Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SA Orthopaedic Journal
versión On-line ISSN 2309-8309
versión impresa ISSN 1681-150X
SA orthop. j. vol.9 no.2 Centurion ene. 2010
CASE REPORT AND REVIEW OF THE LITERATURE
Lumbar osteochondroma causing spinal compression
M ThiartI; H HerbstII
IMBChB, Medical Officer, Department of Orthopaedic Surgery, Worcester Hospital
IIMBChB, MMed(Orth), FC(Orth)SA, Part-time Consultant, Department of Orthopaedic Surgery, Worcester Hospital
Osteochondromas found in the vertebral column are rare; those in the lumbar spine even more so. We discuss a case of an osteochondroma in the lumbar spine causing spinal compression - giving symptoms of weakness in the right leg, and in the L5 and S1 distribution. These symptoms are usually associated with a disc lesion.
Case report
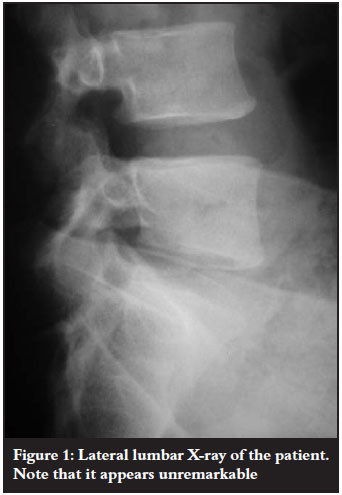
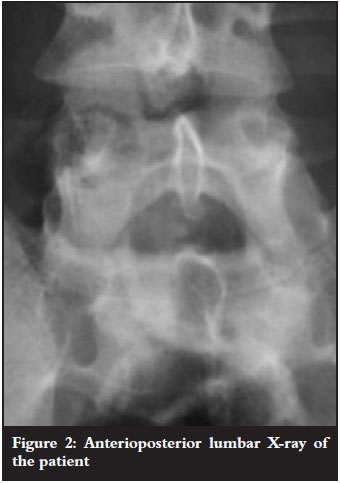
JM, a 37-year-old male, presented to our clinic with progressive weakness in the left leg of a few months' duration. The lumbar X-rays revealed no abnormalities (Figures 1 and 2). On examination, there was weakness in the L5 and S1 distribution on the right side. Our initial diagnosis was that of a disc lesion and an MRI was ordered.
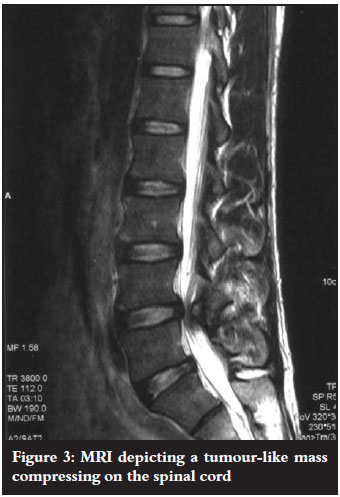
The MRI revealed a mineralised bony mass protruding from the lamina of the vertebral body of L4 with a cortical edge compressing the L5 and S1 right spinal roots. Cauda equina was present (Figures 3-7).
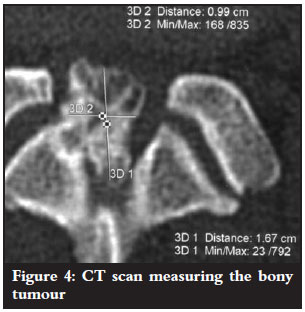
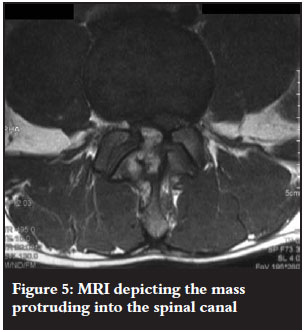
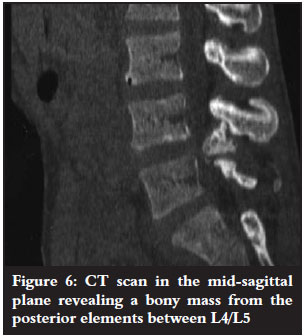

The bony mass had a cartilage cap and the tentative diagnosis of an osteochondroma was made. The patient was not known to have any other exostoses.
Intra-operatively a bony mass with a cartilage cap was found, compressing the L5 and S1 spinal root. The mass was excised and sent for histology. A laminectomy was done.
The histology confirmed an osteochondroma.
Discussion
Of all spinal tumours, 70% of primary bone tumours are benign. These include osteoid osteomas, osteoblastomas, giant cell tumours, osteochondromas, aneurysmal bone cysts, eosinophilic granulomas and fibrous dysplasias.1
Osteochondromas (also known as osteocartilaginous exostoses)2 encompass 10-15% of all bone tumours3 and 36% of all benign bone tumours.4 Primary tumours of the spine are relatively infrequent when compared to lymphoma of the spine, myeloma and multiple myeloma.5
Osteochondromas are solitary (often) and are cartilaginous bony growths, usually appearing in relation to the epiphyseal growth plate.6 They can be pedunculated or sessile exophytic growths. Marrow and cortical continuity with the underlying parent bone defines the lesion.3 They are thought to arise as a metaplastic cartilage focus, and grow through endochondral ossification, either as a consequence of trauma or a congenital perichondral deficiency.4,7
There appears to be no inheritable pattern, but these tumours can arise after exposure to radiation (12-15% of lesions) and occurrence is higher with total body irradiation.3
Solitary osteochondromas affect males more than females; and most patients are usually between 10 and 15 years old.3,4 These tumours increase in size throughout childhood and stop at skeletal maturity. Therefore isolated adult cases are reported.4 They can range in size from 1 to 10 cm.5
Osteochondromas are common in the appendicular skeleton in the metaphyses of the long bones but are rare in the vertebral column.3,4 Of the vertebral kind (1.3-4.1% of solitary osteochondromas),2-4,8,9 cervical (especially the atlantoaxial area) and thoracic types are most common with 50% of tumours being found in the cervical region.6
Clinical symptoms are related to the mechanical effects of the tumour. Pain is not a common symptom but, if it is present, it is progressive and unrelenting, and occurs at night. Radiculopathy, long tract signs and change in bladder or bowel habits are signs of expansion of the tumour.6
Those tumours that do cause cord compression are found in adolescent and young adult patients with hereditary multiple exostoses (HME), and are often those that arise from the posterior vertebral elements (especially the neural arch10) or the head of the ribs. This is due to the adolescent growth spurt causing enlargement of the mass as well.7
Vertebral osteochondromas can cause cosmetic deformity, neurovascular impingement and pathological fractures, and can become malignant.3 The percentage of malignant transformation is unknown but is reported to be between 0.4-2.2% in patients with solitary osteochondromas and up to 27.3% in patients with HME.3 The most frequent malignancy arises from the cartilage cap and is chondrosarcoma.3
The size of the cartilaginous cap is the best indicator of malignancy: <3 cm thick and largely mineralised caps are benign whereas caps >3 cm are more likely to be malignant.4 Those that recur after resection or continue to grow after skeletal maturity should also be considered malignant.4
The radiological appearance is frequently sufficient to make a diagnosis - cortical and medullary bone protruding from and continuous with the underlying bone. This is said to be pathognomonic.11
In the vertebral column however, diagnosis may be delayed due to poor visibility;2 fewer than 21% of cases were diagnosed on X-ray alone.5
Bone scintigraphy findings correlate directly with the degree of enchondral bone formation and metabolic activity.
Prominent radionuclide uptake is seen in younger patients.3
Ultrasound may enable accurate measurement of the hyaline cartilage cap thickness as it distinguishes fat and muscle from the cartilage cap.3
MRI enables one to identify complications and delineate the mass,3,8,9 and is considered the gold standard for the evaluation of intraspinal expansion, myelomalacia and spinal cord compression,2,12 and it identifies lesions that look suspicious of malignant transformation.3
CT scan shows the origin of the osseous mass and displays the fine anatomical detail needed for presurgical planning.8,12
On gross histological examination, the cartilage cap has a bosselated, shiny and glistening blue-grey surface resembling a cauliflower. The cap lies on the periphery where the growth occurs. The cartilage matrix can be calcified, with opaque yellow-grey areas. It is covered with a thin fibrous capsule that functions as a perichondrium. The cap is typically 1-3 cm in young patients and thinner in adults.3
The cut surface appears as a medullary cavity continuous with the underlying bone, as is the cortex and perichondrium. The microscopic features reveal enchondral ossification at the junction between the cartilaginous cap and cancellous bone beneath. The cap resembles a growth plate with columns or clusters of proliferating and degenerating chondrocytes.3
Spontaneous regression in very young male patients has been described - sessile (broad-based) tumours spontaneously resolve. Pedunculated osteochondromas usually regress after a traumatic event but this is unpredictable.3,13
Treatment must be individualised; surgical excision is a successful form of treatment with a low morbidity. Surgery is indicated in cases of progressive pain, neurological fallout and malignant transformation.4,6 Neurological recovery post-operatively is the norm.3,9
Conclusion
Osteochondromas of the vertebrae are rare but should be considered as a cause for spinal nerve root compression. The gold standard for diagnosis is an MRI, and surgery is a successful form of treatment.
References
1. Erlemann R. Imaging and differential diagnosis of primary bone tumours and tumour-like lesions of the spine. European Journal of Radiology 2006;58:48-67. [ Links ]
2. Jose Alcaraz Mexia M, Izquierdo Nunez E, Santonja Garriga C, Maria Salgado Salinas R. Osteochondroma of the thoracic spine and scoliosis. Spine 2001;26:1082-5. [ Links ]
3. Mavrogenis AF, Papagelopoulos PJ, Soucacos PN. Skeletal osteochondromas revisited. Orthopaedics 2008;31:1018. [ Links ]
4. Gene E, Quirini JR, Meyer H, Russell EJ. Osteochondroma of the thoracic spine: an unusual cause of spinal cord compression. AJNR May 1996;961-4. [ Links ]
5. Murphey MD, Andrews CL, Flemming DJ, Temple HT, Smith WS, Smirniotopoulos JG. Primary tumours of the spine: radiologic - pathologic correlation. Continuing Education 1996;15(5):1131-58. [ Links ]
6. NeuroWiki Editorial Board. Benign tumours of the vertebral column. NeuroWiki Congress of Neurological Surgeons July 2008. [ Links ]
7. Twersky J, Kassner G, Tenner MS, Camera A. Vertebral and costal osteochondromas causing spinal cord compression. American Journal of Roentgenology May 1975;124-8. [ Links ]
8. Govender S, Parbhoo AH. Osteochondroma with compression of the spinal cord. JBJS (Br) 1999;81-B:667-9. [ Links ]
9. Bhosale PB, Raut VA, Hussain N. Spinal osteochondromas causing cord compression - a rare cause of para-paresis. Bombay Hospital Journal 1999;41(2). Case Report No 11. [ Links ]
10. Kulkarni AG, Goel A, Muzumdar D. Solitary osteochondroma arising from the thoracic facet joint. Neurol Med Chir 2004;44:255-7. [ Links ]
11. Murphey MD, Choi JJ, Kransdorf MJ, Flemming DJ, Gannon FH. Imaging of osteochondroma: variants and complications with radiologic-pathologic correlation. Radiographics 2000;20(5):1407-34. [ Links ]
12. Lee KCY, Davies AM, Cassar-Pulicino VN. Imaging the complications of osteochondromas. Clinical Radiology 2002;57(1):18-28. [ Links ]
13. Reston SC, Savva N, Richards RH. Spontaneous resolution of solitary osteochondroma in a young adult. Skeletal Radiology 2004;33(5):303-5. [ Links ]
 Reprint requests
Reprint requests
Dr M Thiart
62 Strawberry Fields Cedarwood Road Goedemoed 7550
Cell: 082 3234 847 Fax: (023) 347-5158
Email: marithiart@lantic.net
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article.














