Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.103 n.6 Pretoria Jun. 2013
RESEARCH
Factors associated with contraceptive use in a rural area in Western Cape Province
N PeerI, II; N MorojeleIII, IV; L LondonV
IMB ChB, LLM (Medical Law), FCPHM (SA), MMed (Public Health). School of Public Health and Family Medicine, University of Cape Town, South Africa
IIHealth Impact Assessment Directorate, Department of Health, Western Cape Provincial Government, Cape Town, South Africa
IIIBSc (Hons), MSc, PhD. Alcohol and Drug Abuse Research Unit, Medical Research Council, Pretoria, South Africa
IVSchool of Public Health, University of the Witwatersrand, Johannesburg, South Africa
VMB ChB, MD, MMed (Public Health), DOH, BSc Hons (Epi). School of Public Health and Family Medicine, University of Cape Town, South Africa. Health Impact Assessment Directorate, Department of Health, Western Cape Provincial Government, Cape Town, South Africa
ABSTRACT
BACKGROUND: Safe and effective contraceptive use can substantially improve women's reproductive health. Although the contraceptive prevalence rate (CPR) in South Africa is comparable to rates globally, inequalities in CPR affect poor and rural women. This study aimed to determine the CPR and factors associated with contraceptive use in a rural district of Western Cape Province.
METHOD: Cross-sectional survey data based on 412 face-to-face interviews with female participants between 18 and 44 years of age were collected in 2006 for a primary fetal alcohol syndrome prevention study in a rural district in Western Cape Province. The study used effective contraception (ECC) as the outcome variable. ECC included use of oral contraceptives, condoms, injectables or sterilisation. Independent variables included socio-demographic factors, substance use, psychosocial factors, community factors, childbearing characteristics and partner characteristics.
RESULTS: Women were more likely to use ECC if they reported high self-esteem (compared with low or moderate self-esteem (prevalence risk ratio (PRR)=1.23; 95% confidence interval (CI) 0.99 - 1.53); if they strongly or moderately agreed that their culture entitled men to make decisions regarding child-bearing compared with those who disagreed (PRR=1.28; 95% CI 0.96 - 1.71); and if they had one child or more compared with no children (PRR=1.62; 95% CI 1.24 - 2.11).
CONCLUSION: The CPR for sexually active women in this study was low at 39.3%. To promote contraceptive use in similar rural populations, family planning programmes should focus on increasing men's approval of contraception, improving partner communication around family planning and bolstering women's confidence in their reproductive decision-making, and particularly their self-esteem. There should be greater focus on nulliparous women.
Contraception is defined as the prevention of pregnancy through temporary or permanent means.[1] Safe and effective contraception has the potential to improve women's reproductive health and their children's lives. Millennium Development Goal (MDG) 5, which focuses on maternal health, aims to decrease the 1990 maternal mortality ratio (MMR) by 75% by 2015.[2] Compared with other middle-income countries with similar levels of economic development, South Africa (SA) has a higher MMR, particularly among poorer women.[2] Owing to data inconsistencies, there are varying estimates currently for MMR in SA, ranging from 230 to 702 per 100 000 live births.[2] This MMR has been increasing since 1990 and was 425% higher by 2008 than predicted, were SA on track to achieve MDG 5.[2]
The contraceptive prevalence rate (CPR), which is the percentage of all sexually active women aged 15 - 49 using a modern contraceptive method,[3] increased modestly in SA from 61.2% in 1998 to 64.6% in 2003, attributable mainly to a rise in the rural CPR from 52.7% to 61.8%, while the urban rates remained more or less stable.[3] SA's CPR is slightly higher than the global CPR of 63% and that of 62% for less developed countries.[4] While global CPRs refer to sexually active women who are married or in a union, marital rates in SA are low. Therefore, use of sexually active women as the denominator is a more realistic basis for estimating CPR than women who are married or in a union. However, this limits comparability with global CPRs.
Cultural values, beliefs and communication with partners affect women's use of contraceptives. SA society, particularly in the rural areas, is still male-dominated, and women feel pressure to prove their fertility.[5] Better communication between women and their partners is reported to increase the likelihood of using contraception,[6] as is high reported self-esteem among women.[7] SA women with higher education levels have been found to be more likely to use contraception[3,8] as is the case in other studies globally.[9-11]
The South African Demographic and Health Survey (SADHS) for 2003 showed that CPR was highest among sexually active women in the 15 - 19-year age group (68.7%), and lowest in the 45 - 49-year age group (57.2%).[3] Women younger than 20 years have complained of barriers to obtaining contraceptives arising from a lack of knowledge, obstacles to access, concerns over side-effects, fear of future infertility[12] and the negative attitude of nursing staff in the clinics.[13] In terms of race groups, black women had the lowest CPR (62.2%) and white women the highest (80.9%).[3] SA's history of racial discrimination, accompanied by gross inequalities in access to education, economic opportunities and health services, probably explains some of these inequities in CPR[14] and is mirrored in similar experiences of disenfranchised or marginalised racial groups elsewhere.[15]
Contrasting the rising national trends, the SADHS showed a 10% decline in the CPR in the Western Cape (WC), from 73.7% in 1998 to 63.4% in 2003.[3] Globally, it is suggested that CPR rates are lower in rural areas and, while rural rates in the SADHS have risen, they are still lower than urban rates. It is therefore possible that poor contraceptive uptake in rural areas may be responsible for the decline in CPR in the WC. Therefore, it is important to look at rural contraceptive use and identify potential predictors. This study attempts to direct attention to rural women who are under-represented in reproductive health research.[11]
The aim of the study was to describe the prevalence of effective contraceptive (ECC) use in fertile women between 18 and 44 years of age in a rural WC population, and to determine socio-demographic, substance use, psychosocial, and childbearing experiences and partner characteristics associated with women's contraceptive use.
Methods
In 2006, a project to develop a comprehensive fetal alcohol syndrome prevention model began in SA. The project included a baseline cross-sectional household survey in an urban and rural area to determine the prevalence and predictors of risk for an alcohol-exposed pregnancy (AEP) among women of child-bearing age.[8] Data collected for the AEP risk study included socio-demographic factors, history of last pregnancy, substance use variables, partner characteristics and contraceptive use, among others. The present study was conducted as a re-analysis of the primary data collected in the WC rural site for the larger AEP risk study. The study population was women of reproductive age (18 -44 years), residing in 3 municipalities (Bergrivier, Swartland and Cederberg) which are commercial farming areas in the West Coast District. Stratified cluster random sampling was used with the intention of recruiting 650 women as participants. From a total set of 1 450 farms across the 3 municipalities, 150 farms were randomly selected. Oversampling was done to anticipate uncontactable, ineligible and non-functional farms. All eligible women who met the inclusion criteria in every household (approximately 7 per farm) within each of the 58 participating farms were asked to participate in the study.
Using a structured questionnaire, trained fieldworkers conducted face-to-face interviews, lasting between 15 and 90 minutes, with eligible women at their homes in their language of preference. Women interviewed gave their informed consent.
ECC (the outcome variable in this study) was defined as taking the pill, using condoms or injectables or being sterilised (scored as Yes - 1). A score of 0 was allocated for ECC if the participant had not used any contraception or was using ineffective contraception, e.g. calendar/rhythm, withdrawal, traditional/herbs/remedies or abstinence. Effectiveness of use was based on respondents' reports; adherence to usage could not be evaluated.
The independent variables were measured in binary scales and comprised 5 domains of socio-demographic factors: age, education, marital status, ethnicity and socio-economic status. Age was categorised into 3 groups: 18 - 24 years, 25 - 34 years and 35 - 44 years, respectively. Educational status was divided into primary schooling or less v. above primary education. Marital status was categorised into married (legally and traditionally), cohabiting, and not married. Ethnicity was categorised as African, coloured, white, and Asian/Indian. For socio-economic status, unemployment was defined as not currently being in any form of employment; participants who reported possession of 5 or more out of 8 household assets (electricity, radio, TV, telephone, fridge, computer, washing machine, cellular telephone) were categorised into high socio-economic status (SES), and those reporting less than 5 into low SES.
A participant who smoked in the last 30 days was classified as a current smoker. Alcohol use was measured using the 10-item Alcohol Use Disorders Identification Test (AUDIT)[16] where participants who scored >8 were classified as having harmful alcohol consumption.
Psycho-social factors included self-esteem, religious involvement, male entitlement and perceptions about cultural prescriptions on childbearing. Using Rosenberg's (1965) 10-item self-esteem scale, the answers were summed and split across the 75th percentile to denote high v. low self-esteem. Questions assessing the participants' religiosity and level of religious practice were assessed on a 6-item religious orientation scale.[17] Scores were summed, and divided into high and low religiosity, split at the 75th percentile. Using a single-item question answered on a Likert scale, participants' extent of agreement that their culture entitles males to have as many children as they wish, a score of 1 was allocated to those who strongly or moderately agreed. All others were allocated a score of 0 on this measure. A single-item question was used to assess participants' belief that their culture prescribed a childbearing obligation upon women; a score of 1 was allocated to those who agreed (any degree of agreement), and a score of 0 to those who did not agree (any degree of disagreement).
Childbearing experiences included parity and previous unwanted pregnancy. Parity was dichotomised into >1 (1) v. 1 or none (0). For previous unwanted pregnancy, the participants were asked: At the time you became pregnant with your last child, how much did you want to become pregnant then? Polytomous dummy variables were created for the answer options, i.e. a great deal, a little, not much, or not at all. Age at first sex was dichotomised into <18 years (0) and >18 years (1).
Partner characteristics were dichotomised as age <29 years (0) v. >30 years (1) for 'older partner; and education <Grade 9 (0) v. >Grade 9 (1), for 'partner education'.
Statistical analysis
Data were analysed in STATA 10.0. For the estimation of CPR, the number of sexually active women, defined as a woman who reported sex in the last 4 weeks, was used for the denominator for comparability with the SADHS. Logistic regression analysis was used for model building, to determine any significant bivariate associations between each individual predictor and ECC. Independent variables that had an association with ECC at a probability of p<0.1 were then included in multivariate logistic regression models, with ECC as the dependent outcome. Prevalence risk ratios (PRRs) were calculated from the beta-coefficient regression estimates. Likelihood-ratio statistics and Akaike's information criterion (AIC) were used to contrast the relative goodness of fit between competing logistic-regression models. To identify the best model, models were examined for the lowness of their AIC value and tested using a likelihood ratio test that compares difference in deviances of nested models against a chi-squared distribution. Although Male entitlement was not significant at p-value <0.05, the model without it was not as good a fit as the one with it, and was significant at p<0.1. As a result, the model with the best fit was chosen.
Diagnostics, including a plot of residuals v. linear predictors and the Pearson goodness-of-fit test, confirmed adequacy of the models. Multivariate analysis was repeated using the svy command to adjust for the clustering effect from sampling all women in each farm, and the magnitude of the effects remained the same. Two sensitivity analyses were conducted by repeating the analyses on a sub-sample of sexually active women and a second sub-sample excluding women who reported sterilisation.
Ethics approval was granted by the Health Research Ethics Committees of the Universities of Pretoria (121/2005) and Cape Town (026/2012). All relevant stakeholders were also consulted and approached for permission prior to starting the study.
Results
Of the 496 women approached to participate in the study, 83% completed the questionnaire, resulting in 412 respondents from the 3 municipalities, of whom 90% were coloured and whose mean age was 31 years; 59.7% (n=246) were sexually active (Table 1).
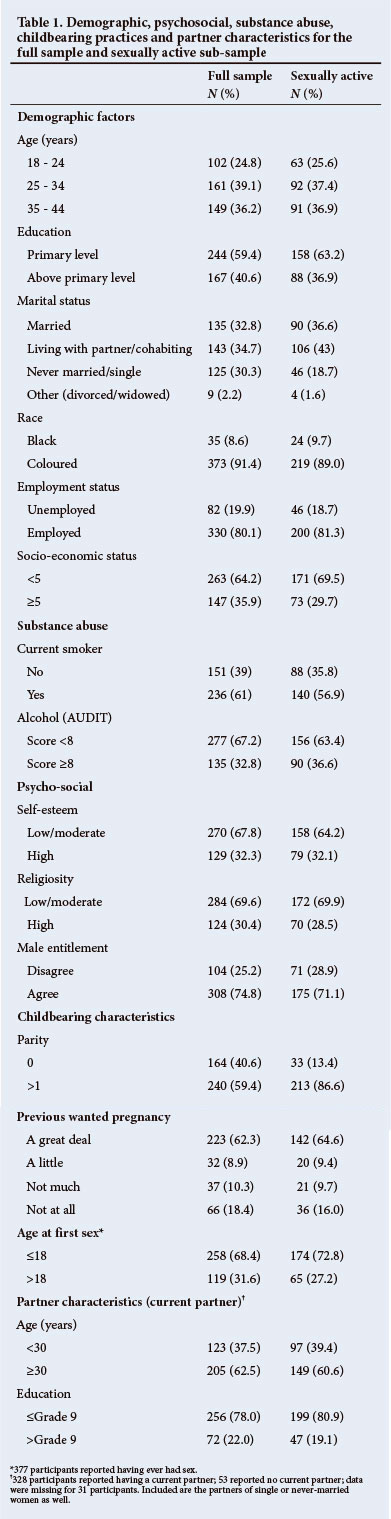
Most (80.1%; n=330) women were employed; 35.9% (n=147) of women reported owning 5 or more household assets; 61% (n=236) reported current smoking; 32.8% (n=135) had an AUDIT score >8; 67.7% (n=270) had low or moderate self-esteem; 74.8% (n=308) agreed that males should be entitled to make fertility decisions; and 40.6% (n=164) had no children (Table 1). There was no difference in the demographic and other characteristics between the sub-sample of sexually active women and the entire sample.
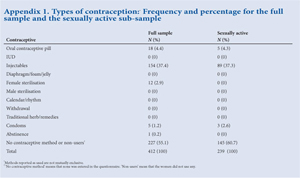
Of participants, 44.9% (n=185) reported using ECC (including the pill (4.4%), injectables (37.4%), sterilisation (2.9%) and condoms (1.2%)), while 55.1% (n=227) reported no contraception or ineffective contraception. Among sexually active women (n=145), the CPR was 39.3% and the types of contraceptives used included the pill (4.3%), injectables (37.3%) and condoms (2.6%). No sexually active woman reported sterilisation as their form of contraception. All women using condoms also reported concurrent use of injectables.
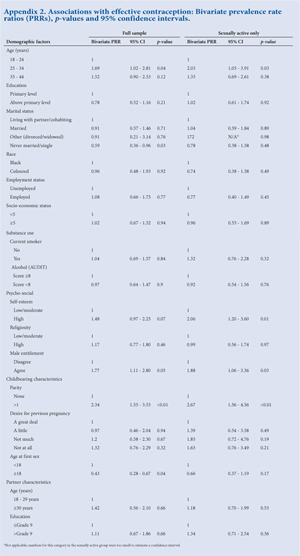
Bivariate analysis in the full sample (data provided in appendices) found significant associations between ECC and the following variables: within age group 2, the 25 - 34-year-olds v. the 18 - 24-year age group (PRR=1.69, 95% CI 1.02 - 2.81); being never married or single v. living with a partner or cohabiting (PRR=0.59, 95% CI 0.36 - 0.96); increasing parity (PRR=2.34, 95% CI 1.55 - 3.53); male entitlement (PRR=1.77, 95% CI 1.11 - 2.80); and age >18 older at first sex v. <18 (PRR=0.43, 95% CI 0.28 - 0.67). The association with high self-esteem v. low was of marginal significance (PRR=1.48, 95% CI 0.97 - 2.25).
Bivariate associations in the sexually active group showed a similar pattern of associations with the measures of effect being generally higher but with slightly wider CIs. However, age >18 at first sex and living with a partner/cohabiting were not associated with contraceptive use.
The results of multivariate modelling are shown in Table 2. After model building and model checking, the final model included only Self-esteem, Male entitlement and Parity. For the full sample, women having a high self-esteem were 1.23 (95% CI 0.99 - 1.53) times more likely to use ECC than those who had low or moderate self-esteem. Women who strongly or moderately agreed that their culture entitled men to make decisions regarding child-bearing were 1.28 (95% CI 0.96 - 1.71) times more likely to use ECC than those women who disagreed. Lastly, women who had >1 child were 1.62 (95% CI 1.24 - 2.11) times more likely to use ECC than those women who did not have children. The findings were similar in the sexually active sub-group, but were somewhat attenuated in strength.
Discussion
The study demonstrated some notable findings. Foremost was that the CPR for sexually active women was low at 39.3%, indicating that more women were not using ECC than those who were. This CPR was lower than the national CPR (64.6%) and the rural CPR (61.8%) for sexually active women in SA in 2003.[4] The CPR was also lower than the WC CPR of 63.4% which might suggest large discrepancies between urban and rural women's CPR in the WC. It is known that the study areas are particularly poor socio-economic areas.[18] Globally low SES is associated with poor and inconsistent contraceptive use.[17,19] Lower SES women, and particularly those in rural areas, have limited access to health services, which may limit their contraceptive access.[3,13]
A number of difficulties may explain the the low CPR. Firstly, farm workers live on private farms and are often highly dependent on their employers for healthcare access. Travelling to and from the clinic is typically arranged by, and dependent on, the farmer as employer. Women workers may also be embarrassed or fearful of losing their jobs if having to ask the farmer for transport to the clinic to access family planning.[20] Also, the WC Department of Health has phased out mobile clinics in favour of fixed clinics that are within 5 kilometers of all communities. Evidence presented to a public hearing in 2003 on farm workers' conditions suggested that they are unwilling to risk losing much-needed wages as a result of visiting a clinic.[21]
The population in this study was an older population (women 18 - 44 years old), which could partly explain the lower overall CPR compared with the SADHS figures. The SADHS, however, does not provide rural age-specific rates against which age standardisation might be undertaken.
Secondly, regarding contraceptive choice, an overwhelming majority of women use injectables and a minority the pill. Rates of condom use for contraceptive purposes were very low, and the women who indicated condom use (1.2%) were concurrently using injectables for contraception. This is in contrast with the 7.8% of women in the SADHS who were classified as currently using condoms as contraception. It is noteworthy that no women reported use of IUDs or male partner sterilisation. This fact might reflect poor access to reproductive healthcare and/or cultural preferences, but requires futher study.
Regarding associations with effective contraception, the full sample and the sexually active group showed similar patterns of associations (Table 2), with the latter group having weaker associations and wider CIs, a finding explained by the smaller sample size.
Three factors emerged as potential predictors of ECC usage:
- High self-esteem as a predictor of ECC usage is consistent with other studies. McNair et al.[7] highlighted that females with high self-esteem were more likely to frequently use and sustain contraception. Ethier et al.[21] showed that low self-esteem predicted a lack of contraceptive use. Four of the 5 studies reported in Mecca et alls book The Social Importance of Self-esteem[22] revealed that low self-esteem is associated with less frequent or less sustained use of contraceptives.
- In contrast, the findings for male entitlement (women reporting a belief that men were entitled to make decisions regarding child-bearing were more likely to use ECC in this study) were inconsistent with the literature where, in southern Africa, male domination and pressures on women to prove their fertility are common issues resulting in women not using contraception. A Zambian study found that only 20% of men approved of contraceptive use, believing that contraception will prevent women having the number of children they desire.[19] The study involved a rural site that is a commercial farming area, unlike traditional rural areas where men are the decision makers,[14] which may explain our inconsistent finding. Injectables enable a woman to be on contraception without the knowledge of her partner.
- The third positive association of parity and ECC use is supported by the literature. Morojele et al.[8] in their study on alcohol-exposed pregnancy predictors, using the same sample, hypothesised that having children exposes a woman to family planning and antenatal clinics from which she can learn about accessing contraceptives. Similarly, London's study on Pap smear coverage among rural WC women suggested that parity was associated with improved access to public sector services for cervical cytology,[23] and is consistent with findings in this study.
Some limitations exist. Firstly, a cross-sectional study cannot establish cause and effect and directionality in associations observed. A cohort study would be a better study design. Secondly, the study targeted women between 18 and 44 years old, so no inference can be made about adolescents. Thirdly, the outcome variable Effective contraception use was self-reported, so its validity cannot be corroborated with medical records or any other information sources. The women could have misunderstood the questionnaire or not been honest. However, it is unlikely to account for a 14% difference in CPR from the SADHS findings. Moreover, since the main focus of the primary study was on risk for alcohol exposure in pregnancy, it is not likely that there would be strong reason for the women to misreport contraceptive use. Similarly, alcohol consumption and smoking was self-reported, and possibly under-reported. However, there are other studies[12] among farmworker populations reporting similar rates of smoking and alcohol consumption. Fourthly, it is unknown if the Single or Never married women had regular partners or casual partners. This is a limitation of the data because one of the key issues in contraception use is partner acceptance, and Single or Never married women may have more control over contraceptive use than their Married or Cohabiting counterparts. Notwithstanding these limitations, the findings were generally consistent with the literature.
Conclusion
The CPR among the study population, sampled from rural women in commercial farming areas of the WC, was lower than the rest of the province and country at large, including that of the rural population nationally for sexually active women. To improve CPR, the study findings suggest that the following programmatic interventions may be helpful: To promote contraceptive use, particularly in a rural area, family planning programmes could focus on increasing male support of contraception, improving partner communication around family planning, and bolstering women's confidence in their reproductive decision-making. Efforts should also be made to improve self-esteem of women, in particular younger women between the ages of 18 and 24 years and adolescents. Younger women had the lowest CPR in this study, and their needs should be prioritised. Also, there should be a greater focus on nulliparous women for family planning than their counterparts who already have children. These strategies imply community-based health promotion interventions that address women's reproductive health comprehensively, which would draw on multi-sectoral resources (e.g. departments of Social Development, Labour, etc.), the private sector (e.g. employers) and NGOs). However, given the limitations of a cross-sectional design, it would be ideal to conduct a cohort study to better investigate cause and effect relationships.
ECC use has the potential to greatly improve women's reproductive health. Improving the CPR will contribute substantially to reducing maternal mortality in SA. There needs to be more investment in access to reproductive health services as a tool for improving the lives of SA women and rural farming women in particular. Further studies should seek to explain why rural farming women have a lower CPR than other rural women. In particular, barriers arising from the employer-employee relationship on commercial farms, which are not applicable to other rural settings, may explain the particularly low CPR in this population.
Acknowledgements. This research was supported by Co-operative Agreement Number 1 U01 DD00044 from the Centers for Disease Control and Prevention (CDC). Its content is solely the responsibility of the authors and does not necessarily represent official views of the CDC. We gratefully acknowledge the field co-ordination and supervision efforts of Nontobeko Jacobs, the Dopstop Association, Chantel Mazok, Molefe Pule, Nosimilo Zama, Owen Manda, Elmarie Nel and Bridget Kekana. Alta Hansen was responsible for entering the data sets. For the West Coast Health District, we acknowledge the support of Carien Bester, Wilma Kamfer, Ester van Ster and Elzette Diedericks.
References
1. Department of Health, Republic of South Africa. National Framework and Guidelines for Contraceptive Services. Pretoria: Department of Health, 2001. [ Links ]
2. Blaauw D, Penn-Kekana M. Maternal Health. In: Fonn S, Padarath A, eds. South African Health Review, 2010. Durban: Health Systems Trust, 2010. [ Links ]
3. Department of Health, Republic of South Africa. South African Demographic and Health Survey 2003. Pretoria: Department of Health, 2005. [ Links ]
4. United Nations, Department of Economic and Social Affairs, Population Division. World Contraceptive Use 2010 (POP/DB/CP/Rev2010). Geneva: United Nations, 2011. [ Links ]
5. Department for Economic and Social Information and Policy Analysis Population Division, UNO. Family Planning, Health and Family Well-Being: Proceedings of the United Nations Expert Group Meeting on Family Planning, Health and Family Well-Being. Bangalore, India, 26 - 30 October 1992. New York: UNO, 1996. [ Links ]
6. Sayem MA, Begum HA. Socio-cultural determinants of contraceptive use among rural women aged 1529 years from marriage to first live birth. Ibrahim Med Coll J 2008;2:49-54. [ Links ]
7. McNair LD, Carter JA, Williams MK. Self-esteem, gender and alcohol use: relationships with HIV risk perception and behaviours in college students. J Sex Marital Ther 1998;24:29-36. [ Links ]
8. Morojele NK, London L, Olorunju SA, Matjila MJ, Davids AS, Rendall-Mkosi K. Predictors of risk of alcohol-exposed pregnancies among women in an urban and rural area of South Africa. Soc Sci Med 2010;70:534-542.[http://dx.doi.org/10.1016/j.socscimed.2009.10.040] [ Links ]
9. Moronkola OA, Fakeye JA. Reproductive health knowledge, sexual partners, contraceptive use and motives for premarital sex among female sub-urban Nigerian secondary students. Int Q Community Health Educ 2007-2008;28:229-238. [ Links ]
10. Hartlage SA, Beaux C, Gehlert S, Fogg L. Rural and urban midwestern United States contraception practices. Contraception 2001;63:319-323. [ Links ]
11. Kham MH, Shah H, Saba N, et al. Study of contraceptive user women in D I Khan, Pakistan. Biomedica 2007;23:24-26. [ Links ]
12. Williamson LM, Parkes A, Wight D, Petticrew M, Hart GJ. Limits to modern contraceptive use among young women in developing countries: a systematic review of qualitative research. Reprod Health 2009;(6):3. http://www.reproductive-health-journai.com/content/6/1/3 (accessed 13 December 2011). [ Links ]
13. Wood K, Jewkes R. Blood blockages and scolding nurses: Barriers to adolescent contraceptive use in South Africa. Reprod Health Matters 2006;14:109-118. [http://dx.doi.org/10.1016/S09688080(06)272318] [ Links ]
14. Cooper D, Morroni C, Orner P, et al. Ten years of democracy in South Africa: documenting transformation in reproductive health policy and status. Reprod Health Matters 2004;12:70-85.[C] [ Links ]
15. Saxena S, Copas AJ, Mercer C, et al. Ethnic variations in sexual activity and contraceptive use: national cross-sectional survey. Contraception 2006;4(3):224-233. [http://dx.doi.org/10.1016/j.contraception.2006.03.025] [ Links ]
16. Babor FT, Higgins-Biddle JC, Saunders JB, Monteiro MG. The Alcohol Use Disorders Identification Test. Guidelines for use in primary care. Geneva: World Health Organization, Department of Mental Health and Substance Dependence, 2001. [ Links ]
17. Idehen EE. The development and evaluation of a religiosity scale. IFE PsychologIA 2001;9:58-69. [ Links ]
18. Jacobs P, Makaudze E. Understanding rural livelihoods in the Cape West Coast: Policy Brief 1. Cape Town: The Surplus Project, June 2009. http://www.spp.org.za (accessed 12 December 2011). [ Links ]
19. Biddleton AE, Fapohunda BM. Covert contraceptive use: prevalence, motivations and consequences. Stud Fam Plann 1998;29(4):360-372. [ Links ]
20. South African Human Rights Commission. Final report on the Inquiry into Human Rights Violations on Farming communities: August 2003. http://www.sahrc.org.za/home/21/files/Reports/farming_inquiry_report_prov.PDF (accessed 26 April 2012). [ Links ]
21. Ethier KA, Kershaw TS, Lewis JB, et al. Self-esteem, emotional distress and sexual behaviour among adolescent females: inter-relationships and temporal effects. J Adolesc Health 2006;38:268-274. [http://dx.doi.org/10.1016/j.jadohealth.2004.12.010] [ Links ]
22. Mecca AM, Smelser NJ, Vasconcellos J. The Social Importance of Self-esteem. London, UK: University of California Press Limited, 1989. [ Links ]
23. London L. Pap smear coverage amongst rural workers. S Afr Med J 1993;83(3):172-176. [ Links ]
Accepted 10 January 2013.
 Correspondence: N Peer (naziapeer@gmail.com)
Correspondence: N Peer (naziapeer@gmail.com)
Appendix 1:
Appendix 2: