Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
Journal of the South African Veterinary Association
versión On-line ISSN 2224-9435
versión impresa ISSN 1019-9128
J. S. Afr. Vet. Assoc. vol.82 no.3 Pretoria ene. 2011
CLINICAL COMMUNICATION KLINIESE MEDEDELING
Fatal congenital anaplasmosis associated with bovine viral diarrhoea virus (BVDV) infection in a crossbred calf
A R PypersI; D E HolmII,*; J H WilliamsIII
IVeterinary Services, Western Cape Department of Agriculture and Rural Development, Private Bag X1, Elsenburg, 7607 South Africa
IIDepartment of Production Animal Studies, Faculty of Veterinary Science, University of Pretoria, Private Bag X04, Onderstepoort, 0110 South Africa
IIIDepartment of Paraclinical Studies, Faculty of Veterinary Science, University of Pretoria, Private Bag X04, Onderstepoort, 0110 South Africa
ABSTRACT
Clinical disease resulting from the vertical transmission of Anaplasma marginale has only been reported on 5 occasions despite studies demonstrating successful in utero transmission. During the reported experimental induction of congenital anaplasmosis in calves, the outcome was variable but mostly led to inapparent or mild infection. There are previous case reports of fatal congenital anaplasmosis following natural infection. The clinical findings in a 2-day-old calf presented to the Onderstepoort Veterinary Academic Hospital with clinical signs of congenital anaplasmosis, which was unresponsive to treatment, are described. Subsequent post mortem diagnostic tests revealed that this calf was co-infected with bovine viral diarrhoea virus (BVDV). It is postulated that immunosuppression resulting from BVDV infection predisposed to severe, fatal anaplasmosis in this calf.
Keywords: Anaplasma marginale, bovine, bovine viral diarrhoea, calf, congenital anaplasmosis, immunosuppression.
INTRODUCTION
Anaplasmosis in cattle is an arthropod-borne disease caused predominantly by the intraerythrocytic rickettsia Ana-plasma marginale21. Anaplasmosis is characterised by mucosal pallor, depression, inappetance, general weakness and a rapidly rising parasitaemia21. Pyrexia is an inconsistent finding21. The severity of clinical disease is directly related to the age of the animal: in animals less than 1 year old it is usually subclinical, in yearlings and 2-year-olds it is moderately severe while in older cattle it is severe and often fatal9. Vertical transmission of anaplasmosis has been documented, although its significance in the spread of the diseases is unclear13,27,28,31. Experiments attempting to demonstrate vertical transmission where progeny from known Anaplasma carrier cows were utilised, as well as where cows were acutely infected with Anaplasma during gestation, did not produce clinically ill progeny13,27,31. In utero transmission has either been demonstrated by inoculating the blood of calves born from infected mothers into susceptible animals or by the presence of circulating complement fixating antibodies13,27,28,31. There are, however, 4 cases reported where calves less than a week old were naturally infected in utero and after birth manifested severe, fatal forms of the disease1,17,18,30. A 5th case report describes a neonatal calf that became acutely ill following experimental infection and that recovered after treatment31.
The nature of the immunity to anaplasmosis is not well understood. The humoral response to infection consists of the production of antibodies while the cellular response consists of proliferation and hypertrophy of the splenic cord macro-phages, Kupffer cells of the liver, and reticuloendothelial cells of the bone marrow4. It is also known that the mechanism of resistance of calves to anaplasmosis can be overcome by splenectomy, further emphasising the importance of cell-mediated immunity (CMI) to anaplasmosis21.
The tetracycline drugs effectively inhibit the multiplication of Anaplasma in erythrocytes and have been widely used for the treatment of anaplasmosis, with parasitaemia usually decreasing to 1 % or lower within 4-7 days21. However, tetracyclines, fluoroquinolones and imidocarb dipropionate do not reliably eliminate carrier infections6. A recent study suggested that oxytetracycline produces modest changes to the structure of Anaplasma marginale and is rickettsia-static, therefore the lack of a competent immune response would manifest as treatment failure6.
Bovine viral diarrhoea (BVD) is caused by the BVD virus (BVDV), a Pestivirus (family Flaviviridae) with a worldwide distribution (including South Africa) that can occur either as cytopathic or noncytopathic strains10,23. The non-cytopathic strains are the more common biotypes of the virus and are able to cross the placenta and blood-testes barrier10,23. Horizontal transmission of the virus leads to transient infection (TI) of both biotypes of the virus with viraemia lasting less than 2 weeks23.
When vertical transmission of the non-cytopathic virus occurs during the 1st 100-120 days of pregnancy, the immune system of the foetus is evaded, and immunotolerance to BVDV occurs20. This leads to a calf that is persistently infected (PI), which starts shedding virus immediately after birth19,20. Infection during mid pregnancy (100-150 days) may lead to abortion or the birth of an abnormal or weak calf, while infection after day 150 of gestation usually leads to a healthy calf born with antibodies against BVDV23.
A BVDV PI animal is diagnosed by demonstrating the antigen with 2 consecutive tests 3-4 weeks apart, the 2nd test distinguishing a PI animal from a TI animal at the time of the 1st test15. The diagnostic tests most commonly used at present to detect viral antigen in blood, serum and tissue samples (skin, digestive tract, pancreas, mammary glands, adrenal glands, liver, respiratory tract, spleen, reproductive tract and central nervous system) are immunohistochemistry staining (IHC) and an antigen-capture enzyme-linked immunosorbent assay (AC-ELISA)8,12,15. The sensitivity and specificity of these tests range between 95 % and 100 %8,25. A reverse-transcriptase polymerase chain reaction (RT-PCR) assay is available for detection of viral RNA, and can also be applied to pooled samples15. A new short target real-time RT-PCR assay for detection of BVDV and border disease has recently been developed14.
IHC has been shown to provide the possibility of distinguishing BVD PI from TI animals on tissue samples taken only on 1 occasion, and is of particular diagnostic value in the skin, where strong BVDVimmunoreactivity (BVDV-IR) occurs in the epidermis, follicular epithelium and hair bulbs of PI animals2,12,15,16. The distribution of viral antigen in PI as well as TI animals has been studied in detail16. In PI animals, antigen is widespread in many different tissues, while in TI animals viral antigen is widespread in lymphoid tissue by day 6 after infection, but is mostly eliminated by day 9 and 13 after infection16. When IHC on skin samples is used to detect PI animals, false positive results due to TI animals may occur, especially in herds with a high prevalence of PI animals15. False negative results have also been demonstrated in a strain of BVDV which is not detected by conventional AC-ELISA or IHC29.
BVDV can infect cells of the innate immune system (e.g. neutrophils, monocytes, macrophages, and dendritic cells) and affect their function11,20,23. Lymphocytes and macrophages constitute important target cells for the replication of BVDV23. Interferon production is particularly affected and recent discoveries have shown that the virus is able to prevent interferon production against itself, while maintaining some production of interferon against foreign antigens, explaining how immunotolerance is achieved in otherwise healthy PI animals20.
Immunosuppression caused by infection with BVDV is a result of both destruction of the immunocompetent cells as well as impaired function of the surviving lymphoid cells11,19,23. Calves infected with non-cytopathic BVDV develop qualitative and quantitative abnormalities of lymphoid tissues, in particular between days 5 and 14 after infection11,16. It is apparent that when infection occurs in the presence of other pathogens, BVDV can contribute to disease associated with the other microorganisms due to its effect on CMI11.
This clinical communication proposes 1 possible reason for the sporadic severe signs of neonatal anaplasmosis in calves.
CASE HISTORY
A 2-day-old, 20 kg, female Brahman × Santa Gertrudis calf was presented to the Production Animal Clinic of the Onderstepoort Veterinary Academic Hospital (OVAH), Faculty of Veterinary Science, University of Pretoria on 14 October 2009. Although the owners had noticed the dam thoroughly lick the calf after birth it remained recumbent and was subsequently bottle-fed approximately 1  of colostrum from the dam within 24 hours of birth. The calf still did not rise and seemed weak. The owners noticed intensely yellow urine and treated her with 600 mg of long-acting oxytetracycline (Hitet 300 LA, Bayer) by intramuscular injection before transporting her without the dam to the OVAH.
of colostrum from the dam within 24 hours of birth. The calf still did not rise and seemed weak. The owners noticed intensely yellow urine and treated her with 600 mg of long-acting oxytetracycline (Hitet 300 LA, Bayer) by intramuscular injection before transporting her without the dam to the OVAH.
Clinical signs
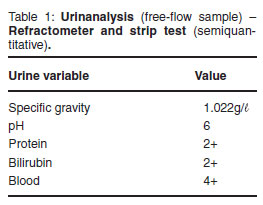
A complete clinical examination, peripheral bloodsmear for light microscopy evaluation and urinalysis with a refractometer and urine dipstick (Combur-Test, Roche Products) were performed after admission according to the standard operating procedures followed at the production animal clinic (PAC) of the OVAH. Upon initial examination the calf was weak, dehydrated, extremely icteric with very dark yellow urine, pyrexic (40.3 ºC), tachycardic (180 beats/min) and severely tachypnoeic (160 breaths/min). It was too weak to stand and had sticky orange faeces adhering to the tail and perineum. The calf had moderate proteinuria and bilirubinuria, and severe haemoglobinuria (Table 1).
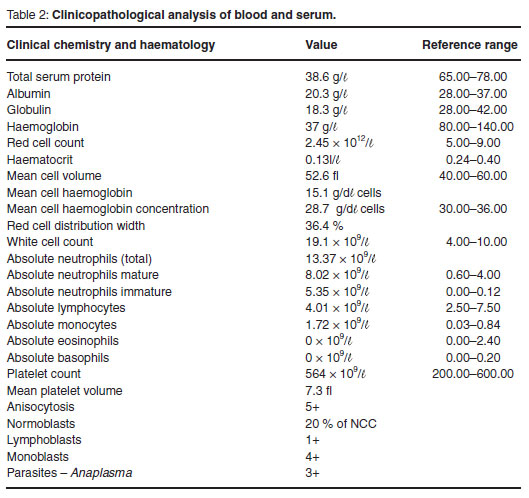
Anaplasma parasites were visible in the red blood cells (RBCs) on a peripheral blood smear. Clinicopathological tests were performed according to standard procedures at the clinical pathology laboratory of the OVAH. Serum chemistry revealed moderate hypoproteinaemia due to mild hypoalbuminaemia and moderate hypoglobulinaemia. There was severe hypochromic, normocytic (regenerative) anaemia with a marked leukocytosis characterised by pronounced left-shift neutrophilia and monocytosis (Table 2).
Treatment
Initial treatment consisted of jugular catheterisation, intravenous crystalloid and colloid fluid therapy, oxygen administration via a face mask every 2 hours for 15 minutes, nursing care in the formof regular turning to prevent the development of pressure sores, and an ocular lubricant to prevent corneal ulcers. Chemotherapy against Anaplasma consisted of 400 mg (20 mg/kg) intravenous oxytetracycline (Engemycin 10 %, Inter-vet Schering-Plough). As a mild sedative, 4 mg (0.2 mg/kg) diazepam (Valium, Aspen) was administered intravenously. The calf developed opisthotonus and horizontal nystagmus overnight and additional diazepam was administered intravenously via the jugular catheter. Bottle feeding of milk was attempted daily, and by day 3 the calf began suckling.
By day 7 it was able to stand for short periods of time and intravenous fluid therapy was stopped, yet it was subsequently unable to maintain adequate blood glucose levels. A further 200 mg (10 mg/kg) oxytetracycline was administered intravenously on days 2, 3, 6, 7, and 8 of treatment but despite this, Anaplasma parasites were still visible on the blood smear and the calf relapsed into pyrexia on day 9. The calf died 10 days after initial admission, at which time haematuria and diarrhoea were noted.
Post mortem findings
Macroscopic examination revealed hepatomegaly with severe hepatic cholestasis and accentuated lobulation with multifocal mottling, generalised renal papillary and multifocal cortical necrosis with pigmentation, moderate lung oedema, interstitial pneumonia, mild accumulation of serous fluid in body cavities and an urachal abscess.
Histological findings in formalin-fixed, alcohol-dehydrated, paraffin wax-embedded tissue sections stained with haematoxylin and eosin revealed purulent pyelonephritis and embolic nephritis, hepatosis with multifocal bacterial hepatic microabscesses, portal bile duct hyperplasia and scattered clusters of neutrophils in sinusoids, mild diffuse interstitial pneumonia and marked, especially neutrophilic, leukostasis of most blood vessels in the brain sections.
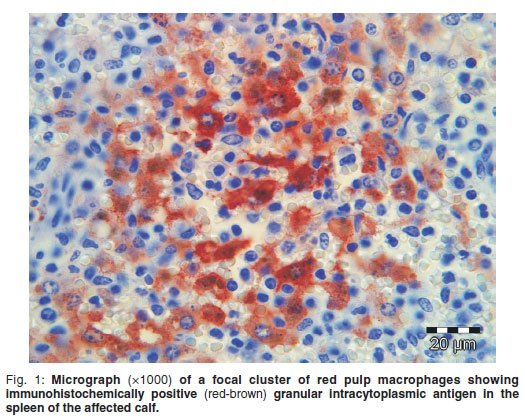
Eleven months later, immunohistochemical (IHC) staining of the same wax-embedded tissues for BVDV antigen using an avidin-biotin complex Elite kit (Vector Laboratories) showed no antigen in liver, lung, kidney and brain sections, but 2 focal clusters of splenic red pulp macrophages showed positive granular intracytoplasmic antigen similar to that observed in the positively-stained control section (Fig. 1).
Subsequent to the latter results becoming available, frozen-stored serum of the calf drawn by venipuncture on day 1 was subjected to the AC-ELISA test for BVDV (IDEXX Laboratories Inc) approximately 1 year after sampling. The optical density (OD) of the test sample was 0.713, while those of the 2 positive and 2 negative control samples were 1.151 and 2.209, and 0.082 and 0.252, respectively. Using standard operating procedure, this was interpreted as a positive result for BVDV antigen.
A year after admission an ear biopsy from the dam of the calf was subject to BVDV IHC staining, which was negative for antigen when compared with a simultaneous correctly-staining known positive control section. The RT-PCR test (Onderstepoort Veterinary Institute) performed on a whole blood sample of the cow was also negative for BVD antigen.
DISCUSSION
Although only anaplasmosis was diagnosed at the time of treatment, the calf was co-infected with BVDV, as evidenced by the persistent viraemia that lasted from 2 days after birth up to day 12 when it died. Although the duration of the viraemia is suggestive of a PI, the limited distribution of antigen on IHC examination in this case (in 2 clusters of splenic macrophages) was more typical of that described towards the end of a transient infection16. The negative ear IHC and blood PCR results for BVD antigen in the dam adds to the uncertainty about the PI status of the affected calf23.
The IHC test on formalin-fixed ear notch samples can decrease in sensitivity over time12, but in this case the spleen sample had been alcohol-dehydrated and embedded in wax and still tested positive after 11 months, consistent with previous reports that indicate that wax embedded samples maintain their sensitivity and specificity for extended periods15,29.
If it is accepted that the immune response to Anaplasma infection in calves is primarily based on CMI and that infection with BVDV causes immunosuppression due to destruction and impaired function of white blood cells (especially macrophages and lymphocytes), it is reasonable to suggest that the clinical signs and treatment failure of anaplasmosis in this calf were due to the immunosuppressive effects of the co-infection with BVDV. An additional hypothesis can be advanced that since calves very rarely show clinical signs of anaplasmosis after infection in utero, the 4 previously reported cases of acutely ill neonates were possibly immune-compromised by an unknown factor.
At the time that oxytetracycline treatment was instituted, the immunosuppressed status of the calf was not suspected, hence the use of a rickettsiastatic did not seem unreasonable. However, in hindsight the failure of the oxytetracycline therapy evidenced by the high parasitaemia still present on day 9 of treatment supports the suspicion that the calf was immunosuppressed.
Although the owners administered colostrum to the calf, its serum chemistry results suggested that inadequate passive transfer occurred. This should be suspected or investigated in neonates with a serum protein level of less than 52 g/ 24, but this was not relevant to the present case because the calf was exhibiting clinical signs of anaplasmosis as soon as the owners first saw her after birth and thus ingestion of adequate colostrum would have had no bearing on the initial presentation. Furthermore, calves under the age of 6 months, irrespective of the immune status of their dams, are normally resistant to severe clinical anaplasmosis21, supporting the fact that immunity to anaplasmosis is not antibody dependent. The (partial) failure of passive transfer in this calf most likely complicated the case by contributing to the development of the urachal abscess and signs of septicaemia evident at necropsy. The latter was likely the principal cause of death.
24, but this was not relevant to the present case because the calf was exhibiting clinical signs of anaplasmosis as soon as the owners first saw her after birth and thus ingestion of adequate colostrum would have had no bearing on the initial presentation. Furthermore, calves under the age of 6 months, irrespective of the immune status of their dams, are normally resistant to severe clinical anaplasmosis21, supporting the fact that immunity to anaplasmosis is not antibody dependent. The (partial) failure of passive transfer in this calf most likely complicated the case by contributing to the development of the urachal abscess and signs of septicaemia evident at necropsy. The latter was likely the principal cause of death.
Further research is needed into the relationship between immunosuppression caused by BVDV infection and the development of concurrent rickettsial diseases, in particular in neonates. The findings of this case suggest that the diagnosis of congenital anaplasmosis warrants further investigation to rule out immunosuppressive conditions such as BVDV infection that may be present in the herd.
ACKNOWLEDGEMENTS
The authors thank Dr Louise Biggs for her dedicated management of the case and the Department of Production Animal Studies of the Faculty of Veterinary Science, University of Pretoria for financial support.
REFERENCES
1. Bird J E 1973 Neonatal anaplasmosis in a calf. Journal of the South African Veterinary Association 44: 69-70 [ Links ]
2. Brodersen B W 2004 Immunohistochemistry used as a screening method for persistent bovine viral diarrhoea virus infection. Veterinary Clinics of North America: Food Animal Practice 20: 85-93 [ Links ]
3. Brown G B, Bolin S R, Frank D E, Roth J A 1991 Defective function of leukocytes from cattle persistently infected with bovine viral diarrhea virus, and the influence of recombinant cytokines. American Journal of Veterinary Research 52: 381-387 [ Links ]
4. Buening G M 1973 Cell-mediated immune responses in calves with anaplasmosis. American Journal of Veterinary Research 34: 757-763 [ Links ]
5. Carson C A, Sells D M, Ristic M 1976 Cell-mediated immunity in bovine anaplasmosis and correlation with protection induced by vaccination (a review). Veterinary Parasitology 2: 75-81 [ Links ]
6. Coetzee J F, Apley M D, Kocan K M 2006 Comparison of the efficacy of enrofloxacin, imidocarb and oxytetracycline for clearance of persistent Anaplasma marginale infections.Veterinary Therapeutics 7: 347-360 [ Links ]
7. Hessman B E, Fulton R W, Sjeklocha D B, Murphy T A, Ridpath J F, Payton M E 2009 Evaluation of economic effects and the health and performance of the general cattle population after exposure to cattle persistently infected with bovine viral diarrhea virus in a starter feedlot. American Journal of Veterinary Research 70: 73-85 [ Links ]
8. Hill F I, Reichel M P, McCoy R J, Tisdall D J 2007 Evaluation of two commercial enzyme-linked immunosorbent assays for detection of bovine viral diarrhoea virus in serum and skin biopsies of cattle. New Zealand Veterinary Journal 55: 45-48 [ Links ]
9. Jones E W, Brock W E 1966 Bovine anaplasmosis: Its diagnosis, treatment and control. Journal of the American Veterinary Medical Association 119: 1624-1633 [ Links ]
10. Kabongo N, Van Vuuren M 2004 Detection of bovine viral diarrhoea virus in specimens from cattle in South Africa and possible association with clinical disease. Journal of the South African Veterinary Association 75: 90-93 [ Links ]
11. Kapil S, Walz P, Wilkerson M, Minocha H 2005 Immunity and immunosuppression. In Goyal S M, Ridpath J F (eds) Bovine viral diarrhea virus: diagnosis, management and control. Blackwell Publishing, Ames: 157-170 [ Links ]
12. Khan F, Vorster J H, van Vuuren M, Mapham P 2011 Evaluation of the effects of long-term storage of bovine ear notch samples on the ability of 2 diagnostic assays to identify calves persistently infected with bovine viral diarrhoea virus. Journal of the South African Veterinary Association 82:18-23 [ Links ]
13. Kuttler K L, Marble D W, Matthews M S 1962 Anaplasmosis complement-fixation response in calves from anaplasmosisinfected dams. American Journal of Veterinary Research 23: 1007-1010 [ Links ]
14. La Rocca S A, Sandvik T 2009 A short target real-time RT-PCR assay for detection of pestiviruses infecting cattle. Journal of Virological Methods 161: 122-127 [ Links ]
15. Larson R L, Brodersen B W, Grotelueschen D M, Hunsaker B D, Burdett W, Brock K V, Fulton R W, Goehl D R, Sprowls R W, Kennedy J A, Loneragan G H, Dargatz D A 2005 Considerations for bovine viral diarrhoea (BVD) testing. Bovine Practice 39: 96-100 [ Links ]
16. Liebler-Tenorio E M, Ridpath J E, Neill J D 2004 Distribution of viral antigen and tissue lesions in persistent and acute infection with the homologous strain of noncytopathic bovine viral diarrhoea virus. Journal of Veterinary Diagnostic Investigation 16: 388-396 [ Links ]
17. Norton J H, Parker R J, Forbes-Faulkner J C 1983 Neonatal anaplasmosis in a calf. Australian Veterinary Journal 60: 348 [ Links ]
18. Paine G D, Miller A S 1977 Anaplasmosis in a newborn calf. The Veterinary Record 100: 58 [ Links ]
19. Peterhans E, Jungi T W, Schweizer M 2003 BVDV and innate immunity. Biologicals 31: 107-112 [ Links ]
20. Peterhans E, Schweizer M 2010 Pestiviruses: how to outmanouver your hosts. Veterinary Microbiology 142: 18-25 [ Links ]
21. Potgieter F T, Stoltsz W H 2004 Bovine anaplasmosis. In Coetzer J A W, Tustin R C (eds) Infectious diseases of livestock (2nd edn). Oxford University Press, Cape Town: 594-616 [ Links ]
22. PotgieterLND 1995 Immunology of bovine viral diarrhea virus. Veterinary Clinics of North America: Food Animal Practice 11: 501-520 [ Links ]
23. PotgieterLND 2004 Bovine viral diarrhoea and mucosal disease. In CoetzerJAW, Tustin R C (eds) Infectious diseases of livestock (2nd edn). Oxford University Press, Cape Town: 946-969. [ Links ]
24. Ristic M 1960 Anaplasmosis. Advances in Veterinary Science 6: 128-129 [ Links ]
25. Russell K E, Roussel A J 2007 Evaluation of the ruminant serum chemistry profile. Veterinary Clinics of North America: Food Animal Practice 23: 403-426 [ Links ]
26. Sandvik T 2005 Selection and use of laboratory diagnostic assays in BVD control programmes. Preventative Veterinary Medicine 72: 3-16 [ Links ]
27. Swift B L, Paumer R J 1976 Vertical transmission of Anaplasma marginale in cattle. Theriogenology 6: 515-521 [ Links ]
28. Trueblood M S, Swift B L, Bear P D 1971 Bovine fetal response to Anaplasma marginale. American Journal of Veterinary Research 32: 1089-1090 [ Links ]
29. Walz P H, Groom D L, Passler T, Ridpath J F, Tremblay R, Step D L, Callan R J, Givens M D 2010 Control of bovine viral diarrhoea virus in ruminants. Journal of Veterinary Internal Medicine 24: 476-486 [ Links ]
30. Wandera J G, Munyua W K 1971 Severe anaplasmosis in a 4-day old calf. Bulletin of Epizootic Disease in Africa 19: 219-221 [ Links ]
31. Zaugg J L, Kuttler K L 1984 Bovine anaplasmosis: in utero transmission and the immunologic significance of ingested colostral antibodies. American Journal of Veterinary Research 45: 440-443 [ Links ]
Received: December 2010.
Accepted: July 2011.
* Author for correspondence. E-mail: dietmar.holm@up.ac.za














