Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 no.11 Pretoria nov. 2011
ORIGINAL ARTICLE
Baseline chest radiographic features of HIV-infected children eligible for antiretroviral therapy
Vicci du PlessisI; Savvas AndronikouII; Gabriel StruckIII; Neil McKerrowIV; Aisne StokerV
IMB ChB, DA (SA), FCRad (Diag) SA. Department of Radiology, Nelson Mandela School of Medicine, University of Kwazulu-Natal, Durban
IIMB BCh, FCRad (Diag) SA, FRCR (Lon), PhD. Department of Radiology, University of the Witwatersrand, Johannesburg
IIIfourth-year medical student. Stony Brook University School of Medicine, New York, USA
IVBA, MB ChB, DCH (SA), FCPaed (SA), MMed (Paed), PG Dip Intl Res Eth. Department of Paediatrics, Nelson Mandela School of Medicine, University of Kwazulu-Natal
VMB ChB, DMRD (Lond), FRCR (Lon). Department of Radiology, Grey's Hospital, Pietermaritzburg
BACKGROUND: South Africa's HIV mortality is primarily due to pulmonary disease. No evidence exists regarding a correlation between specific chest radiographic patterns and CD4 levels of immunity in HIV-infected children.
OBJECTIVES: We aimed to determine the prevalence of specific radiographic features in HIV-infected children initiating antiretroviral therapy (ART) to develop a guideline of expected baseline radiographic appearances, and the radiographic features that predominate at specific levels of immune suppression (defined by CD4 percentage ranges), which would narrow the radiological differential diagnosis.
METHOD: Retrospective review of the baseline chest radiographs of 92 consecutive paediatric outpatients initiating ART.
RESULTS: Normal radiographs were reported in 54% of patients. Those with radiographic abnormalities had parenchymal disease (34%), mediastinal disease (22%) and pleural disease (1%). Parenchymal disease was predominantly air space (28%), and mediastinal disease was predominantly cardiomegaly (21%); lymphadenopathy was rare (1%). Radiological appearances of TB were seen in 9% of patients. A statistically significant association was shown between immune suppression and air space disease (p=0.049) with a relative risk of 0.46 (95% CI 0.24 - 0.88) for air space disease in immune-suppressed children. This association was independent of age.
CONCLUSION: Baseline chest radiographs in paediatric outpatients presenting for initiation of ART are predominantly normal, but also demonstrate a significant number of pathological radiological features - primarily air space disease and cardiomegaly. The only statistically significant association between radiographic features and immune suppression was air space disease, which correlated with a higher level of immunity
South Africa has the highest prevalence of human immunodeficiency virus (HIV) infection in the world, with KwaZulu-Natal Province at the epicentre of the epidemic.1-3 In 2009, 280 000 South African children <15 years old were infected with HIV.4-7 The primary cause of death is pulmonary disease, which is also the most common clinical feature of HIV.8
Chest radiographs are widely available and relatively inexpensive. In the assessment and management of acute and chronic disease in HIV-infected children, they provide an initial differential diagnosis,9 suggest the diagnosis of pulmonary tuberculosis (TB), detect extrapulmonary disease,10 provide a radiological baseline before initiation of antiretroviral therapy (ART), and monitor treatment response,11 including the development of immune reconstitution inflammatory syndrome (IRIS).
In adult patients, specific HIV-related infections and neoplasms occur within defined CD4 lymphocyte count ranges.12 There are no similar reports concerning HIV-infected children. Identification of pulmonary disease radiographic patterns within paediatric clinical and immunological HIV groups will assist the recognition of new disease, chronic disease, and diseases following the initiation of ART.
We aimed to determine the prevalence of specific radiographic features in HIV-infected children preparing to initiate ART so as to develop a guideline of expected baseline radiographic appearances; and the radiological features which predominate at specific levels of immune suppression, which could narrow the radiological differential diagnosis.
Materials and methods
A PubMed database search in March 2008 revealed no English-language articles relating specifically to the prevalence of radiographic patterns in children with HIV infection and correlating these with CD4 levels of immunity or clinical presentation.
The study was approved by the Biomedical Research Ethics Committee, University of KwaZulu-Natal in August 2009 (Ref: BE031/09).
We performed a retrospective review of the clinical records and baseline chest radiographs of 100 consecutive children presenting as outpatients for their first screening visit for initiation of ART from January to July 2009. The data were collected during August 2009 at a single site - the paediatric ART clinic at Edendale Hospital in Pietermaritzburg. The chest X-rays were reported by a paediatric radiologist, and the radiological findings compared with the baseline World Health Organization (WHO) clinical staging and immune status (CD4 lymphocyte results).
Patients included were those aged 6 months to 12 years who were referred to the paediatric ART clinic for initiation of ART. They were confirmed HIV-positive (on HIV antibody and/or virology testing) and deemed eligible for ART according to clinical and/or immunological criteria based on the 2006 WHO guidelines13 as follows:
• Recurrent hospitalisations (>2 admissions per year) for HIV complications or prolonged hospitalisation for HIV (>4 weeks)
OR
• Symptomatic children
• <1 year of age: WHO stage II, III and IV, or CD4 <;35%
• 1 - 5 years of age: WHO stage III and IV, or CD4 <;20%
• >5 years of age: WHO stage III and IV, or CD4 <15%.
Initial work-up and preparation at the ART clinic includes a baseline clinical assessment and staging, blood specimens for baseline CD4 levels, and a frontal chest X-ray to exclude TB.11
The WHO clinical staging system determines disease severity and eligibility for ART, particularly in resource-limited settings where CD4 testing is not available. Clinical stages are categorised as 1 - 4, progressing from primary HIV infection to advanced HIV/AIDS.
We classified patients according to their immune status, based on CD4 percentages according to the 1994 Revised HIV Paediatric Classification System14 as follows:
• >25% (no immune suppression)
• 15 - 24 % (moderate immune suppression)
• <15% (severe immune suppression).
Patients were excluded if the chest X-ray reference number was unrecorded, if the chest X-ray could not be located in the ART clinic or the filing room of the radiology department, or if the X-ray was of such poor technical quality that it could not be interpreted.
Chest radiographic findings were assessed by a paediatric radiologist according to a specified format that categorised findings into 3 main groups: mediastinal, pleural and parenchymal pathology. Mediastinal pathology included cardiomegaly and lymphadenopathy; pleural pathology included pleural fluid/thickening and pleural calcification; and parenchymal pathology included air space disease (focal and diffuse), cavities, nodules, bronchial disease, fibrocystic change and air trapping. The suspected presence or absence of pulmonary TB was also recorded.
The following were recorded: cardiomegaly if the cardiothoracic ratio was >60% in children <2 years of age, or >50% in children >2 years; lymphadenopathy if there were airway compression or deviation, or if there were lobulated masses extending beyond the cardiac or thymic shadow; pleural fluid/thickening if there were either linear lamellar densities along the lateral chest wall or blunted costophrenic angles; bronchial disease as either bronchiectasis (tramline or signet ring signs) or bronchial wall thickening with or without air trapping; air trapping as bilateral if >6 anterior ribs were visible at the mid-diaphragm, and as unilateral if the hemithoraces were asymmetrical in size and density in the absence of rotation; pulmonary TB in the presence of lymphadenopathy (with or without calcification), and/or nodular disease (miliary or larger), and/or cavitation (including bronchiectasis).
The reporting radiologist was blinded to the clinical and immunological data by performing the radiographic interpretation independently of clinical and immunological data collection.
Statistical analysis
Frequencies are described as a number and/or percentage. Descriptive statistics (frequencies and cross tabulations - Pearson's chi-square test and relative risk analysis) were conducted using SPSS Statistics 17.0 for Windows (SPSS, Chicago, IL). Mantel-Haenszel stratified relative risk was calculated in Epi Info version 3.4.3 (CDC).
Results
Of the 100 children, a total of 92 were included in the study (radiographs of 6 were missing and 2 were of inadequate technical quality for interpretation). Ages ranged from 6 months to 12.8 years (median age 4.6 years; mean age 5.4 years); 9 (10%) were <12 months, 41 (45%) were 1 - 5 years, and 42 (46%) were 6 - 12 years; 49 (53%) were boys and 41 (45%) were girls (2 unrecorded).
Clinically, of the total, 11 (12%) were WHO classification stage I, 7 (8%) stage II, 51 (55%) stage III, and 23 (25%) stage IV HIV. Immunologically, 16 (19%) were not immune-suppressed (CD4 % >25%), 31 (36%) had moderate immune suppression (CD4 %: 15 -24%) and 39 (45%) were severely immune-suppressed (CD4 % <15%) (CD4% of 6 children was unrecorded).
Fifty (54%) children had normal radiographs, of whom 7 (14%) were stage I, 1 (2%) stage II, 31 (62%) stage III and 11 (22%) stage IV HIV. Immunologically, 7 (14%) were not immune-suppressed, 21 (42%) had moderate immune suppression, and 19 (38%) were severely immune-suppressed (CD4 % results of 3 children unrecorded).
Forty-two (46%) had abnormal radiographs, of whom 4 (10%) were stage I, 6 (14%) stage II, 20 (48%) stage III, and 12 (29%) stage IV HIV. Immunologically, 9 (21%) were not immune-suppressed, 10 (24%) had moderate immune suppression, and 20 (48%) were severely immune-suppressed (CD4 % results of 3 unrecorded).
Chest radiographs revealed that 31 (34%) subjects had parenchymal disease, 20 (22%) mediastinal disease, and 1 (1%) had pleural disease. Parenchymal disease was predominantly air space disease - 26 (28%). Focal air space disease was present in 14 patients, diffuse air space disease in 12, and air trapping and bronchial disease in 9 (10%) and 6 (7%) patients respectively. Mediastinal disease (predominantly cardiomegaly) was seen in 19 (21%). Lymphadenopathy was seen in only 1 patient (1%). Radiological appearances of TB were reported in 8 (9%) patients - all of whom were in the more severe clinical categories (WHO stages III and IV), and two-thirds had severe immune suppression immunologically.
Table I summarises relevant radiographic features according to the level of immune suppression.
Pearson's chi-square analysis showed no statistically significant association between the presence or absence of radiological findings and clinical staging (p=0.104) or level of immune suppression (p=0.177).
The only radiographic finding with a statistically significant association with immune suppression was air space disease (p=0.049), which was even more significant (p=0.029) when the immune suppression categories were grouped into present (moderate or severe immune suppression) and absent (no immune suppression). The relative risk (RR) of air space disease in those with immune suppression v. those without immune suppression was 0.46 (95% CI 0.24 -0.88), which implies that the presence of air space disease correlates with a higher level of immunity (or conversely that radiographic air space disease is less likely to be seen in patients with moderate or severe immune suppression).
Stratified analysis of immune suppression and air space disease by age group revealed similar trends within all 3 age groups. The Mantel-Haenszel adjusted RR for the association between air space disease and immune suppression (adjusted for age group) was 0.42 (95% CI 0.23 0.76), confirming that this finding was independent of age.
Pearson's chi-square analysis also showed statistically significant associations between age and level of immune suppression (p=0.027), presence of radiographic abnormalities (p=0.039), parenchymal disease (p=0.036), air space disease (p=0.031), and radiographic TB (p=0.034). A larger proportion of immune-suppressed children were in the 6 - 12 years age group (85% of the group were immunesuppressed) compared with the other age groups. This may represent the criteria for qualification for ART which defined our sample population (children >5 years qualify for ART when CD4 <15%, i.e. severe immune suppression). The presence of radiographic abnormalities, parenchymal disease and air space disease were also more predominant in the 6 - 12 years age group. All 8 (100%) of the patients with suspected TB were in the 6 - 12 years age group.
Table II summarises relevant radiographic features according to age group.
Of the 31 patients with parenchymal disease on chest radiograph, 24 (77%) had history of a cough (>2 weeks), 20 (65%) had experienced weight loss, 24 (77%) had a history of fever, 27 (87%) had faltered in growth, 14 (45%) had cervical lymphadenopathy, and 14 (45%) had a diagnosis of pulmonary TB (all of whom were on anti-tuberculous treatment).
Of the 8 patients with radiographic features suggestive of TB, 3 had a confirmed diagnosis of pulmonary TB and were on TB treatment (at the time of the baseline chest radiograph); all 8 had history of a TB contact and cough; 4 had a history of weight loss; one had cervical lymphadenopathy. All patients were in the 6 - 12 years age group.
Discussion
Prevalence of specific radiographic features: expected baseline radiographic appearances
Baseline chest radiographs in paediatric outpatients presenting for initiation of ART are predominantly normal (54%), but also demonstrate a significant number of pathological radiological features (46%).
Pulmonary disease is the most common clinical presentation of HIV in infants and children.8 This correlated well with our results, which demonstrated pulmonary parenchymal disease to be the most common (34%) pathological radiological finding. Air-space disease was seen in nearly a third of patients.
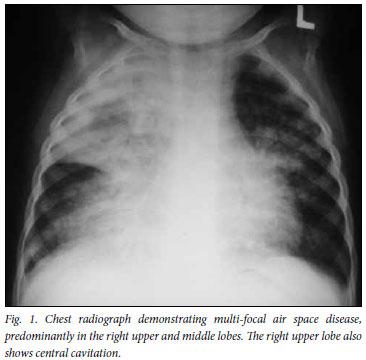
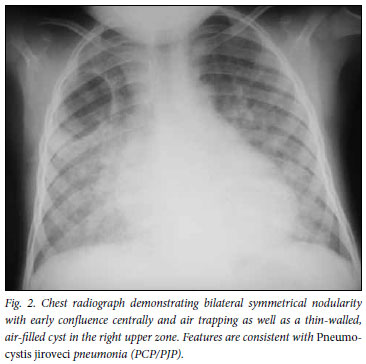
Respiratory infections are the most common cause of pulmonary change on the chest radiographs of HIV-infected children.10 These include bacterial or viral pneumonias, Pneumocystis jiroveci pneumonia (PCP/PJP), or tuberculosis. Bacterial pneumonia typically presents as lobar or segmental consolidation with air bronchograms (Fig. 1).8,15 Diffuse, bilateral 'ground-glass' or alveolar pulmonary opacification (air space disease), which may show some asymmetry, has been consistently documented as the most common radiographic finding in childhood PCP (Fig. 2).16
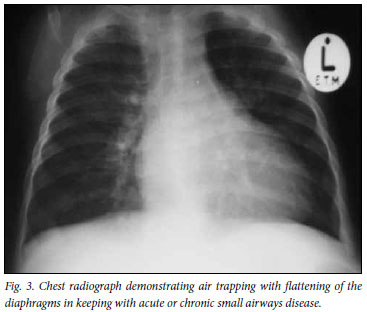
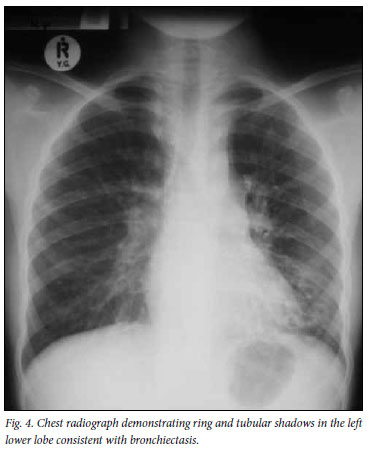
Air trapping and bronchial disease were also prominent features, demonstrated in 10% and 7% of patients respectively (Figs 3 and 4). Bronchiectasis in children who are HIV-infected may occur as a result of recurrent or unresolved pneumonia, as a complication of lymphocytic interstitial pneumonitis (LIP), after aspiration, or as a result of pulmonary TB.17
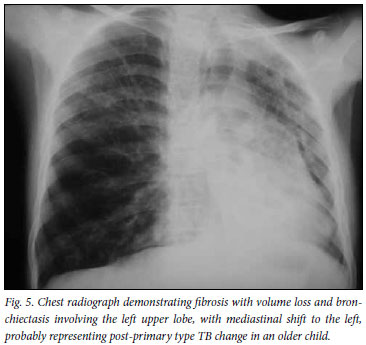
Radiographic features suggestive of TB were present in less than a tenth of patients (Fig. 5). There were 8 radiographs reported as having features of TB, with only one of these demonstrating lymphadenopathy. Although the conventional radiological hallmark of primary tuberculosis in childhood is hilar and/or mediastinal lymphadenopathy with or without concomitant pulmonary disease,18,19 recent studies have shown that, in the setting of HIV infection, classical imaging patterns do not always apply and atypical disease patterns occur.20
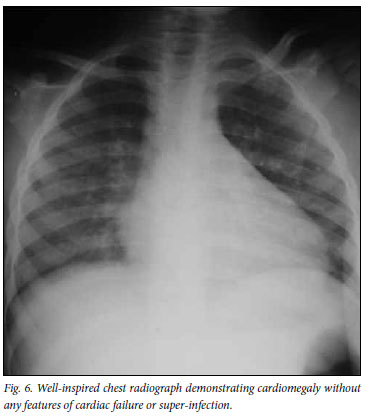
Cardiomegaly was the second most prevalent abnormality (21% of patients) (Fig. 6). Cardiac disease in HIV-infected children is most commonly due to dilated cardiomyopathy with biventricular chamber enlargement.8 Most (25 - 40%) HIV-related heart disease is a primary myopathic abnormality. Cardiac enlargement in HIVinfected children may also be due to primary pulmonary pathology, HIV-related obstructive pulmonary vascular disease in the absence of lung disease, pericardial disease, or anaemia.10
Lymphadenopathy and pleural disease (1% respectively), were rare findings in our cohort of children presenting for initiation of ART.
Comparison: radiographic features and level of immune suppression
In HIV-infected adults, specific HIV-related infections and neoplasms have occurred within defined CD4 lymphocyte count ranges, which aids in narrowing the radiological differential diagnosis.12 We attempted to determine whether certain radiographic features predominate at specific levels of immune suppression in paediatric patients.
We found no association between immune suppression and collective radiological findings. The only specific radiological feature that correlated statistically with the level of immune suppression was air space disease. This was a negative association, and was independent of age. The presence of air space disease correlated with a higher level of immunity. This implies that patients with immune suppression are less likely to demonstrate parenchymal air space disease than those who are immune-competent. We postulate that this may be due to the decreased ability of the patient's immune system to mount an immune response.
The high incidence of TB in HIV-infected children is due to their vulnerability to progress to disease and their increased risk of exposure. The risk of TB increases with severe immune suppression: a 4 times higher risk in children with CD4 % <15% than in those with CD4 % >15%.21 This trend was shown in our study population: of the patients with radiographic features of TB, two-thirds were severely immune-suppressed, and all had clinically severe disease (WHO stages III and IV).
There was no statistically significant association between cardiomegaly and immunity, implying that HIV cardiomyopathy is not unique to a specific level of immune suppression.
Older children (>6 years) showed a higher tendency to be immune-suppressed compared with their younger counterparts. As mentioned previously, this may be due to the criteria that qualify older children for ART (CD4 <15%, i.e. severe immune suppression). When radiographic findings were analysed according to participant age categories, older children consistently showed a higher incidence of collective radiographic findings, parenchymal disease, air space disease, and presence of radiographic TB.
Role of the chest X-ray in ART management
Decision-making about initiating ART is particularly important for children <12 months old as the mortality rate in untreated HIV-infected infants is high - up to a third die in the first year.13,22 Studies demonstrate that early initiation of ART in infancy and in children with advanced disease dramatically reduces the risk of mortality and disease progression.22,23 The WHO has consequently updated the recommendations regarding the optimal time for initiation of ART, advocating treatment of HIV-positive infants regardless of CD4 count/percentage.
According to the current national guidelines, eligibility for the initiation of ART in confirmed HIV-positive children >1 year old is dependent on clinical and immunological criteria, i.e. clinical staging (according to the WHO classification), and immune status (according to the gold standard - CD4 lymphocyte count/percentage).24
South Africa's paediatric ART programme is the largest in the world.25 Nevertheless, in 2009, less than 70% of the estimated number of South African children in need of ART were actually receiving it.7 In resource-constrained settings, the WHO recommends the use of clinical parameters with or without total lymphocyte count to facilitate universal access to ART and enable children to receive treatment even when CD4 results are not available.13
However, studies disagree regarding the association between the WHO classification of HIV-associated clinical disease and CD4 cell count.26-29 Furthermore, absolute lymphocyte count (which is a less technical laboratory investigation to perform) does not always correlate with severe immune suppression, which is based on CD4 cell count.30 The chest radiograph therefore plays an inevitable role in decisionmaking while developing countries try to cope with the demands for wider CD4 count testing and more reliable ways to confirm or exclude the diagnosis of tuberculosis. Our study suggests caution when interpreting baseline chest X-rays before initiating ART. The majority of baseline chest X-rays are normal. There is no correlation between radiological findings and level of immune suppression, and there is a paradoxical, inverse relationship between immune suppression and radiographic air space disease. Therefore, the chest X-ray is not an accurate tool in determining a patient's level of immunity.
Baseline chest radiographs are, however, essential as a comparative tool, allowing monitoring of improvement or progression of disease as an indication of treatment response. The initial chest X-ray is also used to exclude pulmonary TB (in conjunction with clinical findings and laboratory tests). This is important as the co-management of TB and HIV is complicated by drug interactions between ART and antituberculosis drugs, as well as the development of IRIS. Therefore, although chest radiographs should not be used as a surrogate for immunological testing to determine eligibility for ART, knowledge of radiographic patterns of disease in children eligible to start ART is useful for making other management decisions, especially in environments where laboratory testing is limited.
Study limitations
The limitations of this study include the retrospective study design, the small sample size, and the selected inclusion/exclusion criteria (lack of randomisation). Of importance is the inability to measure inter- and intra-observer variation in radiological interpretation owing to the use of a single observer and a single observation. Bias is inherent in a retrospective medical record review owing to the varying quality of recorded information that may limit the accuracy of the accumulated data and lead to under- or over-estimates. The population sample size was limited by time constraints. Owing to feasibility, only chronically ill outpatients were included. Respiratory pathologies affecting acutely ill (hospitalised) patients were therefore not represented. These factors, and the limited sample size, hindered stratification and generalisability. Correlation between the chest radiographic findings and final diagnosis was not performed, but is a future research prospect.
Despite the limitations, this study correlated well with previous studies21,31 in demonstrating that, as the CD4 percentage decreases in HIV-infected children, there is both an increased risk of developing TB as well as a decreased ability to mount an immunological response and produce a radiographic abnormality (in our case, air space disease). In addition, the study has illustrated that a wide range of baseline chest radiographic appearances exists at initiation of ART, thereby providing a platform for further research, particularly regarding IRIS.
Conclusion
Baseline chest radiographs in paediatric outpatients presenting for initiation of ART are predominantly normal, but also demonstrate a significant number of pathological radiological features, primarily air space disease and cardiomegaly. The only statistically significant association between radiographic features and immune suppression was air space disease, which correlated with a higher level of immunity, and was independent of age. Although the chest X-ray is not an accurate tool in determining a patient's level of immunity, baseline chest radiographs are vital in excluding pulmonary tuberculosis before initiation of ART, and for monitoring treatment response.
Acknowledgement. The authors thank Jaco du Plessis and Tonya Esterhuizen for assistance with data entry and statistical analysis respectively.
References
1. Zanoni BC. Epidemiology of HIV in Southern Africa. Pediatr Radiol 39:538-540. [ Links ]
2. The National HIV and Syphilis Prevalence Survey: South Africa 2007. Pretoria: National Department of Health, 2008. [ Links ]
3. Rollins N, Little K, Mzolo S, Horwood C, Newell M. Surveillance of mother-to-child transmission prevention programmes at immunization clinics: the case for universal screening. AIDS 2007;21:1341-1347. [ Links ]
4. Noble R. South Africa: HIV & AIDS Statistics. AVERT http://www.avert.org/safricastats.htm (accessed 31 March 2010). [ Links ]
5. UNAIDS/WHO Working Group on Global HIV/AIDS and STI Surveillance. UNAIDS/WHO Epidemiological Fact Sheets on HIV and AIDS, 2008 Update. WHO UNAIDS UNICEF http://www.who.int/globalatlas/predefinedReports/EFS2008/full/EFS2008_ZA.pdf. (accessed 31 March 2010). [ Links ]
6. UNAIDS. Report on the global AIDS epidemic. http://www.unaids.org/en/KnowledgeCentre/HIVData/GlobalReport/2008/2008_Global_report.asp (accessed 31 March 2010). [ Links ]
7. StatsOnline. P0302 -Mid-year population estimates. http://www.statssa.gov.za/Publications/statsdownload.asp?PPN=P0302&SCH=4437 (accessed 31 March 2010).
8. Marks MJ, Haney PJ, McDermott MP, White CS, Vennos AD. Thoracic disease in children with AIDS. RadioGraphics 1996;16:1349-1362. [ Links ]
9. King LJ, Padley SPG. Imaging of the thorax in AIDS. Imaging 2002;14:60-76. [ Links ]
10. Pitcher R, Goddard E, Hendricks M, Lawrenson J. Chest radiographic pulmonary changes reflecting extrapulmonary involvement in paediatric HIV disease. Pediatric Radiology 2009;39:565-568. [ Links ]
11. McKerrow NH, Naidoo KL, Reddy R, Stephen CR. Step-by-step Guide for the Management of Children on ART. 3rd ed. Durban: Department of Health: KwaZulu-Natal, February 2008. [ Links ]
12. Shah RM, Kaji AV, Ostrum BJ, Friedman AC. Interpretation of chest radiographs in AIDS patients: usefulness of CD4 lymphocyte counts. RadioGraphics 1997;17:47-58. [ Links ]
13. Antiretroviral therapy of HIV infection in infants and children in resource-limited settings: towards universal access, Recommendations for a public health approach; 2006 www.who.int/hiv/pub/guidelines/WHOpaediatric.pdf (accessed 31 March 2010). [ Links ]
14. Caldwell MB, Oxtoby MJ, Simonds RJ, Lindegren ML, Rogers MF. 1994 Revised classification system for human immunodeficiency virus infection in children less than 13 years of age. MMWR 1994;43:1-10. [ Links ]
15. Donnelly LF. Fundamentals of Pediatric Radiology. 1st ed. Philadelphia, USA: WB Saunders, 2001:3,47-54. [ Links ]
16. Pitcher RD, Zar HJ. Radiographic features of paediatric pneumocystis pneumonia - a historical perspective. Clinical Radiology 2008;63:666-672. [ Links ]
17. Theron S, Andronikou S, George R, et al. Non-infective pulmonary disease in HIV-positive children. Pediatric Radiology 2009;39:555-564. [ Links ]
18. Leung AN, NL Müller, Pineda PR, Fitzgerald JM. Primary tuberculosis in childhood: radiographic manifestations. Radiology 1992;182:87-91. [ Links ]
19. Andronikou S, Wieselthaler N. Imaging for Tuberculosis in Children. In: Schaaf HS, Zumla A (eds). Tuberculosis - A Comprehensive Clinical Reference. 1st ed. Philadelphia, USA: Elsevier, 2009:261-295. [ Links ]
20. Andronikou S, Vanhoenacker FM, De Backer AI. Advances in imaging chest tuberculosis: blurring of differences between children and adults. Clin Chest Med 2009;30:717-744. [ Links ]
21. Marais BJ, Rabie H, Schaaf SH, Cotton MF. Common opportunistic infections in HIV-infected infants and children, Part 1 - respiratory infections. SA Family Pract 2006;48:52-57. [ Links ]
22. Antiretroviral therapy for HIV infection in infants and children: Towards universal access, Recommendations for a public health approach, 2010 revision. http://whqlibdoc.who.int/publications/2010/9789241599801_eng.pdf (accessed July 2011). [ Links ]
23. Violari A, Cotton M, Gibb DM, et al. Early antiretroviral therapy and mortality among HIV-infected infants. N Engl J Med 2008: 359:2233-2244. [ Links ]
24. Guidelines for the Management of HIV in Children, 2nd ed. Pretoria: National Department of Health, 2010. http://www.health-e.org.za/documents/35cc37337b5448b6d06f48440fb424cc.pdf (accessed 30 July 2011). [ Links ]
25. Davies M, Keiser O, Technau K, et al. Outcomes of the South African National Antiretroviral Treatment Programme for children: the IeDEA Southern Africa collaboration. S. Afr Med J 2009;99:730-737. [ Links ]
26. Torpey K, Lartey M, Amenyah R, et al. Initiating antiretroviral treatment in a resource-constrained setting: does clinical staging effectively identify patients in need? Int J STD AIDS 2009;20:395-398. [ Links ]
27. McGrath N, Kranzer K, Saul J, et al. Estimating the need for antiretroviral treatment and an assessment of a simplified HIV/AIDS case definition in rural Malawi. AIDS 2007;21 Suppl 6:S105-113. [ Links ]
28. Teck R, Ascurra O, Gomani P, et al. WHO clinical staging of HIV infection and disease, tuberculosis and eligibility for antiretroviral treatment: relationship to CD4 lymphocyte counts. Int J Tuberc Lung Dis 2005;9:258-262. [ Links ]
29. Edathodu J, Ali B, Alrajhi AA. CD4 validation for the World Health Organization classification and clinical staging of HIV/AIDS in a developing country. Int J Infect Dis 2009;13:243-246. [ Links ]
30. Johnson OO, Benjamin DK, Benjamin DK Jr, et al. Total lymphocyte count and World Health Organization pediatric clinical stage as markers to assess need to initiate antiretroviral therapy among human immunodeficiency virus-infected children in Moshi, Northern Tanzania. Pediatr Infect Dis J 2009;28:493-497. [ Links ]
31. Norton KI, Kattan M, Rao JS, et al. P2C2 HIV Study Group. Chronic radiographic lung changes in children with vertically transmitted HIV-1 infection. Am J Roentgenol 2001;176:1553-1558. [ Links ]
Accepted 19 August 2011.
Corresponding author: V du Plessis (vicciduplessis@gmail.com)














