Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.104 n.11 Pretoria Nov. 2014
EDITOR'S CHOICE
Immunology underlies most of the biological and clinical disciplines in medicine. This includes autoimmune diseases, infectious diseases and HIV, primary immunodeficiency, cancer and transplantation medicine. Indeed, the formalised use of immunology knowledge, laboratory techniques and targeted immunotherapies in routine clinical practice is now commonplace in much of the world. It is the most rapidly advancing field, and generalists need to keep up with advances in knowledge that impact on patient management. This is the impetus behind this month's CME, entitled 'Updates in immunology and allergy'. The medical community, both clinical and pathology disciplines, can no longer afford to see immunology as a 'black box' discipline irrelevant to day-to-day patient management or only applicable to the uncommon case of immunodeficiency or autoimmune disease. For South African (SA) doctors this means considering immunology beyond HIV medicine. Is it time for immunology in SA, amid competing public health needs, to be established as a distinct specialty or sub-specialty? This issue of CME provides an overview and an update on clinical immunology that will be indispensable to all practitioners.
'… may we live in a world without lawyers and court cases' (Confucius)
A year ago, I wrote an editorial1 lamenting the current SA penchant for suing health practitioners, sometimes clearly justified and warranted, but often as a means to easy enrichment. I predicted that patients would be the losers.2 This issue of SAMJ carries much that confirms this sentiment.
Howarth et al.3 ask whether the public is unknowingly sleep-walking into a dystopian future. In the face of escalating costs of liability cover for specialists offering obstetric and neonatal care, spinal surgery and neurosurgery, they predict fewer doctors in these high-risk fields, with those remaining practising defensive medicine; an absence or severe curtailing of private specialist obstetric care; paediatricians and ophthalmologists reluctant to manage neonates; and fewer neurosurgeons in private practice, all restricted to the larger urban areas. Patients would have to be treated in already busy state facilities and would have to compete for resources. Any medicolegal liabilities would move across to the state sector hospitals and staff.
As Howarth et al. emphatically state, the medical profession cannot be expected to resolve the situation, as there is no medical answer. Rather, private patients, private providers, public patients, public providers, politicians and policy pundits all have a vested interest in resolving the problem - the issue has to enter the public debate.
Smith et al.4 point out that the annual premium for neurosurgeons in 2013 was R250 900, second only to that of obstetricians (R254 230), this rise having paralleled the increase in the number and amount of awards in malpractice litigation. (SA's highest-ever medical damages settlement of R25 million was awarded in June 2013, to a patient who had undergone neurosurgery). Neurosurgeons are indicating that they would not have chosen the specialty had they envisaged the current medical liability situation. A third of their number have discontinued performing high-risk procedures because of the associated liability risk.
Walters5 suggests mediation as an alternative to litigation in medical malpractice, and states the obvious -thathealthcare would be much better off if the money spent on the legal process were rather channelled into the healthcare system itself.This realisation has led to pursuit of alternative dispute resolution through arbitration or mediation.Walters believes thatmediation is perhaps the most effective, since the majority of complaints against healthcare workers or institutions arise out of miscommunication. Such issues are ideal for the mediation process, involving the two parties, complainant and respondent, communicating through a facilitator. The complainant or aggrieved party defines and addresses his or her complaint to the respondent; the respondent then has the opportunity to explain the events that led to the complaint or grievance. A trained mediator guides both parties to a point of mutual agreement or acceptance.
Looking at the implications of Venter v Roche Products (Pty) Limited and Others for research ethics committees, Strode and Singh6 addresswhat type of compensation research participants would be entitled to in a clinical trial when they have signed an informed consent document excluding certain forms of compensation. In this recent case, the court considered whether the plaintiff was entitled to claim for non-medical costs (pain and suffering, loss of income and general damages). His application for damages was dismissed because he had voluntarily agreed to the limited compensation as set out in the informed consent form, which had been approved by both the local research ethics committees and the Medicines Control Council.
The article warns that research ethics committees have the obligation both to ensure that compensation clauses in informed-consent documents are carefully reviewed and that these are made clear to potential research participants.
Asking 'Who will guard the guards?', Parrish and Blockman7 aim to raise awareness of conflict of interest (COI) issues, including some tactics used by the pharmaceutical industry to influence thought leaders. COI exists when professional judgement in a primary interest is unduly influenced by a secondary interest and fosters a conflict in loyalties that translates into a biased decision, with the potential for harm. A good practical example is that, in the wake of reports regarding the risk of myocardial infarction in diabetics treated with rosiglitazone, authors who had favourable views on the safety of rosiglitazone were three times more likely to have a financial conflict of interest with a pharmaceutical company than were authors who had unfavourable views.8
The Ebola epidemic rages on …
As the Ebola epidemic rages,9 , 10 clinicians should ask every febrile patient: 'Which African country(ies) have you recently visited?' We are also reminded that the occupational risk of infection by blood-borne viruses (BBVs) in healthcare practitioners (HCPs) and students is significant, especially in the developing world.11 Three viral pathogens are known to pose the most serious risk: HIV, hepatitis B virus (HBV) and hepatitis C virus (HCV). The route of transmission can be percutaneous or mucosal, and is related to the work environment and practices of HCPs. Not only are HCPs at risk of acquiring these infections, but they also pose a risk to patients once infected. Rossouw et al. 11offer these recommendations: all HCPs and all healthcare students should know their infection and immune status (as appropriate) for all three major BBVs, and all who are not infected with HBV should be vaccinated and have their immune status confirmed prior to initiation of training.
Appropriateness of CT and MRI scans
Computed tomography (CT) and magnetic resonance imaging (MRI) are now an essential part of modern healthcare, enabling the practitioner to make non-invasive diagnoses. Imaging is one of the fastest-growing services in medicine, amounting to $100 000 billion annually in the USA. The clinical information obtained, and their increased accessibility, has made these modalities attractive to both patients and referring physicians. However, marked increases in imaging utilisation are now straining healthcare expenditure and threatening health system sustainability. Becker et al.[12] question the appropriateness of CT and MRI scans in the Eden and Central Karoo districts of the Western Cape. The increased utilisation of diagnostic imaging (see Fig. 2 of the article, reproduced below) has brought with it significant economic risks, plus medical risks through increased radiation exposure, with its accompanying carcinogenic potential, and the unforeseen gadoliniumrelated nephrogenic systemic fibrosis, over and above the well-known mild allergies and anaphylactoid responses.
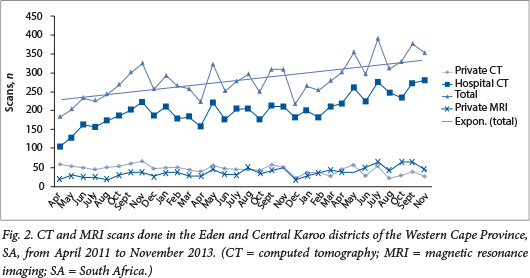
The recommendation is that consultants be required to grant permission for CT or MRI, as at George Hospital, but with awareness of the American College of Radiologists Appropriateness Criteria and and the Royal College of Radiology Guidelines.
REFERENCES
1. Seggie J. The 'boom' in medical malpractice claims - patients could be the losers. S Afr Med J 2013;103(7):433. [http://dx.doi.org/10.7196/SAMJ.7127] [ Links ]
2. Malherbe J. Counting the cost: The consequences of increased medical malpractice litigation in South Africa. S Afr Med J 2013;103(2):83-84. [http://dx.doi.org/10.7196/SAMJ.6457] [ Links ]
3. Howarth GR, Goolab B, Dunn RN, Fieggen AG. Public somnambulism: Public lack of awareness of the consequences of increasing medical negligence litigation. S Afr Med J 2014;104(11):752-753. [http://dx.doi.org/10.7196/SAMJ.8568] [ Links ]
4. Roytowski D, Smith T, Fieggen AG, Taylor A. Impressions of defensive medical practice and medical litigation among South African neurosurgeons. S Afr Med J 2014;104(11):736-738. [http://dx.doi.org/10.7196/SAMJ.8336] [ Links ]
5. Walters J. Mediation - an alternative to litigation in medical malpractice. S Afr Med J 2014;104(11):717-718. [http://dx.doi.org/10.7196/SAMJ.8851] [ Links ]
6. Strode A, Singh PP. Compensation for research-related harm: The implications of Venter v Roche Products (Pty) Limited and Others for research ethics committees. S Afr Med J 2014;104(11):759-761. [http://dx.doi.org/10.7196/SAMJ.8596] [ Links ]
7. Parrish A, Blockman M. Who will guard the guards? Medical leadership and conflict of interest in South African healthcare. S Afr Med J 2014;104(11):757-758. [http://dx.doi.org/10.7196/SAMJ.8546] [ Links ]
8. Wang AT, McCoy CP, Murad MH, Montori VM. Association between industry affiliation and position on cardiovascular risk with rosiglitazone: Cross sectional systematic review. BMJ 2010;340:c1344. [http://dx.doi.org/10.1136/bmj.c1344] [ Links ]
9. Bateman C. Ebola global response: 'not in my back yard'. S Afr Med J 2014;104(11):722-724. [http://dx.doi.org/10.7196/SAMJ.9021] [ Links ]
10. Weyer J, Blumberg L. Ebola virus disease in West Africa - South African perspectives. S Afr Med J 2014;104(11):754-755. [http://dx.doi.org/10.7196/SAMJ.9045] [ Links ]
11. Rossouw TM, van Rooyen M, Louw JM, Richter KL. Blood-borne infections in healthcare workers in South Africa. S Afr Med J 2014;104(11):732-735. [http://dx.doi.org/10.7196/SAMJ.8518] [ Links ]
12. Becker J, Jenkins LS, de Swardt M, Sayed R, Viljoen M. Appropriateness of computed tomography and magnetic resonance imaging scans in the Eden and Central Karoo districts of the Western Cape Province, South Africa. S Afr Med J 2014;104(11):762-765. [http://dx.doi.org/10.7196/SAMJ.8158] [ Links ]














