Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.10 no.4 Centurion ene. 2011
CLINICAL ARTICLE
Autologous intramedullary bone graft harvesting as an alternative to conventional harvesting methods
Francois SprongI; Christian Hugo SnyckersII; Franz Friedrich BirkholtzIII
IMBChB(UP) Senior Registrar. Department of Orthopaedic Surgery, Steve Biko Academic Hospital, University of Pretoria, Pretoria, South Africa
II(MBChB, MMed(Orth)(UP) Consultant. Department of Orthopaedic Surgery, Steve Biko Academic Hospital, University of Pretoria, Pretoria, South Africa
IIIMBChB, MMed(Orth)(UP) Orthopaedic Reconstructive Surgeon. Private Practice, Unitas and Zuid Afrikaans Hospitals, Pretoria, South Africa
ABSTRACT
Conventional bone graft harvesting using the iliac crest is often cited as having significant donor site morbidity and complications. A technique has become available in the form of intramedullary harvesting, using a reamerirrigationaspiration (RIA) system. It is hailed as a safe alternative, with minimal donor site morbidity and pain.
This study presents a retrospective case series of 16 patients where the RIA system was used as a harvesting technique from June 2008 to January 2010. This technique involves harvesting autograft from the femoral canal (anterograde or retrograde) by reaming the intramedullary cavity only once. A single surgeon performed the operations over a 24month period. Fluoroscopy was used to size and measure the width of the canal and to confirm guide wire placement. Outcomes evaluated were postoperative pain perception and patient satisfaction. Bone harvest volumes, intraand postoperative complications and bony union were noted. Telephonic interviews were conducted in all 16 cases.
The average age of the patients was 31 years (15-55 years). The femoral canal was used as the donor site in all the patients. The mean postoperative followup period was 18.8 months (8-27 months). The average amount of bone harvested was 39.6 cc (20-70 cc). Two technical complications were encountered intraoperatively and there were no systemic complications due to reaming. Although
The RIA system was found to be a safe technique, with reliable volumes of autograft obtained. Patients recovered quickly without wound complications and minimal donorsite morbidity. This technique seems to be a viable option as an alternative to conventional bone graft harvesting.
Ethical clearance was obtained from The Research Ethics Committee, Faculty of Health Sciences, University of Pretoria.
Key word: Reamerirrigationaspiration, bone graft harvesting, intramedullary harvesting, RIA, donor site morbidity, donor site complications
INTRODUCTION
Open bone graft harvesting continues to be recognised as the gold standard to obtain an autograft in patients needing additional bone for various reasons.1,2 Patients suffer from significant donor site morbidity following open graft techniques.312
Bone grafting is a standard orthopaedic procedure. Donor bone is usually harvested from the iliac crest. The intramedullary femoral canal can also be used as a donor site. It provides good quantity and quality autograft. To harvest bone from the intramedullary canal a reamerirrigationaspiration (RIA) system (Figure 1) is utilised. The same approach to the intramedullary canal is used as is used in the nailing of femoral fractures. This technique does have its disadvantages in that reaming the intramedullary canal can cause complications such as cortical penetration, iatrogenic fractures and excessive blood loss. The use of fluoroscopy also adds to radiation exposure, not only to the patient, but also to theatre personnel, but this can largely be eliminated.

We propose that bone grafting from this donor area has less donor site morbidity than conventional open bone graft harvesting from the iliac crest and should be made use of much more often.
Although the intramedullary autograft harvesting technique provides one with the same osteoinductive and osteoconductive advantages, no single study could be found reporting primarily on donor site morbidity.
This retrospective review focuses on the postoperative pain and discomfort experienced by the patient at the donor site. Graft volumes obtained during this reaming technique were documented. Progressions to union at the graft site were noted using clinical and radiological assessments although this was not the aim of the study. Not all patients could be followed until bony union occurred.
With permission from both the surgeon and the patient, surgical notes and patient files were examined for data. Graft volume obtained intra-operatively and any intraoperative complications were noted. These volumes could be measured accurately using the calibrated suction canister provided with this system.
Materials and methods
This is a retrospective study from June 2008 to September 2010. All patients who had undergone intramedullary harvesting during this period were reviewed. Twenty patients were treated over this time period by a single surgeon. All nonunions were included. Some of these fractures had multiple previous attempts at union, while other fractures were simply complicated by extensive comminution or severe soft tissue damage. This must be kept in mind when union rates are assessed.
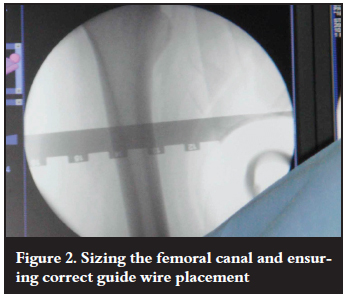
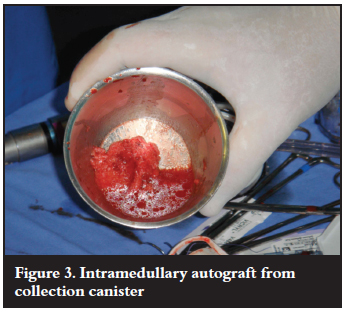
Twenty cases underwent intramedullary bone harvesting using the RIA (Synthes®) system (Figure 1). Four cases were excluded from this study as the indication was to address underlying osteomyelitis. The medullary canal was sized intraoperatively using fluoroscopy (Figure 2). Bone harvesting using a single pass reaming technique was employed in all cases. The bone graft was collected and measured intraoperatively (Figure 3).
The 16 patients included in this study were contacted telephonically following surgery. The final interview was conducted during September 2010. During each interview a questionnaire was completed. Questions regarding pain focused on postoperative pain experienced and pain at the time of the interview. A pain analogue scale ranging from 1-10 (no pain to severe pain) was used to determine a pain score. All complications regarding the donor site were documented and included questions on the following:
• wound breakdown
• any visit to a general practitioner
• any oral antibiotics taken
• aesthetic appearance of the wound
With permission from both the surgeon and the patient, surgical notes and patient files were examined for data. Graft volume obtained intraoperatively and any intraoperative complications were noted. These volumes could be measured accurately using the calibrated suction canister provided with this system.
Results
The 16 patients included four females and 12 males with an average age of 31 years (15-55 years). In all these patients the femur was used as the intramedullary harvest site (retrograde or antegrade). In 13 cases (81%) the tibia served as the graft site. The other three cases included a clavicle nonunion and two non-unions of the femur.
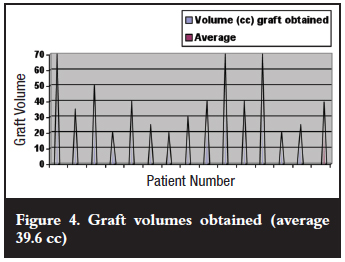
In two cases no documentation of graft volume was available. The average volume of bone harvested was 39.6 cc (20-70 cc) (Figure 4). Two complications occurred during reaming of the canal. In one patient the reamer tip broke off (recovered by guide wire) and in the other case cortical penetration occurred. This patient was treated with protected weight bearing for 6 weeks and recovered uneventfully.
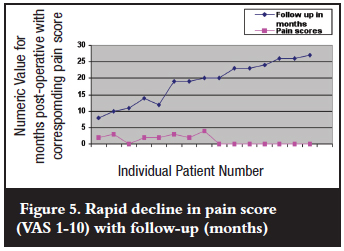
Final followup interviews were conducted during September 2010 establishing an average followup duration of 18.8 months (8-27 months). All patients reported mild to severe pain immediately postop with an average pain score of 6.5 (1-10). Seven patients reported minor pain at the donor site during the last interview. Nine patients had no pain. All patients followed up after 21 months were pain free (Figure 5). No patient reported any complication with regards to the questionnaire on post-operative wound complications.
The incidence of non-union during the study period in the remaining cases can be explained by the complex nature of these injuries. Most of these patients had multiple previous surgical attempts to obtain union. This article focuses on donor site morbidity and not on the time to union. Taking these factors into consideration bony union was still achieved in 56.2% of patients. One patient was lost to long-term followup after an aboveknee amputation at his request.
Discussion
Bone graft donor site morbidity
The osteoinductive and osteoconductive advantages of autogenous bone graft over allograft to ensure bony union of spinal fusions is well known and documented.35 The risks of using allograft include histocompatibility differences, impaired healing, increased risk of infection and transmission of infectious diseases and structural weakness.6 Complications such as haematoma, pain, numbness, limping, scarring, bone contour deficit and irritability of local tissue might necessitate the need for another means of obtaining autogenous bone graft other than from the iliac crest.6,7,12 Less frequent but severe complications of the ilium as donor site include infection, pseudoaneurysm of the pelvic vasculature, urethral injury, nerve injuries (lateral femoral cutaneous or ilioinguinal nerve), peritonitis, herniation and iliac crest fractures.6,8,9 Our aim was to make use of an alternative autograft site that would have the same osteogenic potential as cancellous autograft from the ilium, but without the detrimental side effects of current donor sites.13
A large number of published studies on conventional bone graft harvesting raise concerns about the detrimental sequelae of the procedure.312,1419 The volume of graft taken, the donor site for bone grafting and the method of taking the graft all influence the donor site morbidity.8 Due to its accessibility the iliac crest is the most commonly used graft site.
In a comparative study done by Ahlmann et al The complication rate of posterior iliac crest graft harvesting was found to be less than anterior iliac crest graft harvesting.12 Complication rates following iliac crest bone graft harvesting have been reported to range between 2.8% and 39%.4,10 This wide discrepancy in published figures might be attributed to the difference in analytical methods used.11 Another reason for this large discrepancy may be the fact that the perception of pain is multifactorial, combining mechanical injury with emotional elements.11 Sasso et al confirmed longterm donor site pain at 2 years postoperatively.10 Although harvesting from the proximal tibia was associated with a lower morbidity rate, the amount of graft obtainable is questionable.13
A further study by Sasso et al published data on 202 patients reviewed after undergoing anterior lumbar interbody fusion with bone graft taken from the iliac crest. Only two patients had no donor site pain on discharge from the hospital. After six months 41% of these patients still had donor site pain and this number decreased to an alarming 33% of patients only after 1 year. At the 2year followup review 31% of patients still had pain at their donor site.10
In a retrospective study by Goulet et al reviewing 170 patients who underwent iliac crest grafting, 37.9% of patients still had pain 6 months after surgery at the donor site. This figure declined to 18.3% after two years, indicating a very slow decrease in pain over time.9
Silber et al compiled data from 134 patients retrospectively who underwent anterior iliac crest bone graft harvesting. Difficult ambulation of patients in the acute period (less than 3 months) occurred in 50.7% of patients. The incidence of chronic pain (>3months) at the donor site was 26.1%.4 This study demonstrated significant donor site morbidity even when small amounts of graft were harvested.
Heary et al performed an independent outcome assessment on 105 patients who had iliac crest donor grafts. Sixtysix of these grafts were from the anterior iliac crest, 18 were from posterior and 21 were anteroposterior combined grafts. Independent interviewers determined the incidence in donor site pain to be as high as 34% compared to 8% when the assessment was done by the operating surgeon. This study infers that the incidence of graft harvest site pain may be considerably higher than indicated by the operating surgeon's clinical assessments.11 The same study showed no difference in donor site pain with regards to sex, obesity, site (anterior versus posterior iliac crest) and the volume of graft harvested.11
Of concern is not only the functional outcome of the patient, but also the aesthetic appearance of the wound. In a study published by Sasso et al 16% of patients who had open iliac crest bone harvesting rated their donor site wounds as fair or poor after 2 years.10
With review of the literature it is clear that donor site morbidity is complex in nature and common in prevalence. The discomfort during the postoperative period is substantial and the improvement of symptoms occurs slowly. The surgeon's method of dissection, different approaches to the donor site, the graft volume and even complex emotional patient factors must be considered.11
Effects of intramedullary reaming
Reaming the intramedullary canal is not without complications. First, intramedullary blood supply to the femur is largely destroyed.20,21
CourtBrown refers in his article to the work of Schemitsch et al who showed that cortical revascularisation does occur and takes about 12 weeks.21 In the same article, he mentions that Reichert et al suggest that reaming may actually be beneficial to fracture union by inducing an increase in periosteal blood supply.21 They do not actually show an increase in overall blood supply but postulate that the increase in periosteal supply compensates for the decreased intramedullary circulation.21
Secondly, thermal energy is produced and the risk of thermal necrosis exists. The critical temperature for thermal injury to bone is 56 ºC, but extensive cortical necrosis occurs only at around 70 ºC.20 Although cortical necrosis is often quoted, clinical evidence is rare with only ten cases reported in the literature.20
Thirdly, and probably the most concerning, is fat embolism resulting in fat embolism syndrome and respiratory compromise. The main reason for marrow extravasation is related to the peak pressure generated by the reaming process20,23 and should not exceed 40 mmHg.24
The risk of resultant lung compromise, though, seems to be related to preexisting lung contusion in addition to reaming.20,2325 In a recent review article by Court-Brown21 the conclusion from a number of experimental studies is that reamed intramedullary femoral nailing under most circumstances does not cause significant respiratory compromise. The risk of fat embolisation is further reduced by simultaneous reaming and aspiration, which reduces intramedullary pressure2,25 with resultant decrease in the systemic effects, i.e. lung compromise. Newer reamer designs have also been shown to decrease peak pressures while reaming.23,24
Sarasin referred in his article to the work of Muller et al who showed that a reamer shaft that is narrow and flexible and a head that is hollow with enlarged flutes will also result in lower peak pressures.23 Lastly, reaming should be done with a sharp reamer and a controlled slower rate of reamer advancement down the canal, which will also result in lower pressures.24
When looking at RIA specifically, Belthur et al reported only two reamerspecific complications in their group of 41 RIA harvested patients, namely one with anterior femoral shaft penetration which was managed nonoperatively and one patient who had excessive reaming of the base of the femoral neck as a result of a piriformis entry point. This patient underwent prophylactic femoral neck fixation.2
In a case series reported by Lowe et al, four patients encountered fractures through the donor bone and two patients experienced acute RIAassociated events.26 He concluded that preoperative bone quality evaluation, patient selection and careful fluoroscopicguided reaming may prevent these complications.26
In a cohort study published by Quintero et al, 19 of their 20 patients reported no pain at the entry portal and there were no cases of infection, heterotopic ossification or postoperative antalgic gait due to donor site complications.27 He did, however, warn surgeons to be aware of blood loss from the medullary canal, to prevent unnecessary aspiration while not reaming and to use fluoroscopy to guide and control the reaming process.27 These findings correlate well with a small pilot study done by Newman et al, where they analysed retrospective data of ten patients who underwent RIA bone harvesting. No donor site pain was reported within six weeks of the procedure and the union rate in this series was 90%.28
Finnan et al studied the mechanical effect of reaming the intramedullary canal in 42 cadaveric femurs, using the RIA system to obtain adequate volumes of bone graft. These femurs were subjected to axial and torsional forces after reaming while the contralateral side served as a control. He concluded that intramedullary reaming did not degrade the mechanical behaviour of these femurs, regardless of the reamer entry site.29
The effect of reaming does have benefits. It is a way of autografting aseptic nonunions of tibias and femurs.20,22 Reaming debris is also an excellent source of growth factors and multipotent stem cells, including osteoblasts.1,2,20,30
In a study by Schmidmaier et al on reaming, it was shown to contain higher concentrations of certain growth factors, including BMP2, than pelvic bone grafts.30 Besides the debris as a source of stem cells and growth factors, the reaming process itself has been shown to liberate growth factors within the body, possibly leading to its secondary osteogenic effect.20 The volume of bone graft acquired when using the intramedullary canal as a source is substantial, with the literature reporting 30-90ml.1,26,27 This was validated in a recent study by Belthur et al who reported between 25 ml and 75 ml of bone graft with the use of RIA.2
The effect of intraoperative fluoroscopy
The effect of fluoroscopy intraoperatively on the patient and the surgical team must be taken into consideration when introducing a new method of bone graft harvesting requiring such exposure to radiation. The RIA system will inevitably make use of fluoroscopic control, thereby exposing everybody in theatre to the harmful effects of radiation. These effects have gained increased attention during the past few years. The amount of exposure is determined by a number of factors including the type and difficulty of the procedure, the experience of the surgeon and the radiographer, as well as the protective measures taken.31
Perisinakis et al compared the risk of developing fatal cancer or genetic defects on patients treated for a femoral fracture to that of the normal American population not exposed to irradiation.32 Elderly patients had a risk lower than 1.3 per million for developing fatal cancer and a risk close to zero for genetic birth defects.
By exposing younger patients with fluoroscopic control, this risk increased to 0.4 cases per million with regards to genetic defects and 1.3 cases per million may develop fatal cancer.32 Perisinakis et al also found the age and gender average risk for developing fatal neoplastic disease and for severe hereditary disorders to be 110 per million and 4 per million of patients treated for pedicle screw internal fixation.33 Given the fact that the average risk for spontaneous onset of cancer in the US is 20% (200 000 per million) and the incidence of serious birth defects is 6% (60 000 per million), these figures may be considered acceptable.32,33
Reducing the time of fluoroscopic beam radiation still remains the most effective way to decrease patient exposure.32 The use of pulse fluoroscopy, last image hold and the avoidance of continuous screening together with surgeon and radiographer experience will decrease fluoroscopy time.31 The use of a protective apron and a thyroid shield decreases the effective dose received by theatre staff by a factor of 16.34,35 By ensuring a distance of more than 70 cm from the Xray beam, a significant decrease in radiation exposure was detected.34
Conclusion
Reaming the intramedullary canal to obtain autograft produces good volumes of bone that are rich in bone morphogenetic proteins. Although this procedure is not without complications, adverse events can be prevented by careful patient selection and fluoroscopicguided reaming.
The use of fluoroscopy in theatre is well accepted and commonly practised. Taking the above into account the risks of radiation exposure can never be underestimated. However, current literature supports the fact that with adequate protection, knowledge and understanding of the commonly used Carm, these risks may be very low and do not put the patient at risk of developing fatal cancer or hereditary defects.
No studies specifically focusing on donor site morbidity with regards to the RIA system could be found in our search of the literature.
The results of this study suggest a significant decrease in donor site morbidity. Pain at the donor site area declines rapidly, with most patients not experiencing any pain at the entry site after 21 months.
From the literature it is noted that patients ambulate quickly after surgery, experience less pain at the entry site and are generally more satisfied with the aesthetic appearance of the donor area (Figure 6).
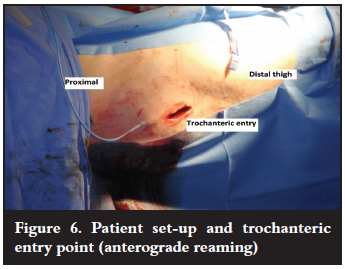
There are some limitations to the study. These include a small sample size, telephonic interviews and subjective quantification of pain. Using this system also adds additional costs, prolonged setup and anaesthetic time to the procedure.
This study shows a significant decrease in donor site morbidity that benefits patients in need of autograft harvesting.
References
1. NicholsTA,SagiHC,WeberTG,GuiotBH.Analternativesourceofautograft bone for spinal fusion: the femur: technical case report. Neurosurgery 2008 discussion E179; Mar;62(3 Suppl 1):E179. [ Links ]
2. Belthur MV, Conway JD, Jindal G, Ranade A, Herzenberg JE. Bone graft harvest using a new intramedullary system. Clin Orthop 2008 Dec;466(12):2973-80. [ Links ]
3. Shamsaldin M, Mouchaty H, Desogus N, Costagliola C, Di Lorenzo N. Evaluation of donor site pain after anterior iliac crest harvesting for cervical fusion: a prospective study on 50 patients. Acta Neurochir (Wien) 2006 discussion 1074; Oct;148(10):1071-74. [ Links ]
4. Silber JS, Anderson DG, Daffner SD, Brislin BT, Leland JM, Hilibrand AS, et al . Donor site morbidity after anterior iliac crest bone harvest for singlelevel anterior cervical discectomy and fusion. Spine 2003 Jan 15;28(2):134-39. [ Links ]
5. Arrington ED, Smith WJ, Chambers HG, Bucknell AL, Davino NA. Complications of iliac crest bone graft harvesting. Clin Orthop 1996 Aug(329):300-309. [ Links ]
6. Schnee CL, Freese A, Weil RJ, Marcotte PJ. Analysis of harvest morbidity and radiographic outcome using autograft for anterior cervical fusion. Spine 1997 Oct 1;22(19):222-227. [ Links ]
7. Colterjohn NR, Bednar DA. Procurement of bone graft from the iliac crest. An operative approach with decreased morbidity. J Bone Joint Surg Am 1997 May;79(5):756-59. [ Links ]
8. Eufinger H, Leppanen H. Iliac crest donor site morbidity following open and closed methods of bone harvest for alveolar cleft osteoplasty. J Craniomaxillofac Surg 2000 Feb;28(1):31-38. [ Links ]
9. Goulet JA, Senunas LE, DeSilva GL, Greenfield ML. Autogenous iliac crest bone graft. Complications and functional assessment. Clin Orthop 1997 Jun(339):76-81. [ Links ]
10. Sasso RC, LeHuec JC, Shaffrey C, Spine Interbody Research G. Iliac crest bone graft donor site pain after anterior lumbar interbody fusion: a prospective patient satisfaction outcome assessment. J Spinal Disord Tech 2005 Feb;18(Suppl):S77-81. [ Links ]
11. Heary RF, Schlenk RP, Sacchieri TA, Barone D, Brotea C. Persistent iliac crest donor site pain: independent outcome assessment. Neurosurgery 2002 discussion 5167; Mar;50(3):510-16. [ Links ]
12. Ahlmann E,MD, Patzakis M,MD, Roidis N,MD, Sheperd L,MD, Holtom P,MD. Comparison of anterior and posterior iliac crest bone grafts in terms of harvestsite morbidity and functional outcomes. Journal of Bone & Joint Surgery-American Volume 2002 May;84A(5):716-19. [ Links ]
13. AltV, NawabA, Seligson D. Bone grafting from the proximal tibia. J Trauma 1999 Sep;47(3):555-57. [ Links ]
14. Banwart JC, Asher MA, Hassanein RS. Iliac crest bone graft harvest donor site morbidity. A statistical evaluation. Spine 1995 May 1;20(9):1055-60. [ Links ]
15. Chen YC, Chen CH, Chen PL, Huang IY, Shen YS, Chen CM. Donor site morbidity after harvesting of proximal tibia bone. Head Neck 2006 Jun;28(6):496-500. [ Links ]
16. FrohbergU,MazockJB.Areview of morbidityassociatedwith boneharvest from the proximal tibial metaphysis. Mund Kiefer Gesichtschir. 2005 Mar;9(2):63-65. [ Links ]
17. Kager AN, Marks M, Bastrom T, Newton PO. Morbidity of iliac crest bone graft harvesting in adolescent deformity surgery. J Pediatr Orthop 2006 Jan-Feb;26(1):132-34. [ Links ]
18. Pollock R,Alcelik I, Bhatia C, Chuter G, Lingutla K, Budithi C, et al . Donor site morbidity following iliac crest bone harvesting for cervical fusion: a comparison between minimally invasive and open techniques. Eur Spine J 2008 Jun;17(6):845-52. [ Links ]
19. Rawashdeh MA. Morbidity of iliac crest donor site following open bone harvesting in cleft lip and palate patients. Int.J.Oral Maxillofac.Surg. 2008 Mar;37(3):223-27. [ Links ]
20. Pape HC,MD, Giannoudis P,MD. The biological and physiological effects of intramedullary reaming. Journal of Bone & Joint Surgery - British Volume 2007 Nov;89B(11):1421-26. [ Links ]
21. Court-Brown CM. The management of femoral and tibial diaphyseal fractures. J R Coll Surg Edinb 1998 Dec;43:374-80. [ Links ]
22. Kanakaris NK, Paliobeis C, Nlanidakis N, Giannoudis PV. Biological enhancement of tibial diaphyseal aseptic nonunions: the efficacy of autologous bone grafting, BMPs and reaming byproducts.[erratum appears in Injury. 2007 Oct;38(10):1224]. Injury 2007 May;38(Suppl 2):S65-75. [ Links ]
23. Sarasin SM, Vannet NB. A comparison of pressures created by various commonly used intramedullary reamers. The Internet Journal of Orthopaedic Surgery 2007;7(2). [ Links ]
24. Smith PN, Perriman D, Sample RR, Gissane J, Li RW.A method of monitoring and controlling intramedullary pressure increase during long bone instramentation. Injury 2007 Jan;38:422-26. [ Links ]
25. Pape HC, Zelle BA, Hildebrand F, Giannoudis PV, Krettek C, van Griensven M. Reamed femoral nailing in sheep: does irrigation and aspiration of intramedullary contents alter the systemic response? J Bone Joint Surg Am 2005 Nov;87(11):2515-22. [ Links ]
26. Lowe JA, Della Rocca GJ, MurthaY, Liporace FA, Stover MD, Nork SE, et al . Complications associated with negative pressure reaming for harvesting autologous bone graft: a case series. J Orthop Trauma 2010 Jan;24(1):46-52. [ Links ]
27. QuinteroAJ, Tarkin IS, Pape HC.Technical tricks when using the reamer irrigator aspirator technique for autologous bone graft harvesting. J Orthop Trauma 2010 Jan;24(1):42-45. [ Links ]
28. Newman JT, Stahel PF, Smith WR, Resende GV, Hak DJ, Morgan SJ.A new minimally invasive technique for large volume bone graft harvest for treatment of fracture nonunions. Orthopedics 2008 Mar;31(3):257-61. [ Links ]
29. Finnan RP, Prayson MJ, Goswami T, Miller D. Use of the reamerirrigatoraspirator for bone graft harvest: a mechanical comparison of three starting points in cadaveric femurs. J Orthop Trauma 2010 Jan;24(1):3641. [ Links ]
30. Schmidmaier G, Herrmann S, Green J, Weber T, Scharfenberger A, Haas NP, et al . Quantitative assessment of growth factors in reaming aspirate, iliac crest, and platelet preparation. Bone 2006 Nov;39(5):1156-63. [ Links ]
31. Botchu R, Ravikumar K. Radiation exposure from fluoroscopy during fixation of hip fracture and fracture of ankle: Effect of surgical experience. Indian J Orthop Oct-Dec 2008; 42(4):47173. [ Links ]
32. Perisinakis K, Damilakis J, Theocharopoulos N, Papadokostakis G, Hadjipavlou A, Gourtsoyiannis N. Patient Effective dose and radiogenic risks from fluoroscopically assisted surgical reconstruction of femoral fractures. Radiation Protection Dosimetry 2004;108(1):6572. [ Links ]
33. Perisinakis K,TheocharopoulosN, Damilakis J, Katonis P, PapadokostakisG, Hadjipavlou A, et al . Estimation of patient dose and associated radiogenic risks from fluoroscopically guided pedicle screw insertion. Spine 2004 Jul 15;29(14):1555-60. [ Links ]
34. Mehlman CT, DiPasquale TG. Radiation exposure to the orthopaedic surgical team during fluoroscopy: 'How far away is far enough?' J Orthop Trauma 1997 Aug;11(6):392-98. [ Links ]
35. Theocharopoulos N, Perisinakis K, Damilakis J, Papadokostakis G, Hadjipavlou A, Gourtsoyiannis N. Occupational exposure from common fluoroscopic projections used in orthopaedic surgery. J Bone Joint Surg Am 2003 Sep;85A(9):1698-703. [ Links ]
 Reprint requests:
Reprint requests:
Dr Francois Sprong
Phone: (+27) 12 333 1654 Fax: (+27) 86 505 3594
Email: fsprong@telkomsa.net














