Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.102 n.6 Pretoria Jun. 2012
RESEARCH
Complement component C5 and C6 mutation screening indicated in meningococcal disease in South Africa
E P OwenI; F LeisegangII; A WhitelawVI; J SimpsonV; S BakerVI; R WurznerX; P PotterVII; A OrrenIII, VIII, IX
IPhD. Division of Chemical Pathology, Department of Clinical Laboratory Sciences,University of Cape Town and National Health Laboratory Service
IIBSc. Division of Chemical Pathology, Department of Clinical Laboratory Sciences,University of Cape Town and National Health Laboratory Service
IIIBSc, MB ChB, MD. Division of Chemical Pathology, Department of Clinical Laboratory Sciences,University of Cape Town and National Health Laboratory Service
IVMB BCh, MSc, FCPath (SA). Division of Microbiology, Department of Clinical Laboratory Sciences, University of Cape Town, and National Health Laboratory Service
VMB ChB, MMed. Division of Microbiology, Department of Clinical Laboratory Sciences, University of Cape Town, and National Health Laboratory Service
VIMSc (Med). Allergy Diagnostic and Clinical Research Unit, University of Cape Town Lung Institute, Department of Medicine, University of Cape Town
VIIMD, FCP (SA), FAAAAI, FACAAI. Allergy Diagnostic and Clinical Research Unit, University of Cape Town Lung Institute, Department of Medicine, University of Cape Town
VIIIBSc, MB ChB, MD. Allergy Diagnostic and Clinical Research Unit, University of Cape Town Lung Institute, Department of Medicine, University of Cape Town
IXBSc, MB ChB, MD. Institute of Infection and Immunity, Cardiff University, UKXMD, PhD. Division of Hygiene and Medical Microbiology, Innsbruck Medical University, Innsbruck, Austria
ABSTRACT
BACKGROUND: Invasive meningococcal disease (MD), caused by Neisseria meningitidis infection, is endemic in South Africa, with a seasonal peak in winter and spring. There were 2 432 laboratory-confirmed cases between 2006 and 2010. Human deficiency of the fifth complement component (C5D) or complete absence of the sixth component (C6Q0) leads to increased risk of MD, which is often recurrent. All attacks are serious and can lead to death or severe long-term consequences.
OBJECTIVE: To determine the frequency of specific disease-associated C5 and C6 gene mutations in patients presenting with MD in the Western Cape.
RESULTS: In 109 patients with confirmed invasive MD investigated for local mutations known to cause C5D and C6Q0, 3 were C5D and 11 were C6Q0. In 46 black patients tested, 3 were C5D and 7 were C6Q0. In 63 coloured patients, none were C5D and 4 were C6Q0. All deficient patients were followed up and offered prophylaxis.
CONCLUSION: C5D and C6Q0 are not rare genetic diseases in South Africa and affected patients are susceptible to repeated MD; 12.8% of MD patients tested were C5D or C6Q0. Blacks were at greatest risk with 21.7% being either C5D or C6Q0. We strongly recommend diagnostic testing for complement C5 and C6 deficiency in the routine work-up of all MD cases in South Africa. Prophylactic treatment should be started in susceptible individuals.
Terminal complement components comprise the final 5 components of the complement cascade (C5 to C9). All combine on antibody-bound (sensitised) target-cell surfaces to produce the membrane attack complex (MAC) which is potentially lytic for bacteria, viruses and mammalian cells. MAC formation is not possible if any terminal components are absent. Patients genetically deficient in any component are typically identified when they present with recurrent meningococcal disease (MD). Infections are endemic in South Africa (SA) with 2 432 cases reported over a 5-year period (2006 - 2010).1 The last epidemic, related to the emergence of serogroup W135,2 occurred in 2005/6 in Gauteng; infection rates in the province increased to 3.98/100 000 from 0.81/100 000 in 2000. Within this period, the Western Cape experienced a decrease in cases from 2.48/100 000 to 1.51/100 000.
About 50 South Africans have been diagnosed with C6Q0 in the Western Cape. The original diagnosis depended on a C6 haemolytic assay.3 C6Q0 subjects have a complete lack of functional C6 - distinct from patients with subtotal C6 deficiency (C6SD), where a small amount of C6 activity remains.4 Four single base pair deletions, each causing a frame-shift mutation, have been found to be responsible for C6Q0;5 the patients were either coloured or black. Three of the mutations were first reported in African-Americans, but the fourth (828delG) was first reported in coloured and black individuals.5-7 Molecular-level investigations of 2 SA families with C5 deficiency have been performed. Preliminary data indicate 3 different C5 mutations in the Cape region.8 Both C5D and C6Q0 can be caused by the identical mutation on both alleles (homozygous) or by 2 different mutations with 1 mutation in each allele (compound heterozygous) on the respective gene.
It is recognised that people with deficiencies of terminal complement components have increased susceptibility to MD.9 However, it is not known how many MD cases in SA are complement deficient. Repeated infections can have long-term consequences including failure to achieve at school, severe headaches, the need for sheltered employment, deafness, and the loss of limbs or digits due to intravascular blood clotting during acute infection.10
In this study we investigated 109 Western Cape patients with culture-confirmed MD; we tested for the 7 molecular defects discussed above (3 in the C5 gene and 4 in the C6 gene).
Methods
The study received ethical approval from the University of Cape Town (REC:REF 259:2007 and approved amendment dated 16 June 2010).
C5 and C6 mutation frequency
Traceable patients diagnosed with culture-confirmed invasive Neisseria meningitidis infection by the National Health Laboratory Service (NHLS) in the Western Cape within the preceding 5 years were included in the study. Race classification for black patients was by name or personal contact. Coloured race was determined by personal contact or information recorded by a health professional. Five white patients were investigated but excluded from the study.
Ethylenediaminetetraacetic acid (EDTA) blood samples were taken from each patient; deoxyribonucleic acid (DNA) was extracted from buffy coat or blood spots. DNA samples were tested for the 2 known C5 gene mutations (Q19X, R1476X) and a third (A252T) that we found associated with C5D.8,11 Four C6 gene mutations (821delA, 828delG, 1138delC and 1879delG), all known to be responsible for C6Q0 in the Western Cape, were examined. The regions of interest were amplified by polymerase chain reaction (PCR) and the mutations detected by allele-specific primers or restriction enzyme digestion. All positive C5D or C6Q0 results were confirmed by DNA sequencing.5,8,12
Frequency controls: 1 500 newborn cord bloods were tested for C5 mutation A252T (750 black, 750 coloured); 400 cord bloods were tested for C5 mutations Q19X and R1476X (200 black, 200 coloured); and 180 white patient samples were tested for all 7 mutations.
C5 and C6 protein levels
C5 protein levels were detected with a specific C5 enzyme-linked immunosorbent assay (ELISA) employing the native restricted monoclonal anti-C5 antibody N19-8 and biotinylated goat anti-C5 antibody (in-house).13 C6 protein levels were not determined because earlier studies showed that homozygosity, or compound heterozygosity, of any 2 of the 4 specific C6 defects resulted in a complete lack of functional C6 activity.5,11
Results
Mutation frequency of C5 and C6 genes
A total of 109 patients (or the parents in the case of one infant) with culture-positive MD agreed to participate in the study. C5D or C6Q0 was detected in 21.7% of black (N=46) and 6.3% of coloured (N=63) patients (Table 1).
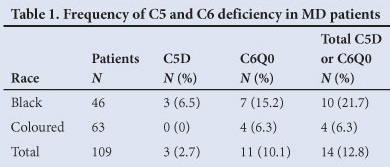
Three black patients were homozygous for C5 mutation A252T. No patient tested positive for C5 mutations Q19X and R1476X. No coloured patient tested positive for C5D. All 4 previously reported C6 mutations (821delA, 828delG, 1138delC and 1879delG) were observed. One patient was homozygous for 828delG and another for 1138delC. Nine patients were compound heterozygous for all 4 mutations in various combinations; 7 of these patients were coloured and 4 were black.
Controls: C5 mutation A252T was found in 55 (45 black and 10 coloured) of 1 500 (750 black, 750 coloured) newborn cord bloods tested (Table 2); no mutant alleles were identified in 400 controls (200 black, 200 coloured) tested for Q19X and R1476X; none of the 7 defects were detected in 180 white patient controls tested. These mutations appear to be rare in whites (the control sample size was relatively small).
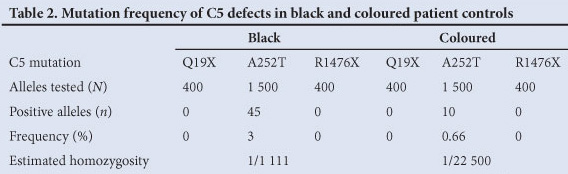
C5 protein levels
C5 levels were tested in 2 of the 3 homozygous C5D-A252T patients (the third died of MD and only DNA was available). ELISA-detected C5 levels were very low (approximately 1 - 2% of normal).
Discussion
Of the 109 MD patients who presented during the preceding 5 years, 2.7% were C5D and 10.1% were C6Q0; 46 were black patients, including 3 C5D (6.5%) and 7 C6Q0 (15.2%); 63 were coloured patients, including 4 C6Q0 (6.3%; none were C5D). A preliminary survey of C5 genetic defects in neonates born in 2002/3, showed expected homozygous C5D-A252T in 1/1 111 black neonates and 1/22 500 coloured neonates.8
It is recognised that C5 deficiency increases susceptibility to MD.11,14,15 We found a significantly increased number of C5-A252T alleles in MD patients compared with the general black population (p<0.005). One heterozygous C5-A252T and no C5-A252T homozygous individuals were found in the coloured MD patients. This may be explained by the small sample number (63 patients) and the low frequency of A252T in the general population.
Based on previous findings in neonates born in 2002/3,10 the predicted C6Q0 frequency was 1/2 873 in blacks and 1/1 600 in coloureds. Yet, we found a much higher prevalence of C6Q0 in black v. coloured MD patients, suggesting a higher susceptibility of the former to MD. This predisposition to MD may be attributed to social factors, poor living conditions and overcrowding.
Based on 2001 census data, there are approximately 1.2 million black and 2.4 million coloured persons in the Western Cape.16 We calculated that approximately 2 000 individuals are C6Q0 and at increased risk of MD. Newborn C6Q0 screening is not available; therefore, it is not possible to speculate as to the percentage of complement-deficient patients that suffer MD. Data from families of C6Q0 patients show that not all C6Q0 siblings suffer MD before the age of 20 years, suggesting that susceptibility is variable.10
A single MD episode can result in serious long-term sequelae; we recently showed that 73% of C6Q0 patients who suffered recurrent MD developed serious illness or died.10 To prevent recurrence, it is essential that all identified C5D and C6Q0 patients can access regular effective antibiotic prophylaxis and vaccination is being considered. Problematically, in the Western Cape approximately 50% of isolated strains are group B,17 for which there is, as yet, no vaccine. Nevertheless, a quadrivalent vaccine (such as Menveo) containing Groups A, C, Y and W135 polysaccharides could be extremely beneficial. A factor H-binding protein, or other protein vaccine, for immunity to Group B and possibly other strains, is currently under investigation.18
One test available for complement deficiency, although only in some centres, involves total haemolytic complement screening. This requires freshly prepared serum samples to be frozen at -80°C until the assay is performed; this is not ideal for screening patients in rural locations. Screening for C5 and C6 deficiency in this study was performed genetically. Samples could be transported at room temperature and DNA could be prepared from blood spots or any blood sample (EDTA blood was preferred). This allowed us to study samples from all over the province.
It is not known whether gene frequencies found in the Western Cape are representative of other black populations across the country. The majority of blacks in the province are reportedly Xhosa;16 ideally, future work should include people from different regions of SA.
Conclusion
We recommend screening for the common C5D and C6Q0 genetic defects in black and coloured patients presenting with meningococcal meningitis in the Western Cape. White patients can be assessed with the total haemolytic complement screen. We hope that the genetic test for C5D and C6Q0 will eventually be available throughout SA. Prophylactic treatment and/or vaccination is/are recommended for patients at risk for MD.
Acknowledgements
This work was supported by the Medical Research Council of South Africa, UCT and the NHLS. AO received support from the Department of Infection, Immunity & Biochemistry, Cardiff University, UK. We thank all MD patients and their families who enabled participation in this study. We also thank the NHLS in the Western Cape for assistance in obtaining blood samples.
References
1. National Institute for Communicable Diseases (NICD). Communicable Disease Surveillance Bulletin 2006, 2007, 2008, 2009 and 2010. http://www.nicd.ac.za (accessed 11 April 201). [ Links ]
2. von Gottberg A, du Plessis M, Cohen C, et al Emergence of endemic serogroup W135 meningococcal disease associated with a high mortality rate in South Africa. Clin Infect Dis 2008;46:377-386. [http://dx.doi.org/10.1086/525260] [ Links ]
3. Orren A, Potter PC, Cooper R, du Toit E. Deficiency of the sixth component of complement and susceptibility to Neisseria meningitidis infections. Studies in ten families and five isolated cases.Immunology 1987;62:249-253. [ Links ]
4. Wurzner R, Orren A, Potter P, et al Functionally active complement proteins C6 and C7 detected in C6- and C7-deficient individuals. Clin Exp Immunol 1991;83:430-437. [http://dx.doi.org/10.1111/j.1365-2249.1991.tb05656.x] [ Links ]
5. Hobart MJ, Fernie BA, Fijen KAPM, Orren A. The molecular bases of C6 deficiency in the Western Cape, South Africa. Hum Genetics 1998;103:506-512. [http://dx.doi.org/10.1007/s004390050858] [ Links ]
6. Nishizaka H, Horiuchi T, Zhu ZB, et al. Molecular bases for inherited human complement component C6 deficiency in two unrelated individuals. J Immunology 1996;156:2309-2315. [ Links ]
7. Zhu ZB, Totemchokchyakarn K, Atkinson TP, Volanakis JE. Molecular defects leading to human complement component C6 deficiency in an African-American family. Clin Exp Immunol 1998;111:91-96. [http://dx.doi.org/10.1046/j.1365-2249.1998.00455.x] [ Links ]
8. Orren A, Owen EP, Potter PC, Leisegang F, Morgan BP, Wurzner R. Complement component 5 deficiency (C5D) in South Africa. Molecular Immunology 2011;48:1863. [ Links ]
9. Figueroa JE, Densen P. Infectious diseases associated with complement deficiencies. Clin Microbiol 1991;4:359-395 [ Links ]
10. Orren A, Owen EP, Henderson HE, et al Complete deficiency of the sixth complement component (C6Q0), susceptibility to Neisseria meningitidis infections, and analysis of the frequencies of C6Q0 gene defects in South Africans. Clinical and Experimental Immunology 2012;167:459-471.[http:// dx.doi.org/10.1111/j.1365-2249.2011.04525.x] [ Links ]
11. Wang X, Fleischer DT, Whitehead WT, et al. Inherited human complement C5 deficiency. Nonsense mutations in exons 1 (Gln1 to Stop) and 36 (Arg1458 to Stop) and compound heterozygosity in three African-American families. J Immunol 1995;154:5464-5471. [ Links ]
12. Parham KL, Roberts A, Thomas A, et al. Prevalence of mutations leading to complete C6 deficiency (C6Q0) in the Western Cape, South Africa and detection of novel mutations leading to C6Q0 in an Irish family. Mol Immunol 2007;44:2756-2760. [ Links ]
13. Wurzner R, Xu H, Franzke A, Schulze M, Peters JH, Gotze O. Blood dendritic cells carry terminal complement complexes on their cell surface as detected by newly developed neoepitope-specific monoclonal antibodies. Immunology 1991;74:132-138. [PMID 1718850] [ Links ]
14. Lopez-Lera A, Garrido S, de la Cruz RM, Fontan G, Lopez-Trascasa M. Molecular Immunology Molecular characterization of three new mutations causing C5 deficiency in two non-related families. Mol Immunol 2009;46:2340-2347. [ Links ]
15. Aguilar-Ramireza P, Reis ES, Floridoa MPC, et al. Skipping of exon 30 in C5 gene results in complete human C5 deficiency and demonstrates the importance of C5d and CUB domains for stability. Mol Immunol 2009;46:2116-2123. [http://dx.doi.org/10.1016/j.molimm.2008.10.035] [ Links ]
16. Statistics South Africa. Census 2001. Pretoria, Statistics South Africa, 2003. http://www.statssa.gov.za/census01/html/default.asp (accessed 11 April 2012). [ Links ]
17. Coulson GB, von Gottberg A, du Plessis M, Smith AM, de Gouvia L, Klugman KP. Meningococcal disease in South Africa, 1999 - 2002. Emerging Infect Diseases 2007;13:273-278. [http://dx.doi.org/10.3201/eid1302.051553] [ Links ]
18. Kedibone MM, du Plessis M, von Gottberg A, et al. Distribution of factor H binding protein beyond serogroup B: Variation among five serogroups of invasive Neisseria meningitidis in South Africa. Vaccine 2011;29:2187-2192. [http://dx.doi.org/10.1016/j.vaccine.2010.11.072] [ Links ]
Accepted 23 March 2012.
Corresponding author: E P Owen (tricia.owen@uct.ac.za)














