Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.10 n.2 Centurion Jan. 2011
ARTICLE
Infection following open reduction and internal fixation of an unstable thoracolumbar fracture of the spine the need to know the HIV status of patients - a case report
M Lukhele
Prof. MBChB, FCS(Orth)SA, MMed(Orth) Head of Department, Division of Orthopaedics, University of Witwatersrand
ABSTRACT
The prevalence of HIV-positive patient is high in the sub-Saharan region. This is a report of two unknown asymptomatic HIV carriers presenting with major thoracolumbar fractures for emergency management. The patients' results were complicated by delayed infection. The cases demonstrate the need to know the HIV status in a major orthopaedic trauma setting to enable additional treatment to be implemented that may improve the treatment outcome.
Key words: infection, spine trauma, asymptomatic HIV carrier
Case 1
A 28-year-old male taxi driver fell from the third floor of a building and presented with a painful back. He was generally well. He was tender over the thoracolumbar spine and had no neurological fallout. X-rays and CT scan of the thoracolumbar spine confirmed a flexion distraction injury at L1/L2 (AO type B1). He also had a stable right pubic ramus fracture. Two days later the spine was stabilised with rods and pedicle screws at L1 and L2. A bone graft was inserted between L1 and L2. After surgery he rehabilitated well. He was discharged home nine days post operation, walking independently without any aids. At the six-week follow-up visit, he was well and walking independently, and the wounds had healed with no signs of infection. He did not report for the subsequent scheduled follow up visits.
Four years later he presented with progressive back pain which he had had over the past year. He had recently noticed fluid draining from the operation scar. He looked chronically ill and had generalised lymphadenopathy. He had altered sensation on the left lower limb with weakness of Oxford grade 4 from L2 level on that limb. Blood examinations confirmed him to be HIV positive with a CD4 count of 100 cells/ml and an albumin of 27 gm/l. X-rays showed sclerosis suggestive of chronic osteitis at L1/L2 with loosening and backing out of the pedicle screws (Figure 1). Staphylococcus aureus which was sensitive to cloxacillin was cultured from the draining scar.
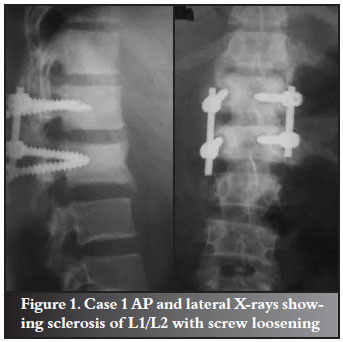
While waiting for removal of implants on an elective theatre list, he lost his bladder and bowel sphincter control. His motor power to the lower limbs deteriorated to Oxford grade 0 on the right and grade 2 on the left.
An urgent MRI showed a collection of pus at the level of L3 compressing the cauda equina (Figure 2). He was taken to the operating theatre as an emergency where all the pus was drained and the spine implants were removed. The fusion at L1/L2 was found to be solid. Post operation he was started on antiretroviral treatment and a high protein diet. The wound continued to drain. He later developed diarrhoea and hypotension. He was managed for septic shock with the assistance of the intensive care physicians but failed to respond and later demised.
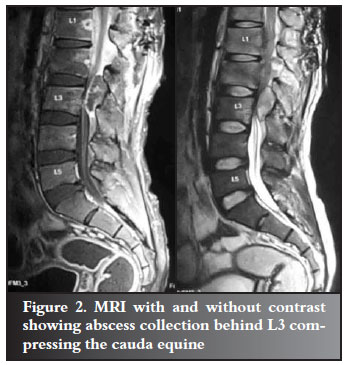
Case 2
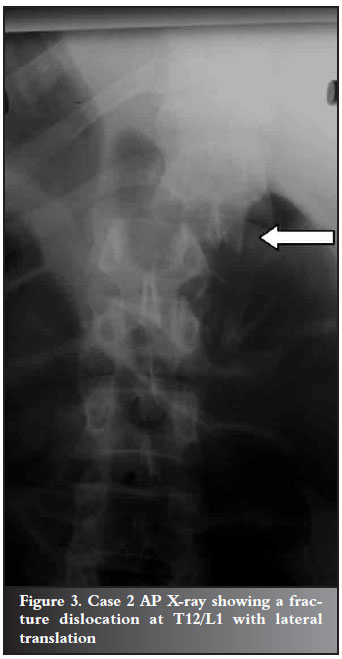
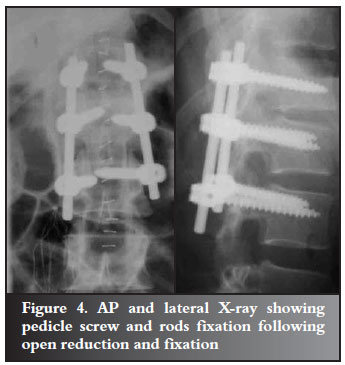
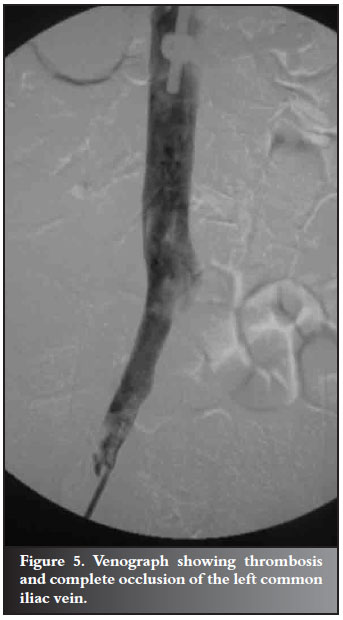
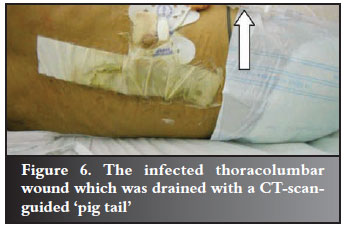
A 44-year-old farm worker overturned a tractor and presented with complete paraplegia from T12. X-rays showed a fracture dislocation at T12 L1 (Figure 3). The fractures were stabilised using posterior instrumentation (Figure 4). Three days later he developed swelling of the left leg. A venogram showed an iliac vein thrombosis (Figure 5). This was managed medically and a filter was inserted in the inferior vena cava. Three weeks later he developed wound sepsis. A CT scan confirmed a big prevertebral abscess around the fracture site. At that stage an HIV test was performed which confirmed that he was HIV positive with a CD4 count of 104 cells/ml and an albumin of 26 grams/l. The abscess was drained using a CT-guided 'pig tail' (Figure 6). He was placed on antiretroviral medications, antibiotics and a high protein diet. The sepsis cleared after 6 weeks.
In the meantime he was rehabilitated for the paraplegia. At last follow-up at 8 months he was mobilising independently on his wheelchair. His CD4 count had improved to 320 cells/ml.
Discussion
Sub-Saharan Africa remains the region most affected by HIV worldwide and an estimated number of 5.7 million of South Africans are living with HIV.1 The South African Department of Health Study conducted in 2009 estimates that 29.4% of pregnant woman were living with HIV.2 The South African National HIV Survey conducted in 2008 found the national prevalence of HIV to be 10.9%.2 This was a population-based study with only 64% of eligible participants agreeing to tests. From these national surveys it can be expected that HIV/Aids is high in patients presenting in emergency trauma settings. At Johannesburg Hospital level 1 trauma unit Bowley et al reported a 30% seroprevalence of HIV in patients being attended for major trauma.3 In our own unit the seroprevalence of patients admitted for orthopaedic trauma was found to be 22% (Dr Sefeane's MMed dissertation).
Patients with HIV/Aids have been shown to have an increased wound infection rate: 3.5% for closed fractures and 11% for open fractures.4 HIV-positive patients have also been reported to present with late infection of implants following elective operation for closed fractures.5 Bahenbeck et al compared the immediate and early outcome of orthopaedic implant surgery in HIV carriers with less than 500 CD4/ml treated with protective antiretroviral and prolonged prophylactic antibiotic therapy in one group (group A), HIV carriers with more than 500 CD4/ml (group B) and non-HIV carriers (group C) treated conventionally.6 In this study they concluded that if prolonged prophylactic antibiotics and systematic antiretroviral therapy are given in HIV immune-depressed carriers, their postoperative infection risk was close to non-HIV carriers.
The current practice in most trauma orthopaedic services is to manage each fracture appropriately on its own merit - meaning that fractures which need stabilisation undergo internal fixation using implants. Before these two cases one did not routinely test for HIV status in patients presenting with thoracolumbar fractures, which may be the case in other centres. In unknown and untreated HIV-positive patients the progressive depletion and dysfunction of the CD4 coupled with defects in macrophages and monocyte function will predispose the patients to infection. If the HIV status of the patient is known, antiretroviral treatment and prolonged prophylactic antibiotics may be administered in addition to the standard management of the fracture and that may prevent wound infection and even deep venous thrombosis which is common in HIV patients.
Recommendation
The author recommends that the HIV status of patients undergoing major orthopaedic trauma procedures should be established before or immediately after the procedure to be able to start early appropriate treatment.
References
1. UNAIDS/WHO. Sub-Sahara latest epidemiological trends 2009 available from: http://www.unaids.org/en/media/unaids/contentassets/dataimport/pub/factsheet/2009/20091124_fs_ssa_en.pdf [ Links ]
2. South Africa HID and AIDS Statistics from: http://www.avert.org/safricastats.htm [ Links ]
3. Bowley DM, Cherry R, Synman T et al. Seroprevalence of human immunodeficiency virus in major trauma patient in Johannesburg. South African Medical Journal 2002 Oct; 92(10):792-93. [ Links ]
4. Harrison WJ, Lewis CP and Levy CB. Wound healing after implant surgery in HIV-positive patients. J Bone Joint Surg Br 2002 Aug;84(6):802-806. [ Links ]
5. Brijlall S, Lioma ID and Govender S. Implant sepsis in the HIV-infected patient. SA Orthopaedic Journal 2003;2(3):26-30. [ Links ]
6. Bahenbeck J, Handy Eone D, Ngo Nonga B et al. Implant orthopaedic surgery in HIV asymptomatic carriers: management and early outcome. Injury, Int J Care Injured 2009;40:1147-50. [ Links ]
 Reprint requests:
Reprint requests:
Prof M Lukhele
Division of Orthopaedics Wits Medical School
7 York Road Parktown
No benefits of any form have been derived by the author from any commercial party related directly or indirectly to the subject of this article














