Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.9 n.2 Centurion Jan. 2010
EXPERT OPINION ON PUBLISHED ARTICLES
The effect of an anterior cervical operation for cervical radiculopathy or myelopathy on associated headaches
Joseph Riina, MD; Paul A Anderson, MD; Langston T Holly, MD; Kathy Flint, RN, CNOR; Kenneth E Davis, MS; K Daniel Riew, MD. JBJS (Am) 2009; 91: 1919-23
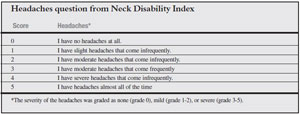
The authors embarked on this study to determine whether anterior cervical reconstructive surgery for the treatment of radiculopathy or myelopathy would also help for associated headaches. A total of 1 004 patient were evaluated by means of the Neck Disability Index questionnaire; 803 patients were followed for 24 months. Arthroplasty as well as anterior cervical discectomy and fusion were evaluated; the arthroplasty cohort had 518 patients and the anterior cervical discectomy and fusion group had 486 patients.
Interestingly, improvement in the Headache Pain Score of at least one grade was reported in 64% of the arthroplasty group and 58.5% of the arthrodesis group. Pain scores for the arthroplasty group worsened in 8.4% and in 13.7% for the arthrodesis group. The rest remained unchanged.
The authors conclude that at two years postoperatively, patients who had anterior cervical surgery (both arthroplasty and arthrodesis) for cervical radiculopathy and myelopathy can be expected to significantly improve with regard to headache symptoms.
The authors point out that the literature previously indicated that headaches most probably originate from the upper cervical spine. In this study single level pathology was addressed from level C3 down to C7. Furthermore, it is emphasised that anterior cervical surgery should not be seen as a treatment modality for headaches but, if performed for radiculopathy and/or myelopathy, it seems that an added bonus in a great majority of patients will be alleviation of headache symptoms.
Although the authors admit to some weaknesses in this study, this is an article of interest to take note of.
Reviewer: Dr PR Engelbrecht
Wilgers Hospital
Pretoria
Tel: (012) 807-1298/9
Residency Review Committee (RRC) Foot and Ankle Curriculum: We don't need to reinvent the wheel
Paul J Juliano, et al.
Foot & Ankle International March 2010; 31(3):260-3
It is not an exaggeration to state that there is a huge void in foot and ankle
(F & A) teaching at all levels. This article highlights several points besides the importance of such a curriculum.
It highlights that there are several bodies that set guidelines for such teaching (to my knowledge, there is no such body in South Africa).
It also highlights the multidisciplinary involvement in health care teaching, as well as a curriculum that extends far beyond the de facto teaching programme of F & A surgery.
The downside of this article is that it only skims the surface and makes several references to 'online supplements'.
By the very nature of the topic, this article can only describe in broad terms what is required for a registrar to become not only an efficient and competent clinician, but also compassionate, ethical and with interpersonal skills in all aspects of F & A practice - in other words, one who sees beyond just hard-core knowledge. This in fact applies to registrars in all disciplines and not only F & A.
I am aware that every department has its own unique programme for F & A teaching; however, I urge all academics to read this comprehensive article and even look up the 'online supplements'. Concentrating on specific topics which individual departments deem important for their registrar training is not enough without the general approach to a F & A curriculum (which includes learning, teaching, research, participation in academic meetings, publications, the keeping of medical records, informed consents, but to mention a few) as set out in this article.
Perhaps most importantly, this article should also be read by the qualified orthopaedic surgeon, as this 'curriculum' does not end after four years of registrarship. The orthopaedic surgeon is 'expected to model the professional behaviour expected of our residents'.
Further reading on the subject
1. Trepman E, et al. Individual didactic sessions or group lectures for teaching the foot and ankle to orthopaedic residents. Foot and Ankle Surgery 2007;13:69-75.
2. Wodey VMR, et al. Orthopaedic Surgery Core Curriculum: Foot and Ankle Reconstruction. Foot Ankle International 2007;28(7):831-7.
Reviewer: Dr Nick P Saragas
Netcare Linksfield Hospital & Orthopaedic Department
and University of the Witwatersrand
P O Box 1153, Highlands North 2037
Tel: +2711485 1974
Fax: +27116405313
Does treatment (non-operative and operative) improve the 2-year quality of life in patients with adult symptomatic lumbar scoliosis?
KH Bridwell, S Glassman, W Horton, et al
Spine 2009; 34: 2171-8
Only one paper in the peer-reviewed published data directly addresses the question of whether treatment for patients with adult symptomatic lumbar scoliosis affects quality of life. That paper suggested that operative treatment was more beneficial than non-operative care. Yet, there are limitations that relate to the historical context, since all the patients were treated with Harrington implants, and to the absence of validated patient-reported outcome data.
In this study, the authors performed a prospective observational chart study with matched and unmatched comparisons to compare the results of adult symptomatic lumbar scoliosis patients treated non-operatively and operatively.
A total of 160 corrective patients were enrolled (age: 40-80 years) with baseline and 2-year follow-up data for five centres. Lumbar scoliosis without prior surgical treatment was defined as a minimum Cobb angle of 30º. All patients had either an Oswestry Disability Index score of 20 or more, or Scoliosis Research Society domains scores of 4 or less in pain, function, and self-image at baseline. Pre-treatment and 2-year follow-up data collected prospectively included basic radiographic parameters, complications and a variety of outcome measures.
At 2 years, follow-up on the operative patients was 95% and for the non-operative patients 45%. The demographics for the non-operative patients followed for a maximum of 2 years and those lost to follow-up were identical. The operative cohorts significantly improved in all quality of life measures. The non-operative cohorts did not improve and non-significant decline in quality of life scores was common. At minimum 2-year follow-up, operative patients outperformed non-operative patients by all measures.
The authors conclude that common non-operative treatments do not change the quality of life in patients with adult symptomatic lumbar scoliosis at 2-year follow-up.
A limitation of this paper is the fact that the follow-up of the non-operative group was only 45% at 2 years. In addition, non-operative treatment is not defined with the result that it is unknown whether a structured rehabilitation with cognitive intervention was followed. Furthermore, the co-morbidities of patients in the surgical group, like osteoporosis, were not evaluated.
Reviewer: Dr E Coetzee
MBChB, MMed (Orth)
Pretoria East Hospital
Tel: (012) 998-4263