Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.9 no.2 Centurion ene. 2010
CLINICAL ARTICLE
Prosthesis sepsis in a tertiary setting: a retrospective analysis
R GollerI; K GollerII; A VisserIII; HF VisserI; JM NelI; CH SnyckersIV
IMBChB(Pret) Senior Registrar, Department of Orthopaedic Surgery, University of Pretoria
IIBPhysT(Pret) Physiotherapist, Newlands, Pretoria
IIIMBChB(Pret), DTM+H, PG(Dip)TM Senior Registrar, Department of Clinical Pathology, University of Pretoria, National Health Laboratory Services, Tshwane Academic Division
IVMBChB(Pret), Dip(PEC)SA, MMed(Orth)(Pret), FC(Orth)SA Consultant, Department of Orthopaedic Surgery, University of Pretoria
ABSTRACT
PURPOSE OF THE STUDY: Annually, more than a million joint replacements are performed worldwide. The most feared complication is infection. The purpose of this study is to establish the spectrum of organisms and their respective sensitivities, cultured during primary and secondary debridements of staged revision surgery. These findings were then utilised to suggest alternative empiric antimicrobial therapy.
DESCRIPTION OF METHODS: A retrospective analysis was performed on patients undergoing revision hip or knee arthroplasty at a tertiary hospital in South Africa from June 2005 to March 2009. Only patients in whom intra-operative deep microbiological cultures had been performed were included.
SUMMARY OF RESULTS: Deep microbiological cultures were performed in all cases on either joint synovium, fluid or pus swabs taken from the site intra-operatively. Following primary debridement of staged revision surgery, 38% of samples submitted were culture positive from 61 patients, rendering 29 isolates (six double infections). The spectrum was highly variable. Although no methicillin-resistant Staphylococcus aureus (MRSA) was isolated in the initial cultures, the majority of organisms were Gram positive (62%).
Fourteen of these patients (23%) required a second debridement; 12 patients had positive cultures (86%), rendering 20 isolates (four double and two triple infections). Gram-negative organisms played a significant role in these patients with the majority of cases culturing multi-resistant organisms.
CONCLUSION: Although no MRSA was cultured, vancomycin is widely used as an empiric postoperative antimicrobial. In this setting, 72% of isolates were sensitive to vancomycin; however, co-amoxyclav also covered 72% of isolates, with the benefit of superior efficiency and fewer side effects. We suggest the possible use of co-amoxyclav with rifampicin as a potential first-line antimicrobial in this clinical setting.
Multi-drug resistance is increasingly important in patients requiring secondary debridements. In this setting a combination of carbapenems with vancomycin should be considered as empiric postoperative antibiotics, as it covered 75% of organisms in our clinical setting.
Introduction
It is estimated that more than a million joint replacements are performed annually, worldwide.1 This procedure offers the benefit of restoring normal function to a limb. Joint replacements are not without complications, of which aseptic loosening is the most common, but the most serious and feared is infection.1-3 The infection rate is quoted to vary from 0.6 to 16% for hip, and 0 to 23% for knee replacements. With modern preventative techniques the risk is reduced to <2% in primary hip replacements and <1% in primary knee replacements. The subsequent risk of infection upon revision ranges from 3 to 4% for hips and <2% in knee revision arthroplasty.4
The duration of the infection seems to have a significant influence on response to treatment. Biofilm formation, although present from an early stage of infection, seems to reach a clinically significant level after about one month of infection - to such an extent that cure with retention of the prosthesis becomes unlikely.5 Once present, biofilms are not only particularly resistant to treatment, but also difficult to culture. Organisms associated with peri-surgical biofilm formation include various Gram-positive cocci and negative bacilli.6
The gold standard management of septic prosthetic joints entails a two-stage re-implantation, during which the prosthesis is removed and infected tissue is resected.1,7 The main advantage of utilising a two-stage procedure is the high success rate in eradicating infection, reported as high as 95%.1
It is generally accepted for this interstage period to be at least six weeks,7,8 during which the patient is on antibiotics. Following this period, the patient is assessed for eradication of micro-organisms by showing a reduction in acute phase markers like C-reactive protein and possibly culture of joint fluid.7,9
This approach does have certain drawbacks since these procedures are usually performed on older patients, in whom prolonged immobilisation may result in significant morbidity and mortality.1
Other issues include the problems of prolonged hospitalisation, repeated special investigations and repeated theatre procedures, all amounting to greater cost.10 For these reasons, a one-step procedure does seem very attractive.
Surgery should always be coupled with appropriate antimicrobial therapy. This may be particularly difficult due to the heterogeneous nature of these cases. Another compounding factor is that treatment case series have limited numbers, making the establishment of guidelines less statistically significant.
Sepsis of prosthetic hip and knee joints is a rare but significant complication in arthroplasty.3 Currently, there are no large groups described and analysis on causation and management is largely based on meta-analyses of smaller study groups. In this current study, we aim to describe the population characteristics, aetiological agents and corresponding sensitivities in patients managed at Steve Biko Academic Hospital with prosthetic sepsis.
Materials and methods
A retrospective analysis was performed on patients managed at the Steve Biko Academic Hospital, Pretoria, South Africa, from June 2005 to March 2009 (46 months). We retrospectively reviewed a series of 61 patients undergoing either hip (n=45) or knee (n=16) revision arthroplasty. Only patients, in whom microbiological cultures had been performed were included.
Laboratory data in the form of infectious markers (white cell count and C-reactive protein) and culture results with sensitivities at the time of prosthesis removal, and again with any subsequent second debridement, were collected. Cases where organisms of doubtful clinical significance were isolated (e.g. coagulase-negative Staphylococcus) were included as they might act as pathogens in select patient populations.
Results
Patient demographics
During the study period, a total of 75 patients required revision surgery, of whom only 61 were included as no microbiological examination was performed in the remainder. The reasons for this are unclear but may include laboratory errors, sampling problems or the treating surgeon's clinical assessment. Of these, 34 were female, with a male to female ratio of 1:1.2. Ages ranged from 25 to 88 years with a median age of 77 years (summarised in Figure 1).
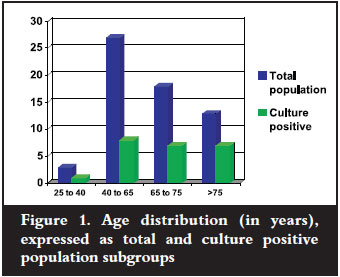
Microbiological data
All microbiological cultures were performed on joint synovium, fluid or deep pus swabs taken from the site intraoperatively.
At the time of revision surgery, 23 patients had positive cultures, rendering 29 isolates (six double infections). Of these, 14 patients had a second subsequent debridement based on the treating surgeon's clinical opinion. Of these 14 patients, 12 had positive cultures, rendering 20 isolates (five double and one triple infection). A significant variety in micro-organisms was isolated, summarised in Table I.
Laboratory data
C-reactive protein levels (CRP) and white cell counts (WCC) were determined in 19 and 23 of the 23 culturepositive cases respectively, and 25 and 36 of the 38 culture- negative cases. WCC did not contribute significantly to the establishment of the diagnosis of infection, as in most cases, the counts were not elevated (see Figure 2).
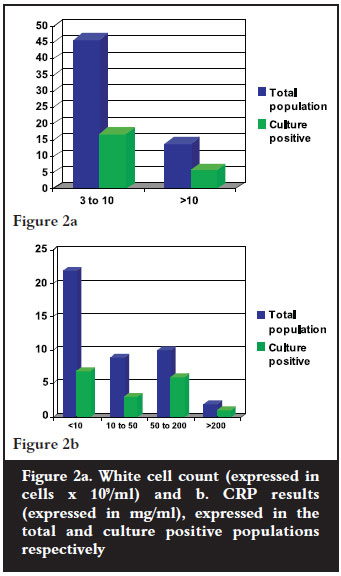
Discussion
Sepsis of the prosthetic hip and knee joints is a rare but significant complication in arthroplasty. Two-stage revision surgery is likely to provide the most consistently successful results.9 An alternative to this is onestage surgery, which is promoted by various authors (particularly in hip arthroplasty1) as having similar outcomes if performed correctly,11,12 but controversy exists.7,13 The option of a one-stage procedure is attractive as it potentially reduces patient morbidity due to prolonged immobilisation,1 and is claimed to be more cost-effective.14
Making the diagnosis of peri-prosthetic infection can be difficult. There is no single diagnostic assay which can provide unequivocal proof of infection,3 and an approach using a combination of tests are typically used. Clinical examination, laboratory examinations (erythrocyte sedimentation rate, C-reactive protein, white cell count and deep tissue cultures) and radiological examinations (radiographs, nuclear and white cell scans) can assist in establishing the diagnosis in prosthesis loosening. Although no single blood investigation can be relied upon to establish the diagnosis, this study showed that CRP levels above 50 mg/ml correlated with joint sepsis in more than 50% of cases, whereas the value of a white cell count was limited. Examination and culture of aspirated joint fluid may provide additional information, but the gold standard in establishing a definitive diagnosis of infection remains deep intraoperative sampling with culture.6,15 The promise of polymerase chain reaction (PCR) testing remains only theoretical.6
Various patient factors may play a role in patient outcome and therefore risk for infection. Immunosuppression16 and advanced age10 have been implicated as major risk factors for complications following major surgery. In the current study, we found that the portion of culture positivity among our population seemed to increase with age. It may therefore be prudent to consider more aggressive therapy in older patients.
The role of microbial virulence in treatment response has also been studied.17,18 It is generally accepted that the success rate of patients infected with so-called low-virulence organisms is higher, but delineation between highand low-virulence organisms have been inconsistent to date.4 In general, Gram-negative organisms, polymicrobial infections, Enterococci and methicillin-resistant Staphylococcus aureus (MRSA) are considered as high virulence organisms.8,18 During the infectious process, the microbes 'compete' with local fibroblasts to establish surface coverage by producing a glycocalyx. This biofilm contains colonies of often sessile bacteria, whose presence can only be detected upon growth overspill into the circulation.6 These organisms are typically significantly more resistant to antimicrobial therapy,19 and use of combination therapies, particularly rifampicin, is advised.1
This improves the bioavailability of the concomitant drug, allowing possible oral administration with comparable serum levels as compared to parenteral therapy.1
This study shows that Staphylococci are still the most common organism isolated in revision arthroplasty. In contrast to international literature, no MRSA was isolated during initial debridements in our population group. From the data collected, the following interesting features were noted:
• There was a significant increase in beta-lactamase production among aetiological agents, increasing from 24% in initial debridements to 83% upon second debridement.
• The portion of Gram-negative organisms increased from 24% to 50% in second cultures.
Various authors advocate the use of vancomycin as empiric antibiotic therapy in revision arthroplasty.16 In this setting, 72% of isolates were sensitive to vancomycin; however, co-amoxyclav also covered 72% of isolates. Although co-amoxyclav does not cover the resistant Staphylococci, it has a broader spectrum, also including certain Gram-negative organisms. The use of co-amoxyclav also has the benefit of superior efficacy, fewer side effects and lower morbidity and mortality as compared to vancomycin.20-22 The concomitant use of rifampicin can further improve the efficacy of co-amoxyclav treatment in eradication of biofilms in prosthesis infection. We suggest the possible use of co-amoxyclav with rifampicin as a potential first-line empiric therapy in our clinical setting. Multi-drug resistance is increasingly important in requiring secondary debridements. In this clinical setting, a combination of carbapenems with vancomycin can be justified, as it covered 75% of organisms.
References
1. Bernard L, et al. Trends in the treatment of orthopaedic prosthetic infections. JAC 2004;53:127-9. [ Links ]
2. Wroblewski B, Siney P, Fleming P. Charnley low-frictional torque arthroplasty in patients under the age of 51 years. Follow-up to 33 years. J Bone Joint Surg. 2002;84B:540-3. [ Links ]
3. Mihalko W, et al. Diagnosis and treatment of the infected primary total knee arthroplasty [Abstract]. Instr Course Lect 2008;57:327-39.
4. Kilgus D, Howe D, Strang A. Results of periprosthetic hip and knee infections caused by resistant bacteria. Clinical Orthopaedics and Related Research 2002;404:116-24. [ Links ]
5. Tsukayama D, Estrada R, Gustilo R. Infection after total hip arthroplasty: a study of treatment of one hundred and six infections. J Bone Joint Surg 1996;78:512-23. [ Links ]
6. Ip D, Yam S, Chen C. Implications of the changing pattern of bacterial infections following total joint replacements. Journal of Orthopaedic Surgery 2005;13(2):125-30. [ Links ]
7. Moyad T, Thornhill T, Estok D. Evaluation and management of the infected total hip and knee. Orthopedics 2008;31(6):581-8. [ Links ]
8. Garvin K, Hanssen A. Current concepts review: Infection after total hip arthroplasty. J Bone Joint Surg [Br] 1995;77A:1576-88. [ Links ]
9. Mont M, Waldman B, Hungerford D. Evaluation of preoperative cultures before second-stage reimplantation of a total knee prosthesis complicated by infection. J Bone Joint Surg 2000;82A:1552-57. [ Links ]
10. Santaguida P, et al. Patient characteristics affecting the prognosis of total hip and knee joint arthroplasty: a systematic review. J Can Chir 2008;51(6):428-36. [ Links ]
11. Wroblewski B. One-stage revision of infected cemented total hip arthroplasty [Abstract]. Clin Orthop 1986;211:103-10. [ Links ]
12. Ure K, et al. Direct-exchange arthroplasty for the treatment of infection after total hip replacement. J Bone Joint Surg Am 1998;80:961-8. [ Links ]
13. Krasin E, et al. Could irrigation, debridement and antibiotic therapy cure an infection of a total hip arthroplasty? J Hosp Infect 2001;47:235-8. [ Links ]
14. Fisman D, et al. Clinical effectiveness and cost-effectiveness of 2 management strategies for infected total hip arthroplasty in the elderly. Clin Infect Dis 2001;32:419-30. [ Links ]
15. Windsor R, et al. Two-stage reimplantation for the salvage of total knee arthroplasty complicated by infection. J Bone Joint Surg [Am] 1990;72:272-8. [ Links ]
16. Segawa H, et al. Infection after total knee arthroplasty. A retrospective study on the treatment of eighty-one infections. J Bone Joint Surg [Am] 1999;81(10):1434-45. [ Links ]
17. Fitzgerald R. Infections of hip prostheses and artificial joints. Infect Dis Clin North Am 1989;3:329-38. [ Links ]
18. Hanssen A, Rand J. Evaluation and treatment of infection at the site of a total hip or knee arthroplasty. J Am Geriatr Soc 1998;80A:910-22. [ Links ]
19. Costerton J, et al. Microbial biofilm. Annu Rev Microbiol 1995;49:711-45. [ Links ]
20. Stryjewski M, et al. Use of vancomycin or first-generation cephalosporins for the treatment of hemodialysis-dependent patients with methicillin-susceptible Staphylococcus aureus bacteremia. CID 2007;44(15 January):190-6. [ Links ]
21. Stevens D. The role of vancomycin in the treatment paradigm. CID 2006;42(Suppl 1):S51-57. [ Links ]
22. Khatib R, et al. Impact of initial antibiotic choice and delayed appropriate treatment on the outcome of Staphylococcus aureus bacteremia. Eur J Clin Microbiol Infect Dis 2006;25:181-5. [ Links ]
 Correspondence:
Correspondence:
Dr CH Snyckers
Department Orthopaedic Surgery University of Pretoria
Tel: (012) 354-2851 Fax: (012) 354-2821
Email: csnyckers@mighty.co.za
This article is the sole work of the authors. No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article although a grant has been applied for.














