Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 no.10 Pretoria oct. 2011
ORIGINAL ARTICLES
Is the attendance of paediatricians at all elective caesarean sections an effective use of resources?
Lloyd J TookeI; Yaseen JoolayII; Alan R HornIII; Michael C HarrisonIV
IMB ChB , FCPaeds, MMed (Paeds), Cert Neon (SA). Neonatal Department, Groote Schuur Hospital and University of Cape Town
IIMB ChB, FCPaeds, Cert Neon (SA). Neonatal Department, Groote Schuur Hospital and University of Cape Town
IIIMB ChB, DCH, FCPaed (SA), Cert Neon (SA). Neonatal Department, Groote Schuur Hospital and University of Cape Town
IVMB ChB, FRCPCH (UK). Neonatal Department, Groote Schuur Hospital and University of Cape Town
ABSTRACT
OBJECTIVES: To determine the need for resuscitation at the birth of babies delivered by elective caesarean section (CS) and to record the time spent by doctors attending such deliveries.
METHODS: Data were collected prospectively on all elective CSs performed at Groote Schuur Hospital over a 3-month period. Data collected included: total time involved for paediatrician from call to leaving theatre, management of infant (requiring any form of resuscitation), Apgar scores and neonatal outcome (e.g. admission to nursery). The CSs were classified as low-risk or high-risk (multiple pregnancy, prematurity, growth restriction, abnormal lie, general anaesthetic or known congenital abnormality).
RESULTS: Data were recorded for 138 deliveries. Three were excluded as they were not elective CS. One hundred and fifteen deliveries were classified as uncomplicated and 20 as high-risk. Only 1 of the babies born from the 115 low-risk CSs needed brief resuscitation, whereas 9 of the 20 high-risk deliveries resulted in newborn resuscitation. The reasons for low-risk CS were: previous CS (81); infant of diabetic mother (IDM) and previous CS (16); IDM alone (6); estimated big baby (10); and other (2).The average time spent at each elective CS by the paediatrician was 37 minutes.
CONCLUSIONS: For low-risk CS, the same medical attendance (i.e. a midwife) as for an uncomplicated normal vaginal delivery (NVD) would be appropriate; this can free a doctor for other duties, and assist in de-medicalising a low-risk procedure.
Newborn resuscitation has an interesting and colourful history which stretches back hundreds of years. However, until the middle of the 20th century, there were very few effective techniques, and this sometimes led to desperate and often bizarre methods to attempt to revive the neonate. Some 19th century methods were swinging the baby upside-down (Schulz swinging); rhythmic traction of the tongue (the Laborde method); tickling the chest, mouth or throat; yelling; shaking; dilating the rectum using a raven's beak or a corn cob; electric shocks; nebulisation with brandy mist; and insufflation of tobacco smoke into the rectum.1 Fortunately, these have long since been abandoned.
Even though paediatrics became a specialty in 1930, it was only from the 1970s that paediatricians, and later neonatologists, became actively involved with the care of newborns and their resuscitation. By the 1980s, resuscitation guidelines had been drawn up in the UK and the USA, and there was active training of doctors and midwives in newborn resuscitation.1
Some would argue nowadays that paediatricians are over-involved in the care of newborns, especially low-risk infants.2 This trend could lead to over-medicalisation of the birth procedure, with unnecessary procedures such as suctioning the baby's airways or use of medications such as oxygen. These procedures, although seemingly relatively innocuous, might harm the baby.
Vaginal deliveries in labour wards are usually attended by a midwife, with only the complicated deliveries or high-risk babies requiring a paediatrician to be present. It has, however, become a standard of care in most South African hospitals for a paediatrician to be present at all caesarean section (CS) deliveries, both emergency and elective, as these are seen as high-risk deliveries. This is the case despite several studies from the developed world demonstrating that the need for resuscitation after an uncomplicated elective CS delivery is equivalent to, or even less than, that needed for a vaginal delivery. They conclude that elective CSs under regional anaesthesia are low-risk deliveries and do not require the presence of experienced paediatric medical staff.3-7
If these recommendations were followed, scarce medical resources could be redeployed more effectively as doctors would not be tied up in theatre for long periods. We decided to determine whether we could make similar recommendations for our population of babies.
Subjects and methods
Groote Schuur Hospital (GSH) is a tertiary teaching hospital in Cape Town. About 5 800 deliveries a year take place, with 1 - 4 elective CSs every weekday.
Data were collected prospectively on all elective (non-emergency) CSs performed at GSH from March - May 2010. The attending paediatricians were trained to complete a structured pro forma. Data included: reason for CS, other relevant history, type of anaesthetic, total time involved for paediatrician from call to leaving theatre, management of infant (including the amount and type of resuscitation), Apgar scores and neonatal outcome (baby admitted to the nursery or stay with the mother).
Data sheets were collated into an Excel spreadsheet and divided into complicated or uncomplicated (low-risk) deliveries. Complicated deliveries included any of the following: multiple pregnancies, low birthweight <2 kg, prematurity <36 weeks, general anaesthetic, abnormal lie (e.g. breech), and known congenital abnormality.
Babies who needed any resuscitation or were admitted to the nursery were then further reviewed by obtaining both their and their mother's folders.
Ethical approval for this study was obtained from the GSH research ethics committee.
Results
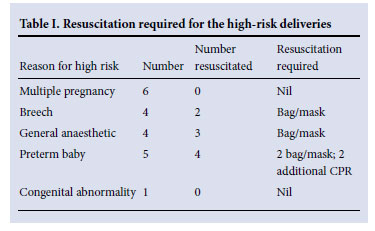
Data were collected for 138 elective CS deliveries, 3 of which were emergency CS and were excluded, leaving 135 deliveries. Twenty deliveries did not fit the criteria for uncomplicated CS, the reasons being: multiple pregnancies (6 - of which 5 sets of twins, 1 set of triplets); prematurity less than 36 weeks (5); general anaesthetic (4); abnormal lie (4 - all breech); and significant congenital abnormality (1- situs inversus totalis). Nine of these infants required resuscitation; 7 of them required bag-mask ventilation, with the other 2 also receiving CPR (Table I).
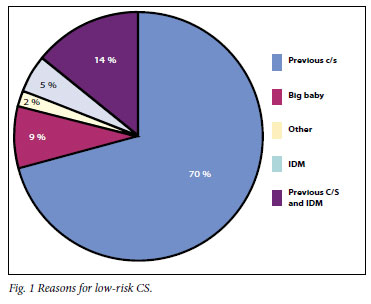
The remaining 115 deliveries were low-risk (Fig. 1). The reasons for low-risk CS were: previous CS (81); infant of diabetic mother (IDM) and previous CS (16); IDM alone (6); estimated big baby (10); and other (2).
Only 1 low-risk infant out of a total of 115 deliveries required moderate resuscitation with bag and mask for a short period, and did not require admission to the nursery. This CS was done because of a previous CS.
The average time spent at each elective CS by the paediatrician was 37 minutes. This did not include time answering their bleeper/phone or walking to theatre.
Discussion
We aimed to determine the need for resuscitation at elective CS. Our findings are similar to other studies: uncomplicated CS is a safe delivery for the baby with little need for resuscitation. However, once there was a complicating factor making the CS higher risk (multiple pregnancy, low birthweight <2 kg, prematurity <36 weeks, general anaesthetic, abnormal lie; or known congenital abnormality), the resuscitation rate was 45%.
For those concerned about the rare unexpected resuscitations that are bound to happen at some point - as they would in labour ward - a paediatrician could be called. Midwives should be properly skilled to begin resuscitation.
Many (22 out of 115) low-risk infants were exposed to maternal diabetes. Babies delivered by elective CS are at higher risk ofrespiratory complications,8,9 which risk is increased by maternal diabetes.10 Although these IDMs were often admitted to the nursery for glucose monitoring and respiratory distress syndrome, we found that maternal diabetes did not increase the need for resuscitation, with none of these babies needing resuscitation at birth.
Unlike in developed nations, the risk of unexpected pre-term delivery is greater in settings like ours where early ultrasound scans are seldom performed to determine gestational age. However, there is as much risk of this also happening in a labour ward, and we felt that this was not a good reason for having a doctor at all elective CSs.
We intend to implement our recommendations and do a follow-up study to determine whether babies are compromised in any way by the new practice.
In summary, we argue that it would be appropriate to have the same kind of medical attendance for an uncomplicated NVD as for a lowrisk CS, i.e. a midwife. Not only would this free up a doctor for other duties, but it would also assist in de-medicalising a low-risk procedure.
References
1. O'Donnell C, Gibson A, Davis P. Pinching, electrocution, ravens' beaks, and positive pressure ventilation: a brief history of neonatal resuscitation. P Arch Dis Child Fetal Neonatal Ed 2006;91:F369-F373. [ Links ]
2. Johanson R, Newburn M, Macfarlane A. Has the medicalisation of childbirth gone too far? BMJ 2002;324:892-895. [ Links ]
3. Gordon A, Mckechnie E, Jeffery H. Pediatric presence at caesarean section: Justified or not? Am J Obstet Gynecol 2005;193:599-605. [ Links ]
4. Atherton N, Parsons SJ, Mansfield P. Attendance of paediatricians at elective Caesarean sections performed under regional anaesthesia: is it warranted? J Paediatr Child Health 2006;42:332-336. [ Links ]
5. Gonzalez F, Juliano S. Is pediatric attendance necessary for all cesarean sections? JAOA 2002;102:127-129. [ Links ]
6. Parsons SJ, Sonneveld S, Nolan T. Is a paediatrician needed at all Caesarean sections? J Paediatr Child Health 1998;34:241-244. [ Links ]
7. Davies P, Miles R, Harrington J, Lawrence S. Which births are high risk?: Condition of neonates at birth and risk of intervention associated with type of delivery and thickness of meconium in the district general hospital setting. The Internet Journal of Pediatrics and Neonatology 2003, Vol 3 No 1. [ Links ]
8. Zanardo V, Simbi AK, Franzoi M, Solda' G, Salvadori A, Trevisanuto D. Neonatal respiratory morbidity risk and mode of delivery at term: influence of timing of elective caesarean delivery. Acta Paediatr 2004;93:643-647. [ Links ]
9. Kamath BD, Todd JK, Glazner JE, Lezotte D, Lynch AM. Neonatal outcomes after elective caesarean delivery. Obstet Gynaecol 2009;113:1231-1238. [ Links ]
10. Nold J, Georgieff M. Infants of diabetic mothers. Pediatr Clin N Am 2004;51:619-637. [ Links ]
Accepted 7 March 2011.
Corresponding author: L Tooke (lloyd.tooke@uct.ac.za)














