages of 14 and 65 years conducted between 2006 and 2008 with the clinical diagnosis of CECS were studied. These patients were referred to our unit for an ultrasound examination of the symptomatic muscle compartment to exclude other pathology. All the examinations were conducted by the same operator (>10 years musculoskeletal ultrasound experience) on a Toshiba ultrasound machine equipped with a 5-7.5 MHz lineararray transducer using the technique described by Van Holsbeeck et al .2
At the time of examination the patient had to be free of residual pain. After the first measurement (rest/pre-exercise), the patient was instructed to repeat the activity which precipitated the symptoms. Once the pain/symptoms were present, the activity was discontinued and a second measurement (post-exercise) was taken. If the increase in depth dimension was <15%, a third measurement was taken after a 10minute rest period. We accepted the values used by Van Holsbeeck et al ; a postexercise depth dimension increase of <15% was interpreted as normal and the postexercise depth dimension should return to the preexercise dimension after resting for 10 minutes.
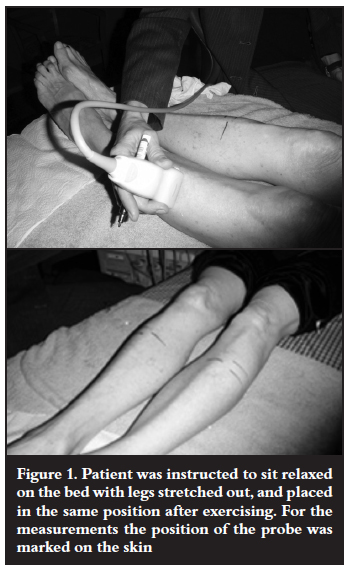
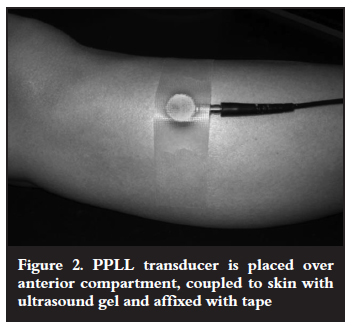
During the examination the patient was instructed to sit relaxed on the bed with legs stretched out, and placed in the same position after exercising (Figure 1). For the measurements the position of the probe was marked on the skin (Figure 2): the probe was placed lightly on the skin without any pressure; each measurement was repeated three times. The depth or anteroposterior dimension of the compartment was measured from the outer border of the superficial fascia of the compartment perpendicular to the outer border of the interosseous membrane or bone surface in millimetres. Only the symptomatic compartment was measured. The examinations were interpreted as positive for CECS if the postexercise depth dimension of the symptomatic compartment increased more than 15% calculated as follows:
post exercise depth (mm) - pre exercise depth (mm)
÷ exerciseivide; pre depth (mm) × 100 =% increase,
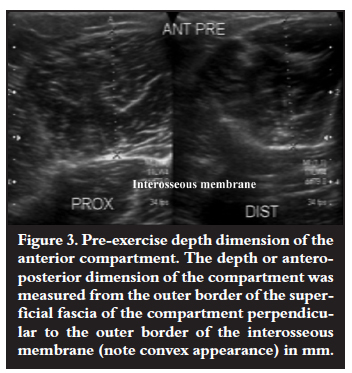
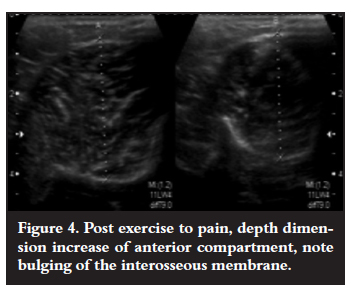
or if the compartment increase post exercise was normal (<15%), and the depth (mm) of the compartment did not return to the pre-exercising measurement after the 10-minute rest period (Figures 3 and 4).
In 2009 all subjects were contacted by telephone with the following questions:
1. What treatment did you receive?
2. Was it successful?
Results
Of the 34 patients assessed, the results of 18 patients (group P) were interpreted as positive for CECS. Thirteen of group P had a postexercise depth dimension increase of >15% (group P1). Four of group P had a postexercise depth dimensions increase of <15% (normal) but the depth dimension of the compartment did not return to the preexercising measurement after the 10minute rest period (group P2). One of group P had a postexercise depth dimension increase of <15% (normal) but several hernias became visible (group P3). Sixteen of the patients' (group N) results were interpreted as negative; the depth dimensions increase post exercise was normal or less than <10% and the depth dimension of the compartment returned to the preexercising measurement after a 10-minute rest period. Thickening or rigidity of the interosseous membrane or fascia was not seen as reported by Van Holsbeeck et al in their study (results given in Table I).
Of the 34 subjects, 25 were contactable for a telephonic interview. Fifteen of the group P patients had surgical release of the symptomatic compartment with success. Three of the group P patients could not be contacted. Ten of the group N patients received conservative treatment with success. Six of the group N patients could not be contacted.
A Fisher's Exact Chisquare test was conducted to examine whether there was a relationship between the 'reality' and the observation by NIUS. It is important to note that three of group P and six of group N could not be contacted. The results revealed that there was a significant relationship between the two variables (pvalue smaller than 0.05, p<0.000) at a 95% level of confidence.
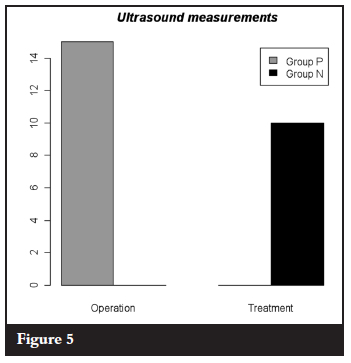
Unfortunately the zeros violated the assumptions of the Chisquare test and the results can only be used as a trend. Group P: 15/18=83.33% had operations with success (correctly classified) three not accounted for. Group N: 10/16 = 62.50% had conservative treatment with success (correctly classified) six not accounted for (Figura 5).
Discussion
Due to an increase in the quest for non-invasive methods to diagnose CECS, we decided to review the ultrasound examinations of cases referred to our practice with a clinical diagnosis of CECS. At present invasive IMP measurement is still considered the gold standard for diagnosing CECS despite the fact that a standard reproducible protocol for IMP measurement has not been described. The non-invasive nature of ultrasound makes it an attractive alternative to direct IMP measurement. It also has the ability to exclude other entities that have to be considered in the differential diagnosis. Other advantages include safety with no radiation, portability, accessibility, high resolution and a relatively lower cost.
Following the ultrasound studies of the lower leg muscle compartments in the early eighties and the method described by Van Holsbeeck et al , there was no further literature published on the use of ultrasound in the evaluation of CECS.
The majority of the early patients were referred to exclude other pathology and not specifically to confirm CECS. The ultrasound examinations reviewed in this study were retrospective and not conducted in a strictly standardised or 'scientific' fashion but they followed closely the described technique of Van Holsbeeck, hence are representative of the clinical situation.
The authors believed it reasonable to deviate from a prescribed exercise protocol as used in previous studies. The production of symptoms varied between individuals, hence it was deemed appropriate to allow each individual to exercise to the point of reproducing the symptoms. The effect of the differences of each exercise regimen may have had an impact but this was not assessed.
That 18 of the 34 patients were shown to be positive for CECS and responded well to surgery is suggestive that ultrasound may be a valuable tool in the diagnosis of this condition. This is further suggested by the outcome of the 16 patients who had a negative test, of whom ten were treated conservatively with good results. The fate of the untraceable patients in this study is not known and problematic.
Although thickening or rigidity of the interosseous membrane or fascia was not seen in this study as reported by Van Holsbeeck et al it is possible that the chronicity of the patients in the study by Van Holsbeeck differed from the patients in our study.
This review of cases has several weaknesses. Being retrospective it was not a welldesigned scientific trial. The clinical history was not documented; only the percentage increase in dimension of the muscle compartment was noted in the report and not the exact measurements; no comparison with normal athletes or nonathletes was made; and there were no controls. With respect to the outcomes, the lack of controls leads to the possibility of false conclusions. The result of the statistical analysis is not of any value due to the fact that 29.4% of patients could not be contacted and treatment received and success thereof is unknown.
Conclusion
At present invasive IMP measurement is still considered the gold standard for diagnosing CECS despite the fact that a standard reproducible protocol for IMP measurement has not been described. The main role of ultrasound in the investigation of patients with the clinical diagnoses of CECS is to exclude other pathology. This retrospective case review shows some promise that ultrasound may be of value as a non-invasive investigation complementing IMP measurement, but prospective controlled trials are needed to evaluate its role in the assessment of CECS.
The content of this article is the sole work of the authors. No benefits of any form have been derived from any commercial party related directly or indirectly to the subject of this article.
References
1. Hislop M, Tierney P. Intracompartmental pressure testing: results of an International survey of current clinical practice, highlighting the need for Standardized protocols. Br J Sports Med 2011;45:956-58. [ Links ]
2. Van Holsbeeck MT, Introcaso JH. Musculoskeletal Ultrasound 2nd ed.2001; 52-56. [ Links ]
3. Wasilewski SA, Asdourian PL. Bilateral chronic exertional compartment syndrome of the forearm. Clin Sports Med. 1992 Jan;11(1):161-88. [ Links ]
4. Gracia Mata S, Hidalgo OA, Martinez GM. Bilateral, chronic exertional compartment syndrome of the forearm in two brothers. Clin J Sport Med. 1999 Apr;9(2):91-99. [ Links ]
5. Gershuni DH, Gosink BB, Hargens AR, et al. Ultrasound Evaluation of the Anterior Musculofascial Compartment of the Leg Following Exercise. Clin Orthop Relat Res. 1982;167:185-90. [ Links ]
6. Martens MA, Backaert M, Vermaut G, Mulier JC. Chronic leg pain in athletes due to a recurrent compartment syndrome. Am J Sport Med.1984;12(2)148-58. [ Links ]
7. Garabekyan T, Murphey GC, Brandon R, et al. New noninvasive ultrasound technique for monitoring perfusion pressure in a porcine model of acute compartment syndrome. J Orthop Trauma.2009;23(3):186-194. [ Links ]
8. Hutchinson M. Chronic exertional compartment syndrome. Br J Sports Med 2011;45:952-53. [ Links ]
9. Hislop M, Batt ME. Chronic exertional compartment syndrome testing: a minimalist approach. Br J Sports Med 2011;45:954-955. [ Links ]
10. Wieman JM, Ueno T, Leek Bt, et al. Noninvasive measurements of intramuscular pressure using pulsed phase-locked loop ultrasound for detecting compartment syndrome: a preliminary report. J Orthop Trauma. 2006;20:458-63. [ Links ]
11. Brahim F, Zaccardelli W. Ultrasound measurement of the anterior leg compartment. Am J Sport Med.1986;14(4)300-302. [ Links ]
12. Lynch JE, Heyman JS, Hargens AR. Ultrasonic device for the noninvasive diagnosis of compartment syndrome. Physiol Meas..2004;25:N1-N8. [ Links ]
 Reprint requests:
Reprint requests:
Dr Z Oschman Jakaranda
Hospital Room 102
Muckleneuk, Pretoria
Tel: (012) 343 5003 Fax: (012) 343 0277
Email: zanet@mweb.co.za














