Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.9 n.4 Centurion Jan. 2010
CLINICAL ARTICLE
Anatomic study of the atlas for surgical planning of lateral mass screw fixation: is it safe in our population?
Dr A ButeeraI; Prof M LukheleII
IMBChB, FCS(Orth)SA, Consultant Orthopaedic Surgeon and Director of Medical and Allied Services, King Faisal Hospital, Kigali, Rwanda
IIMBChB, FCS(Orth)SA, MMed(Orth), Head of Division of Orthopaedics, University of Witwatersrand, Johannesburg, South Africa
ABSTRACT
INTRODUCTION: Atlantoaxial instability is not uncommon and its management can be a challenge. Several stabilisation techniques have been described. All have their challenges because of the paucity of some osseous elements, the neural and vascular structures found in that region. Lateral mass screw fixation is one of the techniques which has been described for selected cases. Like all the other techniques it is a challenging technique to use and calls for full familiarisation with the anatomy at that region.
OBJECTIVES: The objective of the study was to assess if the atlas lateral mass screw can be safely accommodated in our population. The secondary aim was to establish if there were any differences in the size between the male and female or among the white and black population groups.
METHODS AND MATERIALS: Samples of dry adult atlas vertebra from the Raymond Dart Collection of human skeletons at the Wits University Department of Anatomy were measured for several parameters including the height, width and length of the lateral mass using an electronic digital caliper. Atlas of persons below 18 years of age at the time of death and those who had anomalies or deformities were excluded from the study. Data was recorded in Microsoft Excel and was imported in SAS V9.1 (SAS Institute Inc., Cary, NC, USA) for analysis.
RESULTS: One-hundred-and-fifty-nine atlas specimens were studied with almost equal numbers in both sexes and between black and white populations. The mean width of the lateral mass was 13.77 ± 1.23 mm, the height of lateral mass below the overhang was 4.51 ± 0.634 mm and the height of the lowest point of lateral mass was 11.94 ± 1.21 mm. The anteroposterior distance of the lateral mass was 17.64 ± 1.36 mm. The angle of inclination of posterior arch to lateral mass was 76.83 ± 5.12º. Of the 159 vertebrae, two vertebrae had lateral mass height below the overhang of 3.5 mm, and 37 vertebrae had height below overhang of 4 mm.
There were no statistical significant differences between male and female and between the race groups.
The reason for us to assess if there was any difference in the male and female and also in blacks and whites is that in our previous study on the size of the odontoid process we had found a significant difference between the groups. In that study we found that South African blacks had a much smaller odontoid process than South African whites. Interestingly we also found that South African blacks had a smaller odontoid process than African Americans. This indicated to us that there is more than genetic factors playing a role; environmental factors and nutritional factors could have influence. It was for that reason that we felt we could not take it for granted that these groups will have similar findings. This was the secondary aim of the study, not the main aim.
CONCLUSION: The atlas mass morphology was found to be adequate to accommodate the lateral mass screw safely in our population. Only two of the 159 dry atlas bones examined had the potential of not accommodating a 3.5 mm screw risking violating the occiputo-atlas joints. In 37 of the specimens the height of the lateral mass was below 4 mm. For that reason it is advisable not to use 4 mm size screws in our population as there is a significant risk that the occiputo-atlas joint may be violated by it.
Introduction
The atlantoaxial joint presents a challenge because of its limited biomechanical strength, paucity of some osseous structural elements, the neural and vascular structures contained and the frequent variation in anatomy.1 Common mechanisms of atlantoaxial instability include but are by no means limited to trauma, congenital abnormalities, degenerative conditions, infective and inflammatory diseases, and tumours.1,2 Clinically or radiologically significant atlantoaxial subluxation is managed by reduction and stabilisation of the atlas (C1)-axis (C2) mainly through a posterior approach.2,3 Any instrumentation construct to address the above issues must be strong enough to resist forces in multiple axes of motion, yet delicate enough to safely integrate into cervical spine elements providing stability and decreasing chances of pseudoarthrosis.1
Several posterior wiring techniques have been adopted for stabilisation and fusion of the atlantoaxial complex. Gallie in 1939 described a technique where a wire or cable is passed under the arch of the atlas over a corticocancellous bone graft shaped to conform to the posterior process of C1 and C2 and attached to the spinous process of the axis.4 The problem with this method is that it is the least stable of the techniques and therefore needs to be supplemented by a rigid external support.5 It is only adequate in resisting flexion moments but not extension and rotation moments. The sublaminar passage risks injury to the dura/spinal cord and it is contraindicated when the vertebra is displaced posteriorly.3,5 This technique is also not possible where there is a defect of the C1 posterior arch sometimes found in congenital or traumatic situations. Another technique used to stabilise the atlanto-joint instability is the Brooke and Jenkins technique. In this technique two wires are passed sublaminar at C1 and C2.5,6 This is a more stable fixation in resisting extension and axial rotation but passing the wires sublaminar at both C1 and C2 has the risk of injuring the dura and/or spinal cord.2,5,6 The third method is the clamps and hooks technique.7In this technique two laminar hooks are secured on the superior C1 posterior arch and two inferior laminar hooks inserted at C2, and the hooks are joined by rods. The disadvantages of the above methods is that they lack stability of rotation and lateral bending and have nonunion rates of 30% even with adjunct halo vest immobolisation.2,3,7 Transarticular screw fixation was promoted by Magerl and Seeman in 1987.8,9 This method is biomechanically superior to posterior C1-C2 wiring techniques by nearly ten times, thereby decreasing potential for pseudoarthrosis (0.6%).8 It has the shortcomings of risk of injury to the vertebral artery.2,9,10,11 Sufficient space must be available in the pedicle for screw fixation. In some cases the artery is anomalous and located in the path of the screw on at least one side in 18-23% of patients demonstrating the need for preoperative computerised tomography. C1-C2 reduction is required before insertion of the screw.2,11,12 It also has a risk of screw malpositioning and instrumental failure.1 It has a steep learning curve.
Another technique of stabilising C1 and C2 is using a lateral mass screw at C1 and a pedicle screw at C2. The clinical application of a lateral mass screw was first reported by Goel and Laheri from Bombay, India in 1994 using a plate and screw fixation from a posterior approach,12 and then largely ignored. They report experience with 30 cases of atlantoaxial instability using the C1 lateral mass and C2 pars interarticularis. They followed up their patients for 19 months with no morbidity, mortality or instrument fracture, and 100% fusion.13 Harms and Melcher developed and modified the technique for screw fixation of the atlas lateral mass and axis pedicle in 2001 using a 3.5 mm poly-axial screw and 3 mm rod system achieving postoperative stability, and long-term fusion.2,3,14
This technique is demanding because of the complex anatomy around C1 and C2. In 2003, Tan et al, from Beijing, China, described the feasibility of screw fixation of the atlas via the posterior arch and lateral mass with slight modification. Fifty dry atlas vertebrae were measured manually and radiologically with vernier calipers, protractors and computerised tomography scan.3 Hong and Dong, in 2004, reported on their study of posterior screw placement of the lateral mass.14 Gupta and Goel looked at the quantitative anatomy of 50 dry atlas vertebrae to detect the appropriate entry and projection of the C1 lateral mass screws.15 To our knowledge no study of the atlas in relation to the lateral mass screw fixation has been conducted in the South African population. This stimulated the authors to undertake this study aimed at looking at the lateral mass and posterior arch of adult C1 vertebrae from the local population (blacks and whites). The aim of this study was to assess the consistency of anatomic landmarks used for posterior insertion of the lateral mass screw of the atlas and to assess the safest projection for posterior lateral mass screw fixation of the atlas.
Materials and methods
This study was conducted in collaboration with the School of Anatomical Science, University of the Witwatersrand, which provided samples of dry adult atlas vertebrae from the Raymond Dart Collection of human skeletons. Approval was obtained from the university's Human Ethics Committee.
Only specimens of persons of the age of 18 years and above at the time of death were used. Any specimen having gross evidence of congenital or acquired vertebral pathology, or gross osteophytes was excluded from the study
An electronic digital caliper (EV150 from TA Toolquip and Allied, Crown Mines, Johannesburg, accuracy ± 0.003 mm) and a goniometer (accurate to 1º) were used to do direct measurements on the specimens.
Figures 1, 2 and 3 show the measurements that were performed on the lateral mass and posterior arch of the atlas. They are summarised in Table I.
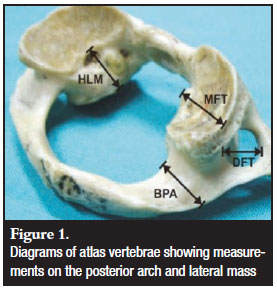
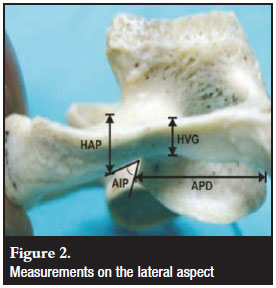
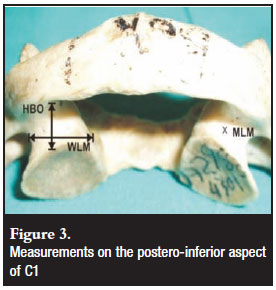
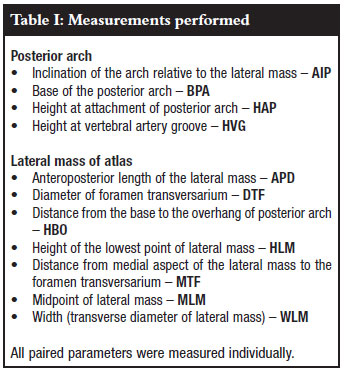
Sample size calculation
The following formula was used to calculate the minimum required sample size for the study.
n = 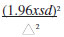
where
n = minimum sample size
Δ = is the size of the error we want to measure, as given by Cohen's D16,17
= 0.26
s.d.= standard deviation of the HVG measurement
= 0.832 mm
Thus,
n = 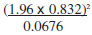
= 39
We needed 39 samples per group and since there are four groups, 156 samples needed to be examined.
Data was recorded in Microsoft Excel and was imported in SAS V9.1 (SAS Institute Inc., Cary, NC, USA) for analysis. The means, standard deviation and confidence intervals for all parameters were established. The difference between groups was done using the Wilcoxon and Kruskal-Wallis test. Significance was considered where P<0.05.
Results
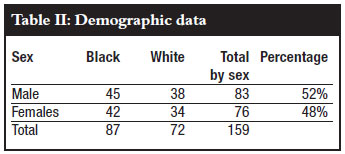
A total of 159 atlas vertebrae, dimensions of the posterior arch and lateral mass and relationship with vertebral artery were measured. Fifty-two per cent of the vertebrae specimens were male and 48% female. Fiftyfive per cent were for black persons and 45% whites (Table II). The mean and standard deviation of anatomic parameters calculated for the left and right are shown in Tables III, IV and V. In summary the width of the lateral mass was 13.77 ± 1.23 mm. The height of lateral mass below the overhang was 4.51 ± 0.634 mm. The height of the lowest point of lateral mass was 11.94 ± 1.21 mm. The anteroposterior distance of the lateral mass was 17.64 ± 1.36 mm. The distance from medial aspect of lateral mass to foramen transversarium was 12.95 ± 1.57 mm.The transverse diameter of the foramen transversarium was 6.14 ± 1.26 mm. The angle of inclination of posterior arch to lateral mass was 76.83 ± 5.12º.The height of the posterior arch at vertebral groove was 4.38 ± 0.84 mm. The height of posterior arch at attachment to lateral mass was 6.06 ± 1.25 mm. The width of posterior arch was 9.47 ± 0.93 mm. No statistical difference was found on any paired parameters measured individually on atlas on both left and right sides. Of the 159 vertebrae, two vertebrae had height below the overhang (HBO) of 3.5 mm, and 37 vertebrae had height below overhang (HBO) of 4 mm.
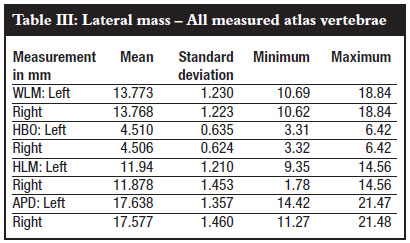
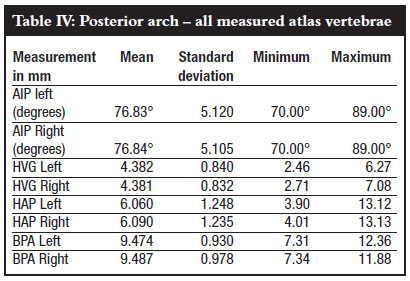
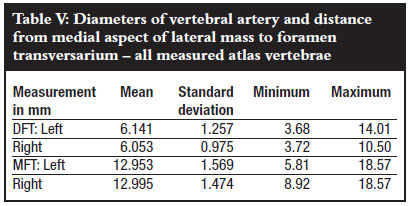
The mean and standard deviation of anatomic parameters were calculated for the male and for blacks and whites and are shown in Tables VI, VII, VIII and IX. The lateral mass height at lowest point was found to be 11.43 mm in female blacks and 12.50 mm in males, in female whites 11.6 mm and 12.1 mm in males. In both races the males have a slightly greater height. In all races the lateral mass height is adequate. The anteroposterior diameter of the lateral mass of the atlas was found to be 18.24 ± 1.28 mm in male blacks, 17.30 ± 1.55 mm in female blacks and 17.90 ± 1.22 mm in male whites as opposed to 11.66 ± 1.31 mm in white females. No significant difference was noted in either race or sex.
Discussion
Harms technique of atlas lateral mass screw fixation represents an alternative and a means to provide safe and efficacious fixation of the atlantoaxial joint.2 This provides one of the solutions to the complexity posed by stabilisation challenges of the atlantoaxial complex in relation to the rest of the spine (Figure 4). This is a result of the unique anatomy of the atlantoaxial complex with horizontal articular surfaces, ligamentous support, no intervertebral discs, and multiple axes of motion and anatomic variations of the vertebral artery.
The lateral mass screw provides the ability to rigidly fix challenging patients with atrophic pars, cervical kyphosis, deficient anterior arch of atlas, medially deviated vertebral artery and where there are absent posterior elements. The fixation can be incorporated as part of the fusion to the occiput and/or the axial spine. The screw at C1 allows direct intra-operative reduction of C1 on C2.2,3,4
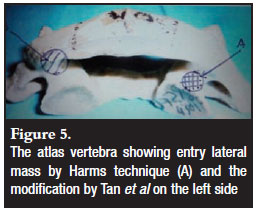
In this study, it was found that the lateral mass will allow placement of a 3.5 mm screw in 98.74% of cases measured. In the case where the height below the overhang of the posterior arch is less than 3.5 mm it would necessitate drilling the inferior part of the posterior arch at its attachment. Tan et al modified the point of entry of the screw at the C1 lateral mass to include part of the base of the posterior arch (Figure 5).3 Since the height of the posterior arch at attachment was 6.06 ± 1.25 mm in this study enough space was available to accommodate a screw without risk to the vertebral artery above.
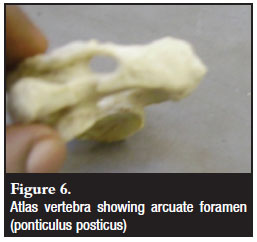
A few atlas vertebrae which were excluded from this study had ponticulus posticus or arcuate foramen on the posterior arch of C1 (Figure 6). Care should be taken to identify this anomaly pre-operatively to prevent injury to the vertebral artery during posterior dissection and placement of C1 lateral mass screws.18 This anatomic variant can be identified on lateral radiography or on computerised scan which are routinely done before surgery.
With regard to the safest projectile, the width of the lateral mass of 13.77 ± 1.23 mm provides enough space for exposure and fixation of 3.5 mm screws and options for medialisation of the screw. The height of the lateral mass at its lowest point was 11.43 ± 1.05 to12.50 ± 0.89 mm. The longest projectile through the lateral mass was 16.56 ± 1.14 to 18.31 ± 1.29 mm (minimum 11.27 and maximum 20.80 mm). The medial aspect of the lateral mass to the foramen transversarium was 12.05 ± 1.15 to 14.36 ± 1.28 mm. The angle of inclination of posterior arch to lateral mass was found to be 76.83 ± 5.12º.
The space available considering these measurements creates a safe projectile to accommodate a 3.5 mm screw in most cases.
The use of a 4 mm screw would prove difficult in 23.27% of our population.
Conclusion
The study shows that the use of 3.5 mm screws is feasible and safe for the size of the lateral mass of the atlas in our population. It requires good pre-operative planning with appropriate radiological evaluations including Xrays and computerised tomographic scans to exclude anatomic anomalies which are common in this region. Superb experience in the technique is mandatory before embarking on this procedure.
References
1. Vender JR, Rekito AJ, Harrison SJ, MacDonnell DE. The evolution of posterior cervical and occipitocervical fusion and instrumentation. Neurosurg Focus 2004 Jan 15;16(1):E9. [ Links ]
2. Harms J, Melcher RP. Posterior C1-C2 fusion with poly axial screw and rod fixation. Spine 2001;26:2467-71. [ Links ]
3. Tan M, Wang H, et al. Morphometric evaluation of screw fixation in atlas via posterior arch and lateral mass. Spine 2003;28:888-95. [ Links ]
4. Gallie WE. Fracture dislocation of cervical spine. Am J Surg 1939;46:495-99. [ Links ]
5. Stauffer ES. Posterior atlanto-axial arthrodesis. The Gallie and Brookes techniques and their modifications. Tech Orthop 1994;9:43-48. [ Links ]
6. Brookes AL, Jenkins EB. Atlanto-axial arthrodesis by wedge compression method. J Bone Joint Surg Am 1978;60:279-84. [ Links ]
7. Moskovic R, Crockard HA. Atlantoaxial arthrodesis using intralaminar clamps: an improved technique. Spine 1992;17:261-67. [ Links ]
8. Grob D, Jeanneret B, Aebi M, Markwalder T. Atlanto-axial fusion with transarticular screw fixation. JBJS (Br) 1991;73-B:972-76. [ Links ]
9. Margerl F, Seeman PS. Stable posterior fusion of the atlas and axis by transarticular screw fixation. In: Kehr P, Weidner A, eds. Cervical Spine, vol.1. New York, NY: Springer-Verlag; 1987:322-27. [ Links ]
10. Gebhard JS, Schimmer RC, Jeanneret B. Safety and accuracy of transarticular screw fixation C1-C2 using an aiming device: an anatomic study. Spine 1998;23:2185-89. [ Links ]
11. IgarashiT, Kikuchi S, et al. Anatomic study of axis for surgical planning of transarticular screw fixation. Clin Orthop and Rel Research 2003;408:162-66. [ Links ]
12. Abou MA, Solanki G, Casey AT, et al. Variation of the groove in the axis vertebra for vertebral artery: implication for instrumentation. J Bone Joint Surg Br 1997;79:820-23. [ Links ]
13. Goel A, Laheri V. Plate and screw fixation of atlanto-axial subluxation. Acta Neurochir (Wien) 1994;129:47-53. [ Links ]
14. Hong X, Dong Y, et al. Posterior screw placement on the lateral mass of the atlas: An anatomic study. Spine 2004;29:500-3. [ Links ]
15. Gupta S, Goel A, Quantitative anatomy of lateral mass of atlas and axis vertebrae. Neurol India 2000;48:120-25. [ Links ]
16. Cohen J. Statistical power analysis for the behavior sciences. 1988, 2ndEdition, Hillsdale, NJ: Erlbaum. [ Links ]
17. Cohen J. A power primer. Psychological Bulletin 1992;112:155-59. [ Links ]
18. J P Young, PH Young, MJ Ackermann, PA Anderson, KD Riew. Ponticulus posticus, implication for screw insertion into first cervical lateral mass. J Bone Joint Surg Am 2005;87A:2495-98. [ Links ]
 Reprint requests:
Reprint requests:
Prof M Lukhele
Dept of Orthopaedics Wits Medical School
7 York Road Johannesburg 2001
Tel: 011 717-2538/Fax: 011 717-2551
email: mkhululi.lukhele@wits.ac.za
No benefits or sponsorship have been received by any of the authors for this study.














