Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.9 n.3 Centurion Jan. 2010
CLINICAL ARTICLE
Spinal deformity in neurofibromatosis
MB NortjéI; RN DunnII
IMMed(Orth), FCOrth(SA). Registar, Department of Orthopaedics, University of Cape Town
IIMMed(Orth)(UCT), FCOrth(SA). Consultant Orthopaedic and Spine Surgeon, Associate Professor, University of Cape Town, Head. Orthopaedic Spine Services: Groote Schuur Hospital
ABSTRACT
Scoliosis is a common orthopaedic condition associated with neurofibromatosis (NF). The associated scoliosis can be severe and tortuous providing management challenges with frequently poor outcome. An awareness and earlier intervention may well improve this.
We present 14 patients with NF seen in our spinal service from mid 2001 until 2008. Clinical presentation, curves and surgical management are reported.
Introduction
Neurofibromatosis (NF) is a multisystem disease characterised by mixed cell tumours of neural origin. It can be classified into four clinical types: Type 1 (peripheral type) previously known as von Recklinghausen's disease, is the most common type. It results from an abnormality of the NF1 gene on chromosome 17. NF1 is a tumour suppressor gene that codes for the protein neurofibromin. It follows an autosomal dominant pattern of inheritance and is one of the most common autosomal dominant conditions. Approximately half the cases are due to new mutations. The incidence is 1 in 4 000 and the manifestations vary from person to person, with only 10% of NF1 patients requiring orthopaedic treatment.1
The diagnosis is made if two or more of the following seven criteria are present (NIH criteria):2
• six or more café au lait macules greater than 5 mm in children and 15 mm in adults
• two or more neurofibromas or one plexiform neurofibroma
• axillary or inguinal freckling
• two or more Lisch nodules (iris hamartomas)
• optic nerve glioma
• sphenoid dysplasia or typical long bone abnormalities (e.g. tibial pseudoarthrosis)
• first degree relative with NF
Scoliosis of the thoracolumbar spine is the most common skeletal manifestation of NF, occurring in 23% of NF1 patients at Crawford's NF clinic in Cincinnati.3
It should be noted that patients do present with cervical spine abnormalities but much less commonly. In the cervical spine the main problems are kyphosis and C1/2 instability, and these are often overlooked because of the more obvious thoracolumbar pathology.4
Scoliosis in NF can be divided into non-dystrophic or dystrophic types. Non-dystrophic is similar in presentation and clinical features to idiopathic scoliosis but tends to have a more rapid progression and less favourable response to surgery because of the development of pseudarthrosis.
Dystrophic curves are typically short segment (four to six vertebrae), sharp curves of the upper thoracic spine. They are associated with characteristic spinal abnormalities, namely:
• vertebral scalloping - mainly the posterior wall
• increased interpedicular distance on the AP radiograph
• widening of the intervertebral foramen on the lateral radiograph
• pencil ribs - ribs that are narrower than the narrowest part of the second rib
• spindling of the spinous processes
• severe rotation of the apical vertebra
Aim of the review
We reviewed NF patients presenting to the spinal clinic with regard to their presenting features and spinal pathology.
Materials and methods
Patients were identified from an electronic database of outpatient attendances from mid-2001 to 2008. The patient folders and radiographs were then retrieved and analysed. Demographic data, the presenting complaint, and other relevant history were documented. The type and severity of the spinal deformity of each patient was recorded. The Cobb angle was used to measure the scoliosis on the anteroposterior radiograph.
Results
Fourteen patients with scoliosis and NF were identified. There were six males and eight females. The median age was 14 years with a range of 3 to 50 years.
The nine children (under 18 years of age) were referred with spinal deformity by other health care providers. None had pain or neurological signs at presentation (Table I).
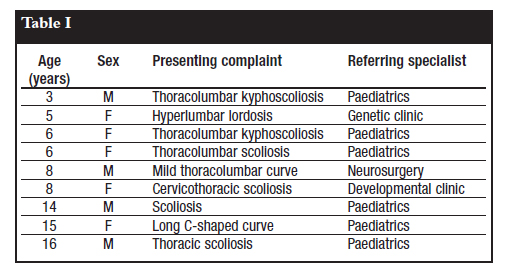
Of the five adult patients, one presented with a painless deformity, two presented with pain and two presented with neurological deficit as their primary complaints (Table II).
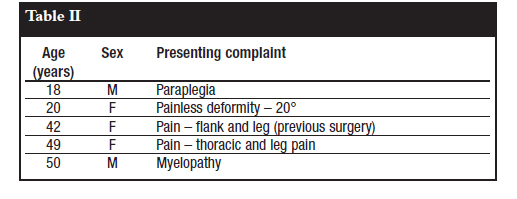
Type of curve
Only four of the 14 patients displayed the dystrophic features of NF on plain radiographs. Many of the curves in this cohort do not lend themselves to quantification on two-dimensional imaging. This is due to a helical type deformity at the apex with both severe kyphus and scoliosis making single plane Cobb measurement meaningless. Those that were measurable ranged from between 32º and 70º in the coronal plane.
Procedures done
In total, nine patients underwent surgery. Of the five patients that have not had surgery, one is on the waiting list, one is being followed up and may require surgery, one defaulted follow-up and one was discharged with a mild curve of 20º.
In the surgery group all but one patient had instrumented fusions because of the high risk of non-union and pseudoarthrosis. Three patients had posterior instrumentation only. Two of these patients had been operated on in the 1970s with Harrington rods, and pre-operative X-rays were not available to measure curve size. The third patient was a 32º curve corrected to 5º. Two patients underwent anterior instrumentation only. These were both thoracolumbar curves of 55º and 60º respectively which corrected to less than 10º. Four patients underwent combined anterior and posterior instrumented fusion. These were severe multiplanar (kyphoscoliotic) deformities with a helical apex not amenable to accurate quantification (Figure 3a).
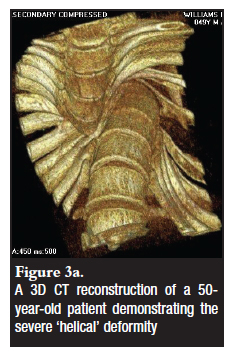
In two patients the planned procedure was aborted. These were both adult cases with severe tortuous thoracic kyphoscoliosis and presenting with pain and myelopathy. The planned procedures were anterior transthoracic corpectomies to decompress the canal followed posterior fusion. The experienced difficulties were not appreciated pre-operatively. On entering the chest laterally, the helical nature of the apex resulted in the spine itself blocking access to the apex (Figure 3a). In addition, the aorta required multiple segmental ligation to mobilise. This was felt to be inadvisable in the context of myelopathy and an already sub-optimal cord. Thus a strut was placed, wedged between the kyphotic spine with some correction in the hope rather than the belief that the slight correction and rigidity would protect the cord from further deterioration.
Discussion
Although NF is one of the most common hereditary conditions, the orthopaedic manifestations are still sufficiently rare to be seen in any meaningful numbers only in large referral centres.
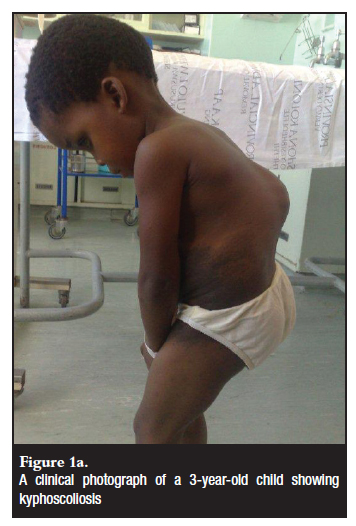
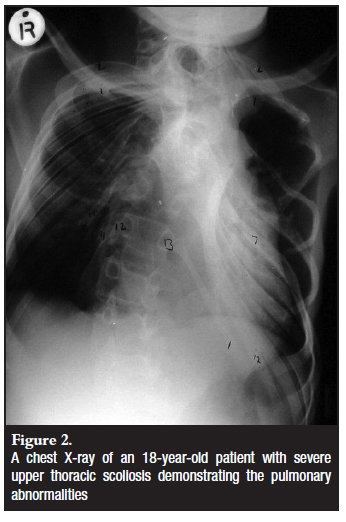
In the immature patients the presenting complaint mirrored that of patients with idiopathic scoliosis, i.e. deformity (Figure 1a). In contrast, the older patients presented with more severe symptoms. Two of them presented with signs of cord compression. In the older patients the more severe symptoms related to more severe curve types. One patient had a severe kyphoscoliosis with resultant chest deformity and respiratory compromise posing a risk to the surgery (Figure 2). In fact he continued to deteriorate to type 2 respiratory failure in the post-surgical follow-up period.
The presenting complaints in this small study can be classified as one or a combination of pain, deformity or myelopathy. The symptoms represent a spectrum based on the time to presentation and the severity of the curve suggesting a natural history of curve progression and myelopathy with ageing.
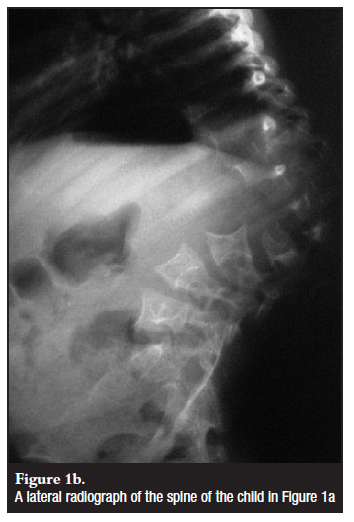
In the paediatric group most had non-dystrophic curves and appeared radiographically not unlike idiopathic scoliosis. Although only four of the patients had radiographic features that were suggestive of NF (pencil ribs and scalloped vertebrae), the clinician should always scrutinise imaging for dystrophic features (Figure 1b).
Seven of our patients had other more readily diagnostically suggestive features of NF (café au lait spots, freckling and neurofibromas). These were also present in the patients who had radiographic spinal features.
When it comes to surgery various approaches and types of implants have been used. In immature patients the deformity tends to be flexible and standard surgical techniques are applicable. Risks of non-union necessitate instrumentation and consideration of posterior and anterior fusion may be necessary for both fusion rates and the prevention of the crankshaft phenomenon in the growing spine.
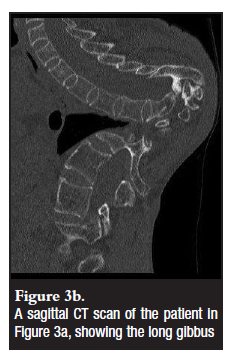
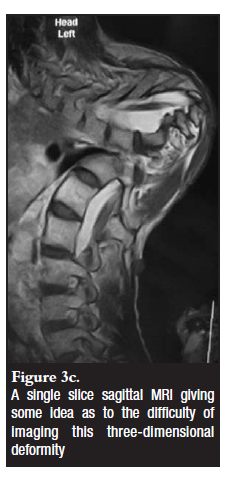
In the older patient, the deformities can be severe and pose a substantial surgical challenge due to the rigidity and tortuous nature limiting access to the apex (Figures 3b and c). In our experience, attempted decompression had to be aborted on two occasions and compromised to anterior strut graft. This is because we were unable to safely access the internal gibbus as the aorta was tightly adherent and would have required multiple segment ligation with increased risk of cord ischaemia. The posterior vertebral body resection procedure (PVCR) may well be a better approach and should be considered to improve access and reduce intra-operative risk to the cord and patient.
References
1. Crawford AL. Orthopaedic complications of von Recklinghausen's disease in children. Current Orthopaedics 1996;10:49-55. [ Links ]
2. National Institutes of Health Consensus Development Conference Statement: Neurofibromatosis. Neurofibromatosis 1988;1:172. [ Links ]
3. Crawford AL, Parikh S, Schorry EK, Von Stein D. The immature spine in Type-1 Neurofibromatosis J Bone Joint Surg Am 2007(89)123-42. [ Links ]
4. Craig JB, Govender S. Neurofibromatosis of the cervical spine. A report of eight cases. J Bone Joint Surg Br 1992;74:575-8. [ Links ]
 Reprint requests:
Reprint requests:
Prof Robert Dunn
Tel: (021) 404-5387, Fax: (021) 404-5389
Email: info@spinesurgery.co.za
This article is the sole work of the authors. No benefits of any form have been or are to be received from a commercial party related directly or indirectly to the subject of this article.














