Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SA Orthopaedic Journal
On-line version ISSN 2309-8309
Print version ISSN 1681-150X
SA orthop. j. vol.9 n.1 Centurion Jan. 2010
CASE REPORT AND REVIEW OF THE LITERATURE
Achilles tendonitis: latent foreign body
NP SaragasI; PN FerraoII
IMBBCh(Wits), FCS(SA)Ortho, MMed(Ortho Surg)(Wits), Division of Orthopaedic Surgery, University of the Witwatersrand, Johannesburg Netcare Linksfield Orthopaedic Sports & Rehabilitation Centre (Clinic), Johannesburg
IIMBChB(Pret), FCS(Ortho)(SA)(Wits), Division of Orthopaedic Surgery, University of the Witwatersrand, Johannesburg Netcare Linksfield Orthopaedic Sports & Rehabilitation Centre (Clinic), Johannesburg
Introduction
Although foreign-body injuries are quite common, 15 to 55 per cent of these are misdiagnosed at the initial emergency room visit.1 The normal clinical course of a foreign-body injury is that of sudden pain at the time of injury followed by a dormant asymptomatic phase that can last from one month to a couple of years.1 The patient can, however, develop an acute flare-up at any stage. The length of this dormant phase may obscure the inciting incident, thus separating it from the onset of these 'late' symptoms.
Another problem leading to the occasional incorrect diagnosis is caused by the composition of the foreign body. If the foreign body is radiopaque it is easily detected on a standard radiograph or fluoroscopy. The problem arises when the foreign body is not radiopaque, as is the case with a wooden splinter or thorn. These can remain undetected even with surgical exploration and will only become evident when a toxic reaction to the foreign body causes inflammation with synovitis due to local irritation.2
We present a case report of Achilles tendonitis secondary to a retained thorn of the date palm (Phoenix caneriensis) (Figure 1).

Case report
A 32-year-old healthy male presented to his GP with a history of feeling 'something puncture' his left ankle while working in the garden. There was a 1 mm puncture wound on the lateral aspect of his ankle. The GP prescribed painkillers and discharged him. He is an avid long distance runner, and had successfully completed two previous Comrades marathons. He attempted the Comrades again four months after his injury but was unable to complete the race due to severe pain in his left Achilles tendon (AT). He returned to his GP who diagnosed Achilles tendonitis and gave him anti-inflammatories. He resumed his running again but kept having flare-ups in his left AT. He received treatment from numerous physiotherapists, seeking relief from the tendonitis until he was finally referred to our practice seeking a second opinion.
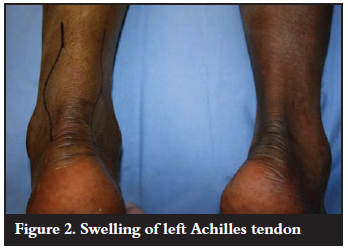
The clinical examination revealed a diffuse swelling over the Achilles tendon (Figure 2) proximal to its insertion. The AT was tender on deep palpation and although the excursion was equal to the unaffected side, there was discomfort with passive stretching. The patient was neurovascularly intact. The rest of the foot was asymptomatic.
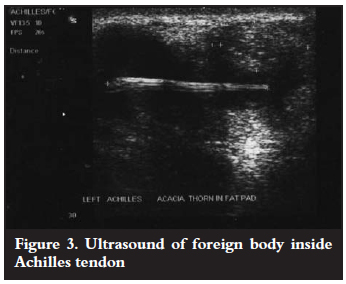
Radiographs of the left ankle revealed soft-tissue swelling around the AT. The patient was then sent for an ultrasound that clearly showed a foreign body within the tendon (Figure 3).
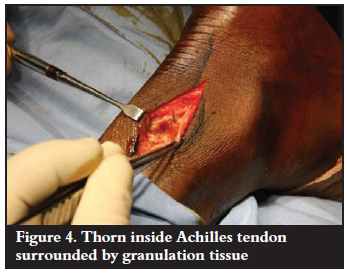
The patient was taken to the theatre for the removal of the foreign body, debridement and repair of the AT. Surgical exploration through a medial para-Achilles tendon incision revealed marked synovitis and chronic inflammation of the tendon sheath (Figure 4).
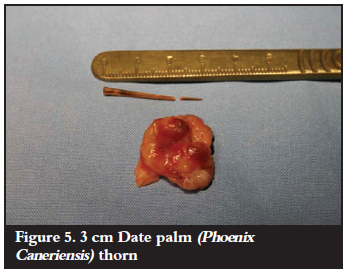
A 3 cm thorn of the date palm (Phoenix caneriensis) (Figure 5) was removed from the tendon. Post-operatively the patient resumed physiotherapy for rehabilitation. Nine months after the surgery, the patient ran the Comrades marathon and was awarded a medal. A year post-surgery the patient is doing well and has had no subsequent flare-ups.
Discussion
The foot is the second-most common location for retained foreign bodies.3 Such retention is especially frequent in developing countries where walking barefoot is very common. Thus the feet are at risk for trivial injuries, which can result in inflammation or infection.4 The foreign bodies most often retained in the hand and foot are thorns, glass, needles or wooden fragments. Retention of these foreign bodies results in a soft-tissue or bony granuloma.5 A retained foreign body can present in numerous ways, including mechanical dermatitis, cellulitis, abscess, foreign-body granuloma, peritendonitis, tendonitis, pericapsulitis, synovitis, acute septic arthritis or chronic monoarticular non-suppurative inflammation. Many aetiologies have been described to explain the pathogenesis in the sudden flare-up after a period of latency: low-grade infection, protein coating of the foreign body, toxins, mitogens in the foreign body and the crystalline structures of the foreign bodies.1
Taking a thorough history and doing a clinical examination are the first steps in making the diagnosis of a foreign body, but even so, 38% of cases are overlooked.6 Plain radiographs done for these patients fail to show wooden foreign bodies in 85% of cases.2 Therefore we started using ultrasonography, magnetic resonance imaging (MRI), and computed tomographic scanning (CT scan) to facilitate detection of these foreign bodies.
Studies using ultrasound to detect foreign bodies have reported sensitivities of 95 to 100% and specificities of 89.5 to 100%.2 The problem with ultrasound is, however, that it is very user-dependent. The modern ultrasound machines can detect foreign bodies as small as 5.6 mm in length and 1 mm in width. Foreign bodies made of metal, plastic, glass and fresh wood are bright sonographically and cast a distal shadow due to attenuation of the beam. Wooden objects decompose with time, which makes them difficult to detect with ultrasound after long periods of latency. A major benefit of ultrasound is the precise localisation of the foreign body in three dimensions.1
MRI is a good early modality for the detection of foreign bodies, especially wood. This enters the body dry (filled with air pockets), but within a week wood absorbs surrounding fluid and becomes attenuated on MRI.1,7 Wood will appear hypo-intense on T1-weighted images. A thin rim of enhanced tissue will be seen after the intravenous injection of gadolinium. On T2-weighted, however, the high-signal intensity of the granulation tissue may outshine the foreign body and make identification difficult.5,8
A CT scan is 5 to15 times more sensitive than plain radiographs for the identification of foreign bodies.3 Studies have, however, shown CT scans to be inferior to ultrasound and MRI in identifying foreign bodies.6 Considering that ultrasound is far cheaper, a CT scan should not be used.
Since foreign bodies present as an inflammation or infection, a biopsy or aspiration is sometimes done in order to make the diagnosis. It is possible to differentiate reactions to foreign bodies from other inflammatory arthropathies, whether septic or non-septic. Septic arthritis has diffuse polymorphonuclear (PMN) cell infiltrates and is generally culture positive. Non-septic inflammatory conditions have similar findings, except for the fact that they are generally without the foreign body PMNs. In contrast, foreign-body inflammation has diffuse lymphocytic infiltrate and focal collections of PMN cells found in foreign body giant cells.1,9,10
Despite all these special investigations, the gold standard for a chronic foreign-body synovitis is exploratory surgery with synovectomy and foreign-body excision for accurate diagnosis and management.5
Conclusion
The primary dilemma regarding foreign bodies is that the inciting event can be temporarily separated from the onset of the symptoms that made the patient present to a medical facility. If clinical suspicion remains despite negative imaging and failure to resolve with conservative treatment, most authors advocate surgical exploration for removal of suspected retained foreign bodies.
References
1. Bode KS, Haggerty CJ, Krause J. Latent foreign body synovitis. Journal of Foot & Ankle Surgery 2007;46(4):291-6. [ Links ]
2. Kobs JK, Hansen AR, Keefe B. A retained wooden foreign body in the foot detected by ultrasonography: A case report. J Bone Joint Surg Am 1992;74:296-8. [ Links ]
3. Yewlett A, Oakly J, Makwana N, Patel H. Retained blackthorn causing peroneal tendonitis: A case report. Foot Ankle Surg 2009;doi:10.1016/j.fas.2008.11.005 [ Links ]
4. Vidyadhara S, Rao SK. Thorn prick osteomyelitis of the foot in barefoot walkers: a report of four cases. J Orthop Surg 2006;14(2):222-4. [ Links ]
5. Hassan, FOA. Retained toothpick causing pseudotumor of the first metatarsal: A case report and literature review. Foot and Ankle Surgery 2008;(14):32-5. [ Links ]
6. Jacobson J, Powell A, Craig J, Bouffard J, van Holsbeeck M.Wooden foreign bodies in soft tissue: Detection at US. Radiology 1998;206:45-8. [ Links ]
7. Peterson JJ, Bancroft LW, Kransdorf MJ. Wooden foreign bodies: imaging appearance. AJR Am J Roentgenol 2002;178:557-62. [ Links ]
8. Durr HD, Stabler A, Muller PE, Refior HJ. Thorn induced pseudotumor of the metatarsal. J Bone Joint Surg (A) 2001;83(4):580-4. [ Links ]
9. Stevens KJ, Theologis T, McNally EG. Imaging of plantthorn synovitis. Skeletal Radiol 2000;29:605-8. [ Links ]
10. Adler M, Kaul A, Jawad AS. Letters to the editor: foreign body synovitis induced by a crown-of-thorns starfish. Rheumatology (Oxford) 2002;41:230-1. [ Links ]
 Reprint requests:
Reprint requests:
Dr P Ferrao
PO Box 281 Allensnek 1737
Tel: +27 11 485-1974/5 Fax: +27 11 640-5313
Email: paulo@cybersmart.co.za
No benefits of any form have been received from a commercial party related directly or indirectly to the subject of this article.














