Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.9 n.3 Centurion Jan. 2010
CLINICAL ARTICLE
It is not always tuberculosis of the spine: ganglioneuroblastoma
EN MutetiI; S GovenderII
IMBChB(Moi), MMed(Mak), FCS(Ecsa). Spine Fellow, University of KwaZulu-Natal, King George V Hospital Spine Unit
IIMBBS, MD, FRCS. Professor and Head of Orthopaedic Surgery, University of KwaZulu-Natal, Head of King George V Hospital Spine Unit
ABSTRACT
Tuberculosis has been said to be the great mimicker of our times because of the spectrum of clinical and radiological presentation. We report the case of a 15-year-old girl who was referred as tuberculosis of the spine, but which was in fact a ganglioneuroblastoma of the spine. This case report highlights the radiologic features of spinal tuberculosis and the importance of obtaining a tissue diagnosis prior to treatment.
Introduction
Tuberculosis has been said to be the great mimicker of our times because of the spectrum of clinical and radiological presentation.1 We report the case of a 15-year-old girl who was referred as tuberculosis of the spine, but which was in fact a ganglioneuroblastoma of the spine.
Case presentation
A 15-year-old female presented with back pain and weakness of the lower limbs for 6 months. These symptoms started 6 months prior to presentation when, while walking, her knees suddenly gave way and she fell to the ground. She was not able walk without support because of weakness in the lower limbs and pain in her back. The back pain was severe, especially at night, throbbing in nature and localised to the dorsolumbar junction. Both the back pain and lower limb weakness were getting progressively worse. However, she did not have numbness or pain in the lower limbs, bowel/bladder disturbances or night sweats. She had lost weight and appetite. Her father had died of pulmonary tuberculosis in the previous year. The local clinic, suspecting spinal tuberculosis, commenced antituberculosis treatment for 6 months. She was referred to the spine unit because of the progressive nature of the disease.
Examination revealed generalised wasting and anaemia but no jaundice, oedema or lymphadenopathy. She had a mild right lower thoracic scoliosis with the apex at T11/T12 and her lumbar spinal lordosis was flattened. The dorsolumbar junction was warm and tender. Sensation was intact. Motor function was poor at the knees and ankles (MRC power 2). She was continent. The upper limbs were normal. The cranial nerves, neck, respiratory and cardiovascular systems were normal.
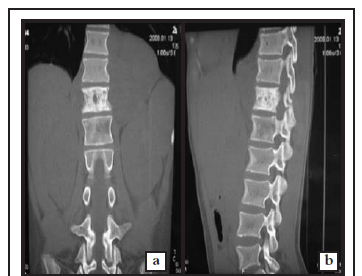
The haemoglobin was 10.7 g/dl. Erythrocyte sedimentation rate was 39 mm/hr. White blood cell count, differential, renal function and liver function tests were normal. The HIV test was negative. Plain radiographs demonstrated a mild right dorsolumbar kyphoscoliosis extending from the T10 to L2 vertebrae with the apex at T12/L1. T12 vertebral body was sclerotic and the pedicles were not clearly visualised. A paravertebral soft tissue shadow was noted in the T10-L2 region. The chest radiograph was normal. CT scan of the spine showed dense sclerosis of the T12 vertebral body and posterior elements, a lytic lesion of the left side of L1 vertebral body and a large paravertebral soft tissue component around the lower thoracic spine. The disc spaces were preserved (Figures 1a, 1b, 1c).
The spine MRI scan revealed abnormal marrow changes from T11 to L1 vertebral bodies and posterior elements. The paravertebral soft-tissue lesion extended from T11 to L1 anteriorly with destruction of the posterior elements. This was contiguous with a posterior epidural component through an enlarged neural foramen. Part of the soft tissue lesion lay superficial to the T12 vertebral arch.
The distal cord was slightly expanded with patchy T2 hyperintensity suggesting compressive neuropathy (Figures 2a, 2b, 2c). MRI scan of the brain was normal.
The above features suggested a chronic infective spondylitis, most likely tuberculosis of the spine with compression. The differential diagnosis was atypical mycobacterial or fungal infection. Therefore, biopsy and decompression of the cord was done through a left-sided costo-transversectomy of the dorsolumbar junction. Granulation material compressing the conus medullaris was noted. Histopathologic examination of a biopsy specimen of this mass demonstrated features consistent with the diagnosis of a retroperitoneal ganglioneuroblastoma of the spine. Ultrasound and MRI revealed no lesions in the adrenals and retroperitoneum. The patient was commenced on chemotherapy and radiotherapy. She currently remains Frankel C one year postoperatively.
Discussion
Tuberculosis is common in the developing world. According to the World Health Organization (WHO), more than 2 billion people, equal to one-third of the world's population, are infected with the tuberculous bacillus. Spinal tuberculosis accounts for 2-5% of all cases of tuberculosis, and the prevalence of spinal tuberculosis in South Africa is 948 per 100 000 people.1,2 The majority of these are children and young adults, presenting with several months of back pain, constitutional symptoms, kyphosis and neurologic deficit.3 Our patient was 15 years old, presented with chronic back pain, neurologic deficit and a family history of tuberculosis suggesting spinal tuberculosis. She also had anaemia of chronic illness in keeping with the duration of her symptoms. The ESR was modestly elevated. The low signal intensity in the T1-weighted image of the MRI scan, and a high signal intensity in the T2-weighted image, closely resembled spinal tuberculosis.
Ganglioneuroblastoma is a very rare disease and the estimated annual incidence rate is <5 per 1 million children. It is a neuroblastic tumour that arises from foetal neural crest cells that fail to regress in the eighteenth week of development. It predominantly affects infants and young children, and rarely occurs above 10 years of age.4 Ganglioneuroblastomas are malignant tumours containing mature ganglion cells, Schwannian stroma and immature neuroblasts. The most common locations are the adrenal medulla and the retroperitoneum.5,6,7 In our patient, the tumour was retroperitoneal. It is possible that this was a very slow-growing tumour, with a higher benign tissue component, thus presenting much later in life. Pain and neurologic deficit were prominent features suggesting that the tumour was aggressive.
Spinal tuberculosis does present atypically on radiologic examination as single vertebral disease. The vertebra may or may not undergo concentric collapse. It could also present as an ivory vertebra (similar to our case), isolated neural arch tuberculosis or as circumferential (pan) vertebral involvement.8 However, the MRI scans showed characteristic lobulation, a dumbbell extension in to the spinal canal and a soft tissue component involving the posterior elements and superficial to the posterior vertebral arch.4,5 This is unusual with tuberculosis.
Conclusion
Ganglioneuroblastoma of the spine is very rare, while spinal tuberculosis is much more common in our setting. This case report highlights the importance of obtaining a tissue diagnosis prior to treatment.
References
1. Dunn R. The medical management of spinal tuberculosis. SA Orthop J 2010;9(1):37-41. [ Links ]
2. World Health Organization. WHO REPORT 2009 Global Tuberculosis Control. Website http://www.who.int. [ Links ]
3. Cheung KMC, Leong JCY. Adult spinal tuberculosis. In: Govender S, Leong JCY (eds). Inflammatory diseases of the spine. Singapore. TTG Asia Media; 2003:11-3. [ Links ]
4. Rha SE, Byun JY, Jung SE, et al. Neurogenic tumors in the abdomen: tumor types and imaging characteristics. Radiographics. Jan-Feb 2003;23(1):29-43. [ Links ]
5. Lonergan GJ, Schwab CM, Suarez ES, Carlson CL. Neuroblastoma, ganglioneuroblastoma, and ganglioneuroma: radiologic-pathologic correlation. Radiographics. 2002 Jul-Aug;22(4):911-34. [ Links ]
6. Shimada H. Tumors of the neuroblastoma group. Pathology (Phila). 1993;2(1):43-59. [ Links ]
7. Joshi VV, Silverman JF. Pathology of neuroblastic tumors. Semin Diagn Pathol 1994 May;11(2):107-17. [ Links ]
8. Pande KC, Babulkar SS. Atypical spinal tuberculosis. In: Symposium on osteo-articular tuberculosis. Clinical Orthop.2002; 398:67-74. [ Links ]
 Reprint requests:
Reprint requests:
Prof S Govender
Department of Orthopaedic Surgery, Nelson Mandela School of Medicine, University of KwaZulu-Natal
Private Bag 7
4013 Congella Durban South Africa
Tel: +27(0)31 260 4297 Fax: +27(0)31260 4518
Email: katia@ukzn.ac.za
The content of this article is the sole work of the authors. We, the authors, confirm there is no financial or personal relationship with other people or organisations that may have inappropriately influenced this work. All authors were fully involved in this study and the preparation of the manuscript. We confirm that the material has not been submitted for publication elsewhere. Approval by ethical committee: Yes. Informed consent was obtained: Not applicable (retrospective case study).