Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.9 no.2 Centurion ene. 2010
CASE REPORT AND REVIEW OF THE LITERATURE
Isolated loss of flexor pollicis longus function after plating of the radius
R SalkinderI; Dr E LiebenbergII
IMBChB(UCT) Registrar, Department of Orthopaedic Surgery, University of Stellenbosch
IIMBChB, MMed(Orth), FC(Orth)SA Head of Orthopaedics: Paarl Provincial Hospital
ABSTRACT
A patient presented with an open midshaft radius and ulna fracture which was treated with debridement and open reduction and internal fixation using the LC-DCP technique. Postoperatively the patient had isolated loss of flexor pollicis longus function which recovered fully after 10 weeks with a 'wait-and-see' policy. An isolated traction neuropraxia of the branch of the anterior interosseous nerve to the flexor pollicis longus muscle is the presumed cause.
Introduction
Isolated loss of flexor pollicis longus (FPL) function after plating of a midshaft radius fracture is a rare complication. The presumed aetiology is thought to be a traction neuropraxia of the branch of the anterior interosseous nerve (AIN) supplying the muscle. We report such a case where full recovery occurred after a period of 10 weeks post surgery.
Case report
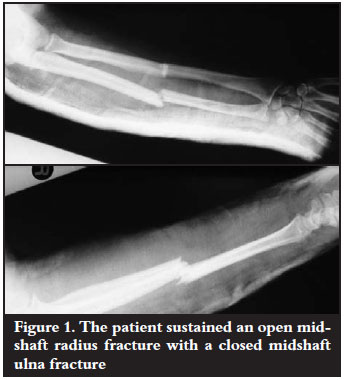
An 18-year-old female was referred to the trauma unit after being assaulted with a blunt object. She sustained a Gustilo and Anderson grade 2 open midshaft radius fracture with a closed midshaft ulna fracture (Figure 1). She presented with a swollen and deformed right mid-forearm with a 2 cm wound dorsally over the radius. Initially a debridement of the wound and fracture was performed. On initial assessment and post debridement evaluation she had full function of all muscles of her forearm and hand including FPL.
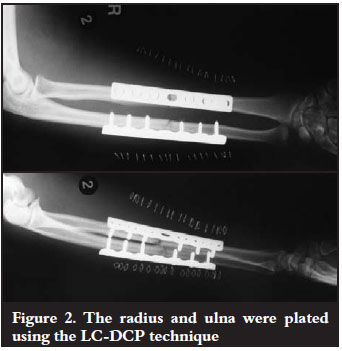
Plating of both the radius and ulna using the LC-DCP (Limited Contact Dynamic Compression Plating) technique was subsequently done (Figure 2). The Henry's volar surgical approach was used for the radius and the posterior approach for the ulna. She was diagnosed as having isolated but complete loss of FPL function on day 1 post surgery. The surgeon was confident that the FPL muscle and tendon was in continuity and not ruptured or caught underneath the plate. The clinical test described by BS Mody1 and explained later in the article confirmed this. The patient was treated conservatively for the loss of muscle function. Full recovery was noted after 10 weeks.
Discussion
Plate osteosynthesis of forearm fractures is the preferred method of fixation of many authors in order to obtain an anatomical reduction and rigid fixation, and to permit early mobilisation. The LC-DCP technique makes use of a plate designed with a grooved undersurface which minimises the disruption of periosteal blood supply to the bone and fracture site; it also has specially designed holes which allow bidirectional compression. Both these features permit quicker healing of the fracture. By using Henry's volar surgical approach, the risk of trauma to the AIN is a rare complication. In fact in large published reports, neurological injuries are not even mentioned as a complication of radius plating.2 A more commonly reported complication is posterior interosseous nerve injury following proximal radius osteosynthesis. Our literature search revealed only 11 cases of isolated AIN injury to the FPL muscle following radius plating, eight of which had full recovery with conservative management.3-5
In most cases of AIN injury following radius plating, an isolated loss of FPL function is described as opposed to the loss of function of all three muscles supplied by the nerve. The anatomy of the nerve as documented by a postmortem study by Griffiths3 and Spinner4 and highlighted below is most likely to be the explanation.
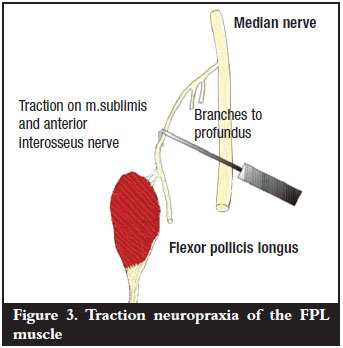
The AIN is the largest branch of the median nerve. It arises from its radial aspect, 5-8 cm distal to the level of the lateral condyle, and passes between the two heads of pronator teres. It runs along the volar surface of flexor digitorum profundus and then passes between flexor digitorum profundus and FPL on its way to pronator quadratus. It innervates the three muscles mentioned: FPL, flexor digitorum profundus to the index and middle digits, and pronator quadratus. Between one and six motor branches to FPL arise from the AIN just 4 cm distal to its origin and enter the muscle in its proximal third, and run obliquely from medial to lateral. These branches are taut in supination. In contrast, the branches to flexor digitorum profundus run more parallel with the median nerve. When a soft tissue retractor is used, the flexor digitorum superficialis together with the median nerve is retracted medially. This causes a traction neuropraxia of the FPL muscle due to the oblique nature of the fibres supplying it while the more parallel fibres to flexor digitorum profundus are relatively protected3-4 (Figure 3).
Other aetiologies have also been described including postoperative compression neuropraxia caused by haematomas and oedema;5 extensive stripping of the FPL muscle;5 and crush neuropraxia.
Haematomas and oedema causing a compression neuropraxia are more likely to present from the second postoperative day onwards.5
Extensive stripping of the muscle belly is sometimes unavoidable, but according to the literature, the time to recovery following muscle inhibition secondary to operative trauma is never longer than five weeks.5
Many authors recommend that stripping of the FPL muscle belly be done in a subperiosteal fashion and from a radial to ulna direction. This prevents the FPL branches of the AIN as well as the main AIN trunk from being trapped under the plate or under the bone-holding forceps causing a crush neuropraxia as demonstrated by a cadaveric study performed by Hope.6 Added to this, subperiosteal stripping allows the FPL muscle to fall medially thereby releasing the tension on the nerve.4
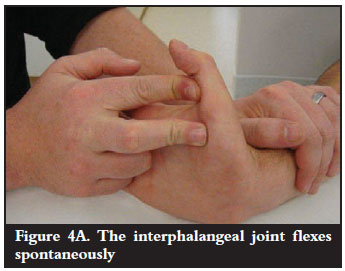
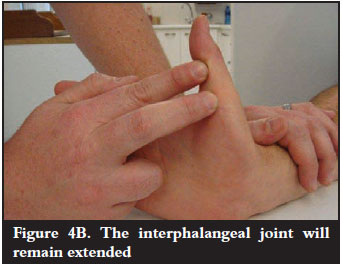
The clinical test described by Mody1 is a useful test to differentiate between AIN paralysis and a disrupted muscle or tendon. The examiner dorsiflexes the palm with his/her own middle, ring and little fingers. He/she then hyperextends the thumb at the carpometacarpal and metacarpophalangeal joints with his/her own index finger. In the case of the FPL tendon being paralysed (but in continuity) through an AIN injury, the interphalangeal joint flexes spontaneously (Figure 4A). Conversely, if the tendon is ruptured, the interphalangeal joint will remain extended (Figure 4B).
Nerve conduction studies done to pinpoint the lesion are of little value and are often falsely negative. Seror pointed out that interpretation of the nerve conduction studies requires considerable expertise and that often the nerve is reported as being intact due to the fact that the other muscles being supplied by the median nerve retain their latency and mask the anterior interosseous lesion.7
Conclusion
Iatrogenic injury to the FPL branch of the AIN is a rare complication following radius plating. The most likely cause is a traction neuropraxia caused by soft tissue retractors placing excessive force on the oblique nature of the nerve branches supplying it. Subperiosteal stripping from a radial to ulna direction protects the AIN from a crush injury as well as decreasing the tension on the specific branches to the FPL muscle. A thorough preoperative examination is recommended with specific testing of the FPL function. If an isolated loss of FPL function is diagnosed postoperatively and the tendon and muscle are deemed to be intact, an initial conservative approach is recommended before any nerve exploration or tendon transfer procedure is undertaken.
References
1. Mody BS. A simple clinical test to differentiate rupture of flexor pollicis longus and incomplete anterior interosseous paralysis. J Hand Surgery Br 1992;17B:513-4. [ Links ]
2. Stern PJ, Drury WJ. Complications of plate fixation of forearm fractures. Clin orthopaedics and related research 1983;175:25-9. [ Links ]
3. Griffiths JC. Nerve Injuries after plating of forearm bones. British Medical Journal 1966;2:277-9. [ Links ]
4. Spinner M. The anterior interosseous nerve syndrome: with special attention to its variations. J Bone and Joint Surgery Am. 1970;52:84-94. [ Links ]
5. Keogh P, Khan E, Cooke E, McCoy G. Loss of flexor pollicis longus function after plating of the radius: Report of 6 cases. J of Hand Surgery Br 1997;22B:375-6. [ Links ]
6. Hope PG. Anterior interosseous nerve palsy following internal fixation of the proximal radius. J Bone and Joint Surgery Br 1988;70B:280-2. [ Links ]
7. Seror P. Anterior interosseous nerve lesions. Clinical and electrophysiological features. J Bone and Joint Surgery Br 1996;78B:238-41. [ Links ]
 Reprint requests:
Reprint requests:
Dr R Salkinder
B44 Punta Del Mar Milton Road Sea Point 8005
Cell: 082 9018 700
Email: rsalkinder@yahoo.com
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of the article.














