Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SA Orthopaedic Journal
versão On-line ISSN 2309-8309
versão impressa ISSN 1681-150X
SA orthop. j. vol.10 no.4 Centurion Jan. 2011
CLINICAL ARTICLE
Pyogenic osteomyelitis of the forearm bones in children
MN Rasool
FCS(Ortho)SA, Consultant Paediatric Orthopaedic Surgeon, Department of Orthopaedic Surgery, Nelson R Mandela School of Medicine, Durban, South Africa
ABSTRACT
Twelve children, aged 1-10 years at presentation, diagnosed with pyogenic osteomyelitis of the forearm bones, were reviewed retrospectively. The radius was involved in six patients, the ulna in five and both bones in one child. Three children had acute osteomyelitis; the remaining nine had features of chronic osteomyelitis. The acute infections had incision and drainage and healed well. In six patients with chronic osteomyelitis treatment involved curettage, debridement and sequestrectomy, with resulting bone defects. Three children with chronic infection were referred with established defects from outlying hospitals. Corticocancellous iliac bone chips were used in defects <2 cm in two children; and in two children with larger defects (6-8 cm), segmented bicortical iliac bone graft was used over a K wire. Two children with distal ulna resorption had radioulnar synostosis. Two children had radial club hand deformity with loss of the radial shaft. One had transposition of the residual metaphysis of the radius to the distal ulna, and the other had transposition of the carpus to the ulna. The remaining child had shortening of the radius following multifocal osteomyelitis in infancy. All reconstructive procedures healed by 3 months. All children had improved function. Shortening of the forearm ranged from 2-20 cm.
Key words: Osteomyelitis, forearm bones, radial club hand, radio-ulnar synostosis
INTRODUCTION
The radius and ulna are rare sites for haematogenous osteomyelitis in children (<3%).14 The infection usually involves the metaphyses and can destroy the whole bone. In infants, the forearm involvement may be a manifestation of a multifocal infection. The acute infection presents with fever, pain, swelling, pseudoparalysis and occasionally, a compartment syndrome. Although cure rates have improved due to early detection and improved antibiotics, the diagnosis is not always obvious and may be delayed. Chronicity may occur resulting in a pathological fracture, sequestrum formation, discharging sinuses and pseudarthrosis.
Weakness of grip, shortening and a cosmetic deformity are complications which occur later due to continuing growth of the intact bone. Osteomyelitis of the radius with a large defect can result in overgrowth of the ulna resulting in dislocation of the distal radioulnar joint, radial deviation of the hand and weakness of grip. Radial club hand type of deformity may occur with extensive defects. Defects of the ulna shaft can result in curvature of the intact radius and consequent dislocation of the radial head resulting in instability of the elbow and a cosmetic deformity.5,6
Various methods have been used to reconstruct the forearm. These include cancellous bone grafting4,7 and strut grafts for shaft defects,810 radioulnar synostosis for larger defects with joint involvement515 and carpal transposition to the ulna for radial club hand type deformity.16 Vascularised bone grafting and lengthening techniques have also been used.1720 The aim of this paper is to highlight the sequelae of osteomyelitis of the forearm bones and the treatment methods used to reconstruct the defects. This is mainly a descriptive account of the experience with pyogenic osteomyelitis of the radius and ulna.
Materials and methods
Twelve children, aged 1-10 years of age at first presentation, were reviewed retrospectively between 1999 and 2010 at a local hospital (Table I). Two infants were younger than a year at the time of primary infection. Three children presented acutely (<4 days), one with infection of the proximal and two, the distal radius. The remaining nine children were seen later, after two weeks, with established signs of chronic infection. The majority were boys and the dominant side was involved in seven patients. Staphylococcus aureus was confirmed on pus swabs as the causative organism in all patients.
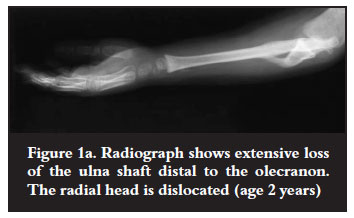
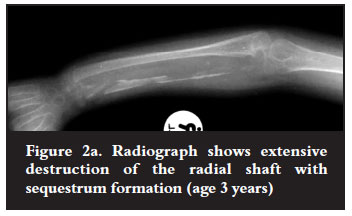
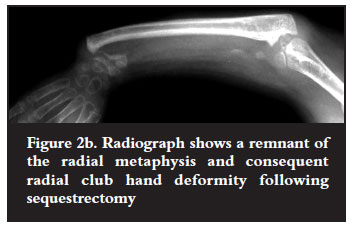
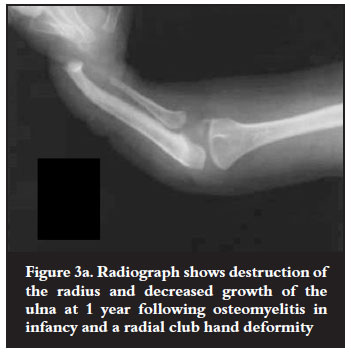
The radius was involved in six children and the ulna in five. One child had both bones involved. In the patients with chronic osteomyelitis, gap defects with sequestra were seen in two patients and two others had large sequestra with bone defects of 6-8 cm. Destruction of the entire ulna distal to the olecranon was seen in two patients: one presented with an established deficiency and the other with a large sequestrum and sinuses. These two patients also had radial head dislocation (Figure 1a). Destruction of the radial shaft was seen in one patient. The metaphysis remained intact and he presented with a radial clubhandlike deformity (Figures 2a and 2b). Another child with a similar deformity had infection in the neonatal period and presented with a stunted ulna and a small proximal radius with marked shortening (Figure 3a). There was a history of drip infiltration, followed by incision and drainage in infancy. The remaining child presented with a short radius. He had a history of incision and drainage of the femur and tibia treated in infancy.
Treatment
The three patients with acute osteomyelitis underwent early incision and drainage (Table I). One had proximal radial involvement and required fasciotomy of the forearm for early compartment syndrome. He required skin grafting and healed. The remaining two had distal radial involvement and pus was found deep to the pronator quadratus muscle at surgical exploration. Both patients improved.
Reviewing the nine patients with chronic osteomyelitis, one child with multifocal bone involvement in infancy had decreased growth of the radial shaft resulting in 4 cm shortening of the forearm and radial deviation of the wrist. Regarding the remaining eight patients, two children had established bone defects, and six underwent surgery with debridement of granulation tissue, sequestrectomy and curettage of the bone ends. Three had insertion of antibiotic beads in the bone defect following sequestrectomy.
Reconstruction was performed when the infection healed.
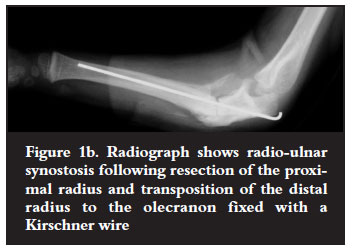
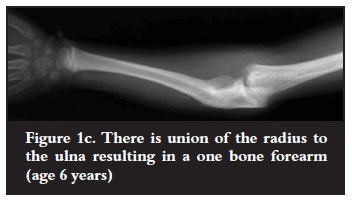
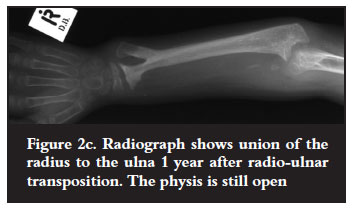
Two patients with gap defects <2 cm had grafting with corticocancellous chips. Two with defects of 6-8 cm, had segmented bone grafts 1.5 × 2 cm, threaded over a Kirschner (K) wire and fixed through the shaft of the ulna. All grafts were taken from the iliac crest. The two children with resorption of the ulna distal to the olecranon had transposition of the radial shaft to the proximal ulna through a defect in the interosseous membrane to create a onebone forearm. A 2 mm K wire was used to transfix the cut ends (Figures 1b and 1c).
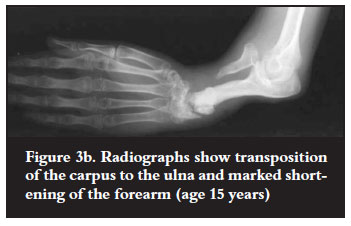
The resected proximal radius was used as bone graft around the synostosis site, following its subperiosteal removal. One child with the radial club hand deformity had transference of the radial metaphysis to the distal ulna following resection of the styloid (Figure 2c) and the other had transfer of the whole carpus to the distal ulna (Figure 3b). Both were fixed with K wires. The wrist was kept in a neutral position in all transfers.
Results
All three patients with acute pyogenic osteomyelitis of The radius healed well without radiological defects following incision and drainage (Table I). Corticocancellous iliac bone chips used for shaft defects <2 cm in two patients incorporated well with good forearm function. Two children with bicortical iliac crest segments over a K wire showed good union by six weeks when the K wires were removed. One patient was lost to followup after 12 weeks. The two patients who had transposition of the distal radial shaft to the proximal ulna developed a good radioulnar synostosis. The wires were removed at 8 weeks. There was a residual elbow flexion contracture of 20º in one patient. One child with radial metaphyseal transfer to the ulna for radial club hand had a stable wrist after 6 weeks and at 1 year the physis remained open (Figure 2c). The other patient with radial club hand deformity, had shortening of 20 cm due to growth arrest of the radius and ulna in infancy. The wrist was stable following carpal transposition to the ulna. The metacarpophalangeal joints remained stiff. However, mobility of the interphalangeal joints and thumb resulted in a weak but useful grip (Figure 3b). The children with radioulnar transposition and radiocarpal transfer compensated for loss of elbow rotation with adequate rotation of the shoulder joint. One child with multifocal osteomyelitis in infancy had a shortened radius (4 cm) at followup, with a prominent ulna styloid and radial deviation of the carpus. He had adequate wrist function and grip and did not want further treatment. Followup ranged from 4 months to 14 years. Shortening was between 2 cm and 20 cm in eight children.
Discussion
Primary haematogenous osteomyelitis in growing bone is still a major challenge despite advancements in treatment. Involvement of the radius and ulna is rare and constitutes less than 3% of all acute osteomyelitis.14 The diagnosis may be missed for more common conditions such as trauma around the metaphyses, or pulled elbow.21,22 Children may present with a pseudoparalysis of the upper limb or rarely with compartment syndrome of the forearm, as seen in this study, and others.23 Although the acute form is commonly primary haematogenous in form, osteomyelitis following forearm fracture,2426 child abuse,27 animal bites28 and venous cannulation30 has been reported. Occasionally the forearm infection may be part of a multifocal sepsis and may manifest later with a cosmetic deformity due to growth disturbance.31,32
The acute infection is commonly due to Staphylococcus aureus and starts in the metaphysis of the radius or the ulna. Pus may be located deep to muscle as seen in cases 2 and 3. Primary epiphyseal involvement has also been reported.33 Periosteal stripping and thrombosis of the nutrient vessels result in bone destruction and pus formation. In the chronic stage, osteomyelitis of the ulna or radius may be associated with pathological fracture, sequestrum formation, cavities and sinuses. Bone deficiency may occur following resorption, extrusion of sequestra or following surgical removal.
The bone defects may be small or extensive. Longterm effects occur with growth arrest and deforming forces, resulting in cosmetic deformity. Unequal growth results in joint instability at either end.4,5 When the defect in the radius is large, relative overgrowth of the ulna results in subluxation of the distal radioulnar joint and radial deviation of the hand. The ulna may angulate with growth, resulting in an acquired radial club hand deformity. Deficiency of the proximal radius results in a cubitus valgus deformity and curvature of the ulna.
Defects in the ulna mainly occur distal to the olecranon. The proximal interosseous membrane and annular ligament may become deficient following bone infection.34 As radial growth continues, discrepancy between the radius and the ulna results in a cubitus varus deformity, lateral curvature of the radius and a shortened forearm. Ulna deviation occurs at the wrist. The stability provided by the ulna at the elbow and at the wrist by the radius is lost and stress is transmitted from the radius to the ulna. Unimpaired radial growth results in dislocation of the radial head. Posterior interosseous palsy may result.34 Scar tissue with tethering on the ulna side also contributes to the bowed radius resulting in distal inclination of the articular surface.
The treatment of the bone defects following pyogenic osteomyelitis is challenging. Primary diaphysectomy was a favoured operation as a lifesaving or curative procedure prior to antibiotics. However, most surgeons opposed it because of the complex reconstructive problems which followed failure of bone regeneration.7,16 Emphasis was placed on suturing the periosteum and preserving its continuity after diaphysectomy.35 Although the diaphysis reformed in some cases, the procedure had unpredictable results.7 Bosworth found that regeneration was more likely to occur in children under 6 years.36 Most surgeons wait for demarcation of the sequestrum and involucrum formation before sequestrectomy.7,16
Restoration of bony continuity following pyogenic osteomyelitis of the forearm with defects is difficult. A high rate of complications and low union rates have been reported.37 Various methods have been used. Spontaneous regeneration of segmental gap defects have been reported in osteomyelitis due to compound fractures of the radial shaft.29,35 The authors emphasised the role of osteoprogenitor cells in the inner layer of the periosteal tube in restoring bone continuity. However, in cases seen in this study the periosteal tube was destroyed in the infective process. There was some continuity of periosteum of the ulna which formed a useful bed for incorporation of bone graft.
Grafting of bone defects depends on the length of the defect, quality of the underlying bone, soft tissue cover and the experience of the surgeon. Radical eradication of sequestrum, granulation tissue and residual pus, followed by antibiotic bead insertion in selected cases, is usually the first stage of treatment. This may be repeated in severe cases until a granulating bed with good soft tissue cover is established. Methods used to obtain bone union include cancellous bone, strut grafts from the iliac crest or the tibia, bone segments over a wire, nonvascularised fibular struts, vascularised pedicle grafts, bone transfer and carpal transposition to the ulna.
Small defects <2 cm heal with cancellous chips.7 Morcellised bone grafts have been used with some success.38 These methods rely on creeping substitution. To obtain union Dugdale4 used tibial corticocancellous grafts for interposition of a midsubstance loss of the radius for small defects (± 3.5 cm) and Kirkos, for large defects (15 cm).39 Boyd40 used dual only grafts with disappointing results. Spira successfully managed forearm defects with full thickness iliac grafts maintained over an intramedullary rod.9 Others have used a plate fixation.8,15
Non-vascularised strut grafts are technically much easier. However, they may take many months to incorporate, lose strength and are susceptible to fracture. Free fibular grafts have a high infection rate when used for osteomyelitis (29%-57%).10,41 Resorption of the graft, development of compartment syndrome, nerve damage and muscle tethering have been observed. Donor site morbidity includes valgus tilting of the ankle due to proximal migration of the lateral malleous.41 Segmented bone grafts, ±1.5 × 2cm, threaded over a Kirschner wire were used in this study for defects up to 8 cm with successful incorporation in two cases and small defects <2 cm healed with cancellous chips.
Vascularised grafts become incorporated sooner. They are technically demanding. However, a high thrombosis rate of graft vessels has been reported.18,42 Helm et al 34 had success with reconstruction of the ulna midshaft with vascularised fibula graft in a child aged 5 years. Mattar et al 43 had good results in 12 patients with defects between 6-12 cm. Donor site morbidity was minimal.
When there is massive bone defect associated with loss of the articulating surface, it may be technically impossible to place a graft in such an area to restore a painless and stable forearm with good function. It is in this type of patient that the procedure of performing a onebone forearm is indicated.5,6 Radioulnar transposition is an alternative to bone grafting. Loss of rotation of the elbow is compensated for successfully by shoulder rotation. Correction of the deviation of the hand onto a solid forearm gives a much stronger grip. Elbow flexion and wrist movements are not impaired. Longitudinal growth continues and improvement in cosmesis occurs.5,6 The requirements for a radioulnar synostosis are an intact radiocarpal and humeroulnar joints.5 Greenwood11 described successful radioulnar synostosis in a child with osteomyelitis of the distal radius. Since then, several case reports have appeared on the reconstruction of a onebone forearm for large radial or ulna defects.57,1216 Various methods have been used by surgeons to hold the radius to the ulna including catgut sutures, cerclage wires, sidetoside cross union with screws or K wires, plating and intramedullary pinning of both shafts. The procedure works well with distal ulna defects or large proximal radial defects. For large ulna defects with an intact olecranon, the distal radius was transferred to the proximal ulna through a small defect in the interosseous membrane and fixed in neutral rotation with an intramedullary pin through the olecranon into the radius in two patients in this study. The proximal radius was excised subperiosteally and used as graft around the synostosis site with successful union. There was good grip and function of both joints.
When a large part or whole of the radius is absent due to osteomyelitis, a radial clubhandlike deformity occurs. The distal radial metaphysis maybe intact or resorbed, resembling a congenital radial club hand. The forearm is short, the wrist unstable and the hand grip is weak. The ulna styloid is prominent. Treatment of the radial club hand deformity due to osteomyelitis has been described by several authors.4,5,7,1316 Ono et al 13 described nine cases and emphasised the difficulty in treatment. The choice of surgical reconstruction depends on what remains of the diaphysis. When the distal radius is absent, centralisation of the carpus on the remaining ulna is recommended.16 One case in this study required this procedure. Haque16 resected the proximal carpal row to centralise the distal ulna to the remaining carpus. If the distal radial epiphysis is intact and a large radial defect is present, then construction of the single bone forearm transposing the distal radial metaphysis onto the ulna following resection of the styloid is the option of treatment, as in case 5. Vascular problems may occur.5
The circular external fixation apparatus with its ability to correct deformity, gain length and transport bone, maybe a useful adjunct in treating radial club hand deformity.13 The Wagner device and monolateral frames have also been used. However, complications with these devices occur, including nerve palsies, sympathetic dystrophy, malunion, refractures, loss of motion and infection.13 The procedures require expertise, meticulous pin care and good underlying bone. Zhang et al 19 reported good results in defects between 3 and 8 cm in 13 patients with intact radial growth plates and metaphyses by callus distraction. The distal radial metaphysis was osteotomised and distracted after correcting the radial deviation first using a monoplane frame. Repeat grafting was required in three patients.
Growth plate arrest due to sepsis remains a difficult problem.20,31 Neonatal sepsis occurring in the forearm bones with septic arthritis is rare.32,44 The type of physeal bar that results from adjacent infection is very difficult to resect and the early age of such arrest predisposes to major limb length discrepancy. Many of the neonates have more than one site of sepsis.31,32,44 Growth plate arrest of the distal radial physis results in relative overgrowth of the ulna. One case was seen in this series associated with multifocal infection. Infection may damage the growth plate directly or enter the physis through the transphyseal vessels that exist at this age. Ischaemia or direct damage to the growth plate may manifest many years later when the secondary centre of ossification has grown sufficiently to demonstrate a bony tether with the metaphysis.20,44 These growth disturbances and physeal bars may not be clinically evident for several years after the initial infection has been treated usually with several antibiotics in a nursery. It has been recommended that neonates with sepsis of the bone and joint be followed up until maturity.32 Treatment is difficult. Limblengthening techniques may need repetition.
Conclusion
The reconstruction of the forearm bones for defects following pyogenic osteomyelitis can be difficult especially if the articular surfaces and bone ends are resorbed. Small defects of the shaft <2 cm were treated successfully with corticocancellous chips from the iliac crest. Larger defects up to 8 cm healed with iliac crest bicortical segments inter positioned into the defects over a K wire. The wire provides temporary support and the segments increase the surface area for bone healing and incorporation. Transposition of the shaft of the radius to the remnant of the proximal ulna produces a stable forearm in patients with distal ulna deficiency and improves function of the elbow and wrist. The resected proximal radius can be used as bone graft around the synostosis site. Children with deficiency of the distal radius present with a radial club hand deformity. If the remnant of the distal radial metaphysis is present, transfer to the distal ulna is a useful salvage procedure. If metaphyseal and articular deficiency of the radius exists, transposition of the carpus to the ulna produces a stable wrist and improves cosmesis. Children with multifocal osteomyelitis must be followed up for growth defects. They may present later with features of skeletal dysplasia following insults to the growth plates in infancy. Bonelengthening procedures and vascularised grafts are technically demanding and should be undertaken by an expert team when simple methods have failed.
Acknowledgement
I wish to thank Ms Tendani Mercy Raphalalani for typing this manuscript.
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article. The contents of this article is the sole work of the authors.
References
1. Blockey NJ, Watson JT. Acute osteomyelitis in children. J Bone Joint Surg 1970;52B:77-87. [ Links ]
2. Morrey BF, Peterson HA. Hematogenous pyogenic osteomyelitis in children. Orthop Clin North Am. 1975;6:935- 51. [ Links ]
3. Shandling B. Acute haematogenous osteomyelitis. A review of 300 cases. S Afr Med J 1960;34:520-24. [ Links ]
4. Dugdale TW, Pillsbury SL, Cates KL, Ogden JA. Successful autogenous cortico-cancellous grafting of a radial defect complicating acute haematogenous osteomyelitis in an infant. J. Pediatr Orthop 1985;5:479-82. [ Links ]
5. Lowe HG. Radioulnar fusion for defects in the forearm bones. J Bone Joint Surg 1963;45B:351-59. [ Links ]
6. Lloyd-Roberts GC. Treatment of defects in children by establishing cross union with the radius. J Bone Joint Surg 1973;53B:327-30. [ Links ]
7. Griffiths JC. Defects in long bones from severe neglected osteitis. J Bone Joint Surg 1968;50B:813-21. [ Links ]
8. Nicoll EA. The treatment of gaps in long bones by cancellous insert grafts. J Bone Joint Surg 1956;38B:70-82. [ Links ]
9. Spira E. Bridging of bone defects in the forearm with iliac graft combined with intramedullary nailing. J Bone Joint Surg. 1954;36B:642-46. [ Links ]
10. Steinlechner CWB, Mkandawire NC. Non-vascularized fibular transfer in the management of defects of long bones after sequestrectomy in children. J Bone Joint Surg 2005;87B:1259-63. [ Links ]
11. Greenwood HH. Reconstruction of the forearm after loss of the radius. Br J Surg 1932;20:58. [ Links ]
12. Watson-Jones R. Reconstruction of the forearm after loss of the radius. Br J Surg 1934;22:23. [ Links ]
13. Ono CM, Albertson KS, Reinker KA, Lipp EB. Acquired radial club hand deformity due to osteomyelitis. J Pediatr Orthop 1965;15:161-68. [ Links ]
14. Dreyfuss U. Acquired radial club hand. A case report. Hand. 1977;9:268-71. [ Links ]
15. Netrawichien P. Radial clubhand-like deformity resulting from osteomyelitis of the distal radius. J Pediatr Orthop 1995;15:157-60. [ Links ]
16. Haque IU. The production of one-bone forearm as a salvage procedure after hematogenous osteomyelitis. J Bone Joint Surg 1982;64B:454-55. [ Links ]
17. Weiland AJ, Kleinert HE, Kutz JE, Daniel D. Free vascularized bone grafts in surgery of the upper extremity. J Hang Surg 1979;4A:129. [ Links ]
18. Yajima H, Tamai S, Ono H, Kizai K, Yamauchi T. Free vascularized fibular graft in surgery of the upper limb. J Reconstr Microsurg 1999;15:515-21. [ Links ]
19. Zhang X, Duan L, Li Z, Chen X. Callus distraction for the treatment of acquired radial club hand deformity after osteomyelitis. J Bone Joint Surg 2007;89B:1515-18. [ Links ]
20. Price CT, Mills WL. Radial lengthening for septic growth arrest. A case report. J Pediatr Orthop 1983;3:88-91. [ Links ]
21. Fitoussi F, Litzelmann E, Ilharreborde B, Morel E, Mazda K, Pennecot GF. Haematogenous osteomyelitis of the wrist in children. J Pediatr Orthop 2007;27:810-13. [ Links ]
22. Gorman R, Mohammed A. Osteomyelitis of the ulnar head in a presumed "pulled elbow". Emerg Med J 2009;26:463- 64. [ Links ]
23. Lundy DW, Lourie GM, Morrissy RT. Acute compartmental syndrome from haematogenous osteomyelitis of the ulna. Am J Orthop 1998;27:571-73. [ Links ]
24. Canale ST, Puhl J, Watson FM Gillespie R. Acute osteomyelitis following closed fractures Report of three cases. J Bone Joint Surg 1975;57A:415-18. [ Links ]
25. Birch T, Levin T, Glaser JH. Salmonella osteomyelitis complicating an acute fracture. Clin Infect Dis 1994;19:545-46. [ Links ]
26. Veranis N, Laliotis N, Viachos E. Acute osteomyelitis complicating a closed radial fracture in a child. A case report. Acta Orthop Scand 1992;63:341-42. [ Links ]
27. Ribe K, Changsri C. A case of traumatic osteomyelitis in a victim of child abuse. Am J Forensic Med Pathol 2008;29:164-66. [ Links ]
28. Dietlein E, Küpeli K, Rütt J. Osteomyelitis caused by Pasturella multocida following dog bite. Med Klin 1988;83:494-95. [ Links ]
29. Lin HC, Hsu CC. Regeneration of a segmental bone defect after acute osteomyelitis due to an animal bite. Injury 2004;35:1316-18. [ Links ]
30. Straussberg R, Harel L, Bar-sever Z, Amir J. Radial osteomyelitis as a complication of venous cannulation. Arch Dis Child 2001;85:408-10. [ Links ]
31. Bergdahl S, Ekengren K, Eriksson M. Neonatal haematogenous osteomyelitis: risk factors for long term sequelae. J Pediatr Orthop 1985;5:564-68. [ Links ]
32. Peters W, Wing J, Letts M. Long-term effects of neonatal bone and joint infections on adjacent growth plates. J Pediatr Orthop 1992;12:806-10. [ Links ]
33. Maffulli N, Fixen J. Osteomyelitis of the proximal radial epiphysis. Acta Orthop Scand 1990;61:269-70. [ Links ]
34. Helm RH, Pho RWH, Tonkin MA. The sequelae of osteomyelitis of the proximal ulna occurring in early childhood. J Bone Joint Surg 1992;17B:232-34. [ Links ]
35. Varma BP, Srivastava TP. Successful regeneration of large extruded diaphyseal segment of the radius. J Bone Joint Surg 1979;61A:290-92. [ Links ]
36. Bosworth DM, Liebler WA, Nastasi AA, Hamada K. Resection of the tibial shaft for osteomyelitis in children. J Bone Joint Surg 1966;48A:1329-39. [ Links ]
37. Han CS, Wood MB, Bishop AT, Cooney WP. Vascularized bone transfer. J Bone Joint Surg 1992;74A:1441-49. [ Links ]
38. Christian EP, Bosse MJ, Robb G. Reconstruction of large diaphyseal defects, without free fibular transfer. J Bone Joint Surg 1989;71A:994-1004. [ Links ]
39. Kirkos JM, Haritis JH. Reconstructive surgery for a defect in the shaft of the ulna due to osteomyelitis. Acta Orthopaedica Blgica 2009;66:397-401. [ Links ]
40. Boyd BH. The treatment of difficult and unusual nonunions. J Bone Joint Surg 1943;25A:535-52. [ Links ]
41. Jupiter JB, Baer CJ, May JW Jr. The reconstruction of defects of the femoral shaft with vascularised transfer of bone. J Bone Joint Surg 1987;62A:1039-58. [ Links ]
42. Minami A, Kasashima T, Lwasaki N, Koto H, Kaneda K. Vascularized fibular grafts. J Bone Joint Surg 2000;82B:1022-25. [ Links ]
43. Mattar J, Azze RJ, Ferreira MC, Starck R, Canedo AC. Vascularized fibular graft for management of severe osteomyelitis of the upper extremity. Microsurgery 1994;15:22-27. [ Links ]
44. Strong M, Lejman T, Michno P. Septic arthritis of the wrist in infancy. J Pediatr Orthop 1995;15:152-56. [ Links ]
 Reprint requests:
Reprint requests:
Mr MN Rasool
Department of Orthopaedic Surgery Nelson R Mandela School of Medicine
Private Bag 7
4013 Congella South Africa
Tel: 0312604297
Fax: 0312604518
Email: katia@ukzn.ac.za