Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.112 no.4 Pretoria abr. 2022
http://dx.doi.org/10.7196/samj.2022.v112i4.16077
RESEARCH
Percutaneous left atrial appendage occlusion: A South African experience
A P DippenaarI; J A SaaimanI; P A BrinkII, III; M J HeradienII, III; P van der BijlIV
IMB ChB, MMed (Int Med); SAEndovascular, Kuils River Netcare Hospital, Kuils River, Cape Town, South Africa
IIMMed (Int Med), PhD; SAEndovascular, Kuils River Netcare Hospital, Kuils River, Cape Town, South Africa
IIIMMed (Int Med), PhD; Department of Medicine, Faculty of Medicine and Health Sciences, Stellenbosch University, Cape Town, South Africa
IVMMed (Int Med), PhD; SAEndovascular, Kuils River Netcare Hospital, Kuils River, Cape Town, South Africa
ABSTRACT
BACKGROUND: Atrial fibrillation (AF) is associated with all-cause mortality, heart failure and non-fatal stroke, and thromboprophylaxis is traditionally provided with oral anticoagulants (OACs). Percutaneous left atrial appendage occlusion (LAAO) with a dedicated device is an alternative approach to thromboprophylaxis in patients with AF who are: (i) intolerant to OACs (e.g. life-threatening haemorrhage); (ii) non-adherent to OACs; or (iii) at a high bleeding risk with OACs. Non-inferiority of LAAO compared with OACs was demonstrated in e.g. the WATCHMAN Left Atrial Appendage System for Embolic Protection in Patients With Atrial Fibrillation (PROTECT AF) trial. Only very limited data are available on percutaneous LAAO in South Africa (SA), and no local outcome data have been reported
OBJECTIVES: To compare the safety and efficacy outcomes of an SA percutaneous LAAO programme with larger international series
METHODS: All patients undergoing percutaneous LAAO from 2013 to 2020 at a single centre (SAEndovascular, Kuils River Netcare Hospital, SA) were included from an ongoing registry. Survival analysis was performed with the Kaplan-Meier method
RESULTS: Of 101 LAAO recipients (mean (standard deviation) age 77 (10) years, 64% male) analysed, 90 (90%) had permanent AF, 1 (1%) persistent AF and 9 (9%) paroxysmal AF. The most common indication for LAAO was previous severe bleeding (n=23; 23%). The mean device size was 23 (3) mm and the procedural success rate was 98%. After a median (interquartile range) follow-up of 21 (5 - 41) months, 6 patients (6%) experienced stroke or all-cause mortality. Four patients (4%) had a life-threatening procedural complication (tamponade n=2 (2%) and device embolisation n=2 (2%)). These outcomes are comparable to large international series, e.g. PROTECT AF
CONCLUSIONS: The safety and efficacy outcomes of an SA percutaneous LAAO programme were comparable to large international series. A successful percutaneous LAAO programme is feasible in a southern African context
Atrial fibrillation (AF) is a major global health challenge, with an estimated prevalence in the general population of 1 - 2%.[1] It becomes more common with age, and affects up to 15% of octogenarians.[1,2] AF has been shown to be independently associated with all-cause mortality, heart failure and non-fatal stroke.[1,3]
Oral anticoagulants (OACs) have traditionally been used for the prevention of stroke, but many AF patients are intolerant to OACs, non-adherent, or at an unacceptably high bleeding risk when taking OACs.[4] Percutaneous left atrial appendage occlusion (LAAO) with a dedicated device is an alternative approach to thromboprophylaxis in such individuals.[2] Percutaneous LAAO has been shown to be non-inferior compared with OACs for stroke prevention in large clinical trials, e.g. the WATCHMAN Left Atrial Appendage System for Embolic Protection in Patients With Atrial Fibrillation (PROTECT AF).[2] Only very limited data are available on percutaneous LAAO in South Africa (SA), and no local outcome data have been reported. We therefore compared the safety and efficacy outcomes of an SA percutaneous LAAO programme with larger international series.
Methods
Study population and data collection
All adult patients (>18 years) who underwent percutaneous LAAO from 2013 to 2020 at a single centre (SAEndovascular, Kuils River Netcare Hospital, Cape Town) were included from an ongoing clinical registry. Patients with incomplete clinical data were excluded. Written informed consent was obtained pre-procedure for all patients undergoing LAAO. Patients were followed up for the primary endpoint of all-cause mortality and stroke. Survival data were collected from medical chart review and telephonic follow-up. All data used in the current study were collected for routine clinical purposes and handled anonymously. The study protocol was approved by the Health Research Ethics Committee, Faculty of Medicine and Health Sciences, Stellenbosch University (ref. no. N20/11/119) and the Netcare Research Operations Committee (ref no. TRIAL-2021-0050).
Percutaneous LAAO insertion technique
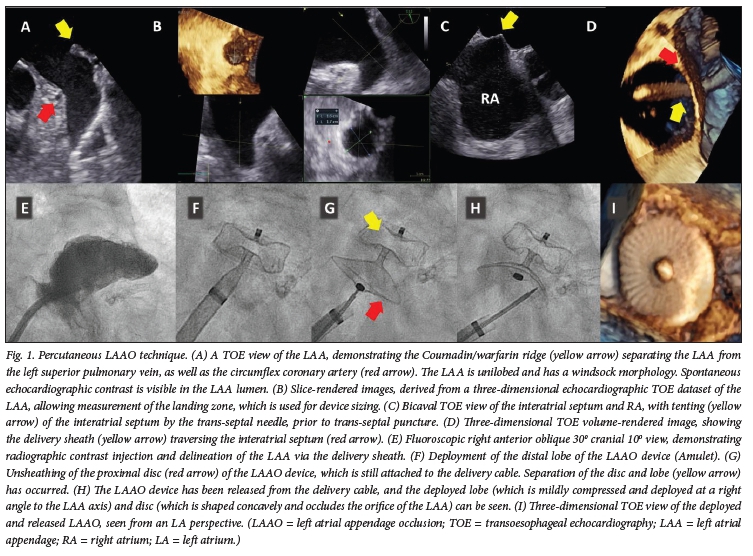
All LAAO procedures were performed under transoesophageal echocardiography (TOE) guidance. Trans-septal puncture was performed via right femoral venous access, and the sheath and dilator were advanced into the superior vena cava before being exchanged for a trans-septal needle. The interatrial septum was punctured under TOE guidance, whereafter a stiff 0.035-inch guidewire was advanced into the left atrial appendage (LAA) under TOE guidance, facilitated by low-volume radiographic contrast (Iomeron; Bracco, Italy) injections. Systemic anticoagulation was achieved with intravenous heparin administration after successful trans-septal puncture. The trans-septal sheath was subsequently exchanged for a 14F TorqueVue 45 x 45 delivery sheath (Abbot Vascular, USA), which was advanced into the LAA. The appendage was delineated with a contrast injection and measured fluoroscopically. Amplatzer or Amulet (Boston Scientific/ Abbot Vascular, USA) LAAO devices were deployed via the delivery sheath under fluoroscopic and TOE guidance. After ensuring correct placement of the LAAO with a tug test, fluoroscopic confirmation of mild lobe compression, separation of the lobe and disc, and a concave shape of the disc, deployment of the lobe at a right angle to the LAA axis was performed. Finally, major peri-device leaks were excluded with TOE before the device was released and the delivery cable and sheath retracted from the left atrium (LA) (Fig. 1).
Statistical analysis
Normality was assessed by visual comparison of data histograms with a normal probability curve, as well as Q-Q plots and detrended normal Q-Q plots. Continuous data are presented as means and standard deviations (SDs) when normally distributed, and as medians and interquartile ranges (IQRs) when not normally distributed. Categorical data are expressed as frequencies and percentages. Survival analysis was performed with the Kaplan-Meier method. All tests were two-sided and a p-value <0.05 was considered statistically significant. Analyses were performed with SPSS for Windows version 25.0 (IBM Corp., USA) and GraphPad Prism 9 (GraphPad Software, USA).
Results
Baseline patient characteristics and indication for LAAO
A total of 101 LAAO recipients (mean (SD) age 77 (10) years, 64% male) were analysed. The baseline characteristics of the study population are summarised in Table 1. Underlying vascular risk factors were common, and almost two-thirds of the patients had comorbid coronary artery disease. The most common type of AF was permanent, followed by paroxysmal and, lastly, persistent.
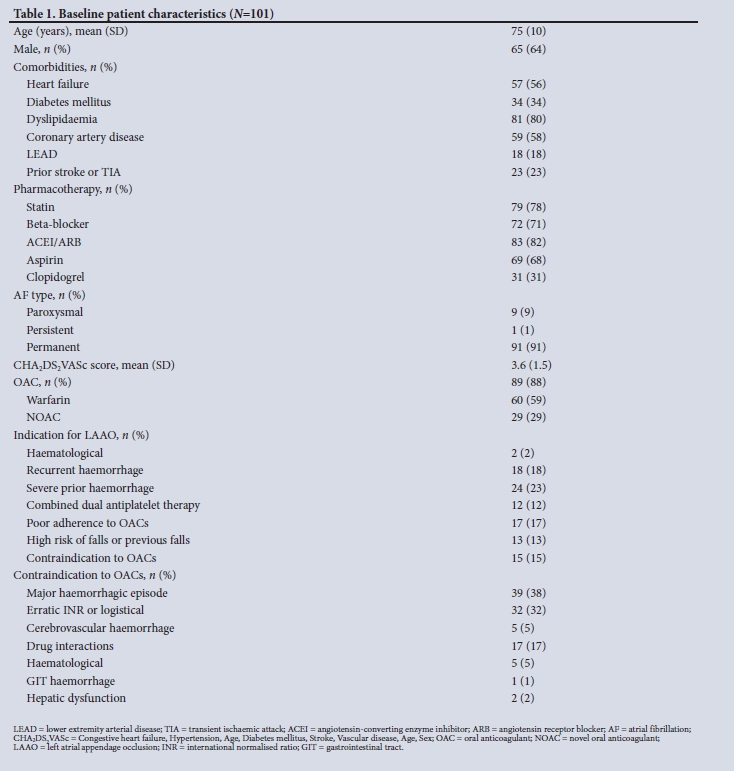

Severe prior haemorrhage was the most common indication for LAAO, and a major haemorrhagic episode was the most frequent contraindication to OACs.
Procedural aspects of LAAO
The mean (SD) device size was 23 (3) mm and the procedural success rate was 98%. The mean fluoroscopy time was 31 (24) minutes, and the mean total procedural dose area product was 122.8 (116.2) Gy.cm2. Four patients (4%) had a life-threatening procedural complication: tamponade n=2 (2%) and device embolisation n=2 (2%). The mean time to hospital discharge was 2.8 (5.4) days.
Long-term outcome after LAAO
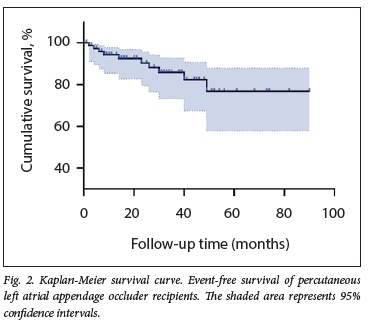
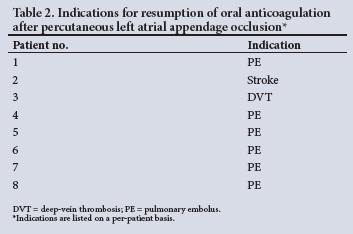
After a median (IQR) follow-up of 21 (5 - 41) months, 6 patients (6%) experienced stroke or all-cause mortality. The cumulative event rate for stroke or all-cause mortality was 0%, 2% and 7% at 20, 40 and 60 months' follow-up, respectively (Fig. 2). Eight patients (8%) resumed OACs after LAAO. A breakdown of the reasons is provided in Table 2, from which it can be seen that the majority were not related to failure of LAAO.
Discussion
AF and stroke prevention: Balancing risks and benefits
Patients with AF are at increased risk of systemic thromboembolism, particularly ischaemic stroke. The incidence of stroke in patients with non-valvular AF is -5% per year, and 25% of ischaemic strokes may be ascribed to cardiac embolism due to underlying AF[5] Moreover AF-related strokes are associated with higher mortality and morbidity than non-AF strokes, emphasising the need for more effective stroke prevention in these individuals.[6]
Traditionally, anticoagulation with vitamin K antagonists (VKAs), e.g. warfarin, is employed to reduce the thromboembolic risk in AF[4] A meta-analysis of five randomised clinical trials has shown that oral anticoagulation (OAC) results in a relative risk reduction of 68% (95% confidence interval (CI) 50 - 79%; p<0.001) for ischaemic stroke.[7] Novel oral anticoagulants (NOACs), however, are currently recommended in preference to VKAs, except in the presence of moderate to severe mitral stenosis or a mechanical heart valve.[1,3] NOACs include dabigatran, rivaroxaban, apixaban and edoxaban (the last currently unavailable in SA). Recent randomised trials have furnished evidence that not only are NOACs non-inferior or superior to VKAs for the prevention of ischaemic stroke, but they also demonstrate a decreased risk of cerebrovascular haemorrhage among AF patients with a moderate to high stroke risk. In contrast to VKAs, NOACs have the advantage of not requiring therapeutic drug monitoring.[8] VKAs and NOACs are indicated for the prevention of thromboembolism in AF in the presence of a CHA2DS2VASc (Congestive heart failure, Hypertension, Age, Diabetes mellitus, Stroke, Vascular disease, Age, Sex) score >1 - 2.[1,3,9]
The major unwanted effect of OAC (using VKAs or NOACs) is bleeding. Various factors have to be taken into consideration when deciding on the risk-benefit ratio of initiating OAC in a patient with AF. The HAS-BLED (Hypertension, Abnormal liver and renal function, Stroke, Bleeding, Labile international normalised ratio (INR), Elderly, Drugs or alcohol) score was developed to assess the 1-year risk of major haemorrhage in patients receiving OAC for
thromboprophylaxis in AF.[10] A HAS-BLED score of >3 maybe used to identify individuals at high risk of bleeding.[9] In addition, previous or current life-threatening haemorrhage or a patient s perceived frailty and a high risk of traumatic falls should be taken into consideration when deciding to initiate OAC.[11-13] Furthermore, the effective use of OAC (VKAs or NOACs) is dependent on patient adherence.
AF thromboprophylaxis: The role of the LAA and LAAO
The pathogenesis of thrombus formation in non-valvular AF is multifactorial, and still not fully understood. It is increasingly being recognised that, in addition to LA stasis secondary to the arrhythmia itself, a procoagulant state exists that contributes to thrombus formation in AF.[14] Underlying this prothrombotic milieu are endothelial and/or endocardial dysfunction, altered haemostasis, platelet dysfunction and dysregulation of fibrinolysis. Inflammation of both the LA and the pericardial adipose tissue, as well as LA fibrosis, are also implicated in the pathogenesis of AF and thrombus formation.[15] The LAA is the only region within the LA composed of pectinate muscles and is a low-flow zone, making it particularly prone to stasis of blood and thrombus formation.
LAAO in AF is predicated on the fact that only a small percentage (<10%) of clinically relevant emboli in non-valvular AF originate outside the LAA.[5,16-18] After excluding the LAA as an embolic source, additional thromboprophylaxis with a VKA or NOAC can be avoided in patients who are intolerant to these medications or nonadherent, or have a high bleeding risk.[3] LAA occlusion techniques have evolved from being primarily surgical to being percutaneous. Originally, surgical ligation of the LAA at the time of mitral valve or coronary artery bypass surgery was shown to reduce the incidence of cardioembolic events in patients with AF.[17,19] Percutaneous LAAO was developed as a less invasive alternative, and the PLAATO (Appriva Medical, USA) device represented the first iteration of percutaneous LAAO.[18] This was followed by several others, most notably the WATCHMAN device (Boston Scientific, USA), the Amplatzer Cardiac Plug (Boston Scientific, USA) and the Amulet device (Abbot Vascular, USA).
The PROTECT AF trial was a prospective study that randomised 70 patients with non-valvular AF and a CHADS, score (precursor of the CHA,DS,VASc score) >1 to either LAAO with the WATCHMAN device or warfarin in a 2:1 fashion.[2] The mean (SD) age of the intervention group was 72 (9) years, and 70% of patients were male;[2] 17% of participants in the intervention group had had a previous stroke or transient ischaemic attack (TIA).[2] Baseline characteristics were therefore comparable to our cohort. Patients were followed up for the primary composite endpoint of stroke, cardiovascular or unexplained death or systemic embolism.[2] After 24 months of follow-up, the cumulative event rate (which served as the basis for the definition of the primary endpoint in our study) was 5.9% (95% CI 3.1 - 8.8) for the LAAO arm, compared with 8.3% (95% CI 4.0 - 12.5) for the control group, which is almost identical to our results.[2] After 24 months, the composite safety endpoint (excessive bleeding, e.g. intracranial or gastrointestinal, or procedure-related complications, e.g. serious pericardial effusion, device embolisation or procedure-related stroke) was 10.2% (95% CI 7.4 - 13.0), which is higher than that of our patient cohort.[2]
Although the Evaluation of the WATCHMAN LAA Closure Device in Patients With Atrial Fibrillation Versus Long Term Warfarin Therapy (PREVAIL) trial, following the original PROTECT AF protocol, failed to demonstrate non-inferiority of LAAO to warfarin using an identical endpoint, a significantly lower adverse event rate was recorded for LAAO recipients.[20] More recently the Interventional Left Atrial Appendage Closure vs. Novel Anticoagulation Agents in High-risk Patients With Atrial Fibrillation (PRAGUE-17) study performed a head-to-head comparison between NOACs and LAAO, demonstrating non-inferiority (subdistribution hazard ratio (sHR) 0.84; 95% CI 0.53 - 1.31; p=0.44; p=0.004 for non-inferiority).[21,22] There were no between-group differences for the following endpoints: stroke/TIA (sHR 1.00; 95% CI 0.40 -2.51; p=0.99), clinically significant bleeding (sHR 0.81; 95% CI 0.44 - 1.52; p=0.51) and cardiovascular death (sHR 0.75; 95% CI 0.34 - 1.62; p=0.46).[21,22] On the basis of current evidence, the European Society of Cardiologys AF guideline provides a class lib recommendation to LAAO for 'stroke prevention in patients with AF and contraindications for long-term anticoagulant therapy (e.g. intracranial bleeding without a reversible cause)'.[1]
LAAO in SA
VKAs remain the primary mode of AF thromboprophylaxis in SA patients. In the Atrial fibrillation Clopidogrel Trial with Irbesartan for prevention of Vascular Events (ACTIVE W), however, INRs were in the therapeutic range only 40% of the time for SA participants.[23] LAAO is therefore a viable and attractive alternative to OAC but is being performed in only a few centres in SA. As far as the authors are aware, only a single case series of percutaneous LAAO has been published from SA, and no outcome data were reported.[24] The establishment of a multicentre registry may be of value to both clinicians and funders.
We have demonstrated that a successful LAAO programme can be established locally, with outcome data that are comparable to large international series, e.g. PROTECT AF. We advocate for the appropriate and timely referral of AF patients who are intolerant or non-adherent to OACs, or who have an unacceptably high bleeding risk, so that LAAO can be considered as an alternative prophylactic strategy. Potential obstacles to this approach are: (i) the dedicated training that is required for both peri-procedural imaging and performance of LAAO itself; (ii) lack of awareness of the availability of LAAO and established referral pathways; (iii) the perception of high cost of LAAO; and (iv) the limited number of local centres currently offering percutaneous LAAO.
Study limitations
This was a single-centre, retrospective analysis, and may have been subject to selection bias. Clinical events were adjudicated locally and not by a central committee. Systematic follow-up with TOE was not performed at regular time intervals for all patients, and therefore the incidence of peri-device leak could not be reported on. Mortality data are available for all-cause mortality only, and sub-analyses for cardiac and non-cardiac mortality could not be performed. The number of patients receiving a NOAC was too small to perform a sub-analysis comparing them with warfarin.
Conclusions
The safety and efficacy outcomes of an SA percutaneous LAAO programme were comparable to large international series. A successful percutaneous LAAO programme is feasible in an SA setting.
Declaration. None.
Acknowledgements. None.
Author contributions. APD: conception and design of the study; collection, analysis and interpretation of data; drafting of the manuscript; final approval of the manuscript. JAS: conception and design of the study; revision of the manuscript; final approval of the manuscript. PAB: conception and design of the study; revision of the manuscript; final approval of the manuscript. MJH: conception and design of the study; revision of the manuscript; final approval of the manuscript. PvdB: conception and design of the study; collection, analysis and interpretation of data; drafting of the manuscript; final approval of the manuscript.
Funding. None.
Conflicts of interest. MJH received financial support from Medtronic and is a Hamilton Naki scholar. The remaining authors have nothing to disclose.
References
1. Hindricks G, Potpara T, Dagres N, et al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J 2021;42(5):373-498. https://doi.org/10.1093/eurheartj/ehaa612 [ Links ]
2. Holmes DR, Reddy VY, TuriZG,et al. Percutaneous closure of the left atrial appendage versus warfarin therapy for prevention of stroke in patients with atrial fibrillation. A randomised non-inferiority trial Lancet 2009;374(9689):534-542. https://doi.org/10.1016/S0140-6736(09)61343-X [ Links ]
3. Correction to. 2019 AHA/ACC/HRS Focused Update of the 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation. A Report of the American College of Cardiology/ American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society Circulation 2019;140(6). https://doi.org/10.1161/cir.0000000000000719 [ Links ]
4. Go AS, Hylek EM, Borowsky LH, et al. Warfarin use among ambulatory patients with nonvalvular atrial fibrillation. The AnTicoagulation and Risk Factors in Atrial Fibrillation (ATRIA) study Ann Intern Med 1999;131(12):927-934. https://doi.org/10.7326/0003-4819-131-12-199912210-00004 [ Links ]
5. Baman JR Mansour M, Heist EK, Huang DT, Biton Y. Percutaneous left atrial appendage occlusion in the prevention of stroke in atrial fibrillation. A systematic review Heart Fail Rev 2018;23(2):191-208. https://doi.org/10.1007/s10741-018-9681-4 [ Links ]
6. Lin HJ, Wolf PA, Kelly-Hayes M, et al. Stroke severity in atrial fibrillation. The Framingham Study Stroke 1996;27(10):1760-1764. https://doi.org/10.1161/01.str.27.10.1760 [ Links ]
7. Risk factors for stroke and efficacy of antithrombotic therapy in atrial fibrillation. Analysis of pooled data from five randomized controlled trials. Arch Intern Med 1994;154(13):1449-1457. https://doi.org/10.1001/archinte.l994.00420130036007 [ Links ]
8. Patel MR Mahaffey KW, Garg J, et al. Rivaroxaban versus warfarin in nonvalvular atrial fibrillation N Engl J Med 2011;365(10):883-891. https://doi.org/10.1056/NEJMoal009638 [ Links ]
9. Lane DA, Lip GY. Use of the CHA2DS2-VASc and HAS-BLED scores to aid decision making for thromboprophylaxis in nonvalvular atrial fibrillation. Circulation 2012;126(7):860-865. https://doi.org/10.1161/CIRCULATIONAHA.111.060061 [ Links ]
10. Pisters R Lane DA, Nieuwlaat R, et al. A novel user-friendly score (HAS-BLED) to assess 1-year risk of major bleeding in patients with atrial fibrillation. The Euro Heart Survey Chest 2010;138(5):10931100. https://doi.org/10.1378/chest.10-0134 [ Links ]
11. Ahr O, Doshi S, Kar S, et al. Quality of life assessment in the randomised PROTECT AF (Percutaneous Closure of the Left Atrial Appendage Versus Warfarin Therapy for Prevention of Stroke in Patients With Atrial Fibrillation) trial of patients at risk for stroke with nonvalvular atrial fibrillation. J Am Coll Cardiol 2013;61(17):1790-1798. https://doi.org/10.1016/j.jacc.2013.01.061 [ Links ]
12. Bungard TJ, Ghali WA, Teo KK, McAlister FA, Tsuyuki RT. Why do patients with atrial fibrillation not receive warfarin? Arch Intern Med 2000;160(1):41-46. https://doi.org/10.1001/archinte.l60.1.41 [ Links ]
13. Hylek EM, Evans-Molina C, Shea C, Henault LE, Regan S. Major hemorrhage and tolerability of warfarin in the first year of therapy among elderly patients with atrial fibrillation. Circulation 2007;115(21):2689-2696. https://doi.org/10.1161/circulationaha.l06.653048 [ Links ]
14. Meus R, Son M, Sobczyk D, Undas A. Prothrombotic state in patients with a left atrial appendage thrombus of unknown origin and cerebrovascular events. Stroke 2016;47(7):1872-1878. https://doi.org/10.1161/STROKEAHA.116.012856 [ Links ]
15. Boldt A, Wetzel U, Lauschke J, et al. Fibrosis in left atrial tissue of patients with atrial fibrillation with and without underlying mitral valve disease. Heart 2004;90(4):400-405. https://doi.org/10.1136/hrt.2003.015347 [ Links ]
16. Ohtsuka T, Ninomiya M, Nonaka T, et al. Thoracoscope stand-alone left atrial appendectomy for thromboembolism prevention in nonvalvular atrial fibrillation. J Am Coll Cardiol 2013;62(2):103-107. https://doi.org/10.1016/j.jacc.2013.01.017 [ Links ]
17. Yao X, Gersh BJ, Holmes DR Jr, et al. Association of surgical left atrial appendage occlusion with subsequent stroke and mortality among patients undergoing cardiac surgery. JAMA 2018,319(20):2116-2126. https://doi.org/10.1001/jama.2018.6024 [ Links ]
18. Sievert H, Lesh MD, Trepéis T, et al. Percutaneous left atrial appendage transcatheter occlusion to prevent stroke in high-risk patients with atrial fibrillation. Circulation 2002;105(16):1887-1889. https://doi.org/10.1161/01.cir.0000015698.54752.6d [ Links ]
19. Melduni RM, Schaff HV, Lee HC, et al. Impact of left atrial appendage closure during cardiac surgery on the occurrence of early postoperative atrial fibrillation, stroke, and mortality. A propensity score-matched analysis of 10 633 patients. Circulation 2017;135(4):366-378. https://doi.org/10.1161/CIRCULATIONAHA.116.021952 [ Links ]
20. Holmes DR Jr, Kar S, Price MJ, et al. Prospective randomised evaluation of the Watchman Left Atrial Appendage Closure device in patients with atrial fibrillation versus long-term warfarin therapy. The PREVAIL triai J Am Coll Cardiol 2014;64(1):1-12. https://doi.org/10.1016/j.jacc2014.04.029 [ Links ]
21. Osmancik P, Herman D, Neuzil P, et al. Left atrial appendage closure versus direct oral anticoagulants in high-risk patients with atrial fibrillation. J Am Coll Cardiol 2020;75(25):3122-3135. https://doi.org/10.1016/j.jacc.2020.04.067 [ Links ]
22. Osmancik P, Tousek P, Herman D, et al. Interventional left atrial appendage closure vs novel anticoagulation agents in patients with atrial fibrillation indicated for long-term anticoagulation (PRAGUE-17 study). Am Heart J 2017;183:108-114. https://doi.org/10.1016/j.ahj.2016.10.003 [ Links ]
23. Aalbers J. South Africa's poor warfarin control raises questions of benefit above other anticoagulant therapies in atrial fibrillation. Cardiovasc J Afr 2011;22(4):220. [ Links ]
24. Abelson M. Left atrial appendage closure in patients with atrial fibrillation in whom warfarin is contra-indicated. Initial South African experience. Cardiovasc J Afr 2013;24(4):107-109. https://doi.org/10.5830/CVJA-2013-018 [ Links ]
 Correspondence:
Correspondence:
A P Dippenaar
dradippenaar@gmail.com
Accepted 21 December 2021














