Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
Journal of the South African Veterinary Association
versión On-line ISSN 2224-9435
versión impresa ISSN 1019-9128
J. S. Afr. Vet. Assoc. vol.82 no.4 Pretoria dic. 2011
CLINICAL COMMUNICATION KLINIESE MEDEDELING
Patent ductus arteriosus repair in general practice
L James*; C Black; G Futter
Saint Francis Veterinary Hospital, 157 Main Road, Bergvliet, Cape Town, 7495 South Africa
ABSTRACT
A 3-month-old female German Shepherd puppy was presented for routine vaccination. Clinical evaluation revealed a grade 5/6 continuous murmur with the point of maximal intensity over the left 4th intercostal space. Echocardiography revealed a patent ductus arteriosus (PDA). The PDA was closed by a team of general practitioners using the Jackson-Henderson technique, via a standard 4th intercostal thoracotomy. A multi-modal approach to analgesia and premedication was employed. A successful outcome was achieved with no murmur or evidence of cardiac disease present 6 months after surgical occlusion. The literature is reviewed with an emphasis placed on choosing techniques that are appropriate to the level of expertise of the surgical and anaesthetic teams, as well as the surgical facilities available.
Keywords: canine, congenital cardiac disease, Jackson-Henderson technique, patent ductus arteriosus, thoracotomy.
INTRODUCTION
The ductus arteriosus is a foetal blood vessel connecting the pulmonary artery and the aorta in order to divert blood away from the foetal lungs6. The ductus arteriosus should close during the 1st few days of life. Patent ductus arteriosus (PDA) is a congenital cardiac condition commonly seen in puppies resulting from failure of the vessel to close2,7,9. Blood subsequently shunts continuously from the aorta to the pulmonary artery due to the higher aortic pressure. This is called a left to right shunting PDA and leads to over-circulation of the pulmonary vasculature and left side of the heart11. Studies usually show over-representation of female canine patients, ranging from 67- 78 % of patients diagnosed7,9. Closure of a left to right PDA is considered remedial15, whereas failure to close usually results in congestive heart failure by 1 year of age3. In rare cases over-circulation of the pulmonary vasculature leads to pulmonary hypertension to levels greater than the aorta and this causes a reversal of the shunt right to left causing deoxygenated blood to be pumped to the caudal half of the body11. Ligation of a completely reversed PDA (right to left) is contraindicated6. There are several surgical techniques available to close a left to right shunting defect including division and over-sewing of the 2 ends6, placement of haemostatic clips15, and more conventionally, ligation using either the standard6 or the Jackson-Henderson method10. Recently, repair has been conducted via trans-catheter coil occlusion (TCO)5. TCO was developed to allow closure of a PDA without the need for thoracotomy, but it requires fluoroscopic guidance to place the coil and is therefore usually limited to large specialist referral centres7. A recent study comparing TCO and surgical ligation for PDA showed no significant difference in mortality between the 2 techniques, but initial procedure success was better with surgical ligation7.
Minor complications were seen more frequently in cases treated with TCO, and although major complications (such as major haemorrhage, cardiac arrest and respiratory insufficiency requiring ventilator support) were more likely with surgical ligation, both approaches were considered to be acceptable PDA treatments7.
CASE HISTORY
A 13.2 kg, 3-month-old female German Shepherd presented for routine vaccination was diagnosed with a grade 5/6 continuous cardiac murmur with the point of maximal intensity over the left 4th intercostal space. The rest of the cardiac and general clinical examination was unremarkable. The owners had noticed no clinical signs and described her exercise tolerance as good. The location and type of murmur strongly suggested a PDA and the patient was referred for an echocardiogram. Colour flow doppler echocardiography revealed a left to right shunting PDA with no secondary changes in any of the cardiac chambers. Pressures over the pulmonic and tricuspid valves were within normal limits, indicating no pulmonary hypertension. No clinical signs of heart failure were present.
Based on the findings of the echocardiogram, closure of the PDA was recommended. The recommendation of referral to a specialist surgeon was declined by the owner due to financial constraints, so the decision was taken to perform the operation within general practice.
MATERIALS AND METHODS
The patient was admitted to hospital 24 hours before the surgery to allow for the application of a 50 µg/h fentanyl patch (3 µg/kg/h fentanyl) (Durogesic, Janssen, Pharmaceutica, USA) to provide intraand post-operative analgesia and food was withheld for 12 h pre-operatively. The following day she was given ketamine at 0.3 mg/kg (Anaket, Bayer AH, South Africa) and morphine at 0.65 mg/kg (morphine sulphate, Intramed (Pty Ltd), South Africa) pre-medication and anaesthesia was induced with 4 ml intravenous (IV) propofol (4 mg/kg drawn up into a syringe and then patient dosed to effect) (PropoFlo, Abbot AH, USA). Two 20-gauge IV catheters (DELTA VEN T, DeltaMed, Italy) were placed, 1 acting as a dedicated fluid line and the other for immediate intravenous access if required. Constant fluid management using Ringers lactate at 10 ml /kg/hr was employed. Adrenaline at 20 µg/kg diluted in 10 ml normal saline (Adrenotone, SCP Pharmaceuticals (Pty) Ltd.), atropine at 0.04 mg/kg (Atropine, Bayer Ltd.), lignocaine at 2 mg/kg (Lignocaine, Bayer AH), and doxapramat 5 mg/kg (Dopram, Intramed (Pty) Ltd) were drawn up to be available throughout the procedure in case of complications. The patient was maintained on 2 % inspired isoflurane (Isoflo, Abott Animal Health) and oxygen during surgical preparation. During this time the left thorax was clipped from just caudal to the scapula to the posterior aspect of the last rib. Intercostal nerve blocks of 2 ml bupivicaine (Macaine 0.5 %, Adcock Ingram Ltd, South Africa) were instilled into intercostal spaces 3, 4 and 5 in preparation for a standard 4th intercostal thoracotomy. Anaesthesia was monitored throughout the procedure with pulse oximetry, indirect blood pressure measurement, capnography, electrocardiography, heart rate, respiratory rate and temperature measurement (Cardell Veterinary Monitor Model 9405, USA). Carbon dioxide saturation was maintained below 30 % to prevent spontaneous respiration and allow manual respiration to be performed without resistance from the patient. Upon incising the parietal pleura, mechanical ventilation was started at a rate of 10-15 breaths per minute. The caudal part of the cranial left lung lobe was reflected caudally, after which the vagus nerve was dissected free and retracted dorsally using a penrose drain (Fig. 1). Bradycardia was transient and only noted while the vagus nerve was being dissected, during which period the patient remained stable. The aorta, pulmonary artery and PDA were then all clearly visible. At this point, the lung was repositioned and normal manual inflations were performed for a period of 2 min to prevent damage to the alveoli from hypo-perfusion of the previously reflected portion of lung. The lung lobe was then reflected once more to clear the surgical field.

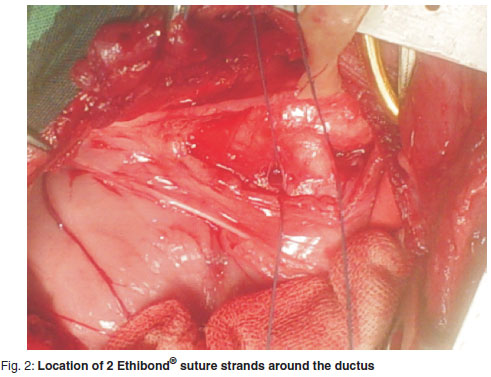
The Jackson-Henderson technique was used to close the PDA8.The mediastinum was incised dorsal to the aorta between the left subclavian and 1st aortic intercostal arteries. The index finger of the left hand was placed behind the aorta, just cranial to the PDA. Right-angled forceps were passed through the mediastinal wall at this point, guided by the index finger, from ventral to dorsal. Using the forceps, a piece of Ethibond® size 1 USP suture material was grasped at its midpoint and the forceps then pulled back to their original penetration site to leave the mid-point of the suture material cranial to the PDA and 2 free ends in the mediastinum dorsal to the aorta. The 2 free ends of suture material were then passed caudal to the PDA in a similar manner. The midpoint of the suture was cut to create 2 strands of material. The 2 strands were tied around the PDA, 1 just ventral to the aorta and the other just dorsal to the pulmonary artery (Fig. 2). The ligature adjacent to the aorta was slowly tied 1st. The other ligature was then tied in the same manner. Immediately the 'thrill' associated with the PDA disappeared and the heart rate adjusted from c. 120 bpm pre-ligation, to c. 100 bpm post-ligation. Change in heart rate was evident within 1 min of complete ligation.
The thoracic cavity was closed in a routine manner using 8, size 1 USP nylon sutures (Clinisuit, SA). Circum-costal sutures were all preplaced and then tied from dorsal to ventral. During placement of the last suture, a thoracocentesis was performed using a fenestrated tube. Suction with a 50 ml syringe was performed until a negative pressure was felt. Routine muscle, subcutaneous and skin sutures were placed. Postoperative analgesia comprised of a low-dose continuous-rate ketamine infusion (60 µg/kg/h) for 4 h, followed by morphine injections at 0.2 mg/kg every 4 h for 24 h. The fentanyl patch was removed after 72 h and was not replaced as the dog appeared comfortable at this time. Carprofen (Rimadyl, Pfizer AH) was given at a dose of 4.4 mg/kg once daily for 10 days after surgery.
RESULTS
The post-operative recovery period was smooth and unremarkable with well controlled pain. The patient was hospitalised to ensure pain control and confinement. The owners were instructed to continue the Carprofen for 3 more days, as well as exercise restrictions for a further 7 days. The sutures were removed after 14 days with no wound healing complications. At the time of writing (12 months postoperatively) there have been no problems associated with surgery. The patient remains clinically healthy with no respiratory or cardiovascular abnormalities on clinical examination and no recurrence of the murmur. The owners have declined follow-up echocardiography due to financial constraints.
DISCUSSION
Successful surgical ligation of a PDA was performed in general practice with a team of 3 non-specialist veterinarians. A multi-modal approach to analgesia, both intra-and post-operatively, is considered the gold standard for optimum pain control, prevention of wind-up pain and the reduction of side effects associated with high dosage single modal therapy4,13.In this case a combination of 4 classes of analgesics were chosen: N-methyl D-aspartate (NMDA) antagonists (ketamine), local nerve blocks (bupivicaine), opioids (morphine and fentanyl) and non steroidal anti-inflammatories (carprofen).
Two methods of surgical PDA ligation have been described. With the standard closure technique the mediastinal pleura must be separated and the vagus, phrenic and recurrent laryngeal nerves protected. After removal of the pleura from the lateral aspect of the aorta, pulmonary artery and PDA, right-angled forceps are used to dissect on the medial aspect of the ductus8. This dissection usually starts caudally and moves cranially in order to create a tunnel through which the suture can be guided and tied around the PDA6. This requires blunt and blind dissection medial to the ductus and the ductus may stretch and even tear at the right pulmonary arterial junction8. In contrast, with the Jackson-Henderson technique, no blind dissection is necessary and there are no vessels or fragile structures medial to the aorta in the mediastinum, the area through which the forceps are passed8.
There is no significant difference in mortality between the Jackson-Henderson and the standard techniques1. However, mortality from surgical PDA repair often results from haemorrhage and, although no statistical difference exists between the techniques, when it does occur, it is always in the cranial medial portion of the ductus9. This is the area in which the forceps are opened to grasp the suture following blind dissection with the standard technique9. Conversely, the Jackson-Henderson technique has been shown to result in greater PDA reperfusion postclosure14. This is assumed to result from entrapment of the mediastinal fascia14. While this may favour use of the standard technique, the clinical significance of reperfusion has yet to be established12. Consequently, the Jackson-Henderson technique was chosen in this case to avoid the need for blind dissection around the ductus by a non-specialist surgeon.
Specialist referral is usually recommended by general practitioners for PDA closure and this will often remain the most appropriate course of action for the majority of cases. Unfortunately, it is the reality in South Africa that in many cases clients will be unable to finance specialist referral. This report concludes that in these circumstances it is possible to have a favourable outcome treating a PDA with a team of general practitioners.
ACKNOWLEDGEMENTS
We would like to thank Dr Russel Leadsom for conducting the echocardiogram and for all of his advice about the case and management. We would also like to thank Dr Merle Futter and Dr Richard Sherley for their advice with this manuscript. Finally, we would like to thank our theatre support staff, without whom a successful outcome would not have been possible.
REFERENCES
1. Birchard S J 1990 Results of ligation of patent ductus arteriosus in dogs: 201 cases (1969-1988). Journal of the American Veterinary Medical Association 196:2011-2013 [ Links ]
2. Bureau S, Monnet E, Orton E C 2005 Evaluation of survival-rate and prognostic indicators for surgical treatment of left-toright patent ductus arteriosus in dogs. Journal of the American Veterinary Medical Association 227:1794-1799 [ Links ]
3. Corti L B, Merkley D, Nelson O L, Ware W A 2000 Retrospective evaluation of occlusion of patent ductus arteriosus with haemoclips in 20 dogs. Journal of the American Animal Hospital Association 36:548-555 [ Links ]
4. Egger C M 2008 The prevention and treatment of allodynia and hyperalgesia. Advances in Small Animal Medicine & Surgery 21:1-3 [ Links ]
5. Fellows C G, Lerche P, King G and Tometzki A 1998 Treatment of patent ductus arteriosus by placement of two intravascular embolisation coils in a puppy. Journal of Small Animal Practice 39:196-199 [ Links ]
6. Fossum T W 2007 Small animal surgery (3rd edn). Mosby Elsevier, Missouri [ Links ]
7. Goodrich K R, Andrew E K, Kass P H and Campbell F 2007 Retrospective comparison of surgical ligation and transarterial catheter occlusion for treatment of patent ductus arteriosus in two hundred and four dogs (1993-2003). Veterinary Surgery 36:43-49 [ Links ]
8. Henderson R A, Jackson W F 1998 Heart and great vessels: modified double ligation and division of patent ductus arteriosus. In Bojrab M J (ed.) Current techniques in small animal surgery (4th edn). William's & Wilkins, Nevada: 656-657 [ Links ]
9. Hunt G B, Simpson D J, Beck A J, Goldsmid S E, Lawrence D, Pearson M R B, Bellenger C R 2001 Intraoperative hemorrhage during patent ductus arteriosus ligation in dogs. Veterinary Surgery 30:58-63 [ Links ]
10. Jackson W F, Henderson R A 1979 Ligature placement in closure of patent ductus arteriosus. Journal of the American Animal Hospital Association 15:55-58 [ Links ]
11. Luis Fuentes V, Johnson L R, Dennis D 2010 BSAVA Manual of canine and feline cardiorespiratory medicine (2nd edn). BSAVA, Gloucester [ Links ]
12. Miller M W, Stepien R L, Meurs K M 1994 Echocardiographic assessment of patent ductus arteriosus (PDA) after occlusion. American College of Veterinary Internal Medicine. Proceedings of the 12th Annual Veterinary Medical Forum (abstr), San Francisco, California, 2-5 June 1994, 12:305-306 [ Links ]
13. Slingby L 2008 Multimodal analgesia for post operative pain relief. In Practice 30:208-212 [ Links ]
14. Stanley B J, Luis-Fuentes V, Darke P G 2003 Comparison of the incidence of residual shunting between two surgical techniques used for ligation of patent ductus arteriosus in the dog. Veterinary Surgery 32:231-237 [ Links ]
15. Van Israel N, Dukes-McEwan, French A T 2003 Long-term follow up of dogs with patent ductus arteriosus. Journal of Small Animal Practice 44:480-490 [ Links ]
Received: June 2010
Accepted: November 2011
* Author for correspondence. E-mail: saintf@mweb.co.za














