Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
Journal of the South African Veterinary Association
versão On-line ISSN 2224-9435
versão impressa ISSN 1019-9128
J. S. Afr. Vet. Assoc. vol.82 no.4 Pretoria Dez. 2011
CLINICAL COMMUNICATION KLINIESE MEDEDELING
Barbiturate ingestion in three adult captive tigers (Panthera tigris) and concomitant fatal botulism of one
J H WilliamsI,*; L BesterII; L VenterIII; D PretoriusIV; F GreylingI,V
ISection of Pathology, Department of Paraclinical Sciences, Faculty of Veterinary Science, University of Pretoria, Onderstepoort, 0110 South Africa
IISection of Anaesthesiology, Department of Companion Animal Studies, Faculty of Veterinary Science, University of Pretoria, Onderstepoort, 0110 South Africa
IIISection of Pharmacology, Department of Paraclinical Sciences, Faculty of Veterinary Science, University of Pretoria, Onderstepoort, 0110 South Africa
IVPO Box 493, Brits, 0250 South Africa
V86 Marulani Lodge, 755 Wapadrand Street, Pretoria, 0081, South Africa
ABSTRACT
Zoo animals, including tigers, have been reported to suffer from barbiturate intoxication, with pentabarbitone being most commonly recorded. Clinical signs range from mild ataxia to general anaesthesia with recovery over hours to days with several factors affecting hepatic barbiturate metabolism and tissue partitioning. Botulism is an often fatal intoxication in man, animals, birds and certain fish. The occurrence in carnivores is uncommon to rare, with only 2 reports found of botulism in felids. This report relates to 3 adult captive cohabiting tigers that simultaneously developed signs of abdominal discomfort, progressive ataxia, recumbency and comatose sleep resembling stage 2 anaesthesia, alternating with periods of distracted wakefulness and ataxic movements. These signs occurred 4 days after being fed the carcass of a horse that had ostensibly died of colic and not been euthanased. The male tiger that was the dominant animal in the feeding hierarchy was worst affected and had to be given intravenous fluids. The female that was lowest in hierarchy was unaffected. After 48-72 hours of treatment at the Onderstepoort Veterinary Academic Hospital the females could eat and made an uneventful recovery. The male tiger showed partial recovery but died during the night a few hours after drinking water on his return to the owner. Necropsy revealed severe oesophageal dilation and impaction with decaying grass; some of this material and water were present in the pharynx and trachea, and had been aspirated causing acute widespread bronchopneumonia. Colon content tested negative for common pesticides but, together with liver, tested positive for barbiturate. Serum taken on the day of admission had tested negative for barbiturate and the residual serum from the 3 animals later tested negative for botulinum toxin. Colon and oesophageal content from the male at necropsy were positive for Clostridium botulinum toxin type C by the mouse bioassay neutralisation test, confirming that this male had had concomitant barbiturate toxicity and botulism, and had succumbed to aspiration bronchopneumonia secondary to pharyngeal, laryngeal and oesophageal paralysis and oesophageal impaction.
Keywords: barbiturate, botulinim type C toxin, botulism, bronchopneumonia, cats, felids, mouse bioassay neutralisation, oesophageal obstruction, oesophageal paralysis, tigers.
INTRODUCTION
A common problem in veterinary medicine is toxin ingestion by carnivorous species. It includes ingestion of carcasses of animals euthanased with barbiturates. This has been reported in dogs and wildlife3,15,30, and zoo animals including tigers13,17,29, with pentobarbitone being the drug most commonly found29. The clinical signs described range from mild ataxia to general anaesthesia, with recovery occurring over a period of hours to days. Previous cases of tigers with pentobarbitone poisoning have survived with intensive care17.
Botulism is a non-febrile, highly fatal intoxication of humans and animals including domestic and wild animals, certain laboratory animals, many species of domestic and wild birds, and certain fish19. Pigs are the most resistant amongst domestic species19. Botulism has uncommonly been reported in carnivores, with the majority of cases being in dogs5,6,26,27, foxes and mink20. A study in Israel showed that 29 % and 3 % of 39 golden jackals had naturally formed antibodies to botulinum toxins types C and D respectively, but red foxes and wolves were negative, suggesting that some wild carnivores do become exposed to the toxin subject to various factors including eating habits26.
Only 2 cases of botulism in felids have been published. One concerned 8 domestic cats that were fed a dead adult white pelican found beneath high-tension electricity lines11 and developed depression, anorexia and ascending paresis/paralysis. Four of the 8 cats died; the remaining 4 recovered. Botulinum intoxication of 6 circus lions (2 males and 4 females) in Britain is also recorded12. Signs developed within 6 hours of the lions being fed broiler chickens that had been inadvertently unrefrigerated for 48 hours. One female developed hindlimb ataxia and became dehydrated and died. Necropsy revealed only non-specific hypostatic congestion and pulmonary oedema with microscopic renal medullary haemorrhages and dissociation of hepatocytes. The other females were able to eat and drink, had stabilised by day 7, and recovered fully. The worst affected lion was weak but could swallow fluids given orally via syringe. This male was recumbent for 41 days but recovered. The lions were treated supportively and both males received type C botulinum antitoxin of equine origin via intraperitoneal route on day 11.
Clinical signs of botulism common to the domestic cats and the lions in the reports11,12 were depression, anorexia, normo-to hypothermia, especially hindlimb ataxia, ascending flaccid paralysis, and recumbency. The domestic cats had no cranial nerve or pain perception deficits, could eat and drink, and their recovery progressed from fore to hind limbs. The lions showed full consciousness, abdominal discomfort, variable vomition, loose faeces, gut stasis and inability to swallow, proptosis of the eyes, and dilated pupils. Recovery was from caudal to cranial.
The most common source of botulinum intoxication is ingestion of decomposed organic matter. This is mostly of animal origin, such as carrion, decomposed meat and fish products, and putrid bones eaten due to phosphorus-deficiency derived pica, but may also be of plant origin, in particular non-acid vegetables such as beans, peas or beets19. The bacterium is a spore-forming obligate Gram-positive anaerobe19. There are 6 phylogenetically and physiologically distinct bacteria: Clostridium botulinum Groups I-IV and some strains of Clostridium barati and Clostridium butyricum22, which produce 7 different protein toxin types (A to G)19. The most common toxin types are C and D, with toxin type C having 2 distinct subtypes designated C alpha and C beta or 2, the latter not being a neurotoxin19. Botulinum neurotoxin is the most potent natural toxin known19,22, and it is heat-labile (80 ºC for 10 minutes).
This report is of 3 of 4 cohabiting adult captive tigers that simultaneously showed intermittent clinical signs of deep sedation due to barbiturate ingestion. The females made uneventful recoveries, but the male made only a partial recovery despite supportive intravenous fluid therapy, and died of acute aspiration pneumonia on its return to the zoo. Various necropsy specimens were positive for barbiturate and Clostridium botulinum type C toxin.
CASE HISTORY
Clinical signs, progression and treatment
Four adult tigers, 3 females and a male, cohabiting in 1 camp were fed a horse carcass that had ostensibly died of colic and not been euthanased.
Four days later 2 females and the male tiger showed acute weakness and severe ataxia and the male became recumbent. The owner had dismissed a farm worker on the morning of the day that the 3 tigers began to show clinical signs; malicious poisoning was suspected by the owner and manager. The private veterinarian (DP) found that the smaller female had a very painful abdomen and the larger female had gas-filled intestines on auscultation. The most subservient female in the hierarchy was not affected. Dexamethasone sodium phosphate 10 mℓ (Dexa 0.2 %, Phenix, Virbac), flunixin meglumine 200 mg (Finadyne, Shering Plough AH 50 mg/mℓ), florfenicol 10 mℓ (300 mg/mℓ Nuflor, Schering Plough AH) and an analgesic spasmolytic (hyoscinen-butylbromide 4 mg/mℓ plus dipyrone 500 m/mℓ; Buscopan Compositum, Bayer Animal Health) were administered once to all 3 affected tigers.
They were transported on the following day without chemical immobilisation owing to their deeply sedated state and partial tameness to the Onderstepoort Veterinary Animal Hospital (OVAH) where they were kept in 2 large padded stables. All 3 presented as comatose, with dilated pupils, but stable vital signs; they appeared to be in stage II anaesthesia. Heart rates were slow (approximately 90 beats per minute) but stable, there was good capillary refill time, slow regular respiration (30 per minute) and blood glucose levels were in low normal range. There was no abdominal gas distension, but borborygmi were very active. Their spleens were palpable. Organophosphate or carbamates were considered unlikely as neither muscle tremors nor salivation were present. Ultrasound scans of their abdomens were normal, and excluded renal failure due to ethylene glycol. Barbiturate toxicity was suspected, but serum barbiturates were undetectable and no evidence of toxic plants or other toxins were found in their camp. The remnants of the horse carcass had been removed previously. Serum albumin, globulin, urea, creatinine, Na, K, and Ca were normal; alanine aminotransferase was slightly elevated. The haematology results showed a normal leucocyte count, with 3+ acanthocytes, large platelets and abnormal red cell membranes.
The females went through cycles of stretching, rising and staggering, then relapsing back into sleep. On the 2nd day after admission, alpha-2 agonist toxicity was suspected, upon which atipamezole HCl 5 mg/mℓ (Antisedan, Pfizer Animal Health) was administered; for a short while the respiration rate of the male was increased. On the 3rd morning the females were fully awake, alert, drinking, and playing. The male, however, would only stretch, rise and relapse back into sleep. At times he made strange neck movements as if trying to swallow or regurgitate. The faeces in his stable were black but according to the owner they had been like that for a couple of weeks prior to this episode. Since he was not drinking, intravenous isotonic crystalloid fluid (Intramed Ringer 's-Lactate solution, Fresenius Kabi) with 500 mℓ aliquots of hydroxyethyl starch and isotonic sodium chloride (Voluven, Fresenius Kabi) were administered 3 times during his stay and again prior to discharge. The decision was made to return the tigers to their home with ongoing monitoring by the referring veterinarian.
Prior to loading and transport, the females were each darted with 2 mg medetomidine HCl (20 mg/mℓ medetomidine Kyron Laboratories) using 1 mℓ Pneudart darts. The effects were reversed with atipamazole 5 mg/mℓ (Antisedan. Pfizer Animal Health), each tigress receiving 1mℓ intramuscularly, with recovery taking approximately 20 minutes. The male was loaded and transported without chemical aid. After offloading, the females began walking around and were given chicken to eat. The male showed severe ataxia, only crawled and drank 3ℓ of water. By 4 pm that day the male had not moved again since arrival so he was brought into shelter and given 4 ℓ of isotonic crystalloid fluid intravenously (Intramed Ringer's-Lactate solution, Fresenius Kabi) with glucose added at 5 %. His capillary refill time was normal at 1.5 seconds, pulse 80-90 beats per minute, respiratory rate very slow at 12-16 per minute and blood glucose low normal (4.2 mmol/ℓ ). After an hour of the infusion he started stretching, his breathing was more rhythmical and he was in a much lighter plane of consciousness. Further complications were not expected. He subsequently moved and defaecated but was found dead at 3 a.m. the following morning. A necropsy was performed at the Onderstepoort Section of Pathology, Department of Paraclinical Sciences, Faculty of Veterinary Science, University of Pretoria a few hours later.
PATHOLOGICAL FINDINGS
Necropsy and histopathology
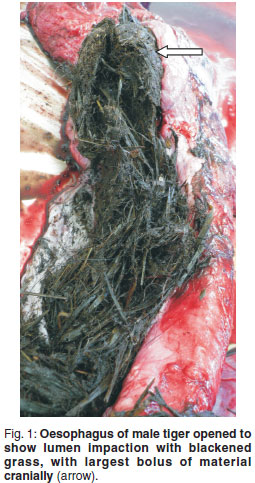
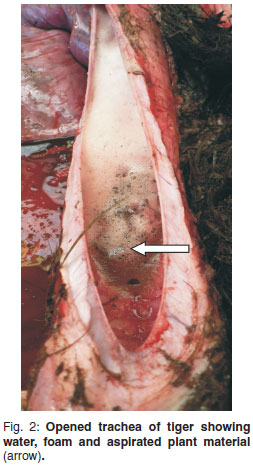
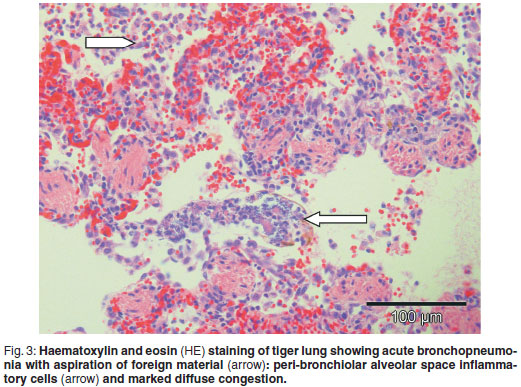
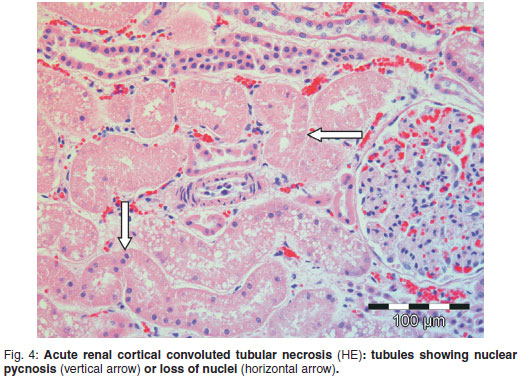
Decomposition at the time of necropsy of the tiger was mild. A peripheral blood smear showed moderate leucocytosis due to neutrophilia as well as mild eosinophilia; there were several erythrocytic Heinz bodies and occasional Howell-Jolly bodies. Faecal flotation in hypertonic saline solution was negative for helminth eggs and protozoa. Body condition was moderately obese, the tongue was cyanotic and swollen and a small amount of dark black-brown faeces exuded from the anus. The entire oesophagus and pharynx were impacted with black-stained grass in lengths of several centimetres, plus matted hairs, with the largest fist-sized compacted bolus directly above the larynx (Fig. 1). The oesophagus was slightly serpentine , appearing to be longer than the trachea. Some of the grass protruded into the laryngeal lumen and was floating in foam-topped blood-tinged water half-filling the tracheal lumen (Fig. 2). The stomach was empty of content apart from a small triangular-shaped piece of tough white autolysed fibrous connective tissue (2 × 1.5 × 0.4 cm) and a small angular piece of semi-autolysed cartilage (0.4 cm3). The gastric mucosa was lined with tacky black fluid. The small intestine contained no food and there was a small amount of black semi-fluid colon content. The mesenteric lymph nodes were moderately enlarged and microscopically active as were the small intestinal Peyer's patches. The lungs were severely congested, oedematous and cyanotic with microscopic acute foreign body (water and plant material) aspiration bronchopneumonia (Fig. 3). There was mild serosanguinous hydropericardium and occasional mild multifocal perivascular lymphoplasmacytic myocarditis. The liver was enlarged, paler than normal, friable, with accentuated lobulation. Histopathological changes were diffuse hydropic feathery cytoplasmic vacuolation of hepatocytes and associated cell swelling, mild occasional portal venous leucostasis and mild congestion. Renal cortices were tan-coloured, bulging and soft in consistency due to severe acute convoluted tubular epithelial necrosis visible histologically (Fig. 4). A large meaty thymus was still present in the anterior mediastinum. Midbrain white matter was mildly oedematous. Adrenal and salivary glands, thyroid and parathyroid, thymus, stomach, skeletal muscle and diaphragm, oesophagus, spleen, cerebellum, hippocampus, lumbar spinal cord and pancreas were without visible macroscopic or histological lesions. The cause of death was acute aspiration pneumonia secondary to pharyngeal, laryngeal and oesophageal paralysis and oesophageal impaction, with acute nephrosis and hepatosis as exacerbating lesions.
Diagnostic tests performed on necropsy specimens
Brain, liver, aqueous humour, kidney, abdominal fat and colon content were sent on ice to the Onderstepoort Veterinary Institute (OVI), Toxicology Depart-ment, for toxicological analysis. Colon content and frozen liver tested negative for pesticides, including organophosphates, organochlorines and carbamates and positive for barbiturate (Varian GC3900, MS 2100T). Attempts to further characterise and quantify the barbiturate were unsuccessful.
Pericardial fluid, oesophageal and colon contents were sent on ice to OVI Bacteriology department for botulism determination. The mouse neutralisation bioassay test using standard operating procedure23,28 showed pericardial fluid to be negative and both oesophageal and colon content to be positive for Clostridium botulinum type C toxin. Stored frozen serum from both females (pooled into a single specimen of 2 mℓ ) and 1ml of stored frozen male serum, taken on the day of admission, were negative.
Aseptically sampled lung was sent on ice to the Department of Tropical Diseases of the Faculty of Veterinary Science for bacterial culture. Klebsiella oxytoca and Bacillus spp. were aerobically cultured, and Clostridium septicum grew under anaerobic conditions. After a couple of weeks of refrigeration, stored colon content was cultured anaerobically after being heated to 80 ºC for an hour, but Clostridium botulinum was not recovered.
Formalin-fixed wax-embedded fibrous and cartilaginous tissue from the tiger's stomach lumen was tested at the Veterinary Genetics Laboratory at the Faculty of Veterinary Science, Onderstepoort, for mitochondrial DNA to determine the species of origin. This was an attempt to elucidate whether they were of equine or other species origin, which, if not equine, may have added evidence to the suspicion of malicious poisoning held by the owner and manager of the tigers. The tissue was too denatured for a result and the tests repeated on the remaining formalin-fixed cartilage and fibrous tissue were equally inconclusive.
DISCUSSION
The tigers were clearly initially suffering from ingested barbiturate toxicity that was affecting them cyclically. This pattern resembles enterohepatic barbiturate recycling or intermittent tissue partitioning into their substantial fat reserves3,18. Tissue partitioning attenuates the effects of barbiturates and it is possible for the patient to relapse as the drug re-circulates back into the plasma18.
Gastrointestinal absorption of barbiturate is variable3. Longer-acting barbiturates are less lipophilic, entering and leaving the brain more slowly than short-acting barbiturates and thus have a more gradual onset and longer duration of effect3,30. Short-acting barbiturates are metabolised very rapidly in ruminants and horses, relatively rapidly in dogs, more slowly in humans and even more slowly in cats3. There is a significant variation in barbiturate metabolism and excretion based on the barbituric derivates, the species of animal and the individual. Barbiturate metabolism is by microsomal P450 enzymes in the liver and may interfere with metabolism of other compounds by either binding to the P450 enzymes to block metabolism or, in chronic exposures, through induction of P450 enzymes to increase the rate of metabolism of substances including endogenous steroids30.
Barbiturate-induced respiratory depression is caused by suppressing chemoreceptors and this effect is more pronounced in cats where the reticular formation governs medullary control of respiration3. Onset of clinical signs depends on the route of exposure and the absence or presence of food in the stomach. Affected animals may show clinical signs within 30 minutes but often with the longer-acting barbiturates, the effects might only be seen after an hour18. The predominant signs of barbiturate intoxication are profound central nervous system (CNS) depression and anaesthesia15,18. Animals may present with severe ataxia, weakness, disorientation and loss of deep tendon reflexes. Hypothermia is common. Pulse is normally rapid but weak and respiratory depression might lead to cyanosis and death3,18. Barbiturates are excreted as the parent compound and metabolites in the urine. Excretion is dependent on urine pH and may be increased 5 to 10 times in alkaline urine through ion trapping30. Alkaline diuresis, however, is ineffective with short-acting barbiturates18.
At the time of serum collection on admission to the OVAH, the barbiturate was at full effect and would have been dissolved in the adipose tissue of the central nervous system. This, together with the tigers being mildly obese and resultant partitioning of lipophilic barbiturate in fat and muscle, might explain why serum levels of barbiturate at that stage were negative or possibly too low to measure. The amount of serum that was stored was too little for reliable or positive results. The level of barbiturate in the colon and oesophageal content was apparently too low after dilution to adversely affect the mice during the botulinum toxin bioassay. In such cases, liver tissue is the ideal sample for toxicological analysis, as high concentrations of barbiturate accumulate in this organ4,17.
The clinical signs seen in these tigers were also similar to those described previously in cats and lions with botulism11,12. Domestic cats retained all of their cranial reflexes plus superficial and deep pain sensation in all 4 limbs, but had no hind limb and weak forelimb withdrawal reflexes as well as weak patellar, sciatic, cranial tibial and gastrocnemius reflexes. A large overflowing bladder is also recorded. They started regaining hind limb withdrawal reflexes 10 h after admission, began crawling thereafter and over time recovered11.
The male tiger was at all times the worst affected. He was dominant in the feeding chain and so most likely ingested the largest amount of barbiturate. His slow and unconvincing improvement compared with that of the 2 females (despite similar treatment), was retrospectively interpreted to be due to the simultaneous progressive clinical signs of botulism. These, in hindsight, included severe muscle weakness, mydriasis, dysphagia due to oesophageal paralysis, foreign material oesophageal obstruction and the inability to vomit or regurgitate, most likely leading to the strange neck movements which had been observed by 1 of the attendants during the time after hospital admission. His initial respiration rate of 30 breaths per minute on admission had dropped to 12-16 per minute hours before he died. At necropsy, pharyngeal and laryngeal paralysis was evidenced by the aspiration of the grass and other material in the proximal oesophagus through the larynx and into the trachea, and the bronchopneumonia ensued from direct pulmonary aspiration of the plant material as well as the water that the animal drank a couple of hours prior to his demise. Acute inflammation of the lungs indicates that the aspiration was not purely agonal, and there was most likely a toxaemia and possibly septicaemia by the time of death.
The tiger only had access to grass in the home camp prior to referral to the OVAH, so the blackened grass found at necropsy in the oesophagus was at least 4 days old. The stasis and hypoxic conditions may have either allowed multiplication and toxin-production of Clostridium botulinum within the alimentary tract, or the toxin may have been ingested with the grass or with animal protein, either from the horse meat previously fed, with possible accumulation of dose over 5 days, or from other meat fed more recently and possibly maliciously to the tigers.
It is unlikely that the original colic horse was the source of the barbiturate since a tiger in an adjacent camp fed simultaneously from the same horse carcass was unaffected, unless different parts fed contained different amounts of barbiturate. Organs and neck of the fed carcass, if euthanased with barbiturates, would contain higher barbiturate concentrations especially if inadvertent subcutaneous injection occurred while using a jugular vein15. The unaffected female in the same camp was also lowest in the dominance hierarchy and would most likely have ingested the least, while the male, who was dominant, would have ingested the most. In addition, in a case of botulism in lions12, clinical signs started within 6 hours of the meal; the delay in developing signs in this case also supports the possibility of malicious poisoning with meat other than the horse carcass. It is unfortunate that mitochondrial DNA testing of the remnant animal tissues in the tiger's stomach content to elicit its species origin/s was unsuccessful.
It is speculated that the acute nephrosis in the male was most likely caused by septicaemia, hypoxia and systemic hypo-tension related to aspiration pneumonia and barbiturate intoxication7 respectively, compounded by barbiturate-and botulism-induced reduced efficiency and rate of breathing, at the time when those parameters should have been physiologically increased. All 3 large tigers in this report were healthy prior to their abrupt clinical signs and all received the same dose of flunixin meglumine (200 mg) only once just prior to admission to the hospital; the females recovered without incident. Hypoperfusion or 'shock' of many origins including cardiogenic, hypovolaemic, septic or neurogenic is the cause of renal cortical necrosis or acute tubular necrosis21. Nephrotoxins such as endo-and exo-toxins are also inciters of renal cortical necrosis.
Of the bacteria cultured from the necropsy-sampled lung specimen, Klebsiella oxytoca, a Gram-negative rod belonging to the Enterobacteriaceae, is known to cause neonatal septicaemia16 and haemorrhagic colitis in antibiotic-treated humans14, and may have genetic over-expression of β-lactamases giving rise to resistance to certain antibiotics; its origin is either environmental such as in water sources16, or from the intestinal tract. It has also been reported as an opportunistic pathogen causing severe suppurative otitis media, urogenital tract infections and pneumonia in laboratory rodents, especially those prone to diabetes mellitus or known immune deficiency, as well as in vole moles2. Faeces of 3 species of zoo-kept reptiles and of a zoo-kept jaybird were positive reservoirs for Klebsiella oxytoca1. In this tiger this bacterium therefore likely originated from the inhaled water and oesophageal plant material.
Other naturally occurring forms of botulism are wound botulism caused by Clostridium botulinum colonisation of necrotic wounds with in situ toxin production25, as has been described in horses and foals19 and intestinal colonisation with toxin production, as in human infants and adults25 and 'toxicoinfectious' botulism in horses19. Inhalation botulism could result from aerosolisation of the toxin, and iatrogenic botulism can result from injection of toxin25. High salt concentrations prevent and cold and dry conditions reduce toxin production19. Small, non-lethal doses of toxin ingested over a period of time will cause intoxication, with the cumulative dose being larger than that required to produce botulism from a single dose19. Spores are fairly heat resistant and only destroyed by high temperatures or radiation19; they are resistant to ultraviolet light, alcohols, phenolic compounds, quarternary ammonium compounds and organic mercurials. Formaldehyde, ethylene and propylene oxide will kill spores but not very rapidly19.
Monitoring, symptomatic and supportive therapy are the basis of treatment for both barbiturate overdose and botulism. Respiratory and cardiac function and body temperature should be monitored closely. Fluid therapy may be required to maintain cardiac and renal function. Re-induction of thiopental anaesthesia occurs with administration of high doses of aspirin and phenylbutazone in rats6. Non-steroidal anti-inflammatory agents displace thiopental from plasma proteins, which leads to an increased blood level of unbound barbiturate with a further depressant effect upon the CNS. Because of their highly carnivorous diet, cats have been little exposed to herbaceous compounds so they have become deficient in UDP-glucuronosyltransferase and therefore glucuronidation as a detoxifying mechanism9. Consequently, a number of drugs are eliminated slowly8,9 via other detoxifying pathways, often giving rise to prolonged half-lives of the parent drugs. Cats are therefore sensitive to the adverse effects of many drugs and toxins that are normally glucuronidated before elimination, NSAIDs being high on the list and barbiturate compounds also being partially glucuronidated7. Extra-label use of nonsteroidal anti-inflammatory drugs in cats is thus contraindicated and remains a risk, especially in circumstances where there may be concomitant dehydration, hypotension and hepatic competition for metabolism of barbiturate or other compounds, thus slowing the process in both. Renal adverse effects of NSAIDs occur due to inhibition of prostanoid synthesis resulting in reduction in renal blood flow, glomerular filtration rate, sodium retention and hyperkalaemia24. Habitual use of NSAID and non-NSAID analgesics can cause analgesic nephropathy, characterised by slowly developing papillary necrosis24. Interstitial nephritis, another adverse NSAID effect, has been postulated to be due to a cell-mediated immune response10.
Although the events described here are probably rare, they serve to highlight the importance of including botulism as a differential or concomitant diagnosis to narcotic overdose and other possibilities in captive wild felids suffering from paresis or paralysis, as well as dysphagia or other intestinal upsets. Radiographs of the head, neck and chest of the male tiger would most likely have shown the oesophageal distension with accumulated ingesta, and later the pneumonia. In hindsight, alkalinising the urine by means of administering citrate salts may have helped in the clearance of barbiturate through the kidneys by ion-trapping of barbiturate metabolites in the renal tubules30.
CONCLUSION
This report highlights the importance of ensuring that chemically euthanased animals are not used for feed and reminds the wider veterinary profession of the potential risk of secondary barbiturate poisoning in wild, captive and domestic carnivores. Anamnesis of animal carcasses to be used to feed carnivores needs to be taken with care as it can be misleading or unreliable. Owners and managers of zoological collections should regularly review their source of meat and ensure that only shot or captive-bolt-euthanased animals are supplied and fed to their carnivores. Carcasses of animals with a history of recent or long-term NSAID treatment should also not be fed, especially to felids, owing to their deficient hepatic glucuronidation detoxification pathway, and for the same reason NSAID treatment of felids is contra-indicated or to be practised with extreme caution.
Great care should be taken not only as to sources and types of food but also of general and feeding security measures for captive large wild felids owing to their great value and possible critically endangered status, as in the case of these tigers. These animals should be closely and regularly monitored for food-related clinical signs. Malicious poisoning could be a reality and necessitates forensic evidence-taking and specimen testing. A full differential diagnostic list should be drawn up, suitable diagnostic specimens taken, and certain diagnoses not necessarily ruled out despite initial negative test results. Treatment choices should take into account possible drug and metabolic interactions and be modified accordingly. Leaving carcasses out in camps to decay should be considered a potential source of various ailments including botulism and preventative botulism vaccination of valuable felids might be a future consideration.
ACKNOWLEDGEMENTS
Dr Awokie Gelaw, Bacteriology Laboratory, ARC-OVI, is acknowledged for doing the mouse bioassay tests and agreeing to work with small serum specimens. Dr Lisa Pretorius is thanked for contributing sensitive and valuable observations of subtle clinical signs of the male tiger. Thanks go to the staff of the Onderstepoort Veterinary Faculty's histopathology lab for sections cut, to Dr Cindy Harper of the Veterinary Genetics Lab for attempts at species identification of the stomach content fragments, to Johan Gouws of the Department of Tropical Diseases for culturing of the lung specimen and attempts to culture Clostridium botulinum from the stored colon contents, and Dr Jackie Picard for some information on Klebsiella oxytoca. The staff of the OVI Toxicology Department is gratefully acknowledged for doing the toxicology testing and for their usual friendly service and helpful advice.
REFERENCES
1. Ahmed A M, Motoi Y, Sato M, Maruyama A, Watanabe H, Fukumoto Y, Shimamoto T 2007 Zoo animals as reservoirs of gram-negative bacteria harboring integrons and antimicrobial resistance genes. Applied and Environmental Microbiology 73:6686-6690 [ Links ]
2. Bleich A, Kirsh P, Sahly H, Fahey J, Smoczek A, Hedrich H J, Sundberg J P 2008 Klebsiella oxytoca: opportunistic infections in laboratory rodents. Laboratory Animals 42:369-375 [ Links ]
3. Branson K R 2001 Injectable anaesthetics. In Veterinary pharmacology and therapeutics (8th edn). Iowa State University Press, Ames: 231-267 [ Links ]
4. Bush M, Phillips L G, Montali R J 1987 Clinical management of captive tigers. In Tilson R L, Seal U S (eds), Tigers of the world. Noyes Publications, Park Ridge: 171-199 [ Links ]
5. Bruchim Y, Steinman A, Markovitz M, Baneth G, Elad D, Shpigel N Y 2006 Toxicological, bacteriological and serological diagnosis of botulism in a dog. Veterinary Record 158:768-769 [ Links ]
6. Chaplin M D, Roszkowski A P, Richards R K 1973 Displacement of thiopental from plasma proteins by nonsteroidal anti-inflammatory agents. Proceedings of the Society for Experimental Biology and Medicine 143:667-671 [ Links ]
7. Charney D S, Mihic, S J, Harris R A 2006 Hypnotics and sedatives. In Brunton L L, Lazo S L, Parker K L (eds) Goodman & Gillman's The pharmacological basis of therapeutics. (11th edn): 414-420 [ Links ]
8. Court M H, Greenblatt D J 1997 Molecular basis for deficient acetaminophen glucuronidation in cats. An interspecies comparison of enzyme kinetics in liver microsomes. Biochemical Pharmacology 53:1041-1047 [ Links ]
9. Court M H, Greenblatt D J 2000 Molecular genetic basis for deficient acetaminophen glucuronidation by cats: UGT1A6 is a pseudogene, and evidence for reduced diversity of expressed hepatic UGT1A isoforms. Pharmacogenetics 10:355-369 [ Links ]
10. De Broe M E, Elseviers M M 1998 Analgesic nephropathy. New England Journal of Medicine 338:446-452 [ Links ]
11. Elad D, Yas-Natan E, Aroch I, Shamir M H, Kleinbart S, Hadash D, Chaffer M, Greenberg K, Schlosberg A 2004 Natural Clostridium botulinum type C toxicosis in a group of cats. Journal of Clinical Microbiology 42:5406-5408 [ Links ]
12. Greenwood A G 1985 Diagnosis and treatment of botulism in lions. Veterinary Record 117:58-60 [ Links ]
13. Hewitt S, Williamson S, Woodger N, Streete P, Cracknell J 2010 Secobarbital poisoning in an Amur tiger (Panthera tigris altaica) Veterinary Record 167:167-180 [ Links ]
14. Hoffmann K M, Deutschmann A, Weltzer C, Joainig M, Zechner E, Högenauer C, Hauer A C 2010 Antibiotic-associated haemorrhagic colitis caused by cytotoxinproducing Klebsiella oxytoca. Pediatrics 125: e960-e963 [ Links ]
15. Humphreys D J, Longstaffe J A, Stodulski J B 1980 Barbiturate poisoning from petshop meat: possible association with perivascular injection. Veterinary Record 107:517 [ Links ]
16. Jeong S H, Kim W M, Chang C L, Kim J M, Lee K, Chong Y, Hwang H W, Bael Y W, Chung H K, Wood I G, Ku J Y 2001 Neonatal intensive care unit outbreak caused by a strain of Klebsiella oxytoca resistant to aztreonam due to over production of chromosomal Ä-lactamase. Journal of Hospital Infection 48:281-288 [ Links ]
17. Jurczynski K, Zittlau E 2007 Pentobarbitol poisoning in Sumatran tigers (Panthera tigris sumatrae). Journal of Zoo and Wildlife Medicine 38:583-584 [ Links ]
18. Kisseberth W C, Trammel H L 1990 Illicit and abused drugs. Veterinary Clinics of North America Small Animal Practice 20:405-418 [ Links ]
19. Kriek N P J, Odendaal M W 2004 Botulism In Coetzer JAW, Tustin RC (eds), Infectious diseases of livestock Vol. 3 (2nd edn), Oxford University Press, Cape Town: 1885-1902 [ Links ]
20. Lindström M, Nevas M, Kurki J, Sauna-aho R, Latvala-Kiesilä A, Pölönen I, Korkeala H 2004 Type C botulism due to toxic feed affecting 52 000 farmed foxes and minks in Finland. Journal of Clinical Microbiology 42:4718-4725 [ Links ]
21. Maxie M G, Newman S J 2007 Urinary System. In Maxie G M (ed.), Jubb, Kennedy, and Palmer's pathology of domestic animals Vol. 2, (5th edn). City, Elsevier: 446 [ Links ]
22. Peck M W 2009 Biology and genomic analysis of Clostridium botulinum. Advances in Microbiological Physiology 55:183-265, 320 [ Links ]
23. Quinn P J, Carter M E, Markey B, Carter G R (eds), 1994 Clostridium species. In Clinical veterinary microbiology, Wolfe Publishing, Mosby-Year Book Europe 17:191-200 [ Links ]
24. Schlondorff D. 1993 Renal complications of nonsteriodal anti-inflammatory drugs. Kidney International 44:643-53 [ Links ]
25. Sobel J 2005 Botulism. Clinical Infectious Diseases 41:1167-1173 [ Links ]
26. Steinman A, Millet N, Frenkei C, King R, Shpigel N Y 2007 Presence of antibotulinum neurotoxin antibodies in selected wild canids in Israel. Journal of Wildlife Diseases 43:548-550 [ Links ]
27. Tjalsma E J 1990 Three cases of Clostridium botulinum type C intoxication in the dog. Tijdschrift fur Diergeneeskunde 115:518-521 [ Links ]
28. Walker P D Clostridium 1990 In Carter G R, Cole J R (eds), Diagnostic procedures in veterinary bacteriology and mycology. Academic Press, London: 245-251 [ Links ]
29. Vellayan S 1984 Barbiturate poisoning in Sumatran tigers (Panthera tigris sumatrae) at Zoo Nagara, Malaysia. Malaysian Veterinary Journal 8:27-32 [ Links ]
30. Volmer P A 2005 Recreational drugs. In Peterson M E, Talcott P A (eds), Small animal toxicology (2nd edn). Saunders, Philadelphia: 667 [ Links ]
Received: February 2011
Accepted: November 2011
* Author for correspondence. E-mail: june.williams@up.ac.za














