Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.10 n.2 Centurion Jan. 2011
ARTICLE
Venous thrombotic events in arthroscopic shoulder surgery - a case report and review of the literature
PH LaubscherI; MC FergusonII
IMBChB, MMed(Ortho)Pret, FCS(SA)Ortho
IIMBChB, FCS(SA)Ortho. Orthopaedic Surgeons, Centre for Sports Medicine and Orthopaedics, Rosebank, Gauteng, South Africa
ABSTRACT
The incidence of venous thromboembolism complicating shoulder surgery is low. We present a case of a patient who developed a thrombus in the lower leg and subsequently a pulmonary embolus following an arthroscopic rotator cuff repair. Further investigation revealed a genetic predisposition to venous thromboembolism. A review of the current literature on this topic has revealed very little research related to possible causes or risk factors. It is clear though that prevention by means of a proper patient-screening protocol is essential. Adequate preventative measures need to be taken in high risk cases. Failure to apply an adequate screening protocol can lead to adverse outcomes in patients who undergo arthroscopic shoulder surgery.
Key words: shoulder, arthroscopy, complication, thrombus, prevention
Introduction
Both authors have had patients develop a venous thrombotic event (VTE) after arthroscopic shoulder surgery in recent times. These events were serious and required emergency medical management. In the light of the seriousness of this complication it was decided to investigate our protocols regarding screening and intra-operative techniques. The literature was evaluated for guidelines. The review revealed only a few case reports with no author able to offer any real guidelines regarding possible intra-operative preventable measures. The rate of incidence is remarkably low and would explain the limited literature available. Our case detailed below had a favourable outcome with no long-term complications. This, however, is not always the case.
Case report
Patient RM is a 73-year-old female patient who presented initially in August 2009 with right shoulder pain. Initial history revealed that she had been struggling with right shoulder pain for the previous few years but that it had been getting progressively worse the preceding few months. Symptoms and signs were typical for rotator cuff pathology. A conservative treatment regimen was initiated that included subacromial cortisone infiltrations and physiotherapy concentrating on releasing posterior shoulder capsule stiffness as well as strengthening the scapula stabilisers.
The patient responded poorly to these measures and subsequent high definition small parts ultrasound evaluation of the shoulder revealed a degenerative complete tear of M.supraspinatus with associated degenerative changes in the long head of M.biceps. Arthroscopy of the right shoulder confirmed the ultrasound findings and a successful tenotomy of the biceps tendon was performed as well as a repair of the torn M.supraspinatus tendon. The patient was discharged on day 1 postoperatively without any complications.
The patient returned to her physiotherapist on day 14 post-surgery. During the session the patient complained about a 'feeling of being unwell' that she had noticed the day before. After further enquiry it was determined that the patient had also experienced some degree of shortness of breath and groin discomfort for a few days prior to attending physiotherapy.
Initial examination revealed normal vital signs and no other significant clinical findings. Laboratory tests performed showed a raised D-dimer of 5.53 mg/l and a raised CRP of 143 mg/l. A pulmonary perfusion and ventilation scan was performed. This revealed segmental mismatch in the lingula area of the left lung. The report concluded that there was a 'high probability of pulmonary emboli - mainly the lingula'. A peripheral duplex Doppler confirmed complete occlusion of the right popliteal vein as well as the distal and middle thirds of the right superficial femoral vein. Free-floating non-occlusive thrombi were also noted in the superficial femoral vein. The right common femoral vein and long saphenous vein were patent. The left leg showed no thrombi. No thrombi were noted in the veins of the right upper limb.
The patient was admitted to hospital and treatment was commenced by the physician on call. The patient remained in hospital for eight days. Anticoagulant treatment in the form of Warfarin and enoxaparin (60 mg twice daily) was prescribed. The enoxaparin was stopped when her international normalised ratio (INR) reached the prescribed minimum level. She remained on Warfarin for 12 months.
Investigating the genetic predisposition for thrombus formation in this patient revealed the following: The antinuclear antibodies result as well as the results for tumour markers CA 125 and CEA was negative. The test for factor V Leiden deficiency did, however, reveal genetic autosomal dominant inheritance of the mutation in the R506 gene.
She recovered fully from her shoulder surgery with excellent range of motion. No post-phlebitic syndrome was noted.
Discussion
VTEs associated with arthroscopic shoulder surgery were first reported by Burkhart1 in 1990. A 32-year-old male patient developed a pulmonary embolus due to an upper limb thrombus following arthroscopic shoulder surgery.
The cause was found to be a mediastinal mass (due to Hodgkin's disease) that led to stasis in the upper extremity venous system. In 2003 Polzhofer et al2 also reported on a case of a 48-year-old male patient who developed an upper limb VTE post arthroscopic acromioplasty. The authors speculated that irritation of the subclavian vein by the motorised shaver might have contributed to the development of the thrombus. However, this viewpoint is not supported in the literature by other authors. The real cause is often not determined as Cortes et al3 also showed in their report. Indwelling central catheters and underlying malignancies4 therefore remain the two main mechanical risk factors.
Only 1%-4%5,6 of all reported deep vein thrombi occur in the upper limb regardless of the type of surgery. The reported rate of lower limb deep vein thrombosis after knee surgery alone has been reported at 17.9%.7 To date the largest published study on the rate of incidence was by a group in Italy evaluating the results of questionnaires and operative reports from 59 surgeons. A combined total of 9 385 arthroscopic shoulder procedures8 were evaluated. Of all the cases evaluated only five deep vein thrombi were noted and one pulmonary embolus was reported. The rate of incidence in this study was reported at 0.6/1000 procedures. The study also revealed an average time before clinical presentation of ten days post-surgery.
When their postoperative routines were evaluated 20 surgeons (34%) out of the group of 59 used routine antithrombotic prophylaxis in the postoperative period in all their patients. The other 39 surgeons used antithrombotic prophylaxis only in high-risk patients (female, obese, previous DVT). However, the incidence rate between the two groups did not show a statistically significant difference.
Clinical presentation of upper extremity VTEs can be variable. In general they present early in the postoperative period (2-3 days postoperative) and patients complain of pain and/or swelling in the upper arm. Clinical evaluation can reveal prominent superficial veins on the upper arm or chest and also cyanosis of the hand. Asymptomatic presentation can also occur and a high index of suspicion is therefore necessary.9 The rate of pulmonary embolism from an upper extremity thrombus varies considerably from 2.5% to 36% of cases.10 These events are serious. Hingorani et al pointed out that upper extremity thrombi have a greater incidence of pulmonary embolus and higher mortality rate than when compared with lower extremity VTEs specifically.11
General patient risk factors are therefore the most relevant as these might be the most influential causative factor rather than the procedure itself. A guideline paper on VTE has been published by a panel of experts from the Southern African Society of Thrombosis and Haemostasis.12 The authors underline the importance of considering both patient-related and procedure-related risk factors (Table I).
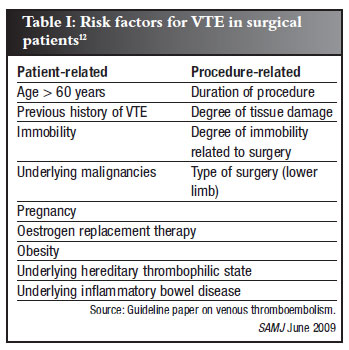
Proper pre-operative evaluation of the patient for possible risk factors will identify patients at risk. Arthroscopic shoulder surgery in itself is a moderate risk factor but in combination with other patient risk factors can create a high-risk environment for the development of a VTE.
A proper screening protocol will therefore have to be based on taking a proper history pertaining to specific risk factors as set out in Table I. In addition to this the attending surgeon should determine the possible length of surgery as well as the use of indwelling vascular catheters. Postoperative ward protocols should also include counselling the patient on symptoms and signs for VTEs and pulmonary embolism. The most appropriate preventative step will be to consider a VTE as a possible complication in arthroscopic shoulder surgery and not only in hip and knee surgery.
Conclusion
It is clear that surgeons performing arthroscopic shoulder surgery also run the risk of their patients developing a VTE (upper or lower limb). The incidence of this happening is, however, not as high as is the case in other orthopaedic-related surgeries. Attending surgeons should assess and examine their patients with as much scrutiny pre-operatively as they would their patients with upcoming knee, hip or spine surgery and should therefore have proper screening protocols in place to identify high-risk patients. A high index of suspicion should also be maintained in the postoperative period. The adverse outcomes following a VTE can be life-threatening and present with very little if any clinical symptoms and signs.
Attending surgeons should assess and examine their patients with as much scrutiny pre-operatively as they would their patients with upcoming knee, hip or spine surgery
Pre-operative assessment of the patient should therefore also investigate the presence of any underlying systemic condition or local anatomic abnormality that can lead to thrombus formation.
References
1. Burkhart SS. Deep venous thrombosis after shoulder arthroscopy. Arthroscopy 1990;6:61-3. [ Links ]
2. Polzhofer GK, Petersen W, Hassenpflug J. Thromboembolic complication after arthroscopic shoulder surgery. Arthroscopy 2003; 19,9:E129-32. [ Links ]
3. Cortes ZE, Hammerman SM, Gartsman GM. Pulmonary embolism after shoulder arthroplasty: Could patient positioning and traction make a difference? J Should Elbow Surg 2007; Vol 16 No 2: e16-e17. [ Links ]
4. Creighton RA, Cole BJ. Upper extremity deep venous thrombosis after shoulder arthroplasty: A case report. J Shoulder Elbow Surg 2007; 16: e20-e22. [ Links ]
5. Prandoni P, Polistena P, Bernardi E et al. Upper-extremity deep vein thrombosis. Curr Opin Pulm Med 1999; 5, 222-9. [ Links ]
6. Horattas MC, Wright DJ, Fenton AH et al. Changing concepts of deep venous thrombosis of the upper extremity: report of a series and review of the literature. Surgery 1988; 104: 561-7. [ Links ]
7. Demers C, Marcoux S, Ginsberg JS et al. Incidence of venographically proved deep vein thrombosis after knee arthroscopy. Arch Intern Med 1998; 158: 47-50. [ Links ]
8. Randelli P, Castagna A, Cabitza F et al. Infectious and thromboembolic complications of arthroscopic shoulder surgery. J Shoulder Elbow Surg 2010;19:97-101. [ Links ]
9. Creighton RA, Cole BJ. Upper extremity deep venous thrombosis after shoulder arthroplasty: A case report. J Shoulder Elbow Surg 2007; 16: e20-e22. [ Links ]
10. Hill SL, Berry RE. Subclavian and axillary vein compression of musculoskeletal origin. Br J Surg 1980; 67: 573-6. [ Links ]
11. Hingorani A, Ascher E, Hanson J et al. Upper Extremity versus lower extremity deep venous thrombosis. Am J Surg 1997; 174:214-7. [ Links ]
12. Jacobson BF, Louw S, Mer M et al. Venous thromboembolism - prophylactic and therapeutic practice guideline. SAMJ June 2009;Vol 99 Nr 6: 467- 473. [ Links ]
 Reprint requests:
Reprint requests:
Dr PH Laubscher
PO Box 413902
Craighall 2024
South Africa
Email: phlaubscher@gmail.com
The content of this article is the sole work of the authors.
No benefits of any form have been derived from any com mercial party related directly or indirectly to the subject of this article. Informed consent was obtained.
Approval by ethical committee: Not applicable














