Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
Journal of the South African Veterinary Association
On-line version ISSN 2224-9435
Print version ISSN 1019-9128
J. S. Afr. Vet. Assoc. vol.84 n.1 Pretoria Jan. 2013
ORIGINAL RESEARCH
Knowledge and practices related to bovine brucellosis transmission amongst livestock workers in Yewa, south-western Nigeria
Hezekiah K. AdesokanI; Peter I. AlabiI; Judy A. StackII; Simeon I.B. CadmusI
IDepartment of Veterinary Public Health and Preventive Medicine, University of Ibadan, Nigeria
IIDepartment of Bacteriology, Veterinary Laboratories Agency, United Kingdom
ABSTRACT
Brucellosis is an endemic disease in the animal population in Nigeria and of major public health importance, particularly amongst livestock workers who are ignorant of the risk of Brucella infection. Therefore, to gain insight into the knowledge and practices related to brucellosis transmission amongst livestock holders (LH) and livestock marketers (LM) in Yewa, an international livestock trading centre in south-western Nigeria, we conducted an interview-based study using a cluster sampling technique. In all, a total of 157 respondents comprising 54 LH and 103 LM were interviewed. Two-thirds (69.5%) of the two groups had poor knowledge of brucellosis with no significant difference between them (p = 0.262). Furthermore, consumption of unpasteurised milk, uncooked meat and its products, co-habitation with animals, and poor hygiene were significant risk practices identified as possible means of transfer of Brucella infection from animals to humans amongst these livestock workers (p < 0.05). In conclusion, our findings revealed that poor knowledge and practices related to the consumption of unpasteurised or unboiled dairy products, contaminated beef, and unhygienic practices are factors that will facilitate Brucella infections amongst livestock workers in Nigeria. Therefore, there is a need for more public health enlightenment programmes, as well as implementation of brucellosis control measures in the cattle populations.
Introduction
Brucellosis is a zoonosis transmitted directly or indirectly by exposure to infected animals (Mandel, Bennet & Dolin 2005). It is considered as one of the most important zoonoses in the world (World Health Organization, Food and Agriculture Organization of the United Nations & World Organization for Animal Health 2004). In humans, brucellosis is often easily misdiagnosed as other febrile syndromes such as malaria and typhoid fever, thereby resulting in mistreatments and underreporting (Bax, Van Veelen & Gyssen 2007). It is acquired in people through breaks in the skin following direct contact with infected animals' tissues or blood or their secretions. Infection may also result from consumption of contaminated unpasteurised milk and milk products (Georgiou et al. 2005). Generally, poor hygiene, prevalence of the disease in animals and practices that expose humans to infected animals or their products influence the occurrence of the disease in humans (Schoonman 2007; Swai & Schoonman 2009). Occupational groups at higher risk of infection include cattle producers, veterinarians, animal health personnel, abattoir workers, laboratory personnel and those amongst the general public who are in contact with infected animals. Prevalence rates of brucellosis reported amongst livestock workers in various parts of the world, especially in developing countries, range from less than 1.00% to as high as 60.00%. For instance, in some of the pastoral and agro-pastoral communities in northern Tanzania, infection rates range between 0.70% and 13.00% of the population (Minja 2002; Mtui-Malamsha 2001). In the same vein, Regassa et al. (2009) reported that 60.60% of Brucella-positive patients in Ethiopia were pastoralists. In Nigeria, seroprevalence of 31.82% and 7.60% amongst livestock workers and hospital patients in the south-western and north-central parts of the country, respectively, have been reported (Cadmus et al. 2006; Ofukwu, Yohanna & Abuh 2011).
In many developing countries, including Nigeria, a high proportion of the population resides in rural areas where agriculture is the main source of their livelihood. Furthermore, a sizeable proportion engages in livestock production, resulting in a high level of contact with animals and increased risk of zoonotic infection. Therefore, adequate knowledge of the epidemiology of bovine brucellosis is of great public health importance, particularly amongst livestock workers as this will greatly assist in mapping out strategies for its control amongst the general public. To this end, we conducted a study to assess the knowledge of brucellosis and document practices related to its zoonotic transmission amongst livestock holders (LH) and livestock marketers (LM) in Yewa Division, south-western Nigeria.
Materials and methods
Study site
The study was conducted in Yewa Division of Ogun State, south-western Nigeria. Yewa is a point of convergence for livestock workers in Nigeria and the neighbouring countries of Burkina Faso, Togo and Chad. In addition, because brucellosis can be spread across international borders, Yewa provides the right environment for envisaged strategic disease control programmes through public health awareness campaigns amongst local and foreign livestock traders.
Subjects and procedure
A meeting was held to inform the leaders of the various occupational groups about the objectives of the study and to facilitate interviews amongst the stakeholders. In all, two different groups were identified, namely the LH, which comprised herdsmen, their wives and children, and LM, who were mainly involved in cattle sales at the market. A sampling frame was not designed for this study as there was no structured outline of LM and LH in the area and specifically because of the migratory nature of their jobs. However, a cluster sampling technique was used, with all the households in the area taken as a cluster. To carry out this study, all consenting LM or LH present in consecutive houses were interviewed, proceeding from the randomly selected starting point until 10% of each population was reached.
Questionnaire administration
A semi-structured questionnaire was administered to the respondents by trained field workers. A translator was used to facilitate communication. Demographic data such as age, sex and tribe were obtained from the participants. Other information obtained included knowledge of Brucella infection and symptoms of the disease, milk and meat consumption habits and occurrence of close co-habitation with animals. For instance, the knowledge of 'what brucellosis is' was assessed using a description of clinical manifestations and the local language that was commonly spoken amongst livestock workers.
Statistical analysis
Data were analysed using SPSS version 15.0 (2006). Knowledge about brucellosis and symptoms of infection amongst others were scored with reference to answers to five questions. Positive responses were scored 1 and negative responses were scored 0. Scores ranged between 0 and 5. Scores > 3 were taken as good knowledge, whilst scores < 3 were taken as poor knowledge. Similarly, ventilation in the animal housing was assessed and adjudged to be adequate if animals were separated into different compartments, allowing for free flow of fresh air. Alternatively, it was said to be inadequate if animals were pooled together in a single shed without flow of air.
Inferential statistical analysis to test for associations between variables was done using the chi-square test and the test level of statistical significance was set at 5%. Prevalence ratios were also calculated.
Ethical considerations
Approval for the protocols of this research was obtained from the Ethics Committee, Faculty of Veterinary Medicine, University of Ibadan, Nigeria (Approval number: Ethics/ 12/10/03).
Potential benefits and hazards
No risk whatsoever was associated with the subject as there were no individual identities attached to the data obtained from them. Potential psychological fears in terms of envisaged apprehension about the possible consequences of their poor practices for brucellosis transmission were taken into consideration. They were counselled to visit a hospital if they had been experiencing protracted fever. Possible benefits to the subject include better enlightenment about the disease and hence limited disease spread to the society in general.
Recruitment procedures
Participation was based on willingness after the purpose of the study had been explained. Potential participants were told they could withdraw their consent to participate in the process of the interview if they felt the need to do so, without any attached penalty.
Informed consent
As most respondents could not read, they were informed verbally that they could choose either to participate in the study or choose not to. Consent was therefore obtained from those who willingly chose to participate by their affirmative response to participation in the study.
Data protection
The information from each respondent was treated with the utmost confidentiality and there was no divulgence of information from one respondent to the other. Each questionnaire was labelled using codes, without any inclusion of names or any other identities that could link the data to any respective respondent.
Results
Demographic characteristics
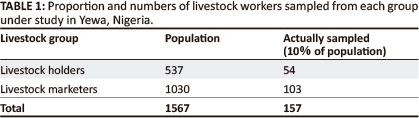
In all, a total of 157 respondents were interviewed about their knowledge and practices in relation to brucellosis transmission and control (Table 1). Of these, 83.4% were men whilst 16.6% were women. A significantly higher mean age of 43.3 years was obtained amongst the LM respondents, as against 38.7 years recorded for the LH respondents (t = 7.53, p < 0.05). The respondents included mostly the Yorubas (59.9%), followed by the Fulanis (36.3%), with other tribes (3.8%) being the minority (Table 2).
Knowledge
At least two-thirds (69.5%) of participants in both groups had poor knowledge of brucellosis and there was no statistically significant difference in the knowledge about the disease between the two groups (p = 0.262). Again, 76.0% and 72.0% of the LH and LM respondents, respectively, did not know what brucellosis was, whilst all (100%) and 95.2% of LH and LM respondents, respectively, did not know the cause of the disease. Furthermore, about 63.0% of each of the two groups did not know the symptoms of the disease in animals and 100% and 92.2% of LH and LM respondents, respectively, did not know its symptoms in humans. Again, about 70.0% and 60.0% of the LH and LM respondents, respectively, also did not know the means of transmission of brucellosis from animals to humans (Table 3).
Practices
Milk and meat consumption behaviour
The proportions of households who drank raw cows' milk were 100% and 95.1% amongst the LH and LM respondents, respectively. Furthermore, all the 54 participants in the LH group preferred raw or soured milk or both, whilst only 98.1 % admitted to this amongst the LM group (Table 4). The varying preference for the milk types was statistically significant between the two groups (p = 0.000). Again, a significant relationship (p = 0.000) was observed between the LH (59.3%) and LM (22.2%) populations regarding the consumption of unboiled milk. Similarly, a significantly higher proportion, 15 (27.8%) of the LH population ate uncooked meat and meat products when compared with 13 (12.6%) of the LM population (p = 0.0196) (Table 4).
Housing, handling of animals and their products
All respondents in the LH group co-habited with their animals in the house, whilst approximately two-thirds (64.10%) of respondents in the LM group reported this practice. Houses with inadequate ventilation were observed in 85.20% of the LH households and the places provided for their animals were found to be unhygienic, with animal feed laden with dung produced over several days in 74.14% and 81.60% of the LH and LM households, respectively. A significantly higher proportion (p = 0.000) of respondents in the LM group (81.60%) handled aborted materials compared with those in the LH group (11.10%). Other risk practices associated with the spread of brucellosis amongst the two groups included milking, herding cattle and goats, and slaughter (Table 4).
Trustworthiness
Reliability
The split half test was used to test the reliability of the instrument. The result obtained was compared and correlated to estimate the level of reliability using Cronbach's alpha method to determine the internal consistency of the instrument.
Validity
To ensure validity, a draft of the modified questionnaire was subjected to proper scrutiny by the members of the research team of the Brucellosis Laboratory at the Department of Veterinary Public Health and Preventive Medicine, University of Ibadan, Nigeria for content and construct validity. Suggestions, recommendations and modifications on the instrument were studied carefully and used to improve the quality of the instrument, as well as the entire study.
Discussion
Our findings reveal that at least two-thirds (69.5%) of the LH and LM respondents had poor knowledge of brucellosis in cattle with respect to its causes, symptoms and mode of transmission, particularly from animals to humans. This is therefore of great importance, particularly when the zoonotic nature and the public health significance of brucellosis are considered. Again, the gravity of this problem is better imagined when there are widespread transboundary infections cutting across both human and animal populations.
Furthermore, the unhygienic eating habits of the workers are sources of concern. From our findings, most (98.7%) of the respondents in both groups consumed raw or soured milk, whilst a higher proportion (59.3%) of the LH group consumed it unboiled. This practice is corroborated by earlier findings that revealed the consumption of unpasteurised milk and milk products amongst Fulani pastoralists who drink milk directly from the udders of cows (Cadmus & Adesokan 2007). Previous reports also indicated that approximately 90.0% of milk consumed in sub-Sahara Africa is raw or soure (Mfinanga et al. 2003; Walshe et al. 1991). However, consumption of unpasteurised dairy products has been reported as a brucellosis risk factor for humans (Cadmus, Adesokan & Stack 2008; Kang'ethe et al. 2000). The gravity of this problem is shown in the 85.7% of cases of human infections resulting from the consumption of raw milk in Ethiopia (Regassa et al. 2009).
Again, the consumption of uncooked meat amongst some (17.8%) of the respondents is also a source of public health concern, given an earlier report that cited this practice as a rare predisposing factor for human brucellosis (Shirima et al. 2010). The habit of eating uncooked meat from various animals is common amongst Africans and this has resulted in the occurrence of different zoonotic infections amongst humans (John et al. 2010). Furthermore, the majority (80.0%) of the respondents in both groups demonstrated poor hygiene practices during animal husbandry activities. Generally, poor hygiene has been implicated in the enhancement of brucellosis or zoonotic infections from infected animal materials to humans (Schoonman 2007) and this has specifically led to human infection in Tanzania. Human infection can also occur via direct contact with infected animals' tissues or blood, or through inhalation of infected aerosols or inoculation of the conjunctival sac of the eyes (Georgiou et al. 2005).
Our findings show that inadequate ventilation and confinement of livestock within human habitation is common and can increase the circulation of infected aerosols within this micro-environment, thereby promoting human infections. Furthermore, these workers are exposed to Brucella infections by different degrees of cuts and abrasions they sustain during their work. Another concern in this regard is the handling of animals and animal products when milking, herding cattle and goats, slaughtering, and handling aborted materials. As observed in the two groups, these activities can potentially predispose them to contracting zoonotic diseases from their animals given the endemicity of the disease in the animal population in Nigeria. Co-incidentally, previous studies from Tanzania reported the highest seroprevalence of brucellosis amongst abattoir workers, particularly those involved in the slaughtering and cleaning of slaughtered animal parts (Walshe et al. 1991). Alavi, Rafiei and Nikkhooi (2007) also reported an association between work practices and Brucella infections amongst nomads in Khuzestan, Iran, whilst a 48% seroprevalence of brucellosis was reported amongst families associated with livestock keeping in Tanzania (Shirima et al. 2010). In the same vein, prevalences of 20% amongst cattle handlers, followed by goat rearers (10%), mixed sheep and cattle rearers (9%), mixed sheep and goat rearers (8%) and 4% each amongst sheep rearers and non-rearers of animals in Nigeria were reported (Baba, Sarkindared & Brisibe 2001).
Despite our findings, this study had some limitations. Firstly, there was no structured outline of the LM and LH groups in the area owing to the migratory nature of their work and therefore construction of a sampling frame was not feasible. Coupled with this was the gradual decline in the number of participants in the study. Secondly, men constituted the majority of the respondents, thus making inferences based on gender unreliable. However, the preponderance of men in this study may be attributable to the fact that men are generally more engaged in livestock trading in most traditional pastoral communities. Moreover, in most African cultures, men are generally allowed to talk to visitors and not women.
Conclusion
The following findings were revealed from this study. Firstly, the majority (78.5%) of people in traditional pastoral communities have poor knowledge of brucellosis with reference to what brucellosis is, its causes, symptoms in animals as well as humans, and transmission from animals to humans. Secondly, they practice risk factors that have the potential of aiding zoonotic transmission of brucellosis. Therefore, because precise knowledge of a disease is important for the development of preventive and control measures, improved information dissemination systems on the public health implications of brucellosis are required amongst livestock workers. This will go a long way towards the reduction of Brucella infection and its zoonotic transmission within and across Nigeria. Furthermore, realistic control measures will also be achieved by screening and quarantining animals before their introduction into existing herds in Nigeria and neighbouring African countries.
Acknowledgements
We are highly indebted to the livestock owners and members of their families in Yewa Division of Ogun State, Nigeria who made this study possible. Sincere appreciation also goes to Dr G.A. Adeleke of the Olabisi Onabanjo University, Ogun State, Nigeria for providing suitable logistic support to carry out this study.
Competing interests
The authors declare that they have no financial or personal relationships which may have inappropriately influenced them in writing this article.
Authors' contributions
H.K.A. (University of Ibadan) and P.I.A. (University of Ibadan) were responsible for the administration of the questionnaires, as well as collation and analysis of data. J.A.S. (Veterinary Laboratories Agency) contributed substantially to the writing of the manuscript, whilst S.I.B.C. (University of Ibadan) was responsible for the concept and design of the study. All authors contributed to the writing and final approval of the manuscript.
References
Alavi, S.M., Rafiei, A. & Nikkhooi, A., 2007, 'The effect of lifestyle on brucellosis among nomads in Khuzestan Province of Iran', Pakistan Journal of Medical Science 23, 358-360. [ Links ]
Baba, M.M., Sarkindared, S.E. & Brisibe, F., 2011, 'Serological evidence of brucellosis among predisposed patients with pyrexia of unknown origin in the north eastern Nigeria', Central European Journal of Public Health 3, 158-161. [ Links ]
Bax, H.I., Van Veelen, M.L. & Gyssen, I.C., 2007, 'Brucellosis, an uncommon and frequently delayed diagnosis', Netherlands Journal of Medicine 2, 352-355. [ Links ]
Cadmus, S.I.B. & Adesokan, H.K., 2007, 'Phenotypic characterization and spoligotype profiles of Mycobacterium bovis isolated from unpasteurized cows' milk in Ibadan, Nigeria', Tropical Veterinarian 25, 65-72. [ Links ]
Cadmus, S.I.B., Adesokan, H.K. & Stack, J., 2008, 'The use of the milk ring test and Rose Bengal test in brucellosis control and eradication in Nigeria', Journal of the South African Veterinary Association 79, 113-115. http://dx.doi.org/10.4102/jsava.v79i3.256, PMid:19244818 [ Links ]
Cadmus, S.I.B., Ijagbone, I.F., Oputa, H.E., Adesokan, H.K. & Stack, J.A., 2006, 'Serological survey of brucellosis in livestock animals and workers in Ibadan, Nigeria', African Journal of Biomedical Research 9, 163-168. [ Links ]
Georgiou, P., Nicholas, A., Mile, B. & Epameinondas, T., 2005, 'Brucellosis', New England Journal of Medicine 352, 2325-2336. http://dx.doi.org/10.1056/NEJMra050570, PMid:15930423 [ Links ]
John, K., Fitzpatrick, J., French, N., Kazwala, R., Kambarage, D., Mfinanga, G.S. et al., 2010, 'Quantifying risk factors for human brucellosis in rural northern Tanzania', PLoS ONE 5, e9968. http://dx.doi.org/10.1371/journal.pone.0009968 [ Links ]
Kang'ethe, E.K., Arimi, S.M., Omore, A.O., McDermott, J.J., Nduhiu, J.G., Macharia, J.K. et al., 2000, 'The prevalence of antibodies to Brucella abortus in marketed milk in Kenya and its public health implications', paper presented at the 3rd All Africa Conference on Animal Agriculture (AACAA), Alexandria, Egypt, 06-09 November. [ Links ]
Mandell, G.L., Bennett, J.E. & Dolin, R. (eds.), 2005, Principles and practice of infectious diseases, 6th edn., pp. 2386-2391, Churchill Livingstone, New York. [ Links ]
Mfinanga, S.G., Mørkve, O., Kazwala, R.R., Cleaveland, S., Sharp, J.M., Shirima, G. et al., 2003, 'Tribal differences in perception of tuberculosis: A possible role tuberculosis control in Arusha, Tanzania', International Journal of Tuberculosis and Lung Disease 7, 933-941. PMid:14552562 [ Links ]
Minja, K.S.G., 2002, 'Sero-epidemiological survey of Brucella antibodies in indigenous cattle and human occupational groups in Babati and Hanang districts', MVM thesis, Department of Veterinary Medicine and Public Health, Sokoine University of Agriculture. [ Links ]
Mtui-Malamsha, N., 2001, 'Epidemiological study of brucellosis in human and animals in Babati and Hanang Districts of Tanzania', MVM thesis, Department of Veterinary Medicine and Public Health, Sokoine University of Agriculture. [ Links ]
Ofukwu, A.R., Yohanna, C.A. & Abuh, H.A., 2011, Brucella infection among hospital patients in Makurdi, north-central Nigeria, viewed 29 September 2011, from http://priory.com/med/brucella.htm [ Links ]
Regassa, G., Mekonnen, D., Yamuah, L., Tilahun, H., Guta, T., Gebreyohannes, A. et al., 2009, 'Human brucellosis in traditional pastoral communities in Ethiopia', International Journal of Tropical Medicine 4, 59-64. [ Links ]
Schoonman, L., 2007, 'Epidemiology of leptospirosis and other zoonotic diseases in cattle in Tanzania and their relative risk to public health', PhD thesis, Department of Veterinary Medicine and Public Health, University of Reading. [ Links ]
Shirima, G.M., Fitzpatrick, J., Kunda, J.S., Mfinanga, G.S., Kazwala, R.R., Kambarage, D.M. et al., 2010, 'The role of livestock keeping in human brucellosis trends in livestock keeping communities in Tanzania', Tanzanian Journal of Health Research 12, viewed 12 September 2011, from http://www.ajol.info/index.php/thrb/article/view/51261 [ Links ]
SPSS version 15.0, 2006, computer software, SPSS Inc., Chicago. [ Links ]
Swai, E.S. & Schoonman, L., 2009, 'Human brucellosis: Seroprevalence and risk factors related to high risk occupational groups in Tanga Municipality, Tanzania', Zoonoses and Public Health 56, 183-187. http://dx.doi.org/10.1111/j.1863-2378.2008.01175.x, PMid:18811674 [ Links ]
Walshe, M.J., Grindle, J., Nell, A. & Bachmann, M., 1991, Dairy development in sub-Saharan Africa, World Bank Technical Paper 135, Africa Technical Department Series, World Bank, Washington DC. [ Links ]
World Health Organization, Food and Agriculture Organization of the United Nations & World Organization for Animal Health, 2004, Report of the WHO/FAO/OIE joint consultation on emerging zoonotic diseases, World Health Organization, Geneva. [ Links ]
 Correspondence to:
Correspondence to:
Simeon Cadmus
Postal address: P.M.B. 001
University Post Office
Ibadan, Nigeria
Email: simeonc5@gmail.com
Received: 08 May 2012
Accepted: 15 Nov. 2012
Published: 06 Mar. 2013














