Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.102 n.11 Pretoria Jan. 2012
RESEARCH
Demographics and management of dog-bite victims at a level two hospital in KwaZulu-Natal
S J W KentI; B NaickerII; D R WoodIII
IMB BCh, BSc. Ngwelezane Hospital, KwaZulu-Natal
IIMB BCh. Ngwelezane Hospital, KwaZulu-Natal
IIIMB BCh, M Phil (EM), FCEM (UK). Ngwelezane Hospital, KwaZulu-Natal
ABSTRACT
INTRODUCTION: Dog bites are a significant cause of morbidity and mortality worldwide, particularly where rabies is endemic. There is also a significant financial burden attached to prophylactic treatment to diminish the risk of rabies infection. KwaZulu-Natal (KZN) has a high incidence of human rabies yet little is known about the demographics of dog bites in the province.
OBJECTIVES: To analyse the demographics of dog bites in Northern KZN.
Methods. Records of all dog bites presenting to the main referral hospital in northern KZN between August 2007 and September 2011 were analysed.
RESULTS: We collected data for 821 instances of dog bite. Male children aged 6 - 10 years are most likely to present with dog bites, while women >40 years are more likely to present than men in the same age bracket. While initial vaccine administration is high (98%) with all grades of bite, only 82% of grade 3 bites receive immunoglobulin.
CONCLUSION: Our results correlate well with two large studies of the demographics of dog bites, but are the first to show a reverse in male preponderance of presentations above the age of 40 years. Reasons for low rates of immunoglobulin administration in grade 3 bites are discussed. Finally, methods are suggested to improve data collection and the care of patients presenting with dog bites.
Dog bites are a major source of morbidity and mortality worldwide, accounting for up to 1.5% of all visits to emergency medicine units (EMUs).1 They represent an even higher financial and disease burden in rabies-endemic areas such as KwaZulu-Natal (KZN),2 because expensive post-exposure prophylaxis, which represents a significant proportion of EMUs' annual drugs budget, must be administered to many bite victims. Since rabies is almost universally fatal, its control is of paramount importance in endemic areas.
Around 10 - 30 human cases of rabies are confirmed each year in South Africa, and result almost exclusively from dogs biting humans.2 A current programme funded by the Bill and Melinda Gates Foundation, that aims to eradicate rabies in South Africa and worldwide, uses dog vaccination and animal contact tracing to prevent dog-to-dog transmission. Yet little is known about dog-to-human transmission.3 Since targeted rabies eradication programmes to prevent dog-to-human transmission may be strategically viable in KZN, understanding the demographics of dog bites plays an important role in understanding and controlling the transmission of the virus.
Immunocompromised patients may present with atypical rabies. Only one paper has been published on this subject, in which a patient in Mali presented atypically with encephalitis following a dog bite.4 Therefore in areas such as KZN, where HIV is epidemic, high diagnostic suspicion for rabies is needed when dealing with the demographic groups who are more likely to have sustained dog bites.
Internationally, dog bites are graded as 1, 2 or 3, depending on severity (Table 1). This grading is important because it guides therapy: only grade 3 bites require immunoglobulin; only grade 2 or 3 bites require vaccine; and grade 1 bites require no treatment.
Administration of rabies vaccine alone is unlikely to have any effect on disease progression if the rabies virus has been transmitted in the bite. This can only be prevented through the use of immunoglobulin, which is effective against the rabies virus for the first 10 days after exposure. Anecdotally, up to a third of emergency department drug budgets may be spent on rabies immunoglobulin. An average adult's administered immunoglobulin costs R2 122, representing a significant financial burden, which could be minimised by targeting therapy only to those at risk.
Internationally, few publications examine the demographics of dog bites, and none looks at their management. Publications suggest that dog bites are most prevalent in children between the ages of 1 and 9 years, but no studies consider sex differences in adults, or are specific to the population of KZN.1, 5
A study examining the demographics of dog-bite victims in KZN is important, as it will inform clinicians about which patient groups must be treated with a high diagnostic suspicion for rabies; inform and refine the rabies eradication programme; and highlight the cost of immunoglobulin and when best to use it.
Therefore, we studied the demographics and treatment of dog-bite victims presenting to a tertiary referral centre in northern KZN.
Methods
Records were maintained for all dog-bite victims presenting to the EMU at Ngwelezane Hospital, the main referral hospital for northern KZN, between August 2007 and September 2011. For each instance of dog bite, information recorded included age (in years), sex, home location, and clinical information including grade of dog bite and treatment given. The grade was determined using the common scale of rabies exposure (Fig. 1).2
Treatment given was (i) advice only; (ii) rabies vaccine; or (iii) rabies vaccine with rabies immunoglobulin. The number of doses of vaccine administered was incompletely recorded and often given at peripheral clinics, and is therefore not included in the final analysis. Treatment was guided by the South African guidelines (Fig. 1). Records were maintained in a paper ledger in the EMU. For our study, each instance was entered onto a prospectively maintained database on a password-protected computer using Microsoft Excel, and analysed using the same programme. Analysis was carried out using simple descriptive statistics. Records were maintained and analysed in accordance with local policy on patient confidentiality and consent.
All information relating to the cost of immunoglobulin was taken from the hospital pharmacy computer system.
The Ngwelezane Hospital ethics committee approved the study.
Results
Between August 2007 and September 2011, a total of 821 patients presented to Ngwelezane Hospital complaining of dog bites. Of these, 458 (55.8%) patients were male, and ages ranged between 0 and 86 years old. Sex was not recorded for 2 patients.
The average age of patients presenting with dog bites was 25 years, and the most common age was 10 years (19 patients). The most common age group to present with dog-bite injuries was age 6 - 10 (148 patients). Younger males were bitten more commonly than younger females, although females >40 years were bitten more commonly than males in the same age group.
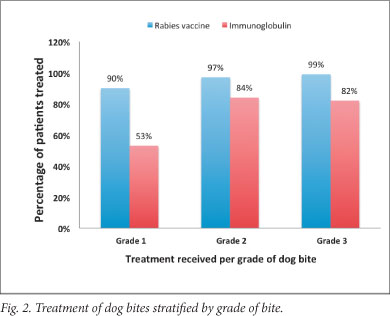
Of the 821 bites, 642 (78%) were grade 3; 84 (10%) were grade 2; and 43 (5%) were grade 1. In 52 cases (7%), grade of bite was not recorded.Treatment with rabies vaccine was started in 90% of cases of grade 1 bites, 97% of grade 2 bites and 99% of grade 3 bites (Fig. 2). Immunoglobulin was administered for 53% of grade 1 bites, 84% of grade 2 bites and 82% of grade 3 bites.
The total cost oftreatment with Rabigam (rabies immmunoglobulin) was R802 767, for 461 120 international units (IU) of rabies immunoglobulin at R530 for 300 IU. Of this total cost, R640 487 was spent on grade 3 bites and R162 279 on grade 1 and 2 bites.
Discussion
A prospectively maintained database was used to demonstrate the demographic features and treatment administered to patients presenting with dog bites to a tertiary referral centre in northern KZN. Males present more frequently than females, and young males (ages 6 - 10) are most likely to present. This trend reverses after the age of 40 years, when females are more likely to present than males. We also showed that 99% of grade 3 bite patients are treated with rabies vaccine, but the rate of treatment with immunoglobulin is lower (82%).
Our results agree with the other large South African study of dog-bite demographics,5 that suggests that the most common age group to present with dog bites is 4 - 7 years, with a mean of 6.84 years. Dwyer et al. also found that young male patients are more likely than females to present with dog bites. The other large study on dog-bite demographics, conducted in Florida, USA, suggests that a younger age group (1 - 4 years) presents more commonly.1
Our results suggest that targeting parents remains the best strategy to ensure that dog-bite patients present at hospitals. This is because most patients are young (6 - 11) and rely on their parents for healthcare and transport. School-based interventions may also be viable, but this may be less effective because northern KZN's population is rural and school attendance is relatively low.6
In immunocompromised patients who are bitten by a rabid animal and do not present to hospital, subsequent development of rabies may go unnoticed or be treated as HIV-associated encephalitis or meningitis. Therefore high levels of suspicion for rabies are advisable in all immuncompromised individuals presenting with neurological symptoms. The rabies virus can be tested for by using PCR on buccal swabs; this is an important measure to identify outbreaks of rabies which might otherwise go unnoticed.
Rabies vaccine is administered to patients presenting with dog bites in a high rate of cases. Grade 1 dog bites need no treatment,2 yet 90% of these patients received vaccination and 53% received immunoglobulin. As immunoglobulin is expensive, its use should be reserved for patients with higher-risk bites. Further education on the risk stratification of dog bites could help to rectify this over-treatment, and decrease spending on immunoglobulin.
Patients with grade 3 bites should be given immunoglobulin. In these cases, vaccine should be initiated on the first visit to hospital and only discontinued if the dog remains healthy after 10 days, or if laboratory samples confirm that the animal does not have rabies. However, only 82% of our patients with grade 3 bites received immunoglobulin. Possible reasons for this include:
- If the dog is known to the patient, is known to be vaccinated, and is healthy, then at Ngwelezane Hospital immunoglobulin is not administered as the risk of transmission is judged to be extremely low.
- Since there were no cases of rabies in our cohort, or at the hospital during our study period, or indeed in the whole of South Africa in 2009,7 healthcare providers may be complacent about the importance of immunoglobulin and vaccine administration in grade 3 bites.
- It is possible that the recording of grade of bite was inaccurate, and that many of the bites did not require immunoglobulin.
Over the three-year study period, immunoglobulin costing over R160 000 was administered to dog-bite victims who did not require it. This represents a potential cost saving of around 25%. Rabies immunoglobulin is the 9th most expensive drug purchased by our hospital (after antiretrovirals, insulin and plasma products) and reducing its use would represent a welcome saving.
The limitations of this study primarily relate to the maintenance of the database. Bites are recorded by EMU nurses and doctors, who see and treat the dog-bite patients, in a paper ledger stored in the EMU. Therefore some cases may be incompletely recorded or not recorded, as is seen in the 7% of cases for which grade of bite is not recorded. New staff, who may not be adequately inducted into the EMU, may be particularly prone to this. The grading system for bites is also open to interpretative error, although this is minimised by displaying the grading system on the wall of the EMU.
Many cases of dog bite will never present to the EMU and will be managed in the community with traditional treatments or no treatment. This is particularly the case for grade 1 and 2 exposures, which are usually not perceived to be a risk to health. This may be why we record so few cases of grade 1 and 2 exposures, even though these must occur more frequently than grade 3 exposures.
Repeated dosing of vaccine is also recorded incompletely in many cases. This is because dosing is often initiated or continued at peripheral clinics. Therefore we did not analyse information pertaining to the number of doses of vaccine patients received.
Educating EMU staff about the importance of recording dog bites, the correct grading of bites, and the recommended treatment modalities would improve patient care. Installing a robust computer database to record demographic data would also improve the quality of record keeping. If this included a hospital-wide computer network, then patient care and follow-up could be vastly improved with minimal financial and time investment.
We have shown that dog bites in northern KZN are most likely to occur in young males between the ages of 6 and 10 years. Treatment with rabies vaccine is almost universal in patients presenting with dog bite, but administration of immunoglobulin to patients with grade 3 bites is lower than expected. Furthermore, the inappropriate use of expensive immunoglobulin in grade 1 and 2 bites places an unnecessary burden on the healthcare budget. We wish to emphasise the importance of correctly classifying the grade of dog bite and of treating with immunoglobulin when necessary, to minimise cost and maximise prevention of further cases of rabies in humans.
References
1. Shelton K. Dog Bites: Epidemiology and Prevention. Tallahassee: Bureau of Epidemiology, Florida Department of Health, May 2010. [ Links ]
2. Bishop GC, Durrheim DN, Kloeck PE, et al. Rabies: The Guide for Medical, Veterinary and Allied Professionals. 2nd ed. Pretoria: Government Printer, 2003. [ Links ]
3. World Health Organization. Bill & Melinda Gates Foundation fund WHO-coordinated project to control and eventually eliminate rabies in low-income countries. http://www.who.int/rabies/bmgf_who_project/en/index.html (accessed 26 March 2012). [ Links ]
4. Adle-Biassette H, Bourhy H, Gisselbrecht M, et al. Rabies encephalitis in a patient with AIDS: A clinicopathological study. Acta Neuropathol 1996;92(4):415-420. [ Links ]
5. Dwyer JP, Douglas TS, Van As AB. Dog bite injuries in children - a review of data from a South African paediatric trauma unit. S Afr Med J 2007;97(8):597-600. [ Links ]
6. Chapman S, Cornwall J, Righetti J, Sung L. Preventing dog bites in children: randomised, controlled trial of an educational intervention. BMJ 2000;320(7248):1512-1513. [ Links ]
7. Society for General Microbiology. Hope For Rabies Eradication Strategy In Africa. ScienceDaily, 24 January 2009. http://www.sciencedaily.com/releases/2009/01/090121091237.htm (accessed 26 March 2012). [ Links ]
Accepted 6 July 2012.
 Corresponding author:
Corresponding author:
S Kent
(sjwkent@gmail.com)














