Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.10 n.1 Centurion Jan. 2011
CLINICAL ARTICLE
Longterm evaluation of polyethylene wear in total hip replacement - a statistical analysis of the association between the degree of wear versus pain, interface change, osteolysis and implant failure
CJ GrobbelaarI; TA Du PlessisII; FE SteffensIII; MJ van der LindeIV
IMBChB, MMed Surg (Orth), MD Orth Professor (extraord) University of Pretoria, Department of Orthopaedic Surgery, University of Pretoria
IIMSc, DSc Gammatron, Pretoria
IIIMSc, DSc, THOD Professor, Department of Statistics, University of Pretoria
IVPhD, Senior research consultant, Department of Statistics, University of Pretoria
ABSTRACT
With over 3.5 decades dedicated exclusively to total joint replacement, our arthroplasty unit has repeatedly identified and reported a clear correlation between cup wear on the one hand, and pain, interface widening and osteolytic failure on the other1. However, in view of the fact that this statement has sparked some controversy, clarification of this correlation became imperative, particularly in view of important clinical consequences.
Materials and methods were provided by a potentially long-lasting gamma crosslinked cup. The arthroplasty follow-up ranged from 10-33 years. Objective clinical, radiographic and pathological evaluations were backed by computer analysis through the Department of Statistics at the University of Pretoria.
We are able to conclude that the statistical correlation between wear, on the one hand, versus pain, interface effects and osteolysis on the other, was no coincidence but instead proved to be clearly conclusive. Of great importance is the fact that this study allowed us to set new objective criteria for true failure as well as impending failure, thus guiding us towards sensible decision-making in terms of revision surgery in these complex issues. Cup wear was thus clearly identified as the overwhelming leading variable in long-term prognosis in this type of total hip replacement.
Introduction
The criteria for revision surgery, due to worn polyethylene hip cups, have long been controversial. Disadvantages of premature revision of a well-performing arthroplasty are obvious, and can only be surpassed by revision performed too late when osteolytic bone damage may already be irreversible. Although over three decades, many surgeons2-5 have identified the relevant variables, wear versus P, I, O (pain, interface changes, osteolysis and revision), we still needed statistical proof of correlation. In this computer-assisted study, these associations have been conclusively verified. It went further to quantify these variables and thus enabled us to be very specific, objective and scientific in decision-making in terms of revision surgery.
To date, traditionally the diagnosis of implant failure essentially depended on the time of implantation to revision surgery. It is our firm belief that failure needs to be identified on a much more sensitive basis and should also include pain, poor function and radiographic issues. Redefinition of failure has thus become imperative (Figure 1).

Materials and methods
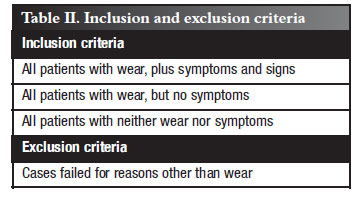
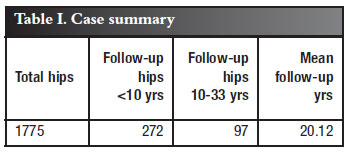
A cohort of 272 total hip arthroplasties was studied. All operations were performed between 1976 and 1983 by the same surgeon. Only patients with a 10 year minimum follow-up were included. There were 97 cases followed over a 10-33 year postoperative period, in this retrospective study. Table I gives the case summary, Table II the inclusion and exclusion criteria, and Table III the demographics. Of particular interest was the relative youth of our patients.

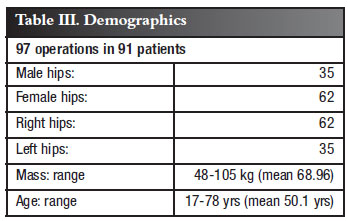
All hips studied utilised a stainless steel monoblock femoral design with a 30 mm head diameter, articulating on a gamma crosslinked ultra high molecular weight polyethylene (UHMWPE) acetabular socket. Clinical follow-up was according to Merle d' Aubigne and Postel6 at 6 months post operation at follow-up 1, when interfaces were considered to have stabilised, and again at their most recent consultation at follow-up 2. Wear measurement at follow-up 2 was according to the Digital Magnification Method (DMM), which became available only in 20027. Earlier measurements were according to a combination of Charnley and Livermore methods, used mainly in followup 1 examinations. Interface widening and osteolysis were measured on the same digital magnified radiographs.
Results an discussion
Compared with the internationally accepted mean wear tempo of virgin polyethylene of 0.1 mm/year8, the results with crosslinked cups in this series was 0.015 mm - a 6.6 times improvement in potential longevity (Table IV).
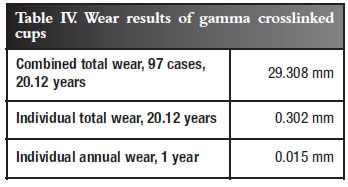
Our study involved four important aspects of cemented arthroplasty follow-up as shown in Table V.
Of particular importance was osteolysis conforming to one of the degrees given in Table VI.
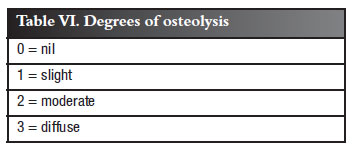
On the basis of these findings, four groups were identified:
Group 1: (7 hips = 7.2%): True failures due to wear
The average total wear over 20.12 years in this group was 1.586 mm (study average was 0.302 mm). Average pain was mode 4 (n=6) and average acetabular interface was 2 mm (n<1 mm). Osteolysis was classified as degree 3 (n=0). Clearly every value proved to be in the 'true failure' range. Consequently seven of the 97 cases had to be revised, and they represented the only wear-related revision operations in the study ('true wear-related revisions').
Group 2: (9 hips = 9.2%): Impending failure
This was a most important and interesting group. Average total wear over 20.12 years was 1.35 mm, which is clearly in excess of the accepted cut-off point of 1 mm. Other variables (dependent) were only moderately raised: pain was 5 M d' A (normal=6), acetabular interface was 1.361 mm (n<1 mm) and osteolysis was degree 2 (n=0).
Revision surgery was not indicated yet; nevertheless the prognosis was poor. All this information was fed into relevant computer programs. Association between wear and the other three variables (P, I, O), again proved convincing with excellent P-values. Perhaps due to especially moderate pain levels, no case in this group reported for revision surgery.
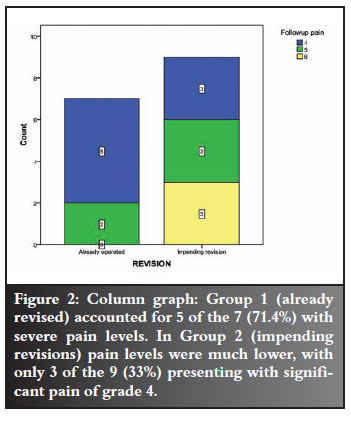
The following statistical figures depicted pain difference between the seven true revisions and the nine impending revisions, and also the effect of wear >1 mm versus <1 mm (Figure 2).
Group 3: (13 hips = 13.4%): Very limite wear
The average total wear in this group was only 0.466 mm, while the average annual wear was 0.019 mm, compared with the series average of 0.015. Dependent variables (P, I, O) also correlated well with only slightly raised values: pain, mode 6 (normal value = 6); acetabular interface 1.15 mm (normal value = 1 mm); and osteolysis amounted to degree mode 0 (normal value < 1). Only routine followup was required in this group.
Group 4: (68 hips = 70.1%): No wear
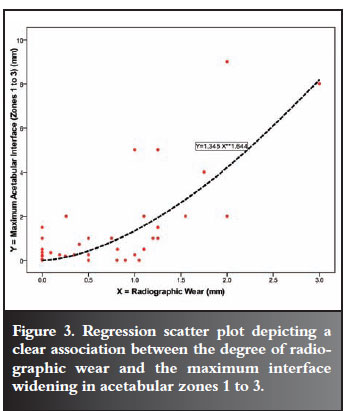
There was no measurable wear in Group 4. In keeping with findings in Groups 1 to 3, there was once again complete association between the independent and dependent variables, i.e. no wear - no pain, no interface widening, no osteolysis (no P, I, O). These findings promised an excellent long-term prognosis. Of particular prognostic value were the 16 cases in Groups 3 and 4 with clear interface improvement, demonstrated in Figure 3 (regression graph) (narrowing).
Examples of statistical analysis
The purpose of this study was to prove the association between wear, as the independent variable, with the three dependent variables P, I, O. For this purpose Least Square Means comparisons, Chi Square Test, Correlation Analysis, Regression, Frequency Procedure and Fisher's Exact Test were considered.
Relationship between radiographic wear and acetabular interface
The following model was fitted to the data by means of non-linear least squares:
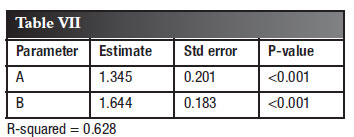
Y=AXB, (which implies a log-log relationship between Y and X), where X = radiological wear and Y = maximum acetabular interface over zones 1 to 3.
The result of the analysis is shown is Table VII. The observed and predicted values are depicted in the scatter plot (Figure 3).
There is a clear association between the degree of radiographic wear and the maximum interface widening in acetabular zones 1-3.
Relationship between degree of radiographic wear and pain
On the basis of the measured radiological wear, patients are divided into two groups: those with wear less than 1 mm and those with wear of 1 mm or more. The pain experienced by the patients was categorised as 4 (severe), 5 (moderate) or 6 (no pain). The relationship between wear and pain is summarised in the cross table shown in Table VIII.
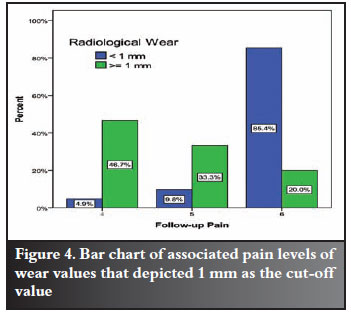
85.4% of patients with less than 1 mm wear had no pain, but of the patients with more than 1 mm wear, 46.7% had severe pain and 33.3% experienced moderate pain.
The relationship was significant, with Fisher's Exact Test yielding a P-value of <0.0001. The bar chart in Figure 4 illustrates the relationship.
Relationship between radiological wear and osteolysis
Osteolysis measurements were categorised into four groups:
0 = nil, 1 = slight, 2 = moderate, 3 = diffuse.
The relationship between radiographic wear and osteolysis is summarised in the cross table in Table IX.
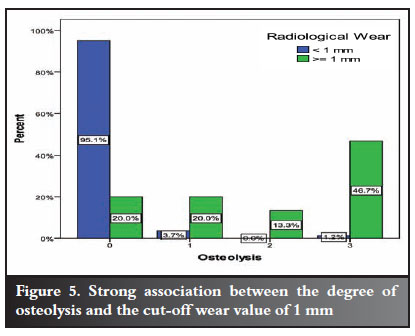
Of the patients with wear less than 1 mm, 95.1% had no osteolysis. Of the patients with wear of 1 mm or more, 46.7% had diffuse osteolysis, and only 20% had no osteolysis. The relationship is statistically significant, the P-value according to Fisher's Exact Test being less than 0.0001. The relationship is depicted in the bar chart in Figure 5.
Relationship between radiographic wear and revision
In terms of revision, patients were classified into four groups:
1 = Already operated
2 = Impending revision
3 = Wear but no impending revision
4 = No wear
The relationship between revision and wear is shown in the cross table in Table X (all 97 cases evaluated).
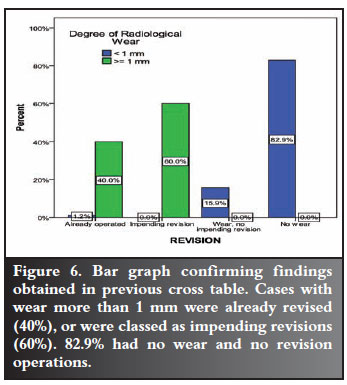
Of the patients with less than 1 mm wear, only 1.2% had already been operated and 15.8% had some wear but no impending revision. Of the patients with wear of 1 mm or more, 40% had already been operated and 60% had impending revision. The relationship is statistically significant (Fisher's Exact Test giving a P-value of less than 0.0001.) The relationship is depicted in the bar chart in Figure 6.
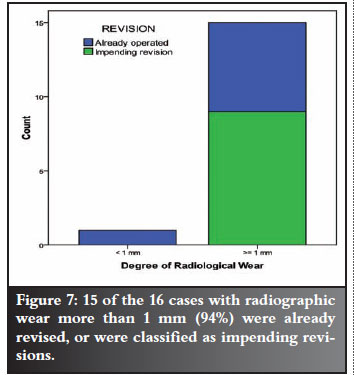
Analysis of all 16 cases with measurable wear is shown in Figure 7.
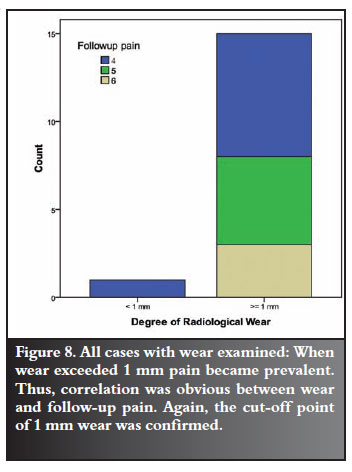
A strong association also existed between the degree of wear and pain in the 16-case cohort with radiographic wear (Figure 8).
Conclusion
This study was directed primarily towards statistical proof in favour of a strong association between cup wear on the one hand, and pain, interface changes and osteolysis (P, I, O) on the other. In our experience with hip replacement over three decades, we have regularly observed these associations. The literature however, is divided on this issue. Wroblewski12 was unable to prove clear correlation between cup wear and particularly osteolysis, and favoured the view of mechanical impingement resulting in looseness of the implant. Other important world leaders in total joint replacement like W. Harris2, Ian Clarke9, Revell11 or Hans Willert10 were individually convinced that at least some of these associations existed. However, the literature still needed positive statistical proof in an ultra-long-term follow-up study. This evidence was successfully provided by our Department of Statistics at the University of Pretoria as summarised in Figure 9.
In this study we have proposed cup wear as the main dependent variable, recorded on the y-axis of column graphs and scatter plots. On the x-axis the three relevant independent variables are represented, namely, pain, interface changes and osteolysis. An exceptionally high level of association was found with p-values as low as 0.0001. According to Fisher's Exact Test, R-Squared equalled 0.628 or better. The association thus proved to be no coincidence, and the null hypothesis could be rejected with confidence.
Finally
The findings reported in this study revealed a new perspective in polyethylene-on-metal total hip replacement. By using computerised calculations we have already reported on a method to predict the remaining lifespan of the implant. Now we are enabled to apply set criteria for routine follow-up versus revision surgery (Table XI).
The choice of treatment in cup wear clearly depends on the quantification (degree) of the three categories of dependent variables, viz. pain, interface status and osteolysis (P, I, O). In this respect we hope that we are able to provide irrevocable proof of the all-important associations of these variables to facilitate a more scientific approach towards management of our arthroplasty patients.
References
1. Grobbelaar CJ, Weber FA, Spirakis A, Du Plessis TA, Cappaert GGA, Cakic JN. Clinical experience with gamma crosslinking of polyethylene - a 14 to 20 year follow-up report. S.A. Bone Joint Surg. 1999; 1X3: 140-49. [ Links ]
2. Harris WH. The problem is osteolysis. Clin Orthop Rel Res.1995; 46:311-16. [ Links ]
3. Schmaltzried TP, Callaghan JJ. Wear in total hip and knee replacements. J Bone Joint Surg. 1999; 81A: 115-36. [ Links ]
4. Ingham J, Fisher J. The role of macrophages. J Biomat. 2005; 26:1271-1286. [ Links ]
5. McKellop HA, Campbell P, Harlan Amstutz, et al. Clin Orth Rel Res. 1995; 311:3-20. [ Links ]
6. M d' Aubigne R, Postel M. Functional results of hip arthroplasty with acrylic prosthesis. J Bone Joint Surg Am. 1954; 36:451-475. [ Links ]
7. Grobbelaar CJ. A new method to measure polyethylene cup wear in total hip replacement - a preliminary report. SA Orth J. 2007; 6:18-24. [ Links ]
8. Zhongmin JIN, et al. Tribology of hip joints. J of Biomech Science and Engin. 2006: Vol I:I. [ Links ]
9. McKellop HA, Clarke IC, et al. Wear Characteristics of UHMWPE: A method of accurately measuring low wear rates. J Biomed Mater Res. 1978; 12:895-927. [ Links ]
10. Willert HG, Buchhorn GH. Particle disease due to wear of ultrahigh molecular weight polyethylene. In: Morrey BF, editor. New York, Raven Press. 1993; 87-102. [ Links ]
11. Revell PA. Biological reaction to debris in relation to joint prosthesis. Proc Inst Mech Eng Med. 1997; 211:187-97. [ Links ]
12. Wroblewski BM, Siney BA. Charnley low-frictional torque arthroplasty - follow up 30-40 years. J Bone Joint Surg Br. 2009; 91B: 447-50. [ Links ]
 Reprint requests:
Reprint requests:
Prof CJ Grobbelaar
PO Box 2083
Brooklyn Square
Pretoria 0075
Email: cjgrobbelaar@netactive.co.za
The content of this article is the sole work of the authors. No benefits of any form have been received from a commercial party related directly or indirectly to the subjectof this article. All subjects included in this study providedtheir written informed consent.














