Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SAMJ: South African Medical Journal
versão On-line ISSN 2078-5135
versão impressa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.102 no.6 Pretoria Jun. 2012
RESEARCH
The prevalence and burden of pain and other symptoms among South Africans attending HAART clinics
Lindsay FarrantI; Liz GwytherII; Natalya DinatV; Keletso MmolediVI; Ntombi HattaVII; Richard HardingIII, IV
IMB BCh, Dip HIV MAN (SA), MPhil Pall Med. Palliative Medicine Unit, School of Public Health and Family Medicine, University of Cape Town
IIMB ChB, FCFP, MSc. Palliative Medicine Unit, School of Public Health and Family Medicine, University of Cape Town
IIIPhD. Palliative Medicine Unit, School of Public Health and Family Medicine, University of Cape Town
IVPhD. Kings College London, Cicely Saunders Institute, Department of Palliative Care, Policy and Rehabilitation, London, UK
VMD, FCOG, MPhil Pall Med. Wits Palliative Care, School of Internal Medicine, University of the Witwatersrand, Johannesburg
VIRN, MPH, Dip Pall Med. Wits Palliative Care, School of Internal Medicine, University of the Witwatersrand, Johannesburg
VIIRN. Wits Palliative Care, School of Internal Medicine, University of the Witwatersrand, Johannesburg
ABSTRACT
BACKGROUND: Since the advent of antiretrovirals, HIV disease has largely come to be considered a chronic disease for those able to access treatment. As such, the concept of ‘living well’ with HIV is important. Increasing evidence suggests a high symptom burden in HIV that persists in the presence of treatment.
OBJECTIVES: Our study aimed to measure the prevalence and burden of pain and other physical and psychological symptoms among South African HIV-positive patients attending highly active antiretroviral therapy (HAART) clinics.
METHODS: The study design was a cross-sectional survey. Simple random sampling was used to recruit 385 adult participants.
RESULTS: The sample had a median age of 40 years (Q1 - Q3=33 - 46) and 98.4% were receiving HAART. The mean latest CD4 count for the participants was 355.06±219/mm³. The mean number of symptoms of the 32 symptoms on the MSAS-SF experienced by participants was 10.24±5.71 (range 1 - 28). All 4 psychological symptoms were in the top 10 most prevalent symptoms, with feeling sad being the most prevalent symptom overall.
CONCLUSIONS: The high prevalence of symptoms and the high symptom burden experienced by the participants in this survey suggest inadequate symptom control and highlight the palliative care needs of an ambulant patient population already receiving HAART. Extension of life without reasonable efforts to also address the patient’s quality of life is not ethically justifiable. In addition, more research appears to be required to answer whether these findings are associated with sub-optimal HAART adherence.
Since the advent of antiretrovirals, HIV disease has been considered to be a chronic disease for those on treatment. The concept of 'living well' with HIV becomes clinically important as treatment access expands and patients and clinicians have greater expectations of reducing morbidity and mortality. To enable patients to maintain relationships, employment and treatment adherence, the burden of the infection and its treatment must be minimised.
HIV clinical care has focused on viral suppression with little attention paid to the patient's experience of the disease, despite a high symptom burden in HIV1 that persists in the presence of treatment.2,3 In general, doctors tend to overlook the assessment of pain and other treatable symptoms (e.g. nausea) and those due to drug side-effects;1 they focus on symptoms that are physically measurable, such as fever and weight loss, and on patients perceived to be severely ill, and they are more vigilant in asking about symptoms in these situations.1 Our study shows that healthcare workers should not assume absence of symptoms unless a detailed history has been taken. An important finding is that an increased burden of symptoms is associated with poor highly active antiretroviral therapy (HAART) adherence.2 Although the prevalence of symptoms may be high and persists alongside treatment, pain and other symptoms can be controlled effectively by HIV palliative care.4 To generate locally relevant data, we measured the prevalence and burden of pain and other physical and psychological symptoms among HIV patients accessing HAART in 3 public sector HIV clinics.
We found that collaborative efforts, in keeping with the palliative approach, are required to address physical and psychological symptoms experienced by HIV patients in South Africa (SA).
Methods
We undertook a self-report cross-sectional survey conducted at 3 public sector adult HIV treatment clinics between 2009 and 2010. Simple random sampling was used to recruit 385 adult participants by inviting every fifth patient attending the clinic on the study days to participate. Informed consent was obtained from participants, with whom research nurses conducted interviews. The research nurse also administered the Memorial Symptom Assessment Scale - Short Form (MSAS-SF), which has been used in international studies including sub-Saharan Africa.2,3,5 It measures the prevalence and intensity of 28 physical and 4 psychological symptoms over a 7-day period. The MSAS-SF was translated from English into isiZulu and Sesotho by forward and back translation and the interview was conducted in the patient's language of choice. Data were entered into STATA for analysis, and descriptive data generated for the sample characteristics and symptom prevalence and burden. The study was approved by the Committee for Research in Human Subjects (Medical) at the University of the Witwatersrand and by the Human Research Ethics Committee of the University of Cape Town.
Results
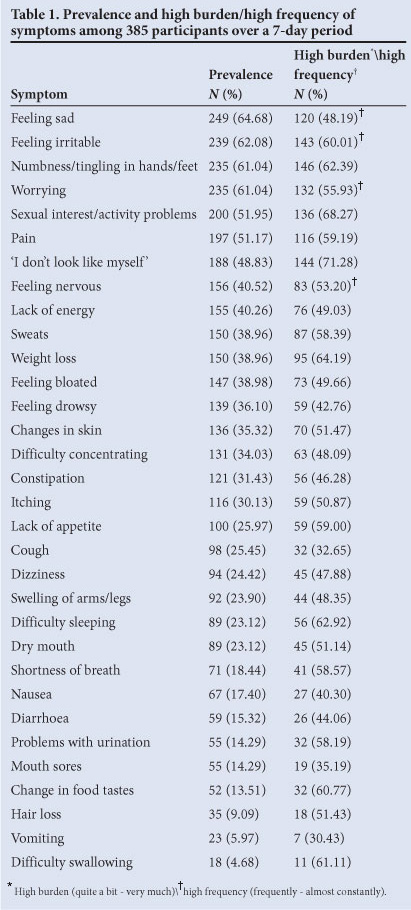
The median age of the sample was 40 years (Q1 - Q3=33 - 46) and 75.8% were women; 98.4% were receiving HAART, reflecting a busy urban HIV treatment clinic; the latest mean CD4 count was 355.06/mm3 (SD 219) and 271 had viral suppression at last viral load check. Participants were all included in the overall symptom prevalence and burden assessment. The inclusion of 7 participants not receiving HAART at the time did not significantly affect the prevalence and burden findings. All participants had at least 1 symptom. The mean number of symptoms of the 32 on the MSAS-SF experienced by participants was 10.24 (SD ±5.71, range 1 - 28). All 4 psychological symptoms (sad, irritable, worrying and feeling nervous) were among the 10 most prevalent symptoms, with feeling sad being the most prevalent. The high frequency (occurring frequently or almost constantly) of the psychological symptoms was over 48% for each of the 4 psychological symptoms, indicating a high burden. The most frequent 'high distress' ('quite a bit' or 'very much') response was generated by the physical symptom 'I don't look like myself', at 71% (Table 1).
Discussion
The mean number of symptoms experienced by our patients is similar to the MSAS-SF symptoms experienced by men in a UK survey, of whom over half were receiving HAART.3 Harding et al.3 found a similar profile of prevalent symptoms, the only marked difference being that in the UK study the participants had a greater frequency of difficulty sleeping, difficulty concentrating and feeling drowsy.3 An outpatient population study in London had a symptom profile similar to that of the UK survey and our study.2,3 The high prevalence and frequency of psychological symptoms is a notable finding of our survey and is supported by other studies among HIV patients,2,3 with symptoms distributed across psychological and physical domains, despite HAART. These findings highlight the importance of the comprehensive response of palliative care, described by the World Health Organization as 'impeccable assessment and treatment of pain and other distressing problems, physical, psychosocial and spiritual'.6 Pain was a common symptom in our study and others.2,3 Numbness or tingling in hands and feet was the most prevalent physical symptom and seems to indicate poorly controlled neuropathic pain. These and other symptoms require adequate acknowledgement and assessment, and appropriate, acceptable and effective treatment to prevent ongoing suffering.
The high prevalence and burden of symptoms experienced by our participants suggest inadequate symptom control. It highlights the palliative care needs of patients treated in outpatient clinics, of whom the vast majority are receiving HAART. Our findings strongly argue for palliative interventions for HIV patients 'in conjunction with other therapies that are intended to prolong life'.6 Extension of life without addressing quality of life is ethically unjustifiable. Palliative care aims to 'enhance quality of life, and may also positively influence the course of illness' by using 'a team approach to address the needs of patients and their families' and to treat for the 'relief from pain and other distressing symptoms'.6
A study assessing symptom prevalence and burden among cancer patients who were already receiving palliative care in SA and Uganda,5 found more symptoms among the advanced cancer patients than among the HIV-positive outpatients receiving HAART surveyed in our study. However, the relevance of the comparison is that the symptom profile of those cancer patients is similar to the symptom profile of the HIV-positive patients in the present study, showing that the symptoms of patients with HIV who receive outpatient HIV care are comparable with the symptoms of patients with advanced cancer, who are receiving palliative care.
Clinicians may be unaware of the applicability of palliative care in chronic disease,6 including for patients with HIV who attend outpatient treatment clinics. Our study and the 2 quoted from the UK, offer evidence that a palliative care approach and service must be included in routine HIV clinic care.2,3 If this is accepted, are treatment protocols for symptom management taught and are appropriate medications available to treat the symptoms arising?
More research is required to answer questions about whether we are negatively affecting HAART adherence by missing a possible connection between uncontrolled symptoms and HAART adherence, as suggested by international research.2
Acknowledgements
We thank participant patients, the management and staff of Wits Palliative Care, Chris Hani Baragwanath Hospital Ntabiseng Clinic, Helen Joseph Hospital Themba Lethu Right-to-Care Clinic, and Charlotte Maxeke johannesburg Academic Hospital HIV Clinic.
References
1. Fontaine A, Larue F, Lassauniere JM. Physicians' recognition of the symptoms experienced by HIV patients: how reliable? J Pain Symptom Manage 1999;18(4):263-270. [ Links ]
2. Harding R, Lampe FC, Norwood S, et al. Symptoms are highly prevalent among HIV outpatients and associated with poor adherence and unprotected sexual intercourse. Sex Transm Infect 2010. [ Links ]
3. Harding R, Molloy T, Easterbrook P, Frame K, Higginson IJ. Is antiretroviral therapy associated with symptom prevalence and burden? Int J STD AIDS 2006;17(6):400-405. [ Links ]
4. Harding R, Karus D, Easterbrook P, Raveis VH, Higginson IJ, Marconi K. Does palliative care improve outcomes for patients with HIV/AIDS? A systematic review of the evidence. Sex Transm Infect 2005;81(1):5-14. [ Links ]
5. Harding R, Selman L, Agupio G, et al. The prevalence and burden of symptoms amongst cancer patients attending palliative care in two African countries. Eur J Cancer 2011;47(1):51-56. [ Links ]
6. Sepulveda C, Marlin A, Yoshida T, Ullrich A. Palliative Care: the World Health Organization's global perspective. J Pain Symptom Manage 2002;24(2):91-96. [ Links ]
Accepted 23 January 2012.
Corresponding author: L Farrant (lindsaygfarrant@gmail.com)














