Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.10 no.4 Centurion ene. 2011
CLINICAL ARTICLE
Proximal thoracic spine fractures: a dangerous blind spot
D HugoI; RN DunnII
IDr. MBChB(US), MPhil(Sports Med)(UCT) Registrar, Department of Orthopaedics, University of Stellenbosch
IIProf MBChB(UCT), FCS(SA)Orth, MMed(Orth) Associate Professor and Head of Spinal Services: Groote Schuur Hospital, Division of Orthopaedic Surgery, University of Cape Town, South Africa
ABSTRACT
INTRODUCTION: The proximal thoracic spine is difficult to visualise on X-ray investigation with up to 22% of proximal fractures being missed. This is a major concern, especially in environments such as South Africa where trauma is endemic.
AIM: To review the challenges of diagnosis and management in patients with proximal thoracic fractures.
METHODS: Thirty-three patients with proximal thoracic fractures in the T1-T4 area managed in a spinal unit were identified. There were 21 males and 12 females with a median age of 31.8 years.
A retrospective review of medical records and radiology was undertaken.
Demographic data, mechanism of injury, diagnostic modalities, diagnostic delay, fracture characteristics, neurological status, associated injuries, hospital stay, management, complications and outcomes were recorded.
RESULTS: The aetiology was 21 MVA passengers, eight drivers, one pedestrian, one assault, one bicycle and one hangglider accident. Eight had a one-day diagnostic delay, two between 2 to 5 days and five greater than 2 weeks. The fractures were A1 in seven, A3 in 14, B1 in seven, C1 in two and C2 in two. Twenty-three patients had neurological compromise, 13 being complete. Twentythree had associated chest and head injuries.
Hospital stay was a mean of 27 days (max of 246). ICU median was 14 (max of 115) days.
Twenty-six patients underwent surgery, posterior instrumented fusion being the commonest procedure.
Although the surgery did not change the median kyphosis (25º pre-op to 20º at 1 year and 21º at 2 years), most kyphotic patients were improved (55º to 45º).
CONCLUSION: Proximal thoracic fractures are most commonly encountered following motor vehicle accidents. There is a risk of delayed diagnosis due to poor visualisation with X-ray investigation. There is a high risk of associated spinal cord injury, chest, limb and abdomino-pelvic injuries that result in prolonged hospital stay. These fractures can be managed successfully by posterior pedicle screw fixation and fusion, only if unstable.
A high index of suspicion for proximal thoracic fractures should be maintained in all patients involved in high impact accidents and with chest injuries, and CT should be employed if X-rays are unclear.
Key words: Thoracic, spine, trauma, fracture, delay
INTRODUCTION
South Africa has a high trauma load. In March 2008 The official South African Road Traffic Report reported 11 577 fatal crashes for the preceding 12 months.1 Six to 30% of trauma patients will have vertebral injuries.24 Clinical assessment and decision-making are heavily influenced by the number and severity of the injuries and also by patient co-operation.
The upper thoracic spine is difficult to visualise with plain X-rays.5,6 Van Beek et al reported missed upper T-spine fractures in 22% of injured patients in their series.7 A high index of suspicion is required to avoid any delay in the diagnosis of potentially unstable upper thoracic spine fractures. Singh et al 5 showed a significant association of cervical and lumbar spine fractures as well as rib fractures with thoracic spine fractures.
Objectives
The aim of the study was to review the challenges of diagnosis and management in patients with proximal thoracic fractures (T1-T4).
Methods
Patients were identified by a search of a prospectively maintained database of the Acute Spinal Cord Injury (ASCI) Unit (2003-2010). Patients with minor fractures (spinous process, transverse process of facet joint fractures) were excluded.
Thirty-three patients who had sustained fractures of the T1-T4 vertebral area were identified. The median age at the time of the accidents was 31.8 (17 - 88 ± 16.1) years and the gender distribution was 21 males and 12 females.
Case notes and imaging were reviewed. Demographic data, mechanism of injury, diagnostic modality, diagnostic delay, fracture characteristics, neurological status, associated injuries, hospital stay, imaging, management, complications and general outcomes were recorded.
Microsoft Excel was used for the tables and graphs of the initial data analysis. Statistical software was used for statistical analysis with paired Student-T for evaluation of continuous data and Fisher exact for categorical data.
Ethical approval was obtained from the Institutional Ethics committee (032/2011).
Results
The most common mechanism of injury was motor vehicle accidents (MVA) accounting for 30 cases (21 passengers, eight drivers, one pedestrian). Other aetiologies included assault, a bicycle and a hang glider accident. Seatbelt use was recorded in only 14 of the MVA cases. Of these 12 were not wearing a seatbelt.
There was a diagnostic delay of more than 2 days in 18% of cases with a median of 18 (5-39) days. In 18 cases the fracture was identified on the same day as the hospital admission (0 days delay).
Eight cases had a delay of 1 day but were artifactual due to overnight admission. A delay of 2 days was present in one case and more than 5 days in six cases. Of the six cases with delays of more than 5 days, two had closed head injuries and the other four were treated in secondary facilities with one being discharged initially.
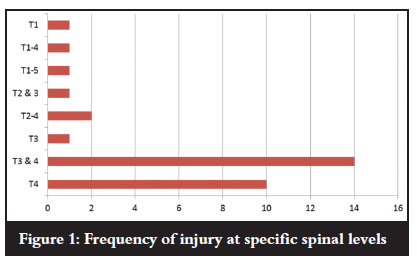
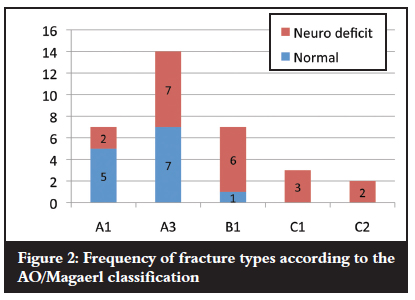
Twenty-one cases had multi-level contiguous fractures and nine had multi-level non-contiguous fractures. The most frequently injured level was when both T3 and T4 were fractures (14 cases), followed by T4 alone in ten cases (Figure 1). In terms of the AO classification, there were seven type A1, 14 type A3, seven type B1, three type C1 and two type C2 injuries (Figure 2).
There were six associated head injuries, 13 chest trauma, 11 limb fractures and three abdomino-pelvic injuries.
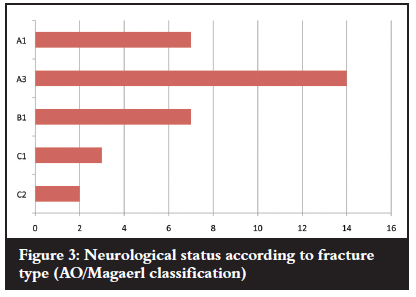
Nine cases were neurologically normal and 24 cases had neurological impairment. Four of the impaired cases were due to the associated cervical spine injury (Figure 3 and 4).
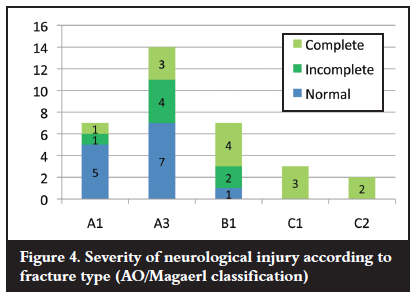
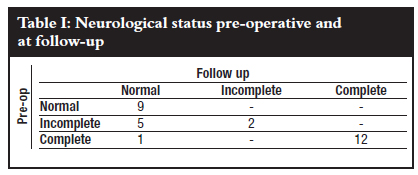
At follow-up (6-60 months) all of the nine neurologically normal cases remained intact; of the seven cases with incomplete injuries five improved to normal (71%) and two remained incomplete. Of the 13 cases with complete injuries, 12 remained complete and one improved to normal (7%) (Table I).
Twenty-six cases underwent surgery with the remainder managed with bed rest and bracing. Posterior pedicle screw constructs and allograft bone graft were used with a median surgical time of 105 (60 - 270 ± 64) minutes and median blood loss of 400 (150 - 2200 ± 514) ml. An additional corpectomy was performed in one incomplete neurologically impaired patient with an A3 fracture and residual compression.
All 26 surgically treated cases showed fusion at 1 year as assessed on X-ray. This was based on the presence of the bone graft and no sign of failure of instrumentation, i.e. peri-screw lucency or instrumentation breakage.
One case required revision for a misplaced pedicle screw. He developed superficial wound infection which was successfully treated with oral antibiotics. Five patients developed decubitus ulcers as a consequence of their spinal cord injury and suboptimal early care before referral. Six developed pneumonia.
Overall there was modest correction of kyphosis from 25º (3º - 55º ± 11.5º) to 21º (5º - 45º ± 9.5º) at one year. The most severe case improved from 55º to 45º.
Table II demonstrates the pre-operative and postoperative kyphotic angles in the operative and nonoperative groups. The surgical group was more kyphotic pre-operatively with a modest improvement. The nonoperative group was less kyphotic and progressed but remained clinically acceptable.
The overall median length of hospital stay was 27 (7 - 246 ± 41.3) days and intensive care unit (ICU) stay was 14 (0 - 115 ± 20.5) days. The comparison of cases with isolated spinal injuries and those with multiple injuries is reflected in Table II. The total ICU days of the isolated injury group comprised 23% (0 - 67 ± 25.9) of their overall length of stay whereas the polyinjured group spent 49% (0 - 68 ± 21.2) of their overall stay in ICU (p = 0.03) (Table III).
Discussion
The rib cage provides increased stability in flexionextension and lateral bending to the thoracic spine. Rotation, on the other hand, is relatively more than in the lumbar spine due mostly to the orientation of the facet joints.810 The thoracic spine is unique due to the fact that it is the only vertebral segment that displays a kyphotic curve. It is also the area of the spine where the spinal canal is relatively narrow compared to the diameter of the spinal cord. The spinal cord occupies 50% in the thoracic area, but only 35% in the cervical spine.9,11 The upper thoracic spine forms part of the 'thoracic cage' and stability is provided by the articulating ribs, sternum and costovertebral ligaments. Thus high energy impact is needed to cause injury to the thoracic spine, resulting in a high incidence of associated chest and cervical and lumbar spine injuries.3,5,11
Bohlman highlighted three important factors that influence injury patterns in thoracic spine trauma, viz. stiffness of this area of the spine requires considerable forces to cause injury; the relatively narrow spinal canal predisposes to cord injuries and thirdly, most injuries are caused by flexion and axial loading due to the rib cage allowing very little rotatory motion in this area.11-13
With the high energy trauma needed to cause upper thoracic injuries it is not surprising that these injuries are most commonly associated with traffic accidents (MVA, PVA, motorcycle/bicycle).24,11 Our group showed 31 of 33 cases injured in traffic accidents, which correlates with other similar studies. Quinlan et al 11 showed 29 of 32 patients who underwent surgery for upper thoracic spine fractures (T1-T6) were involved in traffic accidents. In only 14 of our cases was the use of a seatbelt noted. Of these, two patients had been wearing seatbelts at the time of the accident. The seatbelt as a fulcrum was considered a possible aetiology of the proximal thoracic fracture, but this is unlikely due to the above.
High velocity injuries are associated with polytrauma and patients with upper thoracic spinal fractures have up to 80% incidence of concomitant injuries.5 Singh et al 5 reported cervical and lumbar spine, sternal, clavicular, scapular, lung and rib injuries to be significantly more common in patients with thoracic spine fractures. Quinlan et a' had 20of32 patients with associated injuries in addition to upper thoracic spine fractures (15 chest injuries, 11 sternumrib complex injuries and nine extra spinal fractures).11 In our series, 23 patients had associated injuries, viz. 13 chest, six head, 11 limb, three abdomino-pelvic injuries. Singh et al , in contrast, reported a negative association of lower limb fractures with thoracic spine fractures. In our group only two patients had associated sternum fractures. Some authors feel that the sternum can be regarded as a 'fourth column' of the upper thoracic spine and fractures of the sternum and the upper thoracic spine should be regarded as one entity, which they describe as 'upper transthoracic cage' injuries. Injuries of the 'upper transthoracic cage' indicate a high energy mechanism of injury.5,14 Fracture dislocation of the manubriosternal joint and burst fractures of fracture dislocations of the T4 vertebra are strongly associated with severe trauma and spinal cord injuries.5,15
Our study shows the most common injury involves contiguous fractures of T3 and T4 vertebrae (14 of 33) with an additional ten patients suffering isolated T4 fractures. T4 was involved in a total of 28 fractures when the other contiguous injuries are included (Figure 1). The burst type (AO type A3) was the most common (14 of 33) in our study which correlates with Quinlan's series (20 of 32).11
The thoracic spine is prone to spinal cord injury.9,11,12,16,17 In our study 60% of cases had neurological impairment purely due to thoracic spine injury. The tendency was towards increased incidence of neurological impairment with increasing fracture severity as classified by the AO classification. The incidence of complete neurological lesions also tends to increase with increasing fracture severity. Quinlan's series had 23 of 32 (72%) patients with complete neurological lesions with no improvement in any patient with a complete lesion.11 Our series had 13 of 29 (44%) cases with complete lesions and one improved to normal.
There is consensus in the literature that thoracic spine fractures, especially in the upper thoracic spine, are notoriously difficult to assess. This is attributed mainly to the fact that the upper thoracic spine is difficult to image properly with X-rays and that plain chest films are not adequate to evaluate this area. The other main contributing factor is the fact that most of these patients have multiple injuries that often distract clinicians from the spine and also lead to poor patient cooperation.5,6,11,18 In six of our cases (18%) the diagnosis of a thoracic spine fracture was missed initially and the median delay was 18 days.
Of the six cases, two had closed head injuries leading to prolonged depressed level of consciousness. All 33 patients had the diagnosis confirmed and delineated by computed tomography (CT), magnetic resonance imaging (MRI) or both (11 CT, 15 MRI, seven both). The seven patients with incomplete neurological lesions had an MRI done. Detailed imaging (CT, MRI) has become invaluable as a diagnostic tool as well as for pre-operative planning. Only MRI allows proper visualisation of neurological structures (cord, nerve roots).6,11,12
Early recognition and management of these fractures are essential to the patient outcome and Cotton et al 2 show that less severely injured patients with high thoracic (T1-T6) spinal cord injuries have a significantly higher risk of developing pneumonia and mortality than lower spinal cord injuries. This is further compounded by the associated lung injuries of upper T-spine injuries.
Classically the treatment of upper thoracic spine fractures consisted of prolonged recumbence due to the difficulties of surgical stabilisation and the ineffectiveness of bracing. Frangen et al 2 show that early operative treatment (<72h after injury) of T-spine fractures is not only safe in severely injured patients but significantly reduces intensive care and hospital stay. The cost of the respiratory complications of spinal injuries is often far greater than the primary injury due to prolonged ventilation and ICU stay.19 Early stabilisation in especially T-spine fractures allows early mobilisation and more effective chest physiotherapy and vastly reduces respiratory complications.20
In our series seven patients were treated with bed rest until pain free and then mobilised. None of the seven patients had unstable vertebral fractures or neurological compromise. None of our patients was treated with bracing for thoracic spine fractures. Although bracing is described as a modality of treatment for upper thoracic spine fractures, splinting in this area is already present in the form of an intact rib cage and sternum. An effective orthosis for T1-T4 fractures has to include the cervical spine (cervicothoracic or cervicothoraciclumbosacral orthosis). Bracing over bony prominences, injured, burned or insensate skin is problematic. Constant readjustment of the fit of the orthosis is often necessary.21
The surgical treatment of thoracic spine fractures previously included mainly the use of wires and hooks but recently transpedicular fixation techniques have been proven to be a safe, reliable modality of posterior spinal fixation. It provides rigid, three-column stabilisation with reported.11,13,18,22 good longterm results In their study Marré et al used the following absolute indications for surgery: neurological impairment; mechanical instability (posterior structure disruption, rotational instability); and specific deformities (kyphosis >25º, anterior vertebral wedging >50% and canal narrowing >50%). Relative indications for surgery are to allow early mobilisation out of bed and to aid rehabilitation.11,18 There is increasing recognition of the sternum as the fourth column.
If fractured, or if a sternomanubrium dislocation is present, there may be further consideration to instrument the spine due to the implied high energy injury.
In our series 26 patients underwent surgery. The indication for surgery in all of them was mechanical instability and to allow early mobilisation and rehabilitation. Posterior pedicle screw fixation was performed in all cases. Although our results show only modest kyphotic correction in most cases, there was virtually no loss of correction. At 1-year follow-up a 100% union was attained with no instrumentation failure. We accept that X-ray assessment of fusion, especially in this region, is suboptimal in terms of assessing bone formation. We used coned lateral views at follow-up to improve visualisation but still largely relied on implied fusion by no sign of instrumentation failure such as peri-screw lucency. In the Quinlan e$ a# series 29 (91%) patients had posterior fixation and three (9%) had anterolateral fixation via thoracotomy. They reported no hardware failure and one case of wound abscess treated successfully with incision and drainage.11 Yue et al published a 3year follow-up of 32 patients who underwent posterior pedicle screw fixation for thoracic spine fractures (T2-L1) and reported good to excellent results for all patients and no difference when comparing the outcome of different spinal segments (T1-T4, T5-T9, T10-L1).23 Marré et al 18 reported on 51 patients with thoracic spine fractures (T2-T10) who underwent posterior fixation either with pedicle screw fixation or a combination of laminar/pedicular hooks or claws proximal and pedicle screws distal. Of the 51 patients ten had fractures involving one or more of the first four thoracic vertebrae and only three were fixated using pedicle screws; in the other seven mixed constructs were used.
The most common general complications in our group were pneumonia in six cases (18%) and pressure sores in five cases (15%). All of these complications occurred in patients with neurological compromise. Cotton et al 3 show that patients with high thoracic spinal cord injuries (SCI) have a higher risk of respiratory complications (pneumonia, atelectasis, vventilator-dependent respiratory failure) than lower thoracic and thoracolumbar SCI and similar to that of cervical SCI. Of 231 patients with high thoracic SCI, 29 (12.6%) developed pneumonia.
Croce et al 24 looked at patients with spinal fractures who had early surgical intervention (<72 h) compared to those who had late surgical intervention (>72 h). When looking at thoracic spine fractures specifically, the mean total hospital days, ICU days and ventilated days for the early surgery group were 13.0, 7.0 and 1.2 respectively and for the late surgical group 30.3, 15.1 and 7.6 days (p-values <0.001). In contrast Frangen et al 2 published a similar study that showed no difference between the early and late surgery groups as a whole: in the early surgical group (<72 h) the median total hospital days, ICU days and ventilated days were 28, 2 and 0 days and in the late surgical group 24, 1 and 0 days.
They did, however, show significantly reduced ICU days and hospital days in the early surgery group for the most severely injured patients (Injury Severity Score > 38).
In our study there was no difference in total hospital days when comparing patients with isolated injuries to those with multiple injuries but the multiple injury group had significantly more days in ICU and ventilated days.
Conclusion
Proximal thoracic fractures are most commonly encountered following motor vehicle accidents. There is a risk of delayed diagnosis due to poor visualisation with X-ray investigation.
There is a high risk of associated spinal cord injury, chest, limb and abdomino-pelvic injuries that result in prolonged hospital stay.
These fractures can be managed successfully by posterior pedicle screw fixation and fusion, only if unstable.
A high index of suspicion for proximal thoracic fractures should be maintained in all patients involved in high impact accidents and with chest injuries, and CT employed if X-rays are unclear or a widened mediastinum present.
No benefits of any form have been received from a commercial party related directly or indirectly to the sunject of this article. The content of this article is the sole work of the authors.
References
1. Road Traffic Management Corperation. Road Traffic Report - March 2008. 2008. Ref Type: Report [ Links ]
2. Frangen TM, Ruppert S, Muhr G, Schinkel C. The beneficial effects of early stabilization of thoracic spine fractures depend on trauma severity. J Trauma 2010;68(5):1208-12. [ Links ]
3. Cotton BA, Pryor JP, Chinwalla I, Wiebe DJ, Reilly PM, Schwab CW. Respiratory complications and mortality risk associated with thoracic spine injury. J Trauma 2005;59(6):1400-407. [ Links ]
4. Dai L. Thoracic spine fractures. Chin Med Sci J 2001;16(4):227-30. [ Links ]
5. Singh R, McD TD, D'Souza D, Gorelik A, Page P, Phal P. Injuries significantly associated with thoracic spine fractures: a casecontrol study. Emerg Med Australas 2009;21(5):419-23. [ Links ]
6. Meyer S. Thoracic spine trauma. Semin Roentgenol 1992;27(4):254-61. [ Links ]
7. van Beek EJ, Been HD, Ponsen KK, Maas M. Upper thoracic spinal fractures in trauma patients - a diagnostic pitfall. Injury 2000;31(4):219-23. [ Links ]
8. Andriacchi T, Schultz A, Belytschko T, Galante J. A model for studies of mechanical interactions between the human spine and rib cage. J Biomech 1974;7(6):497-507. [ Links ]
9. el Khoury GY, Whitten CG. Trauma to the upper thoracic spine: anatomy, biomechanics, and unique imaging features. AJR Am J Roentgenol 1993;160(1):95-102. [ Links ]
10. Whitesides TE, Jr. Traumatic kyphosis of the thoracolumbar spine. Clin Orthop Relat Res 1977;128:78-92. [ Links ]
11. Quinlan JF, Harty JA, O'Byrne JM. The need for multidisciplinary management of patients with upper thoracic spine fractures caused by highvelocity impact: a review of 32 surgically stabilised cases. J Orthop Surg (Hong Kong ) 2005;13(1):34-39. [ Links ]
12. Bohlman HH, Freehafer A, Dejak J. The results of treatment of acute injuries of the upper thoracic spine with paralysis. J Bone Joint Surg Am 1985;67(3):360-69. [ Links ]
13. Bohlman HH. Treatment of fractures and dislocations of the thoracic and lumbar spine. J Bone Joint Surg Am 1985; 67(1):165-169. [ Links ]
14. Berg EE. The sternalrib complex. A possible fourth column in thoracic spine fractures. Spine (Phila Pa 1976) 1993;18(13):1916-19. [ Links ]
15. Gopalakrishnan KC, el Masri WS. Fractures of the sternum associated with spinal injury. J Bone Joint Surg Br 1986;68(2):178-81. [ Links ]
16. Dommisse GF. The blood supply of the spinal cord. A critical vascular zone in spinal surgery. J Bone Joint Surg Br 1974;56(2):225-35. [ Links ]
17. Bolesta MJ, Bohlman HH. Mediastinal widening associated with fractures of the upper thoracic spine. J Bone Joint Surg Am 1991;73(3):447-50. [ Links ]
18. Marré B, Ballesteros V, Martinez C, Zamorano JJ, Ilabaca F, Munjin M et al . Thoracic spine fractures: injury profile and outcomes of a surgically treated cohort. Eur Spine J 2011. [ Links ]
19. Winslow C, Bode RK, Felton D, Chen D, Meyer PR, Jr. Impact of respiratory complications on length of stay and hospital costs in acute cervical spine injury. Chest 2002;121(5):154-854. [ Links ]
20. Croce MA, Bee TK, Pritchard E, Miller PR, Fabian TC. Does optimal timing for spine fracture fixation exist? Ann Surg 2001;233(6):851-58. [ Links ]
21. Vialle LR, Vialle E. Thoracic spine fractures. Injury 2005;36 Suppl 2:B65-B72. [ Links ]
22. Fisher C, Singh S, Boyd M, Kingwell S, Kwon B, Li MJ et al . Clinical and radiographic outcomes of pedicle screw fixation for upper thoracic spine (T1-5) fractures: a retrospective cohort study of 27 cases. J Neurosurg Spine 2009;10(3):207-13. [ Links ]
23. Yue JJ, Sossan A, Selgrath C, Deutsch LS, Wilkens K, Testaiuti M et al . The treatment of unstable thoracic spine fractures with transpedicular screw instrumentation: a 3-year consecutive series. Spine (Phila Pa 1976) 2002;27(24):278-287. [ Links ]
24. Croce MA, Bee TK, Pritchard E, Miller PR, Fabian TC. Does optimal timing for spine fracture fixation exist? Ann Surg 2001;233(6):851-58. [ Links ]
 Reprint requests:
Reprint requests:
Prof RN Dunn
Email: info@spinesurgery.co.za














