Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
South African Journal of Sports Medicine
On-line version ISSN 2078-516X
Print version ISSN 1015-5163
SA J. Sports Med. vol.30 n.1 Bloemfontein 2018
http://dx.doi.org/10.17159/2078-516x/2018/v30i1a4267
ORIGINAL RESEARCH
The short-term effects of a sport stacking intervention on the cognitive and perceptual motor functioning in geriatrics: a pilot study
R NaidooI; K MoodleyII
IPhD (Sports Science); Discipline of Biokinetics, Exercise and Leisure Sciences, University of KwaZulu-Natal, College of Health Sciences, South Africa
IIM Sports Science; Discipline of Biokinetics, Exercise and Leisure Sciences, University of KwaZulu-Natal, College of Health Sciences, South Africa
ABSTRACT
BACKGROUND: Sport stacking has been found to be beneficial in improving reaction time, as well as hand-eye- coordination, in children.
AIM: The aim of this study was to determine the effects of a sport stacking physical activity intervention on the motor and cognitive functioning of geriatrics.
METHODS: An intact, convenient sample of 58 geriatrics from a retirement home in KwaZulu-Natal, South Africa, was selected to participate in this study. Twenty-eight participants were exposed to an eight-week intervention consisting of 16 physical activity sessions, combined with sport stacking techniques, while the control group (30 participants) continued with activities as usual. All participants performed selected motor and cognitive functioning tests, pre- and postintervention.
RESULTS: The intervention group had greater improvements in mean reaction time and plate tapping (hand-eye coordination) times compared to the control group. There were no changes in the balance test, memory and quality of life tests.
CONCLUSION: A sport stacking activity intervention may improve reaction times and hand-eye coordination in geriatrics.
Keywords: hand-eye coordination, quality of life, reaction time
Sport stacking is defined as an individual or team activity where participants stack and unstack specially designed plastic cups in predetermined sequences while racing against the clock or an opponent.[1] Sport stacking is an activity usually associated with, and performed by, children. It is easy to learn and has the potential to improve hand-eye coordination.[2] It has been claimed that sport stacking allows for an enhancement of motor skills, such as directionality, laterality, perceptual motor functioning, crossing the midline and hand-eye coordination.[1]
Motor skills are subject to accelerated and progressive decline after the age of 60 years.[3-4] Age is a major contributor to lower reaction times affected by decreases in central processing speed, decreases in passive joint flexibility, more caution before responding to certain tasks, and changes in neuromuscular properties.[5] The upper extremities, specifically the hands, play a vital and active role in the activities of daily life. The hands are also subjected to numerous age-related physiological and anatomical changes that can lead to diminished function.[6] Furthermore, the relationship between increased age and reduced hand dexterity has been widely reported in both the clinical and scientific literature.[7]
Together with a decrease in reaction time in hand precision and dexterity, ageing also results in a decrease in muscular strength, which in turn affects proprioception.[8] Balance is dependent on sensory and musculoskeletal systems which are also affected by the ageing process. Geriatrics who have experienced a fall lose confidence in their physical capabilities, which results in them being hesitant to participate in physical activity/exercise.[9]
In addition, as ageing progresses, memory loss, a reduction in learning ability and a decrease in cognitive functioning occurs.[10] Physical inactivity is also associated with an increased risk of cognitive impairment.[11]
It is evident that the process of ageing affects both motor and cognitive skills. Interventions to improve motor and cognitive functioning may be beneficial in improving cognitive functioning and quality of life.[12] However, to the best of these authors' knowledge, there are no interventions that have included a sport stacking component for geriatrics in their protocol.
Hence, the aim of this study was to determine the short-term effects of a sport stacking intervention programme on the motor functioning (hand-eye coordination, reaction time, balance), cognitive functioning (memory) and quality of life in geriatrics.
Methods
Design
This study was an experimental study with a pre- and postintervention assessment. Permission to conduct this study was given by The Association for the Aged in KwaZulu-Natal, South Africa, and ethical clearance from the University of KwaZulu-Natal's Biomedical Research Ethics Committee (BFC 186/15) was also granted.
Participants
This was a convenient sample consisting of 60 geriatrics aged between 60 and 89 years who volunteered to participate in the study. They were recruited from a local retirement home in KwaZulu-Natal. The sample adhered to the following inclusion criteria: no physical disabilities, not diagnosed with Alzheimer's or Parkinson's disease, no sport stacking experience, not on medication for vertigo, no orthopaedic complications, and a sedentary lifestyle.
A call for participants was posted on flyers at the retirement home. The 60 participants who met the inclusion criteria completed informed consent forms and were then randomly assigned into either the intervention (n=30) or control (n=30) group, and were assigned by means of a random participant code. The participants were only informed of their group allocation once the pre-intervention tests were completed. The authors were responsible for the recruitment and group allocation of the participants.
Tests
Pre- and post-intervention test measurements included body mass index (BMI), and motor and cognitive functioning. Motor functioning tests for hand-eye coordination (plate tapping test), reaction time (position speed test), quality of life (Lawton's Instrumental Activities Daily Living Questionnaire), and balance (Sharpened Romberg Test) were administered. The cognitive functioning test for memory utilised the Short Orientation Memory Concentration Test (SOMCT). All tests were conducted three days prior to the start of the intervention and three days post-intervention.
The intervention
The eight-week sport stacking physical activity intervention consisted of two 60 minute weekly sessions. The sessions were conducted as a 25 minute session with a short ten minute break, and then another 25 minute session. The intervention consisted of a multi-stage progression from basic to advanced techniques of sport stacking, as well as progression from slow to fast speeds when performing the techniques. A physical activity component of walking/jogging/running relays was also included. Sport stacking relays were conducted at the end of sessions as a fun element. Relay teams performed a stacking sequence and would then walk/jog/run 10 to 15 m and tag their partner to sport stack, and so on. In addition, participants performed sit-downs, stand-ups and balancing on one foot as part of the relay.
Participants were required to learn three different sport stacking sequences which were the 3-3-3 (Figure 1), 3-6-3 (Figure 2) and the Cycle stack (Figure 3).


The techniques were designed to use both hands. Sport stacking times were measured and recorded for the intervention group per session.
The intervention group participated in the sport stacking physical activity intervention, while the control group remained sedentary and continued with their daily schedules as usual. On completion of the study, the intervention was offered to the control group.
Instrumentation
Body mass index (BMI) was assessed according to the American College of Sports Medicine guidelines.[13] Height and weight were measured by using the Nagata BW-1122H measuring tool. The scale was calibrated before testing. Thereafter, the BMI was calculated for each participant.
Plate tapping test
The plate tapping test assessed the speed and the coordination of limb movement. It utilised a table with adjustable height and a plate tapping board. The plate tapping board was comprised of two green discs of at least 20 cm in diameter and 60 cm apart on a rectangular piece of wood. Participants placed their non-preferred hand between the two green discs, then moved their preferred hand back and forth between the green discs over their hand in the middle as quickly as possible. This timed action was repeated for 25 full cycles (50 taps). The best time of two attempts was recorded.
Position speed test
The position speed test was an online computer-based test that assessed simple reaction time. Participants were required to respond as quickly as possible to an orange square that appeared on a grid table on the screen. Once the participant clicked on the orange square it randomly moved to another block on the grid. The participants had 30 seconds in which to click on as many orange squares as possible to determine the speed of their reactions. They had two attempts at the test and the best score was recorded.
Sharpened Romberg test
Balance and proprioception were assessed using the Sharpened Romberg test. The participants stood in three different positions in sequence: feet together, semi-tandem, and tandem. Each position was held for ten seconds by the participants, with their eyes open and then another ten seconds with their eyes closed. They had three tries to reach the maximum time of 60 seconds. The longest balance time of the three tries was recorded as their score. The semi-tandem and tandem positions were performed in a heel-to-toe standing position with the dominant foot behind the nondominant foot. If the participants moved their feet from this position, opened their eyes during the "closed eyes" phase or reached the maximum test time of 60 seconds, the timer was stopped. Those who successfully completed two out of three tests were scored as "balanced".
Lawton's Instrumental Activities of Daily Living Questionnaire
This was a functional assessment of the participants' independence, which measured functioning at the present time and attempted to determine improvement or deterioration in functioning. It measured the use of a telephone, shopping, food preparation, housekeeping, laundry, mode of transportation, responsibility for medication, and the ability to handle personal finances. The scoring was as follows: one (1) point was given when able to perform the tasks and zero (0) points were given when unable to perform the task. The higher the score, the more capable, and the lower the score, the greater need for dependence on another person. The final score was out of eight.
Short Orientation Memory Concentration Test (SOMCT)
The SOMCT assessed memory, and was comprised of six questions. These questions were such as 'What year is it?', 'About what time is it?', 'Say the months in reverse order' as well as the repetition of phrases. The test used a negative scoring scale. Each question had a maximum number of errors allowed. The scores for each question were added together to give a total error score out of 28. A score of zero to six was within normal limits, while scores of seven and above would indicate a need for further evaluation to rule out a demention disorder, such as Alzheimer's disease.
All tests took approximately an hour per participant and were conducted over two days, pre- and post-intervention. The tests were conducted by trained exercise scientists, and were supervised by the authors/researchers. All tests were standardised and conducted by the same exercise scientist pre-and post-intervention. Exercise scientists were blinded to the group assignment process to ensure the standardisation of the programme. This assisted with programme adherence as participants developed a rapport with the researcher and were motivated and enthusiastic to attend the sport stacking physical activity intervention sessions.
Statistical analysis
All the data collected in this study was subjected to various statistical procedures. All the data were analysed using the Statistical Package for the Social Sciences Version 19. Descriptive (means and standard deviations) and inferential (t-tests, ANCOVA) statistics were used to test significant differences pre- and post-intervention. T-tests were used to test for significant differences across time within groups and ANCOVA was used to test for significant differences over time between groups. The changes in the mean and standard deviations were compared to the pre- and post-test scores for the intervention and control groups respectively. Cohen's d was used to describe the standardised mean difference of an effect. Sport stacking scores were also analysed to determine whether the participants' times decreased (improved) during the intervention. The non-parametric sign test was used to analyse the data from the balance test. Statistical significance was set at p<0.05.
Results
Pre-intervention included a 100% compliance of the 60 participants. However, due to adverse events (the death of two participants), the data presented represents 58 participants (28 in the intervention group; 30 in the control group).
Participants
Ages ranged from 60 to 89 years, with a mean age of 73 years for the sample. The mean age in the intervention group was 73 (±8) years and 73 (±7) years in the control group.
A total of 12 males and 48 females participated in the study. The intervention group was comprised of five males and 23 females while the control group was comprised of seven males and 23 females.
The mean BMI pre-intervention was 28.98kg/m2 and postintervention was 29.00kg/m2.
Motor functioning components
Table 1 shows the pre- and post-test t-test results for the control and intervention groups.
It is evident that there was a significant difference in the plate tapping test and simple reaction time test scores. The intervention group presented with a significant difference in the plate tapping test and the reaction time test. The control group also presented with a significant difference in the plate tapping test and the reaction time test.
Further analysis showed that the effect size for the intervention group's plate tapping analysis (d=0.85) exceeded Cohen's d [14] convention for a large effect (d=0.80), whereas the control group had a trivial change (d=0.14). Similarly, the intervention group's reaction time test analysis (d=0.64) exceeded Cohen's d [14] convention for a moderate effect (d=0.50), whereas the control group change was small (d=0.22).
When ANCOVA was applied, a significant difference in the reaction time test for the two groups after correcting for the pre-reaction measure (F(1,55) = 6.6, p=0.013) was found. The post-intervention reaction test score was significantly higher for the intervention group than for the control group.
For the balance test, a non-parametric sign test was applied to the pairs of measurements to determine if there were significant differences pre- and post-intervention. The Sharpened Romberg test's pre- and post-intervention mean scores were not significant.
Cognitive functioning components
Table 2 depicts the pre- and post-test results for the control and intervention groups. There were no significant differences between the control and intervention groups.
Sport stacking times
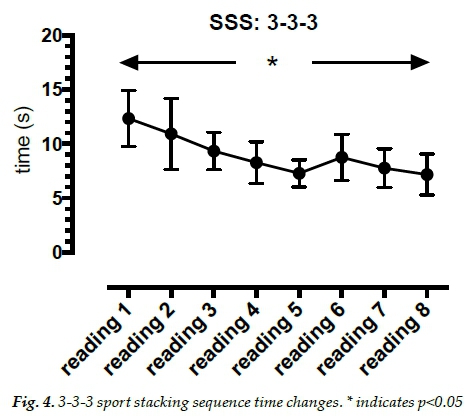
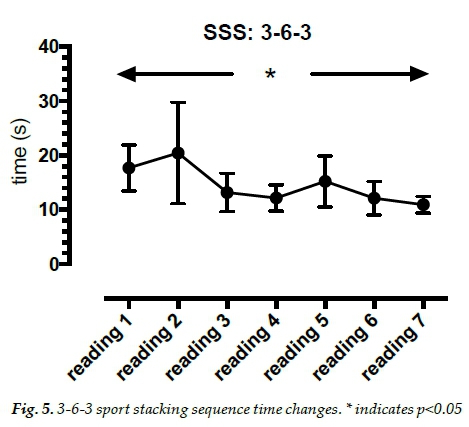
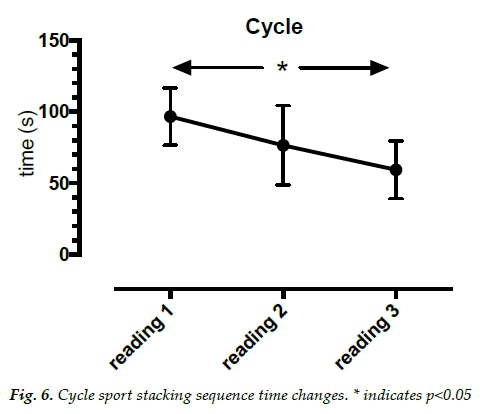
Results indicated improvements in sport stacking times. Average times clearly decreased over time (Figures 4, 5 and 6). There was a significant effect of time on stacking 3-3-3, F(7.42) = 19.2, p<0.0005). There was a significant effect of time on stacking 3-6-3, F(1.43) = 6.1, p=0.029). There was a significant effect of time on stacking the cycle, F(2.14) = 20.0, p<0.0005).
Discussion
This study showed there was a positive effect on the participants' hand-eye coordination and reaction times in both the intervention and control groups. This could be attributed to a learning effect as participants practised sequences and remembered the techniques. Possible reasons for the significant improvements in the control group may be due to participants being motivated to improve their physical activity because of their increased health risks, or as a result of the Hawthorne effect: the alteration of behaviour by the subjects of a study due to their awareness of being observed.[15] However, even though there was a significant improvement in plate tapping in both groups, the effect size in the intervention (d=0.85) group was larger than that of the control group (d=0.15).
Khemthong et al.[16] conducted a study on the effects of musical training on reaction time in elderly individuals and showed that there was almost a 19% increase in visual reaction time. Similarly, in the current study, both the control and intervention groups demonstrated statistically positive increases in reaction time post-intervention. This could be due to both groups now being familiar with the test, although the effect size of the intervention group's improvement (d=0.64) was larger than that found in the control group (d=0.22). Furthermore, the skill of sport stacking also improved significantly improved over time, which could have contributed to the improvements in the intervention group.
The current study did not show an improvement in memory, post-intervention. However, other physical activity intervention studies have been shown to improve memory functioning in geriatrics, specifically when memory loss is detected early, as this may allow for a physical activity intervention to be implemented.[17] Colcombe et al.[18] showed that adults who participated in a regular walking protocol experienced improvements in their cognitive functioning.
A study conducted by Wolf et al.[19] in geriatrics who presented with balance problems found that after a four-to-six-week intervention of 12 individualised balance exercises, significant improvements in balance were noted. However, in the current study, no significant differences in balance were found post-intervention. This could be due to the balance activities having been integrated into the intervention and not been the primary focus of the study and/or individualised.
Visible change, despite the equivocal results, suggests that sport stacking has the potential to improve hand-eye coordination in geriatrics.
It is apparent that studies relating to sport stacking are limited. Additional research needs to be conducted on the cognitive effects of sport stacking, as well as its short- and long-term effects on the geriatric population.
The clinical implications for this study are positive: sport stacking could be a therapeutic option for geriatrics to help promote improvements in hand reaction time and hand-eye coordination.
A long-term sport stacking intervention and larger samples may be needed to ascertain whether it is associated with improvements in both motor and cognitive functioning.
Limitations
There were several limitations in this study. First, there was no random selection, so results are not representative of the geriatric population as a whole. The small sample size influenced the significance of selected results. The study participants were geriatrics from a retirement/old age home and therefore the results are specific to this population and not to geriatrics living in the wider community. Furthermore, the majority of the participants were female (83%).
Conclusion
In conclusion, following 16 physical activity sessions combined with sport stacking techniques, there were improvements in mean reaction time and plate tapping (hand-eye coordination) times. These findings show that a sport stacking activity intervention may improve reaction times and hand-eye coordination in geriatrics.
Acknowledgements: The authors would like to acknowledge and thank the participants at the retirement home who willingly participated in this study.
Conflict of interest: The authors declare no conflict of interest with respect to the authorship and/or publication of this article.
Funding: This study was funded by the College of Health Sciences, University of KwaZulu-Natal.
References
1. Speed Stacks. Sport stacking* with speed stacks: a rationale. https://www.jmu.edu/kinesiology/hpainstitute/documents/SpeedStackingRationale.pdf. Accessed 12 January 2016. [ Links ]
2. Udermann BE, Murray SR, Mayer JM, et al. Influence of cup stacking on hand-eye coordination and reaction time of second-grade students. Percept Mot Skills 2004; 98(2):409-414. [doi: 10.2466/pms.98.2.409-414] [ Links ]
3. Stöckel T, Wunsch K, Hughes CM. Age-related decline in anticipatory motor planning and its relation to cognitive and motor skill proficiency. Front Aging Neurosci 2017; 9:283. [doi: 10.3389/fnagi.2017.00283] [ Links ]
4. Figueiredo PA, Mota MP, Appell HJ, et al. Ceasing of muscle function with aging: is it the consequence of intrinsic muscle degeneration or a secondary effect of neuronal impairments? Eur Rev Aging Phys Act 2006; 3:11. [doi: 10.1007/s11556-006-0011-9] [ Links ]
5. Welford AT. Motor performance. In: J E Birren, KW Schaic (Eds). Handbook of the psychology of aging. 2nd ed. New York: Van Nostrand Reinhold, 1977:450-496. [ Links ]
6. Carmeli E, Patish H, Coleman R. The aging hand. J Gerontol A Biol Sci Med Sci 2003; 58(2): M146-M152. [doi:10.1093/gerona/58.2.M146] [ Links ]
7. Martin JA, Ramsay J. Hughes C. et al. Age and grip strength predict hand dexterity in adults. PLoS One 2015, 10(2), e0117598. [doi: 10.1371/journal.pone.0117598]. [ Links ]
8. Hurley MV, Rees J, Newham DJ. Quadriceps function, proprioceptive acuity and functional performance in healthy young, middle-aged and elderly subjects. Age Ageing 1998; 27(1):55-62. [doi: 10.1093/ageing/27.1.55] [ Links ]
9. Matsumura BA, Ambrose AF. Balance in the elderly. Clin Geriatr Med 2006; 22(2):395-412. [doi: 10.1016/j.cger.2005.12.007] [ Links ]
10. Pang FC, Chow TW, Cummings JL, et al. Effect of neuropsychiatric symptoms of Alzheimer's disease on Chinese and American caregivers. Int J Geriatr Psychiatry 2002; 17(1):29-34. [doi:10.1002/gps.510] [ Links ]
11. Cotman CW, Berchtold NC. Exercise: a behavioral intervention to enhance brain health and plasticity. Trends Neurosci 2002; 25(6): 295-301. [doi:10.1016/s0166-2236(02)02143-4] [ Links ]
12. Sayer AA, Robinson SM, Patel HP, et al. New horizons in the pathogenesis, diagnosis and management of sarcopenia. Age Ageing 2013; 42(2):145-150. [doi: 10.1093/ageing/afs191] [ Links ]
13. Pescatello, Linda S. ACSM's Guidelines for Exercise Testing and Prescription. Philadelphia: Wolters Kluwer/Lippincott Williams & Wilkins Health, 2014: 63-64 [ Links ]
14. Cohen, J. Statistical power analysis for the behavioral sciences. 2nd ed. New Jersey: L Eribaum, 1988: 2-27. [ Links ]
15. Waters L, Reeves M, Fjeldsoe B, et al. Control group improvements in physical activity intervention trials and possible explanatory factors: a systematic review. J Phys Act Health 2012; 9 (6): 884-895. [ Links ]
16. Khemthong S, Pejarasangharn U, Uptampohtiwat T, et al. Effect of musical training on reaction time: A randomized control trial in Thai elderly individuals. Music Med 2012; 4(1):16-21. [doi: 10.1177/1943862111427567] [ Links ]
17. Cockburn J, Collin C. Measuring everyday memory in elderly people: a preliminary study. Age Ageing1988; 17(4):265-269. [doi:10.1093/ageing/17.4.265] [ Links ]
18. Colcombe SJ, Kramer AF, Erickson, KI, et al. Cardiovascular fitness, cortical plasticity, and aging. Proc Natl Acad Sci U S A 2004; 101(9):3316-3321. [doi: 10.1073/pnas.0400266101] [ Links ]
19. Wolf B, Feys H, De Weerdt W, et al. Effect of a physical therapeutic intervention for balance problems in the elderly: a single-blind, randomized, controlled multicenter trial. Clin Rehabil 2001; 15(6):624-636. [doi: 10.1191/0269215501cr456oa] [ Links ]
 Correspondence:
Correspondence:
R Naidoo
naidoor3@ukzn.ac.za














