Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
Journal of the South African Veterinary Association
versión On-line ISSN 2224-9435
versión impresa ISSN 1019-9128
J. S. Afr. Vet. Assoc. vol.85 no.1 Pretoria ene. 2014
ORIGINAL RESEARCH
The effects of midazolam and butorphanol, administered alone or combined, on the dose and quality of anaesthetic induction with alfaxalone in goats
T. Brighton DzikitiI; Gareth E. ZeilerI; Loveness N. DzikitiII; Eva R. GarciaI
IDepartment of Companion Animal Clinical Studies, University of Pretoria, South Africa
IISchool of Health Systems and Public Health, University of Pretoria, South Africa
ABSTRACT
Goats are rarely anaesthetised; consequently, scant information is available on the efficacy of anaesthetic drugs in this species. Alfaxalone is a relatively new anaesthetic agent, of which the efficacy in goats has not yet been studied. In this study, the sedative and alfaxalone-sparing effects of midazolam and butorphanol, administered alone or concomitantly, in goats were assessed. Eight clinically healthy goats, four does and four wethers, were enlisted in a randomised crossover manner to receive intramuscular sedative treatments consisting of saline 0.05 mL/kg, or midazolam 0.30 mg/kg, or butorphanol 0.10 mg/kg, or a combination of midazolam 0.30 mg/kg with butorphanol 0.10 mg/kg before intravenous induction of general anaesthesia with alfaxalone. Following induction, the goats were immediately intubated and the quality of anaesthesia and basic physiological cardiorespiratory and blood-gas parameters were assessed until the goats had recovered from anaesthesia. The degree of sedation, quality of induction and recovery were scored. When compared with saline (3.00 mg/kg), midazolam, administered alone or with butorphanol, caused a statistically significant increased level of sedation and a reduction in the amount of alfaxalone required for induction (2.00 mg/kg and 1.70 mg/kg, respectively). Butorphanol alone (2.30 mg/kg) did not cause significant changes in level of sedation or alfaxalone-induction dose. During induction and recovery, the goats were calm following all treatments, including the control group. Cardiorespiratory and blood-gas parameters were maintained within clinically acceptable limits. The present study showed that midazolam, administered alone or combined with butorphanol, produces a degree of sedation that significantly reduces the dose of alfaxalone required for induction of general anaesthesia in goats, without causing any major adverse cardiorespiratory effects.
Introduction
Administration of sedatives as premedication prior to general anaesthesia is a widely accepted concept in veterinary practice (Bednarski et al. 2011; Dzikiti et al. 2009). Benefits of pre-anaesthetic sedation include reduced patient excitement during anaesthetic induction and fewer drug-related adverse effects, as lesser amounts of anaesthetic agents are required to induce and maintain general anaesthesia (Bednarski et al. 2011). An appropriate selection of premedication drugs can significantly improve intraoperative cardiovascular stability, perioperative analgesia and the quality of recovery from anaesthesia (Waelbers et al. 2009). In small ruminants, the commonly used sedatives before induction of general anaesthesia include: α2-adrenoceptor agonists such as xylazine; phenothiazines such as acepromazine; benzodiazepines such as diazepam and midazolam; and opioids such as butorphanol (Riebold 2007). In goats, induction of general anaesthesia can be achieved by administration of ketamine, propofol or thiopentone (Dzikiti 2013; Prassinos et al. 2005). Recently, alfaxalone has been shown to be an alternative induction agent in: dogs (Ferré et al. 2006; Muir et al. 2008; Suarez et al. 2012); cats (Whittem et al. 2008); sheep (Andaluz et al. 2012); ponies (Klöppel & Leece 2011; Leece et al. 2009); and horses (Goodwin et al. 2011). However, its efficacy as an induction agent in goats has not yet been reported.
Midazolam is a water-soluble benzodiazepine that can be administered either by the intramuscular or intravenous route (Cao et al. 2002; Lemke 2007). It has mild cardiovascular and respiratory effects at clinical dosages and is commonly used as a mild sedative, muscle relaxant and anticonvulsant (Galatos 2011; Lemke 2007). Midazolam is reported to cause a significant reduction in the dose of propofol required for induction of anaesthesia in goats when administered intramuscularly alone and when combined with butorphanol (Dzikiti et al. 2009).
Butorphanol, a synthetic opioid, is an agonist at κ-opioid receptors and an antagonist at µ-opioid receptors (Carroll et al. 1997; Lamont & Mathews 2007; Valverde & Gunkel 2005). Opioids are traditionally included in balanced anaesthetic protocols for their analgesic effects, but they also have species-specific sedative effects (Lemke 2007). Butorphanol has useful analgesic effects in ruminants, but it can also cause central nervous system stimulation (Carroll et al. 2001; Doherty, Rohrbach & Geiser 2002). Butorphanol at a dose range of 0.02 mg/kg - 0.50 mg/kg, administered intramuscularly or intravenously, increases the degree of sedation obtainable from acepromazine or benzodiazepines (Dzikiti et al. 2009; Riebold 2007; Valverde & Gunkel 2005). At the same time, the sedatives (benzodiazepines) help to diminish the inherent excitatory effects of butorphanol (hyperactivity, increased myoclonic activity) in goats (Carroll et al. 2001; Dzikiti et al. 2009).
Alfaxalone is a synthetic, neuroactive steroid hypnotic agent (Ferré et al. 2006); several research teams have recently assessed the anaesthetic and cardiorespiratory effects of it. Its pharmacokinetic and pharmacodynamic profiles make it ideal for intravenous induction and maintenance of general anaesthesia in dogs (Ambrisko et al. 2011; Ambros et al. 2008; Ferré et al. 2006; Jiménez et al. 2012; Maddern et al. 2010; Michou et al. 2012; Muir et al. 2008; Psatha et al. 2011; Rodriguez et al. 2012; Suarez et al. 2012). Alfaxalone has been reported to be a suitable anaesthetic-induction agent at a dose of 2.00 mg/kg in unsedated sheep (Andaluz et al. 2012, Torres et al. 2012), sedated dogs (Maddern et al. 2009; Suarez et al. 2012) and ponies (Klöppel & Leece 2011; Leece et al. 2010). Dosages of 3.47 mg/kg - 4.70 mg/kg have been reported for sedated cats (Martinez Taboada & Murison 2010; Mathis et al. 2012).
To the knowledge of the authors, there are currently no scientific reports on the effects of commonly used sedatives on the induction dose of alfaxalone in goats, as well as the impact of these agents on the quality of general anaesthesia arising from their use. The present study tested the null hypothesis that midazolam, alone or combined with butorphanol, does not affect the induction dose of alfaxalone versus the alternative hypothesis that midazolam and butorphanol affect the alfaxalone induction dose in goats.
Materials and methods
Eight clinically healthy goats, four does and four wethers, were enlisted in this prospective, blinded, randomised, crossover experimental study. The goats were exposed to four treatments, with a three-week interval between treatments. The health status of the goats was determined by a clinical examination, complete blood count and biochemical analysis (total serum protein, albumin and globulin), which were all normal. During the period of data collection, the median age of the goats was 13.5 months (12.8-15.0 months), whilst the median weight was 26.2 kg (23.4 kg - 30.2 kg).
Experimental procedure
Food and water were withheld from the goats for 16-20 h prior to anaesthesia. The goats were weighed on an electronic scale (Shekel Merav 2000 series, Shekel, Johannesburg, South Africa) just before commencement of the experimental procedure. They were placed on a custom-made sling-cum-table for easier restraint. Temperature, pulse rate and respiratory rate were determined during the clinical examination and recorded as baseline values (Table 1 and Table 2).
For measurement of arterial blood pressure and collection of arterial blood samples for analyses, a 24-gauge catheter (Jelco, Medex Medical Ltd, Rossendale, Great Britain) was percutaneously introduced into the auricular artery. The catheter was connected to a recently calibrated transducer (DTX Plus transducer, BD Medical, Johannesburg, South Africa) for measurement of systolic, diastolic and mean arterial blood pressures. For transducer calibration to atmospheric pressure, the scapulo-humeral joint or the point of the sternum were used as zero reference points in sternally-recumbent or laterally-recumbent goats, respectively. Blood pressure readings were read from an electronic strain gauge transducer connected to a multi-parameter monitor (Cardiocap/5, Datex-Ohmeda Corporation, Helsinki, Finland).
The goats were premedicated by the intramuscular route with saline (Intramed Sodium Chloride 0.9%® Fresenius, Bodene, trading as Intramed, Port Elizabeth, South Africa) at 0.05 mL/kg (Treatment Control), or midazolam (Dormicum®, Roche Products, Isando, South Africa) at 0.30 mg/kg (Treatment MID), or butorphanol (Torbugesic®, Fort Dodge Animal Health, Fort Doge, USA) at 0.10 mg/kg (Treatment BUT), or a combination of midazolam at 0.30 mg/kg with butorphanol at 0.10 mg/kg (Treatment MIDBUT). The treatment drugs were calculated, drawn up and injected by a person other than the principal investigator, who was blinded to the treatments until the end of the data collection. This was so that the degree of sedation, the alfaxalone dose required for induction of general anaesthesia, the induction quality score and the recovery quality could be determined without bias. The degree of sedation was scored 30 min after administration of the treatments on a 0-3 scale, with 0 representing absence of apparent sedation (Table 3).
Once sedation had been assessed, an 18-gauge catheter (Jelco; Medex Medical Ltd, Rossendale, Great Britain) was introduced into the left forelimb cephalic vein for administration of alfaxalone and fluids. Thirty minutes (30 min) after administration of the treatments, alfaxalone (Alfaxalone®-CD RTU, Jurox Pty Ltd, Rutherford, Australia) was administered intravenously to induce a level of anaesthesia adequate for placement of an endotracheal tube. The main bolus dosage of alfaxalone at 1.50 mg/kg was administered using a volumetric syringe-driving pump (Perfusor® Space, B Braun Medical, Bethlehem, USA) over a 30 s period, followed by incremental boluses as required, at 0.50 mg/kg every 15 s. Depth of anaesthesia was checked by jaw tone and reflexes, immediately after administration of each intermittent bolus of alfaxalone, until the jaw was relaxed enough, and the swallowing and laryngeal reflexes, to see if they were diminished enough to allow endotracheal intubation. Placement of the endotracheal tube (silicone tube, internal diameter 7.5 mm) was performed using an illuminated laryngoscope, with the goats in sternal recumbency. Immediately after tracheal intubation, the goats were placed in right lateral recumbency and the exact total dose of alfaxalone required for induction of general anaesthesia was recorded. The quality of induction was assessed on a 0-2 score scale, with 0 representing failed intubation (Table 3).
Immediately after induction, the goats were allowed to recover from general anaesthesia, during which time they breathed room air spontaneously. Oxygen was supplemented if the goats became hypoxaemic (saturation of haemoglobin with oxygen in peripheral tissues [SpO2] < 90%). Ringer Lactate solution (Intramed Ringer-Lactate® Fresenius, Bodene, trading as Intramed, Port Elizabeth, South Africa) was administered intravenously using a volumetric fluid infusion pump (Infusomat® Space, B Braun Medical, Bethlehem, USA) at a rate of 4.00 mL/kg/hour, beginning from just before induction of general anaesthesia to about 30 min after induction of general anaesthesia. The endotracheal tube was removed once the goats regained a swallowing reflex. Time to extubation, sternal recumbency, standing and voluntary motion were recorded. All times were determined as the interval between the time the last amount of alfaxalone was administered and the time a particular event occurred. Quality of recovery was scored on a 0-3 score scale, with 0 representing the worst possible quality of recovery (Table 3).
Cardiopulmonary parameters including systolic, diastolic and mean arterial pressures, heart rate, respiratory rate and SpO2, as well as body temperature, were recorded prior to and 30 min after administration of the treatments and 2 min, 15 min and 30 min after administration of alfaxalone (Tables 1 and Table 2).
Arterial blood samples for gas analyses were collected in 2 mL pre-heparinised syringes (BD A-Line, Becton™, Dickinson & Company, New Jersey, USA) prior to (baseline) and 30 min after administration of the treatments, and 2 min and 30 min after administration of alfaxalone. The syringes were sealed immediately and the samples were analysed for blood gases within 5 min. Oxygen tension (PaO2), carbon dioxide tension (PaCO2), hydrogen ion concentration negative logarithm (pH), bicarbonate ion ([HCO3-]) concentration and oxygen saturation (SaO2) were measured using a pre-calibrated blood gas analyser (Rapidlab™ 348 pH/Blood Gas and Electrolyte Analyser, Siemens Medical Solutions Diagnostics, Midrand, South Africa).
To verify respiratory status, the PaO2/ F1O2 ratio was calculated by dividing the measured arterial oxygen tension by the fraction of inspired oxygen (21% or 0.21 in the present study). During normal respiratory function this ratio is greater than 250, whilst in patients with severe respiratory failure the ratio is less than 200 (Lagutchik 2001).
Statistical analysis
Data were analysed using Stata statistical package (Stata® Version 12.1, StataCorp LP, Vienna, Austria). All data were assumed not to be normally distributed due to the small sample size used in the present study (eight goats per treatment) and were therefore expressed as medians and interquartile ranges. Data on alfaxalone dose for induction, scores (sedation, quality of induction and recovery from anaesthesia), and times to extubation, sternal position, standing and voluntary motion were tested for statistically significant differences amongst treatments using the Friedman rank sum test. If statistically significant differences were observed, a post-hoc analysis (pair-wise Wilcoxon rank sum test with a Bonferroni adjustment for multiple testing) was conducted. Repeatedly measured variables (respiratory rate, heart rate, mean arterial blood pressure, SpO2, body temperature and blood-gas analyses data) were tested for statistically significant differences amongst and within treatments using the repeated measures analysis of variance (ANOVA) by ranks followed by post-hoc analysis (Tukey test). A value of p < 0.05 was considered to be significant.
Ethical considerations
The goats used in the present study experienced minimal discomfort. Potentially distressing or painful procedures worth noting were deprivation of food and water overnight, puncture of blood vessels for sample collection and catheterisation for administration of treatments and fluids during the experimental procedure. Puncturing of blood vessels was performed by an experienced veterinary anaesthetist so as to minimise the level of discomfort. The present study was pre-approved by both the Animal Ethics Committee and the Research Committee of the Faculty of Veterinary Science, University of Pretoria.
Results
Statistically significant differences in sedative effects were observed amongst treatments (Table 4). The level of sedation observed following the control treatment was significantly less profound than in both MID (p = 0.0002) and MIDBUT (p = 0.0002) treatments, whilst BUT treatment did not show any statistically significant difference from the control. The levels of sedation observed following MID or MIDBUT treatment were not statistically significantly different from each other.
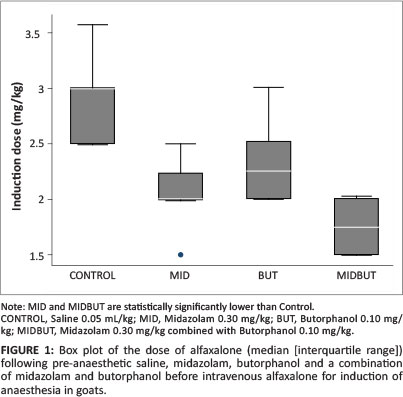
The control dose of alfaxalone required for induction of general anaesthesia was 3.00 mg/kg (2.50 mg/kg -3.00 mg/kg). The alfaxalone induction dose was statistically significantly higher than doses of 2.00 mg/kg (2.00 mg/kg - 2.13 mg/kg) and 1.75 mg/kg (1.5 mg/kg -2.00 mg/kg) required following MID (p = 0.0023) and MIDBUT (p = 0.000038) treatments, respectively. An alfaxalone induction dose of 2.25 mg/kg (2.00 mg/kg -2.52 mg/kg), which was required following BUT treatment was not significantly different from the control dose. The percentage reductions in the dose of alfaxalone required for induction of general anaesthesia following MID and MIDBUT treatments were 33.3% and 41.8%, respectively and were statistically significant, whilst BUT treatment caused a statistically insignificant reduction of 24.9% (Table 4 and Figure 1). The alfaxalone induction doses observed following MID or MIDBUT treatment were not statistically significantly different from each other.
Of the cardiovascular variables assessed, statistically significant differences were observed only in heart rate, which was higher than the baseline reading from within the same treatment group across all treatments, including the control, from 2 min of induction of general anaesthesia onwards (Table 1).
Respiratory and arterial blood gas variables showed very few statistically significant differences (Table 2). Statistically significant increases in PaCO2 were observed 2 min following induction of general anaesthesia within all treatment groups except Control. The PaO2/F1O2 ratio stayed above 250 with all treatments throughout the period of blood gas assessment.
The goats recovered calmly from general anaesthesia following all treatments. Times to extubation and sternal position were statistically significantly longer than the Control equivalents (p = 0.003 and 0.002, respectively) only for MIDBUT treatment. The time taken to attain standing position did not show any statistically significant differences amongst treatments and ranged from 17.5-32.5 min following BUT treatment and both MID and MIDBUT treatments, respectively (Table 4).
Adverse effects observed following induction of anaesthesia with alfaxalone included: frequent bloat of varying degrees; some increased muscle activity in the form of brisk palpebral movements and nystagmus; and muscle twitches and spasms, involving mostly muscles of the face, neck and upper forelimb. The observed increased muscle activity in a select group of muscles did not seem to be associated with gross purposeful movement of any body parts or depth of anaesthesia.
Discussion
Alfaxalone produced anaesthesia of good quality, which was characterised by calm inductions and recoveries in premedicated or un-premedicated goats. Midazolam, in concurrence with earlier studies (Dzikiti et al. 2009; Stegmann & Bester 2001), proved to be an effective sedative in goats. Midazolam, alone or combined with butorphanol, significantly reduced the dose of alfaxalone required for induction of general anaesthesia without causing clinically significant adverse effects, whilst butorphanol premedication alone did not cause any alteration in alfaxalone dose compared with the control treatment.
Midazolam, administered alone or with butorphanol at dosages used in the present study, caused moderate to profound sedation, which was significantly different from that observed following administration of either saline or butorphanol alone. Midazolam has been previously reported to cause profound sedation in goats (Dzikiti et al. 2009; Stegmann & Bester 2001). Butorphanol alone, as with saline, caused no apparent sedation in goats, in agreement with observations reported in earlier studies (Dzikiti et al. 2009). The sedative effects of butorphanol can be unpredictable and erratic (Carroll et al. 2001; Dzikiti et al. 2009), confirming the observations of the present study. Butorphanol does not seem to improve the level of sedation obtainable from midazolam alone, as no differences were observed in the level of sedation when the two were co-administered in comparison with midazolam alone. Butorphanol has been suspected to stimulate the central nervous system in goats, with effects such as restlessness and abnormal vocalisation cited (Carroll et al. 2001; Galatos 2011; Doherty et al. 2002). These excitatory effects were not observed in the present study.
The observed alfaxalone induction doses (1.75 mg/kg -3.00 mg/kg) are similar to those reported in earlier studies in other species such as: sheep (Andaluz et al. 2012; Torres et al. 2012); dogs (Maddern et al. 2010; Suarez et al. 2012); and ponies (Klöppel & Leece 2011; Leece et al. 2009), but lower than doses reported in cats (Martinez Taboada & Murison 2010; Mathis et al. 2012). The reason for the lack of agreement in alfaxalone dose could be the difference in the rate at which alfaxalone was administered. Administration of intravenous anaesthetic drugs for induction at slower rates significantly reduced the total dose required in humans (Berthoud et al. 1993; Peacock et al. 1990) and dogs (Dugdale et al. 2005). If the rate of administration is too rapid, there is a tendency to over-estimate the induction dose (Dugdale et al. 2005). Another factor that can influence the total dose required for induction is cardiac output (Dugdale et al. 2005); which was not measured in the present study.
The reductions in the dose of alfaxalone required for induction, especially following administration of midazolam alone or combined with butorphanol, demonstrate that midazolam-based premedication regimens can be used to supplement alfaxalone anaesthesia in goats, thereby reducing the dose of alfaxalone required to maintain general anaesthesia. The role of butorphanol in clinical settings would be to provide analgesia, especially for minor noxious procedures. The extent of reduction of the alfaxalone induction dose observed in the present study following MID, BUT and MIDBUT treatment of 33.3%, 24.9% and 41.8%, respectively, closely resemble those observed in an earlier study of 39.7%, 22.1% and 38.1% for propofol induction dose reduction following administration of the same premedication drugs at the same dosages in goats (Dzikiti et al. 2009). This observation demonstrates that midazolam and butorphanol reduce the amount of propofol or alfaxalone required for induction of general anaesthesia in a similar way in the goat. Pre-anaesthetic medication of goats with midazolam, alone or combined with butorphanol, clearly has an important role in balanced anaesthetic regimens in which alfaxalone or propofol is the induction agent.
During induction of general anaesthesia the goats were calm, irrespective of the sedation regimen used in the present study. This demonstrates that alfaxalone causes excitement-free induction in goats, even without prior calming of the goats by sedatives. This is similar to what has been reported for propofol, a closely related induction agent (Bettschart-Wolfensberger et al. 2000; Dzikiti et al. 2009; Pablo et al. 1997; Prassinos et al. 2005).
The statistically significant increase in heart rate observed following administration of alfaxalone - a common finding following all treatments in the present study - cannot be explained easily from the basic cardiovascular parameters measured, as the blood pressure did not change much during the same period. Had the other determinants of mean arterial blood pressure, namely cardiac output and peripheral vascular resistance, been measured, it may have been possible to explain the reason for the increase in heart rate observed in the present study. The increase in heart rate, accompanied by hardly any changes in blood pressure, mirror observations previously reported in sheep following alfaxalone administration (Andaluz et al. 2012). Change of body position to lateral recumbency was presumed to be the reason for the increase in heart rate in sheep by Andaluz's research team. Alfaxalone appears not to cause clinically significant alterations in cardiovascular function based on observations from the present study, notwithstanding the increase in heart rate.
Respiratory and blood gas parameters were largely unaffected by the alfaxalone and midazolam or butorphanol administered for premedication. The statistically significant increase in PaCO2 observed in all three treatments was not clinically significant, as the values still remained below the 45 mmHg upper limit. Further confirmation of unaffected respiratory function is obtained from the PaO2/F1O2 ratio, which remained higher than 250 throughout the anaesthetic period. Patients with compromised respiratory function have PaO2/F1O2 ratios below 200 (Lagutchik 2001). In sheep, alfaxalone causes minimal respiratory changes, but induction apnoea and bradypnoea have been reported in dogs (Muir et al. 2008; Whittem et al. 2008).
Recovery from general anaesthesia was excitement-free following all treatments and the goats were able to attain standing position within 30 min of induction, as has been previously reported for propofol in goats (Dzikiti et al. 2009).
The adverse effects observed in the present study have been previously reported following administration of alfaxalone in other species. Bloat is known to occur in laterally recumbent goats despite prior starvation (Dzikiti 2013; Galatos 2011; Taylor 1991). Brisk palpebral movements and nystagmus have been reported in horses (Goodwin et al. 2011). Referred muscle movements have previously been reported in anaesthetised goats and other species, even with other induction agents such as propofol and thiopentone (Benson & Thurmon 1990; Dzikiti et al. 2009; Mathis et al. 2012).
Conclusion
The present study demonstrates that midazolam alone, or combined with butorphanol, is an effective sedative. It also demonstrates that alfaxalone, with or without midazolam and/or butorphanol, produces good-quality anaesthesia, characterised by calmness during induction and recovery, without causing major clinically significant adverse cardiorespiratory effects in goats. The dose of alfaxalone required for induction of general anaesthesia was profoundly reduced by sedation with midazolam-based regimens, but only slightly and not significantly reduced by butorphanol administered alone. This alfaxalone-sparing effect of midazolam alone or combined with butorphanol should be borne in mind when alfaxalone is used for induction of anaesthesia in goats in clinical settings.
Acknowledgements
The funds and necessary infrastructure (facilities, laboratories and equipment) for the present study were provided by the University of Pretoria and the Beit Trust. Mr Peter Tivenga is acknowledged for assisting the principal researcher with logistical aspects during data collection.
Competing interests
The authors declare that they have no financial or personal relationship(s) which may have inappropriately influenced them in writing this article.
Authors' contributions
T.B.D. (University of Pretoria) was responsible for designing the study and writing the manuscript; G.E.Z. (University of Pretoria) assisted during data collection and in writing of the manuscript; L.N.D. (University of Pretoria) performed the statistical analysis of the data; E.R.G. (University of Pretoria) was involved in study design and writing the manuscript.
References
Ambrisko, T.D., Johnson, C.B. & Chambers, P., 2011, 'Effect of alfaxalone infusion on the electroencephalogram of dogs anaesthetised with halothane', Veterinary Anaesthesia and Analgesia 38, 529-535. http://dx.doi.org/10.1111/j.1467-2995.2011.00650.x [ Links ]
Ambros, B., Duke-Novakoski, T. & Pasloske, K.S., 2008, 'Comparison of efficacy and cardiopulmonary effects of continuous rate infusions of alfaxalone-2-hydroxypropoyl-ß-cyclodextrin and propofol in dogs', American Journal of Veterinary Research 69, 1391-1398. http://dx.doi.org/10.2460/ajvr.69.11.1391 [ Links ]
Andaluz, A., Felez-Ocana, N., Santos, L., Fresno, L. & Garcia, F., 2012, 'The effects on cardio-respiratory and acid-base variables of the anaesthetic alfaxalone in a 2-hydroxypropyl- ß-cyclodextrin (HPCD) formulation in sheep', Veterinary Journal 191, 389-392, viewed 12 June 2013, from http://dx.doi.org/10.1016/j.tvjl.2011.03.017 [ Links ]
Bednarski, R., Grimm, K., Harvey, R., Victoria, M.L., Sean Penn, W., Sargent, B. & Spelts, K., 2011, 'Veterinary Practice Guidelines: AAHA anesthesia guidelines for dogs and cats', Journal of the American Animal Hospital Association 47, 377-385. http://dx.doi.org/10.5326/JAAHA-MS-5846 [ Links ]
Benson, G.J. & Thurmon, J.C., 1990, 'Intravenous anaesthesia', Veterinary Clinics of North America Equine Practice 6, 511-526. [ Links ]
Berthoud, M.C., McLaughlan, G.A., Broome, I.J., Henderson, P.D., Peacock, J.E. & Reilly, C.S., 1993, 'Comparison of infusion rates of three i.v. anaesthetic agents for induction in elderly patients', British Journal of Anaesthesia 70, 423-427. http://dx.doi.org/10.1093/bja/70.4.423 [ Links ]
Bettschart-Wolfensberger, R., Semder, A., Alibhai, H., Demuth, D., Shojaee-Aliabadi, F. & Clarke, W., 2000, 'Cardiopulmonary side-effects and pharmacokinetics of an emulsion of propofol (Disoprivan) in comparison to propofol dissolved in polysorbate 80 in goats', Journal of Veterinary Medicine 47, 341-350. http://dx.doi.org/10.1046/j.1439-0442.2000.00289.x [ Links ]
Cao, J.L., Ding, H.L., Zhang, L.C., Duan, S.M. & Zeng, Y.M., 2002, 'Pretreatment with midazolam suppresses morphine withdrawal response in mice and rats', Acta Pharmacologica Sinica 23, 685-690. [ Links ]
Carroll, G.L., Boothe, D.M., Hartsfield, S.M., Waller, M.K. & Geller, S.C., 2001, 'Pharmacokinetics and selected behavioural responses to butorphanol and its metabolites in goats following intravenous and intramuscular administration', Veterinary Anaesthesia and Analgesia 28, 188-195. http://dx.doi.org/10.1046/j.1467-2987.2001.00071.x [ Links ]
Carroll, G.L., Hartsfield, S.M. & Hambleton, R., 1997, 'Anesthetic effects of tiletamine-zolazepam, alone or in combination with butorphanol, in goats', Journal of the American Veterinary Medical Association 211, 593-597. PMid:9290827. [ Links ]
Doherty, T.J., Rohrbach, B.W. & Geiser, D.R., 2002, 'Effect of acepromazine and butorphanol on isoflurane minimum alveolar concentration in goats', Journal of Veterinary Pharmacology and Therapeutics 25, 65-67. http://dx.doi.org/10.1046/j.1365-2885.2002.00371.x [ Links ]
Dugdale, A.H.A., Pinckbeck, G.L., Jones, R.S. & Adams, W.A., 2005, 'Comparison of two thiopental infusion rates for the induction of anaesthesia in dogs', Veterinary Anaesthesia and Analgesia 32, 360-366. http://dx.doi.org/10.1111/j.1467-2995.2005.00198.x [ Links ]
Dzikiti, T.B., 2013, 'Intravenous anaesthesia in goats: A review', Journal of the South African Veterinary Association 84, Art # 499, viewed 12 June 2013, from http://dx.doi.org/10.4102/jsava.v84i1.499 [ Links ]
Dzikiti, T.B., Stegmann, G.F., Hellebrekers, L.J. & Dzikiti, L.N., 2009, 'Sedative and cardiopulmonary effects of acepromazine, midazolam, butorphanol, acepromazine-butorphanol and midazolam-butorphanol on propofol anaesthesia in goats', Journal of the South African Veterinary Association 80, 10-16. PMid:19653513. [ Links ]
Ferré, P.J., Pasloske, K., Whittem, T., Ranasinghe, M., Li, Q. & Lefebvre, H.P., 2006, 'Plasma pharmacokinetics of alfaxalone in dogs after an intravenous bolus of Alfaxan-CD RTU', Veterinary Anaesthesia and Analgesia 33, 229-236, viewed 12 June 2013, from http://dx.doi.org/10.1111/j.1467-2995.2005.00264.x [ Links ]
Galatos, A.D., 2011, 'Anesthesia and analgesia in sheep and goats', Veterinary Clinics of North America: Food Animals 27, 47-59, viewed 12 June 2013, from http://dx.doi.org/10.1016/j.cvfa.2010.10.007 [ Links ]
Goodwin, W.A., Keates, H.L., Pasloske, K., Pearson, M., Sauer, B. & Ranasinghe, M.G., 2011, 'The pharmacokinetics and pharmacodynamics of the injectable anaesthetic alfaxalone in the horse', Veterinary Anaesthesia and Analgesia 38, 431-438. http://dx.doi.org/10.1111/j.1467-2995.2011.00634.x [ Links ]
Jiménez, C.P., Mathis, A., Sandra, S.M., Brodbelt, D. & Alibhai, H., 2012, 'Evaluation of the quality of the recovery after administration of propofol or alfaxalone for induction of anaesthesia in dogs anaesthetized for magnetic resonance imaging', Veterinary Anaesthesia and Analgesia 39, 151-159. http://dx.doi.org/10.1111/j.1467-2995.2011.00678.x [ Links ]
Klöppel, H. & Leece, A.E., 2011, 'Comparison of ketamine and alfaxalone for induction and maintenance of anaesthesia in ponies undergoing castration', Veterinary Anaesthesia and Analgesia 38, 37-13. http://dx.doi.org/10.1111/ij.1467-2995.2010.00584.x [ Links ]
Lagutchik, M.S., 2001, 'Respiratory distress', in W.E. Wingfield (ed.), Veterinary emergency medicine secrets, 2nd edn., p. 20, Hanley & Belfus Inc. Medical Publishers, Philadlephia. [ Links ]
Lamont, A. & Mathews, K.A., 2007, 'Opioids, non-steroidal anti-inflammatories, and analgesic adjuvants', in W.J. Tranquilli, J.C. Thurmon & K.A Grimm (eds.), Lumb and Jones's veterinary anaesthesia and analgesia, 4th edn., pp. 241-271, Blackwell Publishing, Iowa. [ Links ]
Leece, E.A., Girard, N.M. & Maddern, K., 2009, 'Alfaxalone in cyclodextrin for induction and maintenance of anaesthesia in ponies undergoing field castration', Veterinary Anaesthesia and Analgesia 36, 480-184. http://dx.doi.org/10.1111/j.1467-2995.2009.00479.x [ Links ]
Lemke, K.A., 2007 'Anticholinergics and sedatives', in W.J. Tranquilli, J.C. Thurmon & K.A. Grimm (eds.), Lumb and Jones's veterinary anaesthesia and analgesia, 4th edn., pp 203-239, Blackwell Publishing, Iowa. [ Links ]
Maddern, K., Adams, V.J., Hill, N.A.T. & Leece, E.A., 2010, 'Alfaxalone induction dose following administration of medetomidine and butorphanol in the dog', Veterinary Anaesthesia and Analgesia 37, 7-13. http://dx.doi.org/10.1111/j.1467-2995.2009.00503.x [ Links ]
Martinez Taboada, F. & Murison, P.J., 2010, 'Induction of anaesthesia with alfaxalone or propofol before isoflurane maintenance in cats', Veterinary Record 167, 85-89. http://dx.doi.org/10.1136/vr.b4872 [ Links ]
Mathis, A., Pinelas, R., Brodbelt, D.C. & Alibhai, H.K., 2012, 'Comparison of quality of recovery from anaesthesia in cats induced with propofol or alfaxalone', Veterinary Anaesthesia and Analgesia 39, 282-290. http://dx.doi.org/10.1111/j.1467-2995.2011.00707.x [ Links ]
Michou, J.N., Leece, E.A. & Brearley, J., 2012, 'Comparison of pain on injection during induction of anaesthesia with alfaxalone and two formulations of propofol in dogs', Veterinary Anaesthesia and Analgesia 39, 275-281. http://dx.doi.org/10.1111/j.1467-2995.2012.00709.x [ Links ]
Muir, W., Lerche, P., Wiese, A., Nelson, L., Pasloske, K. & Whittem, T., 2008, 'Cardiorespiratory and anesthetic effects of clinical and supraclinical doses of alfaxalone in dogs', Veterinary Anaesthesia and Analgesia 35, 451-462, viewed 12 June 2013, from http://dx.doi.org/10.1111/j.1467-2995.2008.00406.x [ Links ]
Pablo, L.S., Bailey, J.E. & Ko, J.C.H., 1997, 'Median effective dose of propofol required for induction of anaesthesia in goats', Journal of the American Veterinary Medical Association 211, 86-88. [ Links ]
Peacock, J.E., Lewis, R.P., Reilly, C.S. & Nimmo, W.S., 1990, 'Effect of different rates of infusion of propofol for induction of anaesthesia in elderly patients', British Journal of Anaesthesia 65, 346-352. http://dx.doi.org/10.1093/bja/65.3.346 [ Links ]
Prassinos, N.N., Galatos, A.D. & Raptopoulos, D., 2005, 'A comparison of propofol, thiopental or ketamine as induction agents in goats', Veterinary Anaesthesia and Analgesia 32, 289-296, viewed 12 June 2013, from http://dx.doi.org/10.1111/j.1467-2995.2005.00204.x, PMid:16135210. [ Links ]
Psatha, E., Alibhali, H.I.K., Jimenez-Lozano, A., Armitage-Chan, E. & Brodbelt, D.C., 2011, 'Clinical efficacy and cardiorespiratory effects of alfaxalone or diazepam/ fentanyl for induction of anaesthesia in dogs that are a poor anaesthestic risk', Veterinary Anaesthesia and Analgesia 38, 24-36. http://dx.doi.org/10.1111/j.1467-2995.2010.00577.x [ Links ]
Riebold, T.W., 2007, 'Ruminants', in W.J. Tranquilli, J.C. Thurmon & K.A. Grimm (eds.), Lumb and Jones's veterinary anaesthesia and analgesia, 4th edn., pp. 731-746, Blackwell Publishing, Iowa. http://dx.doi.org/10.1111/j.1467-2995.2011.00695.x [ Links ]
Rodríguez, J.M., Munoz-Rascón, P., Navarrete-Calvo, R., Gómez-Villamandos, J., Domínguez Pérez, J.M., Fernandez Sarmiento, J.A., Quirós Carmona, S. & Granados Machuca, M.M., 2012, 'Comparison of the cardiopulmonary parameter after induction of anaesthesia with alphaxalone or etomidate in dogs', Veterinary Anaesthesia and Analgesia 39, 357-365. [ Links ]
Stegmann, G.F. & Bester, L., 2001, 'Sedative-hypnotic effects of midazolam in goats after intravenous and intramuscular administration', Veterinary Anaesthesia and Analgesia 28, 49-55. http://dx.doi.org/10.1046/j.1467-2987.2000.00034.x [ Links ]
Suarez, M.A., Dzikiti, B.T., Stegmann, F.G. & Hartman, M., 2012, 'Comparison of alfaxalone and propofol administered as total intravenous anaesthesia for ovariohysterectomy in dogs', Veterinary Anaesthesia and Analgesia 39, 236-244, viewed 12 June 2013, from http://dx.doi.org/10.1111/j.1467-2995.2011.00700.x [ Links ]
Taylor, P.M., 1991, 'Anaesthesia in sheep and goats', In Practice 13, 31-36, viewed 12 June 2013, from http://dx.doi.org/10.1136/inpract.13.1.31 [ Links ]
Torres, M-D., Andaluz, A., Garcia, F., Fresno, L. & Moll, X., 2012, 'Effects of an intravenous bolus of alfaxalone versus propofol on intra-ocular pressure in sheep', Veterinary Record 170, 226. http://dx.doi.org/10.1136/vr.100399 [ Links ]
Valverde, A. & Gunkel, C.I., 2005, 'Clinical practice review: Pain management in horses and farm animals', Journal of Emergency and Critical Care 15, 295-307. http://dx.doi.org/10.1111/j.1476-4431.2005.00168.x [ Links ]
Waelbers, T., Vermoere, P. & Polis, I., 2009, 'Total intravenous anaesthesia in dogs. A review', Vlaams Diergeneeskunde Tijdschrift [Flemish Veterinary Journal] 78, 160-169.
Whittem, T., Pasloske, K.S., Heit, M.C. & Ranasinghe, M.G., 2008, 'The pharmacokinetics and pharmacodynamics in cats after single and multiple intravenous administration of alfaxan at clinical and supraclinical doses', Journal of Veterinary Pharmacology and Therapeutics 31, 571-579. http://dx.doi.org/10.1111/j.1365-2885.2008.00998.x [ Links ]
 Correspondence:
Correspondence:
Brighton Dzikiti
Private Bag X04
Onderstepoort 0110
South Africa
Email: brighton.dzikiti@up.ac.za
Received: 30 Apr. 2013
Accepted: 23 Oct. 2013
Published: 19 Aug. 2014














