Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SAMJ: South African Medical Journal
versão On-line ISSN 2078-5135
versão impressa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.102 no.1 Pretoria Jan. 2012
FROM THE EDITOR
The job chooses the (wo)man
Some 1 200 - 1 300 new doctors have just graduated in South Africa. They will have begun their internships and in a year's time will commence their Community Service posts. Their thoughts will turn to their future occupations and to their choice of specialisation, including general practice or family medicine.
They may not appreciate that this choice is to some degree pre-ordained according to their personality traits. Psychiatrists, psychologists and behavioural scientists have developed a rich science of the link between personality and choice of specialty.1
Early qualitative surveys2 tested the notion of particular medical specialty personalities and provided some stereotypes: hardheaded, tough, outgoing surgeons, interested in things rather than people; reflective, tender-minded psychiatrists, with imaginative ideas and interested in people rather than things; and GPs deeply interested in people and with friendly and pleasing personalities.
Recently several more comprehensive psychological frameworks, some simple, some extremely complex, have been utilised to describe personality in doctors. The most simple is the Five-Factor Model (FFM) of personality, which posits five chief personality traits. Broadly they are neuroticism (a tendency to hostility, negativity, anxiety and depression); extroversion or sociability (encompassing warmth, gregariousness and assertiveness); openness to experience (finding expression in intellectual curiosity, being excited about new techniques and technologies, having independent judgement, and needing variety); agreeableness (predicting a pleasant, empathetic and accommodating demeanour); and conscientiousness (careful behaviour, dutifulness, self-discipline and an appreciation of strict rules and principles of practice).
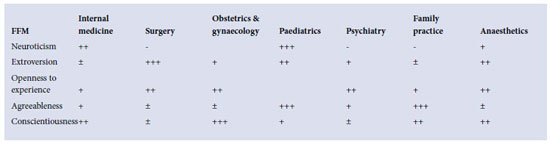
An extensive literature review3that sought to integrate the findings of many studies permits development of a simple table (below), revealing the association between these five main personality traits and the chief career domains. These personalities seem to fit the inherent natures of the jobs. Paediatricians, it can be argued, may naturally experience high levels of anxiety given their responsibility for small, often speechless, patients accompanied by worried ranks of family members. Obstetricians are required to be extra conscientious, arguably because they are responsible for two patients. Anaesthetists may not need to be highly sociable - their patients are unconscious during most of their contact time. Family practitioners are necessarily appropriately highly agreeable and conscientious. Psychiatrists have high emotional stability, which shows in their low neuroticism scores. The surgical stereotype, notable for having a big dominant personality and getting excited about new techniques, seems to be confirmed in high scores for extroversion and openness to experience.
The 'support' specialists in pathology and radiology are open to experience and reasonably agreeable, probably because they must interact with colleagues in all domains; interestingly, they score lowest in the neuroticism factor, perhaps because their role is to generate a report and leave it for the action and concern of clinicians.
Taking personality into account may also be helpful to medical school personnel responsible for student recruitment and admissions and may be of particular importance where schools set out to deliberately produce, say, primary care physicians, family practitioners, generalist physicians and geriatricians, and paediatricians.4 Back in 1986 it was suggested that the process of selecting medical students might be more rational if personality were taken into account.5 If the traits of extroversion, decisiveness, tolerance and service orientation were selected, a school could expect to educate doctors having a good fit for primary care and family practice. The authors advised that a school seeking to admit candidates who were most likely to pursue primary care career paths should preferentially recruit rural and female applicants (women score higher than men in extroversion, openness, agreeableness and conscientiousness2).
A good personality fit determines success and satisfaction within chosen fields.1 Doctors dissatisfied with their occupations are more prone to leave the profession altogether,6 while dissatisfaction with their initial choice causes many doctors to change specialties.7
As members of the so-called millennial generation, today's graduates are likely to factor financial reward, lifestyle preference and perceived prestige of a specialty into their choice. When settling upon their choice women, who outnumber men in current graduating classes, will also take into account running a home and raising a family.
Research continues into how personality serves as a prognosticator of specialty choice with a view to offering career advice and guidance and to enabling young doctors to choose a few specialties that might best suit their personalities. The final choice ought to be secure and happy for a career that will be typically 40 - 50 years long!

Janet Seggie
Deputy Editor
1. Maron BA, Fein S, Maron BJ, et al. Ability of prospective assessment of personality profiles to predict the practice specialty of medical students. Proceedings (Baylor University Medical Center) 2007;20:22-26. http://findarticles.com/p/articles/mi_6802/is_1_20/ai_n28408712/pg_3/2 (accessed 5 May 2011). [ Links ]
2. Borges NJ, Osmon WR. Personality and medical specialty choice: technique orientation versus people orientation. Journal of Vocational Behavior 2001;58:22-35 http://www.sciencedirect.com/science/article/pii/S0001879100917615 (accessed 30 May 2011). [ Links ]
3. Borges NJ, Savickas ML. Personality and medical specialty choice. Journal of Career Assessment 2002;10:362-380. http://jca.sagepub.com/cgi/content/abstract/10/3/362 (accessed 5 May 2011). [ Links ]
4. Markert RJ, Rodenhauser P, El-Baghdadi MM, et al. Personality as a prognostic factor for specialty choice: A prospective study of 4 medical schools classes. Medscape J Med 2008;10:4954. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2270893/ (accessed 5 May 2011). [ Links ]
5. Lazarus J, Van Niekerk JPdeV. Selecting medical students: a rational approach. Med Teach 1986;8:343-357. [ Links ]
6. Landon BE, Reschovsky JD, Pham HH, Blumenthal D. Leaving medicine: The consequences of physician dissatisfaction. Medical Care 2006;44:234-242. http://www.ncbi.nlm.nih.gov/ pubmed/16501394?dopt (accessed 21 October 2011). [ Links ]
7. Goldacre MJ, Lambert TW. Stability and change in career choices of junior doctors: Postal questionnaire surveys of the United Kingdom qualifiers of 1993. Med Educ 2000;34:700-707. http://www.ncbi.nlm.nih.gov/pubmed/10972747?dopt=Abstract (accessed 21 October 2011). [ Links ]