Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.9 no.4 Centurion ene. 2010
CASE REPORT AND REVIEW OF THE LITERATURE
Overlapping pubic symphysis dislocation: a case report and proposal of a classification system
S MaqungoI; I KollerII; S RocheIII
IFCOrtho(SA). Orthopaedic Trauma Service, Department of Orthopaedic Surgery,Groote Schuur Hospital, Cape Town
IIMBChB.Orthopaedic Trauma Service, Department of Orthopaedic Surgery, Groote Schuur Hospital, Cape Town
IIIFCSOrtho(SA).Cape Bone and Joint Centre, Life Orthopaedic Hospital, Pinelands, Cape Town
ABSTRACT
We report on a rare case of pelvic ring injury with an overlapping pubic symphysis dislocation in a patient who was a pedestrian involved in a motor vehicle accident. She sustained a lateral compression pelvic ring injury with an overlapping pubic symphysis dislocation and a mildly displaced zone 2 sacral fracture. She was treated with open reduction and internal fixation of the pubic symphysis and a percutaneously inserted ilio-sacral screw for the sacral fracture. She recovered well and is asymptomatic at 9 months' follow-up. Only one case has been reported previously that was treated in a similar way. We review the literature, offer recommendations on management and propose a classification system for this injury.
Introduction
An overlapping pubic symphysis dislocation (OPSD) is an extremely rare injury that was first described by Eggers in 1952.1 Since then a total of 14 sporadic case reports have appeared in the English literature, with only one having the posterior pelvic ring injury treated simultaneously with surgery. This was reported 19 years ago.2 No classification system has been proposed for this rare injury. We report on one such dislocation, review the available literature on the subject, offer recommendations on management and propose a classification system for these injuries.
Ethics approval has been obtained from our institution and the patient has consented to the study.
Case report
A 22-year-old female ballet dancer was brought into our emergency unit with the history that she was a pedestrian involved in a motor vehicle accident. Her Glasgow Coma Scale was 15/15 and she was haemodynamically stable. Her chest and abdomen examinations were normal. Her left leg was internally rotated but both her legs were lying flat on the stretcher and she had good dorsalis pedis pulses bilaterally. Neurological assessment of the lower limbs was also normal. She was tender over the pubic symphysis and had no bruising around the pelvis. Rectal and vaginal examinations revealed no associated injury. She had no blood at the urethral meatus and a urinary catheter was passed successfully and it drained clear urine.
Antero-posterior (Figure 1) inlet and outlet radiographs of the pelvis revealed an overlapping pubic symphysis dislocation. The left pubic bone was displaced medially and posteriorly behind the right pubic bone but it had not entered the right obturator foramen. A CT scan with 3D reconstruction (Figures 2A & B) confirmed the overlapping symphysis dislocation and also revealed a Denis zone 2 sacral fracture through the foramina (Figure 2C) on the left side that was mildly displaced.
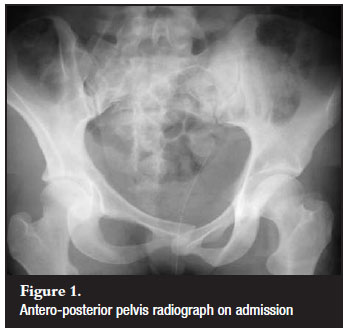
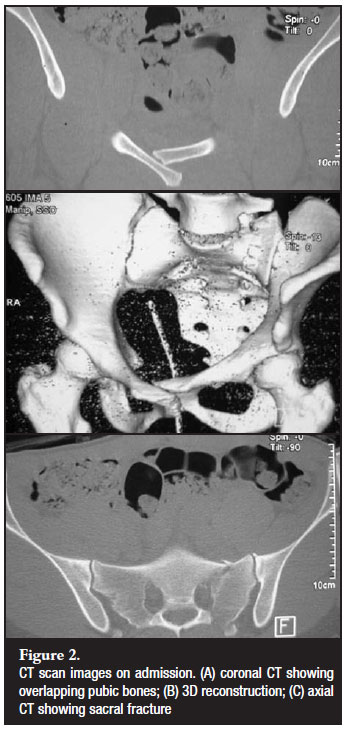
She also had a closed diaphyseal fracture of her right tibia. On the day following her injury her tibia fracture was treated with a locked intramedullary nail. At this stage no attempt at closed reduction of the pelvis was made.
On the third day after the injury she was taken to the operating room for treatment of her pelvic injury under general anaesthesia. Attempted closed reduction by flexion, abduction and applying an external rotation force on the left femur and using the femoral head as a lever was unsuccessful.
We proceeded to open reduction via a Pfannelstiel incision. Both her rectus abdominis attachments onto the pubic bones were intact. Under direct observation and using pointed reduction forceps the left pubis bone was reduced with some difficulty. This involved applying an anterior and lateral pulling force directly on the pubic bone via the pointed reduction forceps with a simultaneous external rotation force applied on the left iliac wing. After successful reduction, the symphysis remained unstable and we proceeded to plate the symphysis pubis. In the same sitting the left sacral fracture was fixed with fully threaded cannulated screw using the method described by Routt et al3(Figure 3).
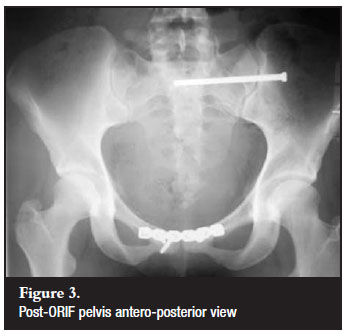
She had an uneventful postoperative course and her urinary catheter was removed after 2 days. Postoperative mobilisation consisted of bilateral partial weight-bearing using crutches for the first 4 weeks. Thereafter she was allowed full weight-bearing and at 6 weeks she was walking unaided.
At 4 months she had returned to ballet dancing, had no urinary symptoms and walked with a normal gait. She was last seen at 9 months post surgery and was discharged with no ill effects. Radiographs showed no signs of osteitis pubis or hardware failure.
Discussion
On perusing the available literature, overlapping pubic symphysis dislocation occurs more commonly in men than in women (11:3). The reasons as suggested by Cannada and Reinert4 are that the female pubic symphysis has a thicker cartilaginous disc and 2-3 mm greater mobility than the male pelvis. These two factors combine to reduce the likelihood of OPSD in females. Tadros et al5 presented the first two fully reported cases affecting women.
The complete mechanism of injury is not fully understood. What is uniformly agreed upon is that this injury occurs from a lateral compression force to the pelvis. From then on it is postulated that this is combined with forced hyperextension and adduction of the hip.1 Eggers then states that the symphysis dislocation can then either be anterior or posterior. All the reported cases have been posterior dislocations1,2,4-11 except the one by Robinson12 where inlet views and a pre-reduction CT scan were not performed and so the direction is uncertain. Tadros et al5 state that anterior dislocation probably does not exist. Indeed, most reported cases have been haemodynamically stable in keeping with the lateral compression nature of this injury.
A CT scan has consistently shown a posterior ring lesion except in the case reported by Sreesobh et al.10 Shanmugasundaram9 and Webb11 did not perform a CT scan. The posterior lesions range from sacro-iliac joint narrowing, a buckle fracture of the sacrum to a displaced longitudinal fracture of the sacrum. Only one of these sacral fractures was treated operatively using two percutaneously placed ilio-sacral screws into S1 and S2 segments.2 In our case the zone 2 left sacral fracture was mildly displaced and she had a contralateral tibial fracture. We took the decision to treat the sacral fracture operatively to allow for postoperative mobilisation without the risk of displacing the sacral fracture and to give added stability and thereby reduce the pain with weight bearing, as the patient would be partially weight bearing on the left leg during postoperative mobilisation. This represents the second case of OPSD where the pelvic ring has been fixed anteriorly and posteriorly. The percutaneous method used for the SI joint screw is both safe and effective.3 It is worth noting that Cannada's patient4 had a sacral fracture on initial CT scan and this was treated nonoperatively. This patient had posterior pain related to athletic activities.
Genito-urinary injuries are the most commonly reported associated injury, affecting 50% of reported cases. All seven of these have been urethral injuries but the patient reported by O'Toole et al8 had an associated extra-peritoneal bladder rupture. Tadros et al state 'in OPSD the urethra is subjected to crushing and shearing forces produced by the overlapping and partial vertical displacement of pubic bones'. Interestingly both the female cases reported by Tadros et al5 and our case did not have any genito-urinary injuries. Consequently, no genito-urinary injuries have been described in females. This may be due to the shorter urethra in females. This common association with genito-urinary injuries mandates that these should be actively looked for both during the initial assessment and at subsequent followup visits.
A pre-catheterisation urethrogram may be advisable5 and urologic assessment sought if there are any abnormalities. Erectile dysfunction as a complication has been reported in three cases.2,4,11
Osteitis of the pubic symphysis is the next commonly reported complication at 14%.5,9 None of these cases have been culture positive nor have they required antibiotics. This type of 'osteitis' may be similar in nature to arthrosis/cystic osteolysis of the acromio-clavicular joint as seen after ACJ disruption. Tadros et al5 treated their patient with NSAIDs. Shanmugasundaram's case9 had radiological evidence of osteitis but no clinical symptoms. Sreesobh's patient10 had postoperative wound infection that necessitated removal of metal ware. This happened despite the fact that this patient had no urinary tract injury.
In these case reports there is a high rate of failure with attempted closed reduction (11 out of 14) and it is widely accepted that achieving reduction of the pubic symphysis is the primary goal of management. This has been attained by both closed and open methods. Robinson et al,12 Webb11 and Dorai et al7all managed closed reduction under anaesthesia and treated their patients non-operatively because the reduction was stable. All these patients remained reduced and had a good result. The position of the displaced pubic bone has been found anywhere along the contralateral pubis bone up to and including being trapped in the obturator foramen.2,4,8,10 When closed reduction has failed all the authors have reverted to open reduction. Both single and dual plate fixation have been described. Cannada4and O'Toole et al8 opted for external fixation due to concerns of infection as both their patients had suprapubic catheters. Shanmugasundaram9 applied a hip spica after open reduction, which was kept for 4 weeks. O'Toole et al8were unable to reduce the incarcerated pubic bone from the obturator foramen and subsequently performed a superior ramus osteotomy of the normal side to aid reduction. To date theirs is the only case that required an osteotomy.
There has been one previously reported case that was left unreduced and the results were poor, with constant discomfort while walking and severe dyspareunia.13 We have one unreported case that presented late to our institution with OPSD that was left unreduced and had a poor result. He had an associated minimally displaced left zone 1 sacral fracture and a minimally displaced left iliac wing fracture. He had a 3 cm leg length discrepancy and anterior pelvic pain on walking.
The two descriptions: 'overlapping pubic symphysis dislocation' and 'locked pubic symphysis' have been used synonymously in the literature regardless of the final resting place of the displaced pubic bone. To this effect we would like to recommend the use of standardised terminology whereby the injury itself as a whole is called 'overlapping pubic symphysis dislocation' (OPSD) and the term 'locked pubic symphysis' be reserved only for cases where the displaced pubic bone is incarcerated inside the opposite obturator foramen.
Young and Burgess14 do not include this type of injury in their landmark article on classification of pelvic ring injuries. We would like to propose a classification system for these injuries that takes into account the following:
• ability to achieve and maintain closed reduction
• incarceration of the pubic bone into the opposite obturator foramen
• the significance of a posterior ring injury.
This classification has three grades:
Grade 1: OPSD where closed reduction can be achieved and maintained
Grade 2: OPSD where open reduction is required
Grade 3: Locked symphysis (incarceration into the obturator foramen).
Each grade has two subtypes:
A: without a significant posterior ring injury
B: with a significant posterior ring injury.
This grading system represents the progression of severity and instability.
Grade 1 injuries can be treated conservatively after closed reduction. Grade 2 and grade 3 injuries require open reduction and fixation. The decision to use single versus double plating or an external fixator will be dictated by the clinical scenario.
Grade 3 injuries also require open reduction but in addition may require an osteotomy of the opposite superior pubic ramus to unlock the displaced pubic bone and aid reduction.
A significant posterior ring injury is one that clinically requires fixation. Again the decision to do an open reduction and internal fixation or percutaneous fixation will be dictated by the clinical scenario.
No cases of open OPSD have been described.
Conclusion
An overlapping pubic symphysis dislocation is a rare injury. The majority of cases require stabilisation by open reduction and internal fixation of the anterior pelvic ring. Posterior lesions, if present, may need to be addressed. Urogenital injuries are the commonest acute associations, which mandates that they be actively excluded in these patients. The commonest long-term complications are urethral strictures, sexual dysfunction and non-infective osteitis pubis.
We have proposed a classification system that will suggest management and lead to uniform reporting to allow different centres to compare their results. We are aware that it is difficult to propose a classification system after a short follow-up period and without a large series but these are rare injuries and from the available case reports a trend is beginning to develop.
References
1. Eggers GWN. Dislocation of the os coxae. Am J Surg. 1952;3:300-307. [ Links ]
2. Gordon RO, Mears DC. Lateral compression injury of the pelvis. A case report. JBJS Am 1991;73-A No.9:1399-1401. [ Links ]
3. Routt ML Jr, Kregor PJ, Simonian PT, Mayo KA. Early results of percutaneous iliosacral screws placed with the patient in the supine position. J Orthop Trauma 1995;9:207-14. [ Links ]
4. Cannada LK, Reinert CM. Locked pubic symphysis. An open reduction technique. Clin Orthop Relat Res. 2009;467:2192-95. [ Links ]
5. Tadros AMA, Lunsjo K, O'Brien P. Overlapping dislocation of the pubic symphysis: report of three cases and review of the literature. Arch Orthop Trauma Surg. 2009;129:679-683. [ Links ]
6. Ansari S, Rollins J, Ebraheim NA. Locked pubic symphysis with ipsilateral fracture neck of a femur. J Trauma 2003;54:376-78. [ Links ]
7. Dorai CR, Kareem BA. Overlapping dislocation of the pubic symphysis. Injury 1991;22:329-30. [ Links ]
8. O'Toole RV, Sagebien C, Andersen RC, Nascone JW. Superior pubic ramus osteotomy to treat locked pubic symphysis. A case report. JBJS Am 2006;88:1609-14. [ Links ]
9. Shanmugasundaram TK. (1970) Unusual dislocation of symphysis pubis with locking. A case report. JBJS Am 1970; 52:1669-71. [ Links ]
10. Sreesobh KV, Sageer AM, RaYc M. Locked overlapping dislocation of the pubic symphysis into the obturator foramen: a case report. J Orthop Surg (Hong Kong) 2006;14:200-203. [ Links ]
11. Webb P. Overlapping dislocation of the symphysis pubis: A case report. JBJS Am. 1977;59:839. [ Links ]
12. Robinson D, Hendel D, Halperin N. An overlapping pubic dislocation treated by closed reduction: Case report and review of the literature. J Trauma 1989;29:883-85. [ Links ]
13. Gamble JG, Simmons SC, Freedman M. The symphysis pubis: Anatomic and pathologic considerations. CORR. 1986;203:261-72. [ Links ]
14. Burgess AR, Eastridge BJ, Young WR, et al. Pelvic ring disruptions: effective classification system and treatment protocols. J Trauma 1990;30:848-56. [ Links ]
 Reprint requests:
Reprint requests:
Dr Sithombo Maqungo
PO Box 13665 Mowbray 7705
South Africa
Tel: +27 (0) 832341723/Fax: +27 (0) 214472709
email: sithombo@msn.com
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article.














