Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
Journal of the South African Veterinary Association
On-line version ISSN 2224-9435
Print version ISSN 1019-9128
J. S. Afr. Vet. Assoc. vol.81 n.1 Pretoria Jan. 2010
CLINICAL COMMUNICATION KLINIESE MEDEDELING
Multiple eyelid apocrine hidrocystoma in a domestic short-haired cat
A SivagurunathanI,*; A D GoodheadI; E C Du PlessisII
IOphthalmology Section, Department of Companion Animal Clinical Studies, Faculty of Veterinary Science, University of Pretoria, Private Bag X04, Onderstepoort, 0110 South Africa
IIVeterinary Anatomical Pathologist, Golden Vetpath, a division of IDEXX
ABSTRACT
A 12-year-old domestic short-haired cat was referred for evaluation of periocular masses. The tail had similar masses and was amputated previously by the referring veterinarian. On examination, multiple pigmented nodules, 3-15 mm in diameter, were found in the periocular skin, primarily involving the palpebral eyelid margin. A wedge excisional biopsy revealed small cuboidal cells forming multiple tubular and cystic structures indicative of apocrine cystadenomas, similar to apocrine hidrocystomas described in humans. The nodules were lanced followed by liquid nitrogen cryofreezing.
Keywords: cat, eyelid margin, hidrocystoma, multifocal, lancing and cryosurgery.
INTRODUCTION
Tumour and tumour-like lesions of the eyelids are more common in dogs than cats32. In the feline, malignant tumours outnumber benign types, with eyelid neoplasms essentially arising from the haired skin10,22,32. Based on 1 study, squamous cell carcinomas, fibrosarcomas and adenocarcinomas constitute 73.5 % of all feline eyelid tumours22.
Apocrine hidrocystomas in cats are rare, solitary and most often occur in the skin of the head, pinna, neck and axilla, limbs and tail28. All variants of apocrine sweat gland tumours constitute 3 % of feline skin tumours17. The term apocrine cystadenoma is a more accurate designation and is synonymous with apocrine hidrocystoma which is one of many types of apocrine sweat gland tumours23. Although apocrine sweat glands exist within the skin of the eyelid and the eyelid margin, where they are called glands of Moll, apocrine sweat gland tumours in this location are uncommon in small animals3,19,27. Multiple cystic lesions originating from apocrine sweat glands and resembling apocrine hidrocystomas of humans have been described in 2 separate papers involving eyelids of 5 Persian cats and 1 Himalayan cat1,7,8.
CASE HISTORY
A 12-year-old, black, neutered, female domestic short-hair cat was referred for evaluation of slowly enlarging, multiple periocular masses around the left eye of 12 months' duration. An excisional biopsy of a similar cystic lesion on the mid tail and left upper eyelid were performed by the referring veterinarian. The histopathology report confirmed benign, apocrine cystadenoma.
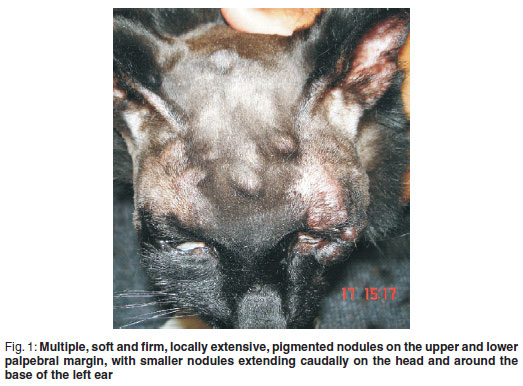
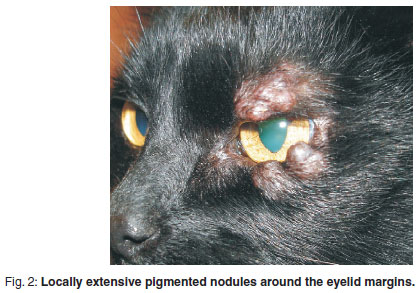
On ophthalmic examination, multiple, soft and firm, locally extensive, pigmented nodules were found on the upper and lower palpebral margin, with smaller nodules extending caudally on the head and around the base of the left ear (Fig. 1). The lesions were nonpruritic, nonpainful, with no evidence or history of self mutilation/trauma with the exception of the lesions on the tail, which was previously amputated. The nodules were measured using callipers and were 3-15 mm in diameter extending dorsally from the medial canthus and around the lateral canthus to the mid-ventral palpebral margin (Fig. 2). The skin overlying the nodules was thin, pigmented and alopecic. The referring veterinarian had previously amputated the tail, based on poor response after surgical lancing and wound management. The nodules previously described on the tail appeared to have a similar presentation to the eyelid margin nodules. No other ophthalmic abnormalities were noted. Eyelid melanoma and mast cell tumour were considered as possible differential diagnosis based on pigmentation and location. Thoracic radiographs performed ruled out the possibility of metastasis. Fine-needle aspirates of the nodules were not taken during our evaluation based on previously published reports showing poor correlation of diagnostic cytology for apocrine hidrocystomas. A tentative diagnosis for apocrine hidrocystoma was made based on the previous biopsy report from the amputated tail mass as well as the location, behaviour and distribution of the mass.
A wide surgical area was clipped from the zygomatic arch to the base of the ears caudally. The patient was premedicated with midazolam (Dormicum, Roche 5 mg/m ) and morphine sulphate (Micromorphine, Microhealthcare Bethlehem SA 10 mg/m
) and morphine sulphate (Micromorphine, Microhealthcare Bethlehem SA 10 mg/m ), induced with Alfaxalone (Alfaxan-CD, Kyron 10 mg/m
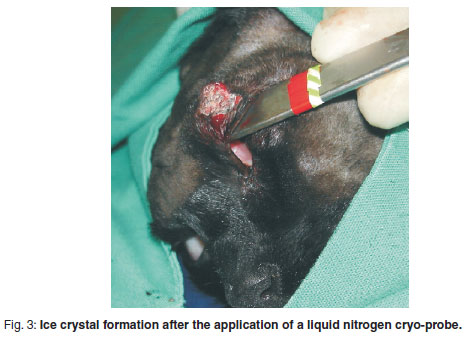
), induced with Alfaxalone (Alfaxan-CD, Kyron 10 mg/m ) and maintained on isoflurane gaseous anaesthesia. Treatment consisted of lancing the palpable nodules, followed by cryosurgery using a liquid nitrogen Cryopen (D&ECryo, 5 mm tip), utilising 2 freeze-thaw cycles of 40 seconds and 20 seconds, 20 minutes apart (Fig. 3). An excisional wedge biopsy sample was taken from a smaller nodule on the ventral eyelid margin to rule out the possibility of other eyelid tumours. At 1 month post-surgery, only a single firm crusting nodule 3 mm in diameter on the ventral eyelid margin was visible (Fig. 4). Hair follicles around the affected area had regrown. Previous cystic nodules were not palpable at their locations. At 8 months post-surgerya5mmfirmnodule was visible and palpable on the dorsal palpebral eyelid margin during a revisit checkup. The rest of the eyelid was normal with new hair growth. Since no signs of lacrimation, pain or discomfort were noted, with consideration of the patient's age and slow recovery from the previous anaesthetic procedure, the owner was advised to leave the nodules untreated unless deemed essential.
) and maintained on isoflurane gaseous anaesthesia. Treatment consisted of lancing the palpable nodules, followed by cryosurgery using a liquid nitrogen Cryopen (D&ECryo, 5 mm tip), utilising 2 freeze-thaw cycles of 40 seconds and 20 seconds, 20 minutes apart (Fig. 3). An excisional wedge biopsy sample was taken from a smaller nodule on the ventral eyelid margin to rule out the possibility of other eyelid tumours. At 1 month post-surgery, only a single firm crusting nodule 3 mm in diameter on the ventral eyelid margin was visible (Fig. 4). Hair follicles around the affected area had regrown. Previous cystic nodules were not palpable at their locations. At 8 months post-surgerya5mmfirmnodule was visible and palpable on the dorsal palpebral eyelid margin during a revisit checkup. The rest of the eyelid was normal with new hair growth. Since no signs of lacrimation, pain or discomfort were noted, with consideration of the patient's age and slow recovery from the previous anaesthetic procedure, the owner was advised to leave the nodules untreated unless deemed essential.

Histopathology
Tissue specimens from the lower eyelid margin were fixed in buffered 10 % formalin for histological examination. The samples were processed and cut according to routine methods, and stained with the usual haematoxylin-eosin stain after which they were evaluated.
The dermis of the eyelid contained multiple cystic neoplastic nodules that were well-demarcated but unencapsulated. The cells lining the cysts were small cuboidal epithelial cells arranged in proliferating multiple layers, or often with a bilayered appearance typical of the apocrine sweat glands. These lining cells also formed multiple small glandular/ tubular structures. Some of the tubules contained lightly eosinophilic secretions in the lumen. The neoplastic epithelial cells had oval hyperchromatic, fairly bland nuclei showing chromatin clumping and margination with few nuclei containing central small nucleoli. The cytoplasm was scant in amount and lightly eosinophilic in appearance and few cells showed apical blebbing. Minimal mitoses were present.
Figure 5 illustrates the glandular/tubular and cystic structures formed by the neoplastic apocrine epithelial cells. Some tubules contain eosinophilic secretions. Figure 6 clearly shows the bilayered appearance of the proliferating cells evident in some areas of the neoplasm.

DISCUSSION
Some apocrine adenomas are also referred to as apocrine cystadenomas when some of the neoplastic tubular structures form cystic spaces. Apocrine cystadenomas are referred to as apocrine hidrocystomas in medical nomenclature1,6,30. They are sometimes called Moll's gland cysts when they originate from the apocrine glands of Moll. The term is confusing and apocrine cystadenoma would more clearly indicate the neoplastic nature of this specific tumour. Multiple lesions are rare in humans and most often affect the face and eyelids. The eyelid lesions of this cat showed the same clinical signs and histological features as those reported in 2 previous studies involving 4 cases (3 Persian cats and 1 Himalayan cat) and 2 cases (Persian cats), respectively.7,8. Histologically they meet the criteria of cystic structures originating multifocally from apocrine sweat glands in the eyelids known as glands of Moll. Apocrine hidrocystomas of the eyelids in humans and cats consist of unilocular and multilocular cystic cavities in the dermis, lined by 1 or several layers of cuboidal to columnar epithelial cells showing decapitation secretion1,6.
The cause of apocrine hidrocystoma is unknown; however, a number of theories exist regarding its pathogenesis in humans. Some authors claim that the lesion is a retention cyst caused by obstruction of the excretory duct10,34. Others believe it represents an adenomatous proliferative tumour (cystadenoma) because of the papillary projections of the cyst wall18,31. Recent histological findings in the cat suggest that the lesions are of a proliferative rather than a retention process because the epithelium was not totally flattened as seen with retention cysts7. Furthermore immunohistochemistry for Ki67 antigen demonstrated that these areas were active foci of epithelial apocrine proliferation7.
Apocrine hidrocystomas are rare in cats and occur most commonly on the head, neck and limbs27. These tumours are uncommon to rare in cats and are usually 1 cm or smaller. To our knowledge this is the 3rd case report describing multiple eyelid hidrocystomas in the cat. The 6 cases previously described have several features in common. All were older animals (7-11 years of age). Five of the 6 cats previously described were Persian cats, suggesting a possible breed predisposition. This is in contrast to the domestic short-haired cat presented in this paper. The gross appearance of the eyelid masses was very similar to that described previously7,8. Multiple, well-circumscribed, tense to fluctuant, smooth nodular structures of 2-10 mm in diameter located in the upper and lower eyelids of cats are highly suggestive of apocrine hidrocystomas. Definitive diagnosis requires excisional biopsy and histopathological examination.
Differential diagnosis for these lesions includes apocrine adenoma, basal cell tumour, adenocarcinoma, fibrosarcoma, mast cell tumour, melanoma, fungal blepharitis and hordoleum17,22,28.
In humans, eyelid apocrine hidrocystomas are benign lesions30. The behaviour appears to be similar in the cat and the therapeutic options include observation without treatment, drainage and surgical excision8. If the lesions are multiple and voluminous, surgical resection may not allow adequate tissue apposition for normal eyelid function. There is also a potential for more lesions to appear at other sites in the eyelids8.
Various treatment options have been described for apocrine hidrocystoma, which include surgical excision, chemical ablation using intralesional trichloracetic acid, diode photocoagulation, liquid nitrous oxide cryotherapy or combinations of the above12,18,33. Successes with these modalities are variable depending on the nature, extent and location of the lesions. Extensive eyelid lesions require surgical planning in order to preserve eyelid function and form, consequently preserving ocular integrity. At present, knowledge about the prevalence and success in the treatment of apocrine hidrocystoma in cats is limited.
The role of cryosurgical techniques in the treatment of tumours of the eye has matured in recent years. The principal use of cryosurgery is in treatment of eyelid tumours Cryosurgery is best suited for tumours with well-defined borders15. Even so, the technique has been utilised for tumours with poorly defined borders involving conjunctiva, such as squamous cell carcinoma, melanoma and lymphoid tumours, which were managed successfully with combined techniques4,13,24. The behaviour of the tumour generally determines the aggressiveness of the cryosurgery technique. Of the various techniques employed, the most lethal effect of repeated freezing results when a complete thawing of the tissue precedes the 2nd freeze-thaw cycle15. This requires considerable time, ranging from 20-30 min depending on the volume of tissue frozen15. Recent experimental reports have suggested that a tissue temperature of -20 ºC to -30 º will produce cell death, but cancer cell death in that range may be uncertain or incomplete9,25,26. Other recent reports have reaffirmed past opinions that temperatures at -40 º to -50 ºC range must be produced to be certain of cell death14,20. The limitation is necrosis of healthy tissue with the latter technique14,20.
Our treatment option involving surgical lancing and concurrent cryofreezing utilising 2 freeze-thaw cycles were based on anecdotal reports from veterinary ophthalmologists who have successfully managed similar eyelid lesions.
CONCLUSION
When previously published papers on apocrine hidrocystoma are considered and our observations through this single case report, a breed predisposition for Persians and Himalayans may well contribute to the occurrence of these lesions; however, it may not be exclusive. Furthermore, the combination of lancing, drainage and cryosurgery appears to have a good prognosis but recurrence is possible if an appropriate tissue temperature is not attained in the 1st freeze-thaw cycle.
ACKNOWLEDGEMENT
The authors would like to acknowledge Dr Shane Bartie for the case referral and the valuable information.
REFERENCES
1. Alessi E, Gianotti R, Coggi A 1997 Multiple apocrine hidrocystomas of the eyelids. Veterinary Pathology 34: 232-234 [ Links ]
2. Apple D J, Rabb M F 1998 Conjunctiva and eyelids. In Ocular pathology, clinical applications and self assesment (5th edn). Mosby, St Louis: 563-604 [ Links ]
3. Bacha W J, Bacha L M 2000 The eye. In Color atlas of veterinary histology (2nd edn). Lippincott/Williams & Wilkins, Philadelphia: 247 [ Links ]
4. Bajaj M S, Pushker N, Kashyap S, Balasubramanya R, Chandra M, Ghose S 2003 Conjunctival malignant melanoma. Orbit 22: 47-53 [ Links ]
5. Banks W J 1993 Eye and ear. In Applied veterinary histology (3rd edn). Mosby Year Book, St Louis: 484 [ Links ]
6. Bures F A, Kotinek J 1982 Differentiating between apocrine and eccrine hidrocystoma. Cutis 29: 616-620 [ Links ]
7. Cantaloube B, Raymond-Letron I, Regnier A 2004 Multiple eyelid apocrine hidrocystomas in two Persian cats. Veterinary Ophthalmology 7: 121-125 [ Links ]
8. Chaitman J, WoerdtAvd, Bartick T E 1999 Multiple eyelid cysts resembling apocrine hidrocystomas in three persian cats and one Himalayan cat. Veterinary Pathology 36: 474-476 [ Links ]
9. Chosy S G, Nakada S Y, Lee F T, Warner T F 1998 Monitoring renal cryosurgery: predictions of tissue necrosis in swine. Journal of Urology 159: 1370-1374 [ Links ]
10. Combemale P, Kanitakis J, Dupin N, Parraud C, Guigon M 1997 Multiple Moll's gland cysts (apocrine hidrocystomas) of the eyelids. Dermatology 194: 195-196 [ Links ]
11. D'hermies F, Morel X, Meyer A, Bairi R, Elmaleh C, Renarc G 1999 Hidrocytome noir du bord libre de la paupière. Journal Français d'Ophthalmologie 22: 599-601 [ Links ]
12. Echague A V, Astner S, Chen A A, Anderson R 2005 Multiple apocrine hidrocystoma of the face treated with a 1450-nm diode laser. Archives of Dermatology 141: 1365-1367 [ Links ]
13. Eichler M D, Fraunfelder F T 1994 Cryotherapy for conjunctival lymphoid tumors. American Journal of Ophthalmology 118: 463-467 [ Links ]
14. Forest V, Peoc'h M, Campos L, Guyotat D, Vergnon J M 2005 Effect of cryotherapy or chemotherapy on apoptosis on a nonsmall-cell lung cancer xenografted into SCID mice. Cryobiology 50: 29-37 [ Links ]
15. Gage A A, Baust J G 2007 Cryosurgery for tumors. Journal of the American College of Surgeons 205: 342-356 [ Links ]
16. Glaze M B, Gelatt K N 1999 Feline ophthalmology. In Gelaat K N Veterinary ophthalmology (3rd edn). Lippincott/Williams & Wilkins, Philadelphia: 1001-1003 [ Links ]
17. Goldschmidt M H, Shofer F S 1992 Skin tumors of the dog and cat. Pergamon Press, Oxford: 2,3, 278-282 [ Links ]
18. Henderer J D, Tanenbaum M 2000 Excision of multiple eyelid apocrine hidrocystoma via an en-bloc lower eyelid blepharoplasty incision. Ophthalmic Surgical Lasers 31: 157-161 [ Links ]
19. Hirai T, Mubarak M, Kimura T, Ochiai K, Itakura C 1997 Apocrine gland tumor of the eyelid in a dog. Veterinary Pathology 34: 232-234 [ Links ]
20. Mala T 2006 Cryoablation of liver tumors - review of mechanisms, techniques and clinical outcome. Minimal Invasive Therapy Allied Technologies 15: 9-17 [ Links ]
21. Malliah U, Dickinson J 2001 Bilateral multiple eyelid apocrine hidrocystomas and ectodermal dysplasia. Archives of Ophthalmology 119: 1866-1867 [ Links ]
22. McLaughlin S A, Whitley R D, Gilger B C, Wright J C, Lindley D M 1993 Eyelid neoplasms in cats: a review of demographic data (1979 to 1989). Journal of the American Animal Hospital Association 29: 63-67 [ Links ]
23. Murphy G F, Elder D E 1991 Non-melanocytic tumors of the skin. In Atlas of tumor pathology. Armed Forces Institute of Pathology, Washington, DC: 109-110 [ Links ]
24. Peksayar G, Altan-Yaycioglu R, Onal S 2003 Excision and cryosurgery in the treatment of conjunctival malignant epithelial tumors. Eye 17: 228-232 [ Links ]
25. Rivoire M C, Voiglio E J, Kaemmerlen P, Molina G, Treilleux I, Finzy J, Delay E, Gory F 1996 Hepatic cryosurgery precision: evaluation of ultrasonography, thermometry, and impedancemetry in a pig model. Journal of Surgical Oncology 16: 242-248 [ Links ]
26. Rupp C C, Hoffmann N E, Schmidlin F R, Swanlund D J, Bischof J C, Coad J E 2002 Cryosurgical changes in the porcine kidney: histological analysis with thermal history correlation. Cryobiology 45: 167-182 [ Links ]
27. Samuelson D A 1999 Ophthalmic anatomy. In Gelaat K N Veterinary ophthalmology (3rd edn). Lippincott/Williams & Wilkins, Philadelphia: 37-43 [ Links ]
28. Scot D W, Miller W H, Griffin G E 2001 Neoplastic and non-neoplastic tumors. In Muller and Kirk's small animal dermatology (6th edn). W B Saunders, Philadelphia: 1379-1381 [ Links ]
29. Scot D W, Miller W H, Griffin G E 2001 Structure and function of the skin. In Muller and Kirk's small animal dermatology (6th edn). W B Saunders, Philadelphia: 51-54 [ Links ]
30. Shields J A, Eagle R C, Shields C L, De Potter P, Markowitz G 1993 Apocrine hidrocystoma of the eyelid. Archives of Ophthalmology 111: 866-867 [ Links ]
31. Smith J D, Chernosky M E 1964 Apocrine Hidrocystoma. Archives of Dermatology 109: 700-702 [ Links ]
32. Williams L W, Gelatt K N, Gwin R M 1981 Ophthalmic neoplasms in the cat. Journal of the American Animal Hospital Association 17: 999-1008 [ Links ]
33. Yang ShihHung, Liu ChenHsuan, Hsu ChiaDa, Yeh LihSeng, Lin ChungTien 2007 Use of chemical ablation with trichloroacetic acid to treat eyelid apocrine hidrocystomas in a cat. Journal of the American Veterinary Medical Association 230: 1170-1173 [ Links ]
34. Yanoff M, Fine B S 1996 Skin and lacrimal drainage system. Cysts, pseudoneoplasms, and neoplasms. In Ocular pathology (4th edn). Mosby-Wolfe, London: 180 [ Links ]
Received: November 2009.
Accepted: February 2010.
* Author for correspondence. E-mail: dramilan@gmail.com














