Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.112 n.10 Pretoria Oct. 2022
http://dx.doi.org/10.7196/SAMJ.2022.v112i11.16614
RESEARCH
Heterologous vaccination of BNT162b2 in Ad26. COV2.S-vaccinated healthcare workers elicits long-term humoral immune response
B JacobsonI, II; A KhanI; A H ShulmanI; B SegalI; E MayneIII, IV; L-G BekkerV; I SanneVI; G GrayVII
IMMed (Haem), PhD; Department of Molecular Medicine and Haematology, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
IMSc, PhD; Department of Molecular Medicine and Haematology, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
IBSc Hons (Physio); Department of Molecular Medicine and Haematology, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
IMSc; Department of Molecular Medicine and Haematology, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
IIMMed (Haem), PhD; Department of Medicine and National Health Laboratory Service, Charlotte Maxeke Johannesburg Academic Hospital, Johannesburg, South Africa
IIIMB BCh, MMed (Haem); Clinical Laboratory Services, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
IVMB BCh, MMed (Haem); Division of Immunology, Faculty of Health Sciences, University of Cape Town, South Africa
VFCP (SA), PhD; Desmond Tutu HIV Centre, Institute of Infectious Disease and Molecular Medicine, Faculty of Health Sciences, University of Cape Town, South Africa
VIDTM&H, FCP (SA); Clinical HIV Research Unit, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg
VIIFC Paed (SA), DSc; South African Medical Research Council, Cape Town, South Africa
ABSTRACT
BACKGROUND: To date, there are no immunological data for the SARS-CoV-2 heterologous vaccination schedule in the South African (SA) population
OBJECTIVES: To assess and compare the immunogenicity and reactogenicity of the Jansen Ad26.COV2.S vaccine with the Pfizer/BioNTech-BNT162b2 booster following prime Ad26.COV2.S in 65 SA healthcare workers
METHODS: In a prospective, quantitative, cross-sectional trial on individuals >18 years of age vaccinated with a single Ad26.COV2.S dose or single Ad26.COV2.S and a BNT162b2 single-dose/both doses booster, participants filled in a questionnaire on their demographics, type of vaccination, breakthrough infection/s (BTI/s), vaccine reactogenicity, prior SARS-CoV-2 infection and dates of vaccination. Qualitative analysis for presence/absence of anti-S (spike) immunoglobulin G (IgG) was performed using the Euroimmun anti-IgG enzyme-linked immunoassay kit, and anti-S IgG titres were quantitatively assessed using the Abbott IgG Quant II kit
RESULTS: Between 28 October 2021 and 30 November 2021, 65 individuals were enrolled and assigned as either prime Ad26.COV2.S (n=18) or Ad26.COV2.S with a BNT162b2 supplement (n=47) at Charlotte Maxeke Johannesburg Academic Hospital, SA (mean age 45 years (95% confidence interval (CI) 29.5 - 58), 42 women (64.6%) and 23 men (35.4%)). The median IgG titre for the primed Ad26.COV2.S group was 4 272.55 (95% CI 68.40 - 10 351.40) and that for the BNT162b2 supplement group was 7 360.80 (95% CI 4 207.40 - 15 372.60). In the univariate model, the BNT162b2 supplement group showed a significant 1.99 times higher antibody titre factor (95% CI 0.045 -5.553; p<0.005) than the Ad26.COV2.S group. In both univariate and multivariate models, age, time since prime vaccination, BTI and prior infection failed to show any statistically significant association (p>0.05) with antibody titres in both groups. However, sex (-55.381 (95% CI -76.984 - -13.498; p=0.018) in a multivariate model was found to have a statistically significant association with anti-S IgG titres observed in both groups. Participants who received their first dose of BNT162b2 9-10 months after their prime Ad26.COV2.S (n=44) had a higher degree of antibody response than those who received it earlier. Reactogenicity was observed to be manageable, with mild/moderate adverse effects in the study population
CONCLUSION: A BNT162b2 supplement given in single or two doses as booster in individuals primed with Ad26.COV2.S induced immunological response, with acceptable and manageable reactogenicity. This study provides novel evidence of the highest degree of antibody response in individuals who received a BNT162b2 first dose 9-10 months after prime Ad26.COV2.S, implying that a longer time gap between the two vaccines stimulates higher antibody response than a shorter gap, and that this antibody response can persist for as long as 6 months after the last BNT162b2 dose
On 31 December 2019, the World Health Organization (WHO) China country office was informed of an outbreak of pneumonia with unknown aetiology in a cluster of patients linked to a seafood market in Wuhan City, Hubei Province. The causative agent, isolated by Chinese authorities on 7 January 2020, was identified as a new type of the Coronavirus (nCoV) severe acute respiratory syndrome Coronavirus 2 (SARS-CoV-2) causing the clinical syndrome Coronavirus disease 2019 (COVID-19). As of 4 May 2022, SARS-CoV-2 had infected >512 million individuals and caused >6.24 million deaths worldwide, according to the WHO Health Emergency Dashboard.
SARS-CoV-2 is a single-stranded RNA virus that encodes for four structural proteins (spike surface glycoprotein (S), small envelope protein (E), matrix protein (M) and nucleocapsid protein (N)), 15 non-structural proteins and 8 accessory proteins.[1] SARS-CoV-2 binds to the epithelial angiotensin-converting enzyme 2 receptor through the receptor-binding domain (RBD) of the spike antigen (SI), facilitating viral entry and early infection in the nasopharynx.[2,3] This domain is the major antigenic target of vaccines aiming to elicit neutralising antibody responses.[4]
As geographical separation of different SARS-CoV-2 viruses tends to result in genetically distinct variants, the emergence of 'variants of concern with multiple mutations in S-glycoprotein alpha (B.l.1.7; 7 substitutions), beta (B.1.351; 9 substitutions), gamma (P.l; 12 substitutions), delta (B.l.617.1, B.l.617.2, B.l.617.3; 17 substitutions)'51 and omicron (B.l.1.529, BA.2 lineage; 36 substitutions)'6,71 has increased the risk of reinfection or resistance to vaccine-elicited antibodies as they are produced against native S-glycoprotein. Vaccine development, focusing on mRNA and adenoviral vector technology, has been rapid.[8] The phase 1 clinical trial of the Moderna mRNA-1273 vaccine started shortly after release of the genetic sequence of nCoV from Chinese researchers. In South Africa (SA), a phase 3 clinical trial of single-dose Jansen Ad.26.COV2.S (called the Sisonke study), involving a national phase I vaccine roll-out in healthcare workers (HCWs), started on 17 February 2021, while a second roll-out (elderly>60 years) with two-dose Pfizer-BioNTech BNT162b2 vaccine started on 17 May In SA, 477 234 HCWs received their first Ad26.COV2.S dose in the Sisonke study as a priority access.[9]
As evidence suggests that Ad26.COV2.S works best as a two-dose vaccine, the HCWs were due to get their booster dose from November 2021 in SA. Because of the uncertainty about the lasting duration of immunity and the possible risk of breakthrough infection (BTI) as new variants emerge, some HCWs elected to receive one or both doses of BNT162b2 to boost anti-COVID-19 immunity before the booster dose of Ad26.COV2.S.
As these individuals were not eligible for the Sisonke booster study (VAC31518COV3012- exclusion criteria), it was important to ascertain their antibody titres and side-effects profile. Furthermore, the effect of such heterologous vaccination remained undetermined In this qualitative (and quantitative), cross-sectional, prospective study, we therefore evaluated antibody titres after booster BNT162b2 dose/s in 47 HCWs already vaccinated with Ad.26.COV.S as a single dose, and compared them with 17 HCWs who had not yet received any booster.
Methods
Ethical considerations
This study received approval from the Human Research Ethics Committee of the University of the Witwatersrand (ref. no. M210992).
Study population
The study population comprised voluntary participants aged >18 years who were invited to participate in the COVintegra study (M210992). They were informed about the research and its purpose and were invited to sign the informed consent. The identity and results of each volunteer were anonymised, and signed informed participant consent was obtained. Participants were requested to complete a questionnaire on their age, sex, previous COVID-19 infection, first (Sisonke) vaccination, any observed adverse event after vaccination, any BTI (if observed), date of first/both dose/s of vaccination with BNT162b2, and any adverse events post BNT162b2. Peripheral blood samples were collected by a qualified phlebotomist at their closest laboratory (Ampath, Lancet or National Health Laboratory Service) in a serum separator tube.
Sample preparation
Samples were transported within 8 hours of collection to a tertiary accredited laboratory for processing at room temperature. All serum tubes were centrifuged for 15 minutes at 3 500 rpm. Serum was separated and samples were stored in 200 μl aliquots at -80°C for batch analysis. Freeze-thaw cycles were limited to one. Once thawed, samples were immediately processed for the qualitative and quantitative immunoglobulin G (IgG) assays.
Serology (qualitative and quantitative IgG assays)
The samples were first evaluated for the presence/absence of the IgG antibodies against SARS-CoV-2 using a commercial anti-IgG enzyme-linked immunosorbent assay (ELISA) (Euroimmun, Germany). This assay has been extensively validated in SA.[10] Samples were diluted in sample buffer and then samples, controls and calibrators were transferred to an ELISA plate precoated with recombinant SARS-CoV-2 spike antigen. Following a 60-minute incubation at 37°C, wells were washed with 450 μL of wash buffer and 100 uL of peroxidase-conjugated anti-human immunoglobulin was added, followed by chromogenic substrate (100 μL), after which a stop solution was added. Sample plates were read using a commercial reader (Euroimmun, Germany) at a wavelength of 450 nm within 30 minutes. Results were interpreted as a ratio of the extinction of sample or control to the extinction of the calibrator as negative (<0.8), indeterminate (0.8 - 1) or positive (>1). All the samples were seropositive (optical density (OD) ratio >1) and were further evaluated for antibody titre determination.
Serum anti-S (spike) IgG antibody levels (titres) were determined with a chemiluminescent microparticle immunoassay using the SARS-CoV-2 IgG II Quant assay kit (Abbott Laboratories, Germany), according to the manufacturer's instructions. The manufacturer recommended the assay to be used for monitoring antibody response in individuals who have received the COVID-19 vaccine, by quantitatively measuring the IgG antibodies against the spike RBD of SARS-CoV-2. The anti-S IgG titres were estimated by running the samples on the Abbott Alinity system (Abbott Laboratories, Germany). Seropositivity was defined as >50 arbitrary units/mL.
Sample size calculations
All sample size estimates were performed for a significance level of 0.05 and a statistical power of 80%. Estimates were produced using the pwr package in R (R Core Team, Austria).[11] No estimates exist for an expected difference in IgG values between vaccine variants, and standard effect sizes were therefore employed from Cohen.[12] A large effect estimate was employed given empirical evidence of a reduced rate of BTIs. The sample size estimate, for multiple linear regression using five degrees of freedom (namely age, sex, dosing interval, BTI history and vaccine type) with an estimated large effect size (f2 = 0.35), was 42 participants. Type of vaccine received was the main predictor, and the other factors were confounders/controls.
Statistical methods
All statistical analyses were performed within the R programming environment.[13] Cohort descriptions and statistical comparisons between variants were produced with the Tableone package.[14] Continuous variables were compared using non-parametric tests based on the observed distribution of recorded values or if the underlying distribution was known not to conform to a Gaussian distribution. All tests were performed as two-sided with an alpha value of 0.05 used as the significance threshold. Modelling proceeded in two phases: the first considering univariate estimates for each recorded variable, and the second using a composite multivariable model using prespecified predictors without variable selection. All variables were retained in multivariable modelling that were evaluated in the univariate configuration. Linear modelling employing a logarithmic transformation was applied to the IgG values to improve the extent to which the collected data conformed to a Gaussian distribution given the strictly positive and right-skewed nature of the raw values. These results provide a multiplicative estimate of the effect of each variable on IgG results. We replicated the analysis with logistic regression for the binary case of predicting a history of BTIs following vaccination. Similarly, we employed the prespecified list of predictors without selection.
Results
A total of 67 participants were recruited during the study period (28 October 2021 -30 November 2021 ), 2 of whom were subsequently excluded from statistical analysis (one had a negative OD result and the other could not provide the exact date of the Pfizer booster). The overall characteristics of this cohort with regard to demographics, prior COVID-19 infection, vaccine history, BTIs and anti-S IgG antibody titres are summarised in Table 1. A prior infection was defined as a confirmed case of COVID-19 either before vaccination or as a BTI after vaccination. Seven individuals (10.4%) had BTIs following their prime Ad.26.COV2.S dose, while 16 (24.6%) had SARS-CoV-2 infection prior to the vaccination.
Patients were classified into two groups, Ad26.COV2.S and Ad26. COV2.S + BNT162b2 (heterologous vaccination group), according to the type of vaccine they received. The heterologous vaccination group Ad26.COV2.S + BNT162b2 had 47 individuals recruited while 17 individuals were sourced with a single (prime) Ad26. COV2.S inoculation and 1 individual was given a booster dose of Ad26.COV2.S. All the study participants tested seropositive in both qualitative and quantitative estimations. Anti-S IgG antibody titres in the single participant with an Ad26.COV2.S booster were not significantly different those in participants who had received single-dose Ad26.COV2.S, so this special case was not studied separately and was registered in the single prime Ad26.COV2.S dose group (n=17 +1 = 18) for all statistical analyses. Surprisingly, individuals receiving either single or both doses of BNT162b2 post Ad26.COV2.S did not have any significant difference in anti-S IgG titres, and both single- and two-dose BNT162b2 recipients were therefore categorised in the heterologous vaccination group. The group that received heterologous vaccination were significantly older (p<0.001) than those with single Ad26.COV2.S vaccination, and had their single Ad26.COV2.S dose at a significantly earlier time (p<0.001) (Table 1).
The two groups did not differ significantly in the rate of prior COVID-19 infections (p=0.491). The anti-S IgG antibody titre value was significantly higher in the heterologous vaccination group (Ad26. COV2.S + BNT162b2) compared with the single-dose Ad26.COV2.S group, but this did not cross the threshold for statistical significance without consideration of potential confounders (p=0.055) (Table 1). Despite the marked difference in anti-S IgG antibody titre value, the overall positivity rate did not vary significantly between the groups (p=0.629).
The temporal nature of the anti-S IgG titres and the time that had elapsed since receiving each vaccination type recorded for each patient are shown in Fig. 1. For patients who were time-matched in having received their initial Ad26.COV2.S dose 10 months previously (300 days), the heterologous vaccination (Ad26.COV2.S + BNT162b2) recipients (with very few outliers) had very high anti-S IgG titres, evidence of a stronger immune response.
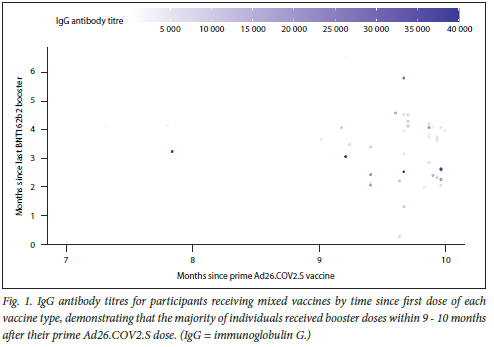
Individuals who received a prime dose of Ad26.COV2.S received booster BNT162b2 dose/s within the first 5-6 months (n=l), 7 - 8 months (n=3) (Fig. 1) and 9 - 10 months (n=44) (Fig. 1) after the prime dose. This is the most important finding of the study - that participants who received their first dose of BNT162b2, 9-10 months after the prime Ad26.COV2.S dose (n=44) had the highest degree of antibody response, implying that a longer time gap between the heterologous vaccination stimulates higher antibody response than a shorter gap, and that this antibody response persists for as long as 6 months after the last BNT162b2dose.
The heterologous vaccination (Ad26. COV2.S + BNT162b2) group showed a median increase in anti-S IgG antibody titre of 1.99 (95% confidence interval (CI) 0.045 -5.153; p=0.003) when compared with Ad26. COV2.S vaccination in a univariate model (Table 2). The type of vaccine received provided a relatively large, positive estimate of an increase in titre values by 199.52% (95% CI 45.79 - 515.34) after receiving a supplement vaccine over a single Ad26. COV2.S dose (p=0.003) when considered in isolation. The multivariable model had similar results to the univariate set, with the vaccine type received remaining a significant predictor of IgG titre (p=0.007) with an even larger estimate of a 281% (95% CI 46.67 -888.48) increase in IgG titre results. Model estimates for age and sex fluctuated between univariate and multivariable models, with male sex resulting in an estimated 55.38% (95% CI 13.50 - 76.98) decrease in IgG titre under the multivariable modelling configuration. The confidence intervals for age remained broad, however, with poor prediction of quantitative titre results. With the width of the associated 95% CI, in the univariate models, the vaccine type received demonstrated significant estimates (Table 2).
Despite the estimated 1.99 (95% CI 0.045 - 5.153) increase in anti-S IgG titre with heterologous vaccine administration, the risk of contracting BTI still persists, so the likelihood of contracting BTI needed to be analysed. A generalised linear model performing logistic regression analysis on the likelihood of contacting BTI was performed, and the odds ratios for both univariate and multivariable models for the BTI risk assessment post vaccination are summarised in Table 3. Overall, among all other predictors including age, sex, prior infection and the time since prime inoculation, the only significant predictor for BTI risk remained vaccination group. An individual receiving a heterologous vaccine (Ad26.COV2.S + BNT162b2) had a 99.98% (95% CI 99.63 - 99.9; p=0.017) lower odds of sustaining a BTI compared with an individual receiving only a single Ad26. COV2.S dose, implying that administering vaccine doses prevents incidents of BTI.
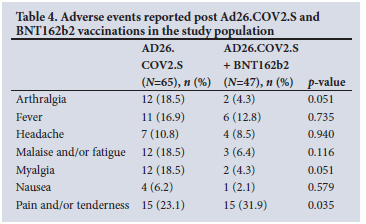
For reactogenicity of each type of vaccination, rates of patient-reported outcomes were grouped by type of vaccine. This resulted in a substantial increase in the number of single Ad26.COV2.S outcome reports, as all individuals from the heterologous vaccination (Ad26.COV2.S + BNT162b2) group had still received a primary dose. The comparison between the two vaccine sets is shown in Table 4. Overall, the BNT162b2 booster did not demonstrate substantial changes in side-effect profile apart from a substantial reduction in post-vaccine arthralgia (p=0.035).
Discussion
The first cases of COVID-19 in SA were described in March 2020 in tourists returning from Europe. Despite a State of Disaster that was declared in March 2020 and a strict lockdown, SA continues to be one of the most severely affected countries in the world, with 3 802 198 laboratory-confirmed cases of COVID-19 as of 4 May 2022 and 100 377 SARS-CoV-2-attributable deaths as per the WHO Health Emergency Dashboard.
Outcome data from the Sisonke study in HCWs in SA showed Ad26.COV2.S to be effective, safe and easily accessible. However, to date there are no data on efficacy of the heterologous vaccine schedule in SA, although reports on different heterologous combinations of COVID-19 vaccines in other populations exist. A combination of Pfizer (BNT162b2) with prime AztraZeneca (ChAdOxl-S) results in a superior immunogenic response with higher SARS-CoV-2 anti-S IgG concentrations than a homologous ChAdOxl-S vaccine schedule. [15,16]It is also evident that for all mix-and-match combinations of Pfizer, Jansen and Moderna COVID-19 vaccines, neutralising antibody titres against a SARS-CoV-2 pseudovirus increase by a factor of 4 to 73, with homologous boosters increasing titres by a factor of 4 to 20 in a US population, whereas heterologous boosters increased titres by a factor of 6 to 73.[17] Administering a single- or double-dose Pfizerbooster post Ad26.COV2.S single dose elicited a stronger humoral response (anti-S IgG titre) and generated stronger cellular immunity compared with the homologous Ad26.COV2.S prime boost vaccination in Singapore.[18]
The present study compared the antibody response (anti-S IgG titre levels) in individuals who received a single dose of Ad.26.COV2.S vaccine with those who received a prime Ad.26.COV2.S and BNT162b2 booster. The study also examined the effect of vaccine selection on the post-vaccination ramification of BTI. Study estimates were produced with controls for participants' age, sex, time since prime vaccine dose, and time since BNT162b2 supplement.
Patient demographic factors, including age, were found to be a significant predictor of IgG titre in the study population. A similar observation has been recorded with a heterologous combination of BNT162b2 and ChAdOxl-S (AstraZeneca) over a full dose of ChAdOxl-S alone.[19] It is possible that demographic factors may predict a different immunological response for different heterologous vaccine combinations. With BNT162b2 and ChAdOxl-S, male sex has shown to be associated with lower anti-S IgG titres compared with females.[19] However, we found male sex to be an insignificant predictor of lower IgG titres. Demographic factor prediction for a variable depends on underlying immunological and comorbidity differences and differences in follow-up interval in the study populations. These underlying immunological and comorbidity differences were not directly observed as part of the present data collection.
BTIs are considered to be one of the factors discouraging homologous booster or heterologous vaccinations in the vaccine-hesitant population, and SA has one of the world's highest proportions of vaccine-hesitant individuals. Our results indicated that the baseline difference in the time interval since receiving the primary Ad26.COV2.S dose (p<0.001) does not significantly predict the risk of BTI (p=0.173), and/or anti-S IgG antibody titre (p=0.470). This is a novel finding, as current studies looking at 'mRNA booster vaccines' typically have a maximum follow-up timeline of 12 - 14 weeks post booster and therefore reflect a short window into the ramifications of time on vaccine effectiveness. The combination of a prime Ad26.COV2.S dose with a first or both BNT162b2 booster dose/s produces a significantly elevated anti-S IgG antibody titre by a factor of 1.99 (95% CI 0.045 - 5.553) compared with a single Ad26.COV2.S dose. Furthermore, elevated antibody response induced by heterologous vaccination protects against the estimated odds of BTI compared with single-agent vaccination (p=0.022). Similar findings have been reported with heterologous vaccination.[20]
In addition, the present study is the first to report the importance of having a longer gap between the two vaccines to elicit a potent and a long-lasting immune response post heterologous vaccination involving Ad26. COV2.S prime and BNT162b2 booster. In response to SARS-CoV-2 exposure, host IgM antibodies are produced first, followed by isotype switching to IgG against N and S proteins; of these, antibodies against the N protein wane over time, while those against S protein persist.[21] However, in the case of COVID-19 vaccines, first exposure of S antigen (Ad26.COV2.S prime dose) results in production of IgG and IgM, after which memory T and B cells are created and stored. In the second exposure of S antigen (BNT162b2 first and second booster dose), a low IgA and IgM and a robust IgG are likely to result in strong immune response. [22] With regard to our findings, it is unclear how this robust response lasted for so long, and whether secretory immunoglobulin A (SIgA) also played a part in this persistent immunity post heterologous Ad26.COV2.S and BNT162b2 vaccination. However, SIgA in the mucus, breastmilk and saliva has been shown to neutralise SARS-CoV-2 in multiple studies,[23] and interestingly has been shown to be important for vaccine efficacy[24]
Heterologous vaccination with BNT162b2 booster and Ad26.COV2.S prime did not show marked reactogenicity in the vaccine recipients (Table 4). Mild pain and tenderness at the injection site were reported by only 20% of the total study population after the first vaccination event of Ad26.COV2.S prime dose (Table 4). However, after the second vaccination event (BNT162b2 firstor second booster), >35% of the study population reported a heavy arm, pain and/or tenderness. Mild manageable nausea, myalgia, malaise, malaise and fatigue, headache, fever and arthralgia were reported in <25% of the study population after the first vaccination event. After the second vaccination event, very few recipients (<15%) reported these side-effects (Table 4). The heterologous administration of BNT162b2 booster after an Ad26.COV2.S prime dose showed a manageable, mild to moderate reactogenic profile in the present study population.
Study limitations
Study limitations are the small cohort size (N=65), and lack of testing for cellular immunity and neutralising antibody. While cumulative reports agree with considering IgG response as a correlate of disease protection,[26] cellular immunity (particularly T cells) has also been documented to mediate vaccine protection against SARS-CoV-2.[27]
Conclusion
Heterologous vaccination using BNTl62b2 supplement in single or two doses in individuals primed with Ad26.COV2.S has an acceptable and manageable reactogenicity profile and induces stronger immunological response compared with the response induced by single-dose Ad26.COV2.S. This study provides novel evidence of the highest degree of antibody response in individuals who received the BNTl62b2 first dose 9-10 months after prime Ad26.COV2.S, suggesting that a longer gap between the two vaccines stimulates higher antibody response than a shorter gap, and that this antibody response persists for 6 months after the last BNTl62b2 dose.
Declaration. None.
Acknowledgements. None.
Author contributions. BJ conceptualised the study with GG, L-GB and IS. EM provided the serology testing. AK designed the study obtained ethical approval, collected the demographic data on the heterologous-vaccinated group and wrote the manuscript. BS performed statistical analysis. AHS obtained demographic data on the prime Ad26.COV2.S-vaccinated group.
Funding. None.
Conflicts of interest. None.
References
1. Kim D, Lee JY, Yang JS, Kim JW, Kim VN, Chang H. The architecture of SARS-CoV-2 transcriptome. Cell 2020;181(4):914-921.el0. https://doi.org/10.1016/j.cell.2020.04.011 [ Links ]
2. Monteil V, Kwon H, Prado P, et al. Inhibition of SARS-CoV-2 infections in engineered human tissues using clinical-grade soluble human ACE2. Cell 2020;181(4):905-913.e7. https://doi.Org/10.1016/j.cell.2020.04.004 [ Links ]
3. Mercurio I, Tragni V, Busto F, de Grassi A, Pierri CL. Protein structure analysis of the interactions between SARS-CoV-2 spike protein and the human ACE2 receptor. From conformational changes to novel neutralizing antibodies. Cell Mol Life Sci 2021;78(4):1501-1522. https://doi.org/10.1007/s00018-020-03580-1 [ Links ]
4. Changrob S, Fu Y, Guthmilier JJ, Halfmann PJ, et al. Cross-neutralisation of emerging SARS-CoV-2 variants of concern by antibodies targeting distinct epitopes on spike. mBio 2021;12(6):e0297521. https://doi.org/10.1128/mBio.02975-21 [ Links ]
5. Mohammadi M, Shayestehpour M, Mirzaei H. The impact of spike mutated variants of SARS-CoV2 Alpha, Beta, Gamma, Delta, and Lambda] on the efficacy of subunit recombinant vaccines. Braz j Infect Dis 2021;25(4):101606. https://doi.org/10.1016/j.bjid.2021.101606 [ Links ]
6. McCormick KD, Jacobs JL, Meliors JW. The emerging plasticity of SARS-CoV-2. Science 2021;371(6536):1306-1308. https://doi.org/10.1126/science.abg4493 [ Links ]
7. COG-UK. COG-UK report on SARS-CoV-2 spike mutations of interest in the UK. 15 January 2021. https://www.cogconsortium.uk/wp-content/up loads/2021/01/Report-2_COG-UK_S ARS-CoV-2-Mutations.pdf (accessed 28 February 2022). [ Links ]
8. Bali P. The lightning-fast quest for COVID vaccines - and what it means for other diseases. Nature 2021;589(7840):16-18. https://doi.org/10.1038/d41586-020-03626-l [ Links ]
9. Sadoff J, Gray G, Vandebosch A, et al. ENSEMBLE Study Group. Safety and efficacy of single-dose Ad26.COV2.S vaccine against Covid-19. N Engl J Med 2021;384(23):2187-2201. https://doi.org/10.1056/NEJMoa2101544 [ Links ]
10. Gededzha MP, Mampeule N, Jugwanth S, et al. Performance of the EUROIMMUN Anti-SARS-CoV-2 ELISA Assay for detection of IgA and IgG antibodies in South Africa. PLoS ONE 2021;16(6):e0252317. https://doi.org/10.1371/journal.pone.0252317 [ Links ]
11. Champely S. Pwr. Basic functions for power analysis, 2020. https://CRAN.R-project.org/package=pwr (accessed 3 March 2022). [ Links ]
12. Cohen J. Statistical Power Analysis for the Behavioral Sciences. 2nd ed. Hillsdale, NJ. L Erlbaum Associates, 1988. [ Links ]
13. R Core Team. R. A Language and Environment for Statistical Computing. Vienna, Austria. R Foundation for Statistical Computing, 2021. https://www.R-project.org/ (accessed 3 March 2022). [ Links ]
14. Yoshida K, Alexander B. Tableone. Create 'Table V to describe baseline characteristics with or without propensity score weights. 2021. https://CRAN.R-project.org/package=tableone (accessed 3 March 2022). [ Links ]
15. Liu X, Shaw RH, Stuart ASV,et al.,Com-COV Study Group. Safety and immunogenicity of heterologous versus homologous prime-boost schedules with an adenoviral vectored and mRNA COVID-19 vaccine (Com-COV). A single-blind, randomised, non-inferiority trial. Lancet 2021;398(10303):856869. https://doi.org/10.1016/S0140-6736(21)01694-9 [ Links ]
16. Chiu NC, Chi H, Tu YK, et aL To mix or not to mix? A rapid systematic review of heterologous prime-boost covid-19 vaccination. Expert Rev Vaccines 2021;20(10):1211-1220. https://doi.org/10.1080/14760584.2021.1971522 [ Links ]
17. Atmar RL, Lyke KE, Deming ME, et al., DMID 21-0012 Study Group. Homologous and heterologous Covid-19 booster vaccinations. N Engl J Med 2022;386(11):1046-1057. https://doi.org/10.1056/NEJMoa2116414 [ Links ]
18. Khoo NKH, Lim JME, Gill US, et al. Differential immunogenicity of homologous versus heterologous boost in Ad26.COV2.S vaccine recipients. Med (NY) 2022;3(2):104-118.e4. https://doi.org/10.1016/j.medj.2021.12.004 [ Links ]
19. Borobia AM, Carcas AJ, Perez-Olmeda M, et al., CombiVacS Study Group. Immunogenicity and reactogenicity of BNT162b2 booster in ChAdOxl-S-primed participants (CombiVacS). A multicentre, apen-label, randomised, controlled, phase 2 trial. Lancet 2021;398(10295):121-130. https://doi.org/10.1016/S0140-6736(21)01420-3 (erratum in. Lancet 2021;398(10300):582). [ Links ]
20. Lopez Bernal J, Andrews N, Gower C, et al. Effectiveness of Covid-19 vaccines against the B.1.617.2 (delta) variant. N Engl J Med 2021;385(7):585-594. https://doi.org/10.1056/NEJMoa2108891 [ Links ]
21. Fenwick C, Croxatto A, Coste AT, et al. Changes in SARS-CoV-2 spike versus nude op rotein antibody responses impact the estimates of infections in population-based seroprevalence studies. J ViroJ 2021;95(3):e01828-20. https://doi.org/10.1128/JVI.01828-20 [ Links ]
22. Wheeler SE, Shurin GV, Yost M, et al. Differential antibody response to mRNA COVID-19 vaccines in healthy subjects. Microbiol Spectr 2021;9(l):e0034121. https://doi.org/10.1128/Spectrum.00341-21 [ Links ]
23. Tsukinoki K, Yamamoto T, Handa K, et al. Detection of cross-reactive immunoglobulin A against the severe acute respiratory syndrome-coronavirus-2 spike 1 subunit in saliva. PLoS ONE 2021;16(11):e0249979. https://doi.org/0.1371/journal.pone.0249979 [ Links ]
24. Zurac S, Nichita L, Mateescu B, et al. COVID-19 vaccination and IgG and IgA antibody dynamics in health care workers. Mol Med Rep 2021;24(2):578. https://doi.org/10.3892/mmr.2021.12217 [ Links ]
25. Wisnewski AV, Campillo Luna J, Redlich CA. Human IgG and IgA responses to COVID-19 mRNA vaccines. PLoS ONE 2021;16(6):e0249499. https://doi.org/10.1371/journal.pone.0249499 [ Links ]
26. Harvey RA, Rassen JA, Kabelac CA, et al. Association of SARS-CoV-2 seropositive antibody test with risk of future infection. JAMA Intern Med 2021;181(5):672-679. https://doi.org/10.1001/jamainternmed.2021.0366 [ Links ]
27. Sahin U, Muik A, Derhovanessian E, et al. COVID-19 vaccine BNT162bl elicits human antibody and TH1 T cell responses. Nature 2020;586(7830):594-599. https://doi.org/10.1038/s41586-020-2814-7(erratum in. Nature 2021;590(7844):E17). [ Links ]
 Correspondence:
Correspondence:
A Khan
amberbiosc@gmail.com
Accepted 12 August 2022














