Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.9 n.2 Centurion Jan. 2010
CLINICAL ARTICLE
Orthopaedic implications of physeal arrest following meningococcal septicaemia
J-P du PlessisI; S Dix-PeekII; CJ HastingsIII; SB LootsIV; EB HoffmanV
IMBChB Registrar, Department of Orthopaedics, University of Cape Town, From the Maitland Cottage Paediatric Orthopaedic Hospital, Cape Town
IIFCS(SA) Orth, MMed (Orth) Consultant Orthopaedic Surgeon, Department of Orthopaedic Surgery, University of Cape Town, From the Maitland Cottage Paediatric Orthopaedic Hospital, Cape Town
IIIFCS(SA) Orth Orthopaedic Surgeon, Vincent Pallotti Hospital, Cape Town, From the Maitland Cottage Paediatric Orthopaedic Hospital, Cape Town
IVFCS(SA) Orth Orthopaedic Surgeon, Chris Barnard Memorial Hospital, Cape Town, From the Maitland Cottage Paediatric Orthopaedic Hospital, Cape Town
VFCS(SA) Orth Associate Professor, Department of Orthopaedic Surgery, University of Cape Town, From the Maitland Cottage Paediatric Orthopaedic Hospital, Cape Town
ABSTRACT
BACKGROUND: Physeal arrest following meningococcal septicaemia is the result of ischaemia secondary to vasculitis. Only two cases have been reported with a long-term follow-up to maturity.
METHODS: We did a retrospective study of 13 patients treated over 17 years (1991-2007) to assess the orthopaedic manifestations, treatment and long-term outcome of the physeal arrest. All patients were followed up clinically and radiologically; eight to skeletal maturity.
RESULTS: The average age of the meningococcal septicaemia was 12 months, and the patients presented with physeal arrest at an average of 5.6 years. Thirty-nine physes were involved: 29 focal, six complete and four had a premature arrest. Sixty two surgical procedures (average 4.6, range 1-11 per patient) were required to prevent or correct angular deformity and/or leg length discrepancy. Seven physeal bars were resected (four successfully), 26 epiphyseodeses, 20 angular corrections (all at the knee or ankle) and nine limb lengthenings were done.
CONCLUSIONS: We concluded that these patients may require several orthopaedic procedures, and should be followed up until skeletal maturity. Once growth is balanced with bar resection or epiphyseodesis, angular correction and limb lengthening have a good outcome.
Introduction
Since the earliest report of bony deformities and growth abnormalities following meningococcal septicaemia in 1981,1 there has been a steady increase in these complications reported in the literature. There have however, been few reports on the surgical management of physeal arrest in this setting and the late outcome of this surgery.2
Meningococcal septicaemia is caused by Neisseria meningitidis, a Gram-negative diplococcus with a lipopolysaccharide in its cell wall.3,4 This acts as an endotoxin to elicit an acute inflammatory response via a complex cascade of events ending in vasculitis, disseminated intravascular coagulopathy (DIC), shock and multi-organ failure with a mortality ranging from 7 to 15%.5,6 The DIC and vasculitis affect all organ systems and the musculoskeletal system is not spared. Clinically this may present as skin necrosis, compartment syndrome and gangrene, resulting in amputations and soft tissue contractures.
Physeal injury occurs in 13 to 21% of patients5,7 as a result of ischaemia secondary to vasculitis and to a lesser extent as a result of osteomyelitis. This has been shown on histological specimens taken at the time of amputation from patients with the acute illness.4,8 Although the osteomyelitic involvement of bone (epiphysis, metaphysis and diaphysis) usually recovers without sequelae, damage to the physis leads to permanent physeal arrest.4,8 This manifests in three different patterns: focal or partial(central or asymmetrical), complete or premature arrest. 4,8,9,10
As the manifestations of physeal damage are growth-dependent they may only present years after the index infection.1,2,4,5,7-12 Surgical correction of these deformities is difficult and complicated by a high incidence of failure of physeal bar resection and recurrence of the deformities after correction.2,4
The management of the initial limb ischaemia, with or without fasciotomy, and the treatment of skin necrosis and soft tissue contractures, has been well described in the orthopaedic literature.2,6,13 The problems associated with amputations (especially below knee), such as stump overgrowth and contractures, often necessitating through-knee amputations, is also well documented.2,4,6
A multicentre study by Belthur et al,2 described the late orthopaedic sequelae due to growth plate arrest in 23 patients, but only two were followed up to skeletal maturity. The purpose of our retrospective study was to describe the orthopaedic manifestations and treatment of growth plate arrest and the long-term outcome in 13 patients (eight to maturity) following meningococcal septicaemia.
Methods
We retrospectively studied the orthopaedic manifestations, treatment and outcome of growth plate arrest following meningococcal septicaemia in 13 patients treated over 17 years (1991-2007).
Their clinical and operative notes, radiographs and MRI scans were reviewed. The degree and type of physeal involvement was assessed on A-P and lateral radiographs. If this was not clear, or if growth plate resection was contemplated, biplanar tomography (initially) and/or MRI (now the gold standard to assess physeal arrest) was done.
All patients are followed up annually both clinically and radiologically; eight of the 13 patients until skeletal maturity. An outcome was regarded as good if leg length discrepancy (LLD) was < 2 cm and the mechanical axis alignment did not exceed 5º.
The Wilcoxon rank sum test was used to test the significance of increased physeal arrest in children who had septicaemia before 10 months of age.
The study was aimed at the management of physeal arrest and therefore problems related to soft tissue contractures, scarring or amputations were not reviewed.
Results
The patients presented to the orthopaedic department at an average age of 5.6 years (range 3-12 years).They presented with leg length discrepancy and/or angular deformities of the limbs.
The average age of meningococcal septicaemia was 12 months (range 3-24 months). Seven of the children were over 10 months of age when they had the acute illness and had an average of 1.7 physes involved per child (range 1-3). Six of the children were under the age of 10 months and had an average of four physes involved per child (range 2-5). This is statistically significant (p<0.05).
Classification and distribution of physeal arrest
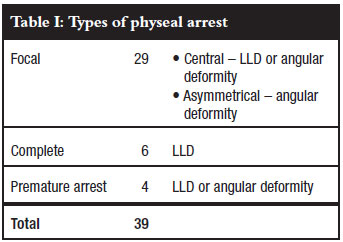
The 13 patients had a total of 39 physes involved; an average of three per patient (range 1-5). Twenty-nine physeal arrests were of the focal type, six were complete and four were premature physeal arrests (Table I).
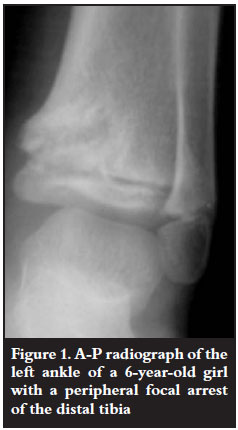
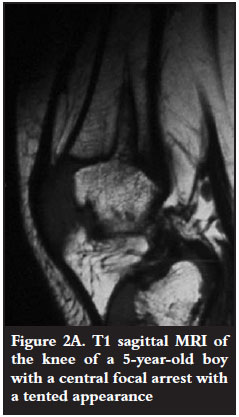
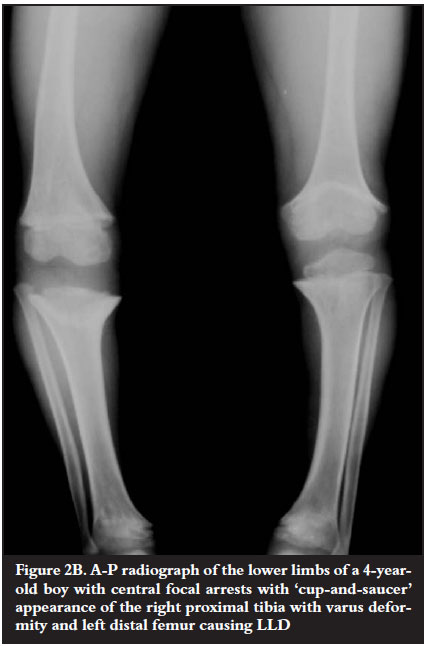
Asymmetrical, peripheral focal arrest resulted in angular deformity (Figure 1). Central focal arrest was either 'tented' (Figure 2A) or had a 'cup-and-saucer' appearance (Figure 2B). Central focal arrest presented with either LLD or an angular deformity (Figure 2B).
The study was aimed at the management of physeal arrest
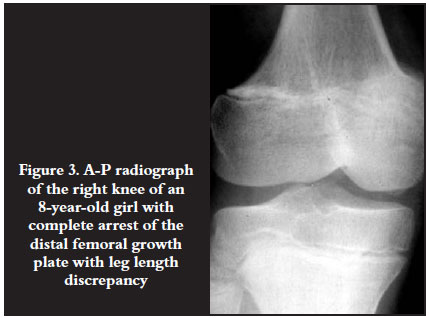
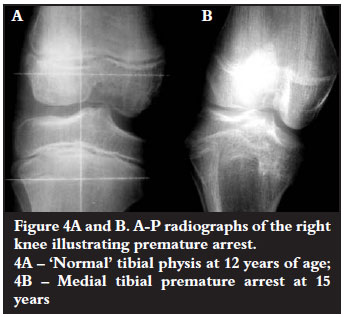
Complete arrest presented as a LLD (Figure 3). Premature arrest occurred when a documented seemingly normal physis arrested before skeletal maturity. This presented as LLD or an angular deformity, depending whether the arrest was symmetrical or asymmetrical (Figures 4A and B).
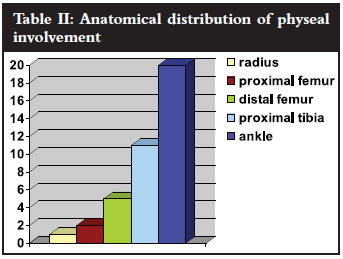
The anatomical distribution is shown in Table II. The vast majority of physeal arrests occurred around the knee and in the ankle with only three of the 39 occurring in the proximal femur or upper limb.
Surgical procedures
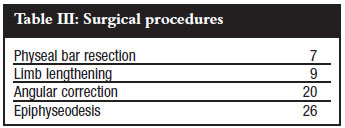
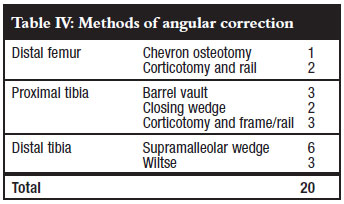
Sixty-two surgical procedures were performed at an average of almost five per patient (range 1-11). Seven physeal bars were resected, 26 epiphyseodeses were done, 20 osteotomies were performed for angular deformities and nine limb segments lengthened (Table III).

Epiphyseodesis
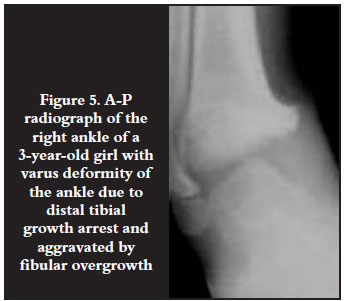
Of the 26 epiphyseodeses done, 18 were performed around the ankle (either distal tibia or fibula). In three cases the epiphyseodesis was done on the contralateral side to address limb length discrepancy. Twenty-five of these procedures successfully arrested growth. The one failure was an epiphyseodesis of the distal tibia in which the growth was not arrested and the angular deformity worsened. Fourteen of the 26 epiphyseodeses were done in the fibula (11 distal and three proximal) to address the inequality of growth between tibia and fibula (Figure 5).
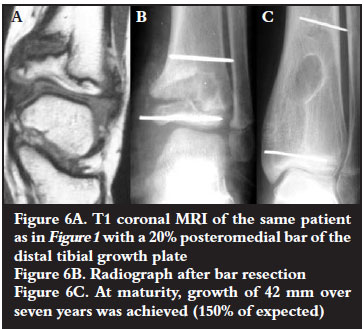
Physeal bar resection
Seven physeal bars were resected. Resection was considered successful if the growth rate postoperatively resumed > expected rate for that physis (Figures 6 A, B and C). Four (57%) of the resections were successful. The four physeal bars that were successfully resected were less than 30% of the physeal surface area. The three failures were 40% of the physeal area.
Correction of angular deformity
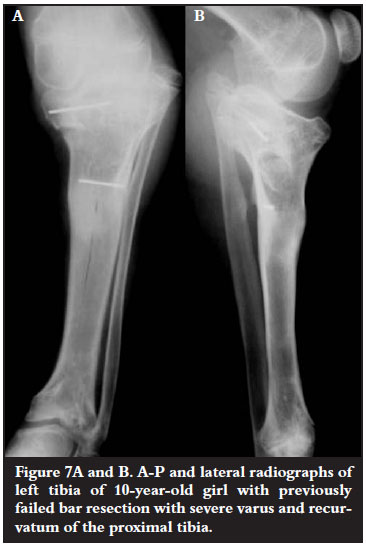
All of the 29 focal arrests occurred around the knee and ankle. Of these 27 resulted in a varus and only two in a valgus deformity. Angular correction was undertaken in 20 cases; the other nine were corrected with either successful epiphyseodesis (especially distal fibular epiphyseodesis for ankle varus) or physeal bar resection. Successful correction was defined as postoperative correction to < 5º of the normal mechanical axis. Nineteen of the 20 angular corrections were successful. A problematic pattern of deformity around the knee was that of severe varus and recurvatum of the proximal tibia. This deformity was particularly difficult to correct and our one failure occurred in this group (Figures 7A and B).
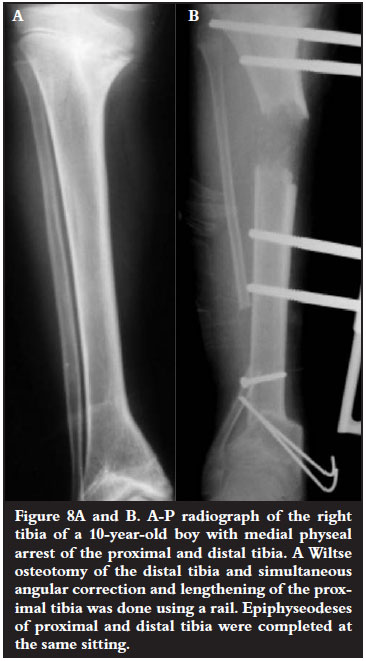
Different techniques were used with similar results (Table IV). At the distal tibia however, we now routinely use the osteotomy described by Wiltse14 as it centralises the talus under the tibia (Figures 8A and B). Five limb segments had simultaneous lengthening using either a rail (Orthofix) or circular frame (Taylor spatial frame) (Figures 9A-E).
Limb lengthening
Nine limb segments were lengthened: five tibiae, three femurs and one radius. Three femurs and three tibiae were lengthened with a rail (Orthofix) (Figures 10A-C); two tibiae with a Taylor spatial frame; and the radius with an Ilizarov circular frame. The average length gained was 5.8 cm with a range of 3.2-9.3 cm. A successful lengthening was defined as lengthening to within 1 cm of the pre-operative target.
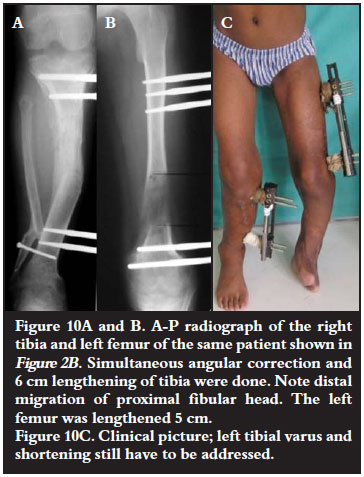
All three tibiae lengthened with a rail had distal migration of the fibular head (Figure 10A).This did not have any clinical significance.
Follow-up
Eight of the 13 patients had reached skeletal maturity at the time of this study and we were able to follow up seven; six had a good result. One patient had residual bilateral ankle varus but copes well clinically.
Discussion
Physeal arrest is caused by ischaemic occlusion of the microvasculature supplying the physis, and to a lesser degree the acute inflammatory response as a result of metaphyseal osteomyelitis. Histological examination of the physis of an acute amputation specimen of a meningococcaemic patient showed areas of disorganisation with loss of the normal columnar pattern of the chondrocytes and relative hypocellularity. The adjacent metaphyseal bone showed a prominent inflammatory infiltrate (acute osteomyelitis). Later specimens taken at revision amputation showed complete recovery of the osteomyelitis, but the ischaemia resulted in bony bridge formation and/or growth plate arrest. These findings were initially reported by Grogan, Love, Ogden et al (1989).4 Other authors reported similar findings.8
We found a significantly higher incidence of growth arrests in patients who had meningococcal septicaemia before the age of 10 months. This concurs with the findings of Buysse, Oranje, Zuidema et al (2009) who suggested that this was probably due to the higher vulnerability of the bony vasculature in younger patients.15
The physeal injuries, being growth-dependent, present later than the bony changes seen in the acute phase of the illness.1,2,4,5,7-12 Patients in our study presented at an average of 4.6 years following the acute illness, with a range of 3-12 years of age at presentation, indicating the unpredictability of this pathological process. This stresses the need for follow-up to skeletal maturity of all these patients.
Classification and anatomical distribution
Complete arrest resulted in limb length discrepancy. Focal arrest resulted in angular deformity if asymmetrical and if symmetrically central, resulted in leg length discrepancy. The central arrests had either a tented appearance (Figure 2A) or are shaped like a 'cup-and-saucer' or 'ball-and-socket' (Figure 2B) as described by Robinow, Johnson, Nanagas et al.10 They postulate that this appearance may be due to two reasons. The centre of the growth plate is more vulnerable than the periphery which receives anastomoses from periosteal vessels. Occlusion of the transphyseal vessel, which exists in infants under one year of age, damages the physis and metaphysis with a resultant cup-shaped appearance.
Premature arrest resulted in either leg length discrepancy or angular deformity depending on their site. They occur in a diffuse irregular pattern in physes previously documented to be normal on radiographic examination. Grogan et al4 suggest that excessive undulation of a growth plate may be a warning sign. This is not our experience (Figures 4A and B), but earlier MRI studies may show small areas of physeal arrest not obvious on radiographs.
The deformities seen in the patients in our study occurred with a similar distribution to those reported in the literature.1,2,4,5,7-12 The majority of arrests (36/39) occurred around the knee and ankle. Only one patient had an upper limb growth arrest (distal radius) which was complete. The reason for the increased incidence in the lower limbs remains unclear.
Bache and Torode5 reported a propensity for skin necrosis around the anteromedial aspect of the knee and that nearly half of the patients requiring debridement and grafting developed growth arrest. They suggest that the high incidence of proximal tibial physeal arrest could be due to the anterior compartment of the leg having a vascular supply from one angiosome only, making the tissues more susceptible to ischaemia.
Treatment
These patients may require several orthopaedic procedures. In our study group 62 surgical procedures were performed on 13 patients, an average of nearly five per patient and as many as 11 in one. Two of these patients are still awaiting further corrective osteotomies and lengthening procedures.
Procedures performed were classified into two broad groups. They were either growth-balancing procedures (epiphyseodesis or physeal bar resection) or salvage procedures (angular correction or leg lengthening). An important point is that salvage procedures should not be undertaken in the presence of unbalanced growth.Procedures from both groups can be done at the same time, but if growth is not balanced the deformities will recur. This was also noted by Belthur et al2 who found that they had a higher recurrence of angular deformities after correction around the knee (when epiphyseodeses were not performed) than at the ankle (when they were). In our study epiphyseodesis or successful bar resection preceded angular correction and/or leg lengthening. There was no recurrence of angular deformity or leg length discrepancy in those patients followed to skeletal maturity.
Epiphyseodesis
The most commonly performed procedure was epiphyseodesis; most commonly performed around the ankle. It was performed for three reasons: to balance the growth in a limb affected by an asymmetrical focal arrest; on the contralateral limb to address limb length discrepancy; or on the proximal or distal fibula to address fibular overgrowth when the adjacent tibial physis was affected. Early epiphyseodesis to balance growth is preferable to the severe angular deformities which may result if it is delayed.
Physeal bar excision
In this study physeal bar excision was unpredictable. Only four (57%) of our seven excisions were successful. Grogan et al4 reported similar results, and Belthur et al2 attempted three resections without success.
Although a discrete bar is radiologically identifiable, one cannot presume that the rest of the growth plate is healthy and there may be a more 'diffuse involvement'. 2,5 Whether this 'diffuse involvement' is detectable as small areas of arrest on MRI is currently being investigated. Similar factors are probably responsible for premature arrest in a previously 'normal' growth plate. Because of the inevitable failure of bar resection in this study where more than 30% of the physeal area was involved, our current policy is to attempt bar resection only if the arrest is <30%, the rest of the growth plate is normal on MRI, and the patient has more than five years of growth remaining.16
Correction of angular deformity
A high recurrence rate of angular deformity following corrective osteotomy has been reported in the literature, and is attributed to failure to complete the epiphyseodesis at the same time.2 This study has shown that if balanced growth is achieved, with completion of epiphyseodesis or with successful physeal bar excision, alignment is maintained.
All 20 angular corrections were at the knee (11) or ankle (9). The vast majority (18) were in varus.
A problematic pattern of deformity was that of severe proximal tibial recurvatum and varus. This has been shown by Grogan et al4 to be due to involvement of the anterior part of the epiphysis of the proximal tibia. This was a particularly difficult deformity to correct and our one failure occurred in such a patient due to peroneal nerve palsy.
Ankle varus
Ankle deformity was varus in seven of eight patients. This was due to focal arrest of the distal tibia with resultant fibular overgrowth. Fibular growth arrests were far less common than in the tibia. The growth arrest in the distal tibia was mainly of the 'cup-shaped' central type described by Robinow et al10 and should have resulted in leg length discrepancy, but fibular overgrowth caused or contributed to a varus deformity (Figure 5).
Belthur et al2 and Bache et al5 showed that early fibular epiphyseodesis prevented ankle varus. In late presenters with established varus, a valgus osteotomy should be done at the same time as the fibular epiphyseodesis. In some late presenters, although the talus was tilted in varus, it was centralised on the tibia. As the foot was well aligned a fibular epiphyseodesis only was required. At long-term follow-up these patients were coping well with a 'ball-and-socket' appearance of the ankle joint (Figure 11).
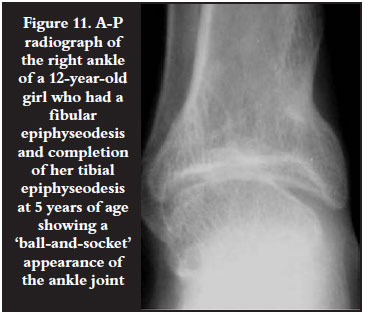
Limb lengthening
Limb lengthening had good results. A complication noted during lengthening of the tibia was that of distal migration of the proximal fibular head (Figure 10A). This occurred as a result of premature union of the distal fibular osteotomy. This had no clinical significance.
Loss of range of motion of adjacent joints is a common complication in lengthening procedures and we stopped lengthening if less than 30º of flexion was achievable at an adjacent joint. Although we noted loss of motion in all patients during lengthening, no lengthenings had to be abandoned and all patients regained full range of motion postoperatively (Figure 9E).
References
1. Fernandez F, Pueyo I, Jimenez JR, Vigil E, Guzman A. Epiphyseometaphyseal changes in children after severe meningococcic sepsis. AJR 1981;136:1236-8. [ Links ]
2. Belthur MV, Bradish CF, Gibbons PJ. Late orthopaedic sequelae following meningococcal septicaemia. J Bone Joint Surg (Br) 2005;87-B:236-40. [ Links ]
3. Feigin RD. Infections due to Neisseriae. In: Behrham RE, Vaughn VC, Nelson WE (eds). Nelson Textbook of Pediatrics, 13th edition. Philadelphia: W.B. Saunders Company;1987:589-1. [ Links ]
4. Grogan DP, Love SM, Ogden JA, Millar EA, Johnson LO. Chondro-osseous growth abnormalities after meningococcemia. A clinical and histopathological study. J Bone Joint Surg (Am) 1989;71-A:920-8. [ Links ]
5. Bache CE, Torode IP. Orthopaedic sequelae of meningococcal septicemia. J Pediatr Orthop 2006;26:135-9. [ Links ]
6. Wheeler JS, Anderson BJ, De Chalain TMB. Surgical interventions in children with meningococcal purpura fulminans - A review of 117 procedures in 21 children. J Pediatr Surg 2003;38:597-603. [ Links ]
7. Santos E, Boavido JE, Barroso A, Seabra J, Carmona da Mota H. Late osteoarticular lesions following meningococcemia with disseminated intravascular coagulation. Pediatr Radiol 1989;19:199-202. [ Links ]
8. Loots SB, Davies JQ, Hastings CJ, Hoffman EB. Physeal arrest following meningococcaemia. Paper presented at the SAOA meeting in Durban September 2000. [ Links ]
9. Appel M, Pauleto AC, Cunha LA. Osteochondral sequelae of meningococcemia: Radiographic aspects. J Pediatr Orthop 2002;22:511-6. [ Links ]
10. Robinow M, Johnson FG, Nanagras MT, Mesghali H. Skeletal lesions following meningococcemia and disseminated intravascular coagulation. Am J Dis Child March 1983;137:279-81. [ Links ]
11. Barre PS, Thompson GH, Morrison SC. Late skeletal deformities following meningococcal sepsis and disseminated intravascular coagulation. J Pediatr Orthop 1985;5:584-8. [ Links ]
12. O'Sullivan ME, Fogarty EE. Distal tibial physeal arrest: A complication of meningococcal septicemia. J Pediatr Orthop 1990;10:549-50. [ Links ]
13. Davies MS, Nadel S, Habibi P, Levin M, Hunt DM. The orthopaedic management of peripheral ischaemia in meningococcal septicaemia in children. J Bone Joint Surg (Br) 2000;82-B:383-6. [ Links ]
14. Wiltse LL. Valgus deformity of the ankle. A sequel to acquired or congenital abnormalities of the fibula. J Bone Joint Surg (Am) 1972;54-A:595-604. [ Links ]
15. Buysse MP, Oranje AP, Zuidema E, Hazelzet JA, Hop WCJ, Diepstraten AF, Joosten KFM. Long-term skin scarring and orthopaedic sequelae in survivors of meningococcal septic shock. Arch Dis Child 2009;94:381-6. [ Links ]
16. Hobbs HR, Dix-Peek S, Dunn RN, Wieselthaler N, Hoffman EB. Physeal bar resection for partial growth arrest. SA Orthopaedic Journal 2007;6:52-60. [ Links ]
 Correspondence to:
Correspondence to:
Professor EB Hoffman
7 Marne Avenue 7700 Newlands
Cape Town South Africa
Tel: +27 21 674 2090 Fax: +27 21 683 0691
E-mail: info@mch.org.za
This article is the sole work of the authors. No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
This study has been approved by the Research Ethics Committee of the University of Cape Town. Rec Ref: 347/2009














