Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 n.9 Pretoria Sep. 2011
ORIGINAL ARTICLES
Newborn hearing screening in the private health care sector - a national survey
Miriam Elsa MeyerI; De Wet SwanepoelII
IBCommPath. Department of Communication Pathology, University of Pretoria
IIPhD. Department of Communication Pathology, University of Pretoria, and Callier Centre for Communication Disorders, University of Texas at Dallas, USA
ABSTRACT
OBJECTIVES: To determine: (i) the national status of newborn hearing screening services in the private health care sector of South Africa; (ii) screening approaches implemented; and (iii) challenges to screening implementation.
DESIGN: A descriptive quantitative national survey was conducted in the private sector of South Africa.
METHOD: All private health sector institutions with obstetric units (N=166) were surveyed telephonically and self-administered questionnaires were subsequently sent to all audiologists in private practice (N=87) who provide newborn hearing screening services at the units with hearing screening.
RESULTS: Nationally 53% of private sector obstetric units offer some form of newborn hearing screening. Universal hearing screening was only offered by 14% of units, while the most common approaches were universal screening on some days of the week (18%) and screening on request (18%). The most prominent challenge to successful screening implementation was the omission of newborn hearing screening from maternity birthing packages at the health care institutions.
CONCLUSION: The vast majority of newborns nationally are not screened for hearing loss, and existing programmes are not sufficiently systematic and integrated to ensure adequate coverage. Hospital management and paediatric health services must prioritise hearing screening as part of standard of care in birthing services.
Approximately 180 000 babies are born with or acquire permanent bilateral hearing loss (>40 dB hearing level (HL)) within the first few weeks of life across sub-Saharan Africa every year.1 In South Africa an estimated 17 babies are born with a significant permanent bilateral hearing loss every day.2 These infants can only be detected early enough for optimal intervention outcomes through widespread newborn and infant hearing screening programmes using objective (oto-acoustic emissions and auditory brainstem response screeners) screening technologies.2-7
Identification is considered late when children are diagnosed after 9 - 12 months of age and have missed access to auditory input during the critical language acquisition period in the first year of life.4,5,8 Late identification impedes language, psychosocial, emotional and cognitive development in early childhood, which undermines educational and vocational outcomes.1,3,4,5-9 The effect on quality of life for these children, who become isolated and stigmatised, is dramatic and severe.1,3,8 From an economic perspective the burden on families, communities and countries has led many countries, including Australia, Canada, the UK and the USA, to adopt universal newborn hearing screening programmes as standard practice in neonatal care.4,7,9 Many of these countries screen 95% and more of all babies for hearing loss within the first month of life.4,5,7,9
In South Africa infant hearing loss is primarily detected passively when parents become concerned about speech and language delays, and usually occurs after 2 years of age.2,8,10 The pervasive lack of systematic newborn hearing screening programmes across the country means that children with hearing loss suffer lifelong deficits in various developmental areas that are essentially preventable.1,2,10 A recent national survey of early hearing detection and intervention (EHDI) services in the public health sector, which service approximately 85% of the South African population,11 reported that only 7.5% of public sector hospitals nationally provide some form of neonatal or infant hearing screening and less than 1% provide universal screening.12 The survey estimated that more than 90% of babies born in South Africa do not have the prospect of early detection of hearing loss.12 To date, however, no national survey of newborn hearing screening services in the private health sector has been conducted.2,8
EHDI services for optimal outcomes are recommended to identify children with hearing loss before 1 month of age, to complete diagnostic assessments before 3 months of age, and to initiate intervention (amplification and language-based intervention) before 6 months of age.4-7 This can only be attained if the very first step, newborn hearing screening, is systematically employed and followed up appropriately.2,3 The current study conducted a national survey on the status of EHDI services in the private health care sector of South Africa.
Method
Population
A survey was conducted nationally in the private health care sector across all provinces of South Africa. The total population included all private health care hospitals or clinics that offer obstetric services and the audiologists in private practice (registered with the Health Professions Council of South Africa) who provide infant hearing screening services at these units. Ethical clearance was obtained before commencing the study.
All private health sector (non-government-funded) institutions in South Africa listed on www.medpages.co.za (2009) were contacted telephonically in order to determine whether the respective institution rendered obstetric services.13 There were 304 such institutions, including hospitals, clinics and private practices, listed for potential inclusion in the sample.13 After removing duplicated listings, 298 hospitals were contacted. Eight of these were not applicable to the current study because they were partially government funded and therefore not private sector institutions. Another three hospitals or clinics no longer existed as functioning private institutions, and one could not be reached after numerous calls to all documented numbers in the national telephone register.
All maternity and/or neonatal wards at those institutions that rendered obstetric services were surveyed, and questionnaires were subsequently sent to the audiologists who conducted hearing screening at the respective private sector institutions with hearing screening services. Participants who worked at more than one private institution were asked to complete one questionnaire per institution to ensure that data were representative for each respective hospital or clinic. The survey aimed: (i) to determine the estimated number of births at each institution; (ii) to find out whether newborn or infant hearing screening services were rendered; (iii) if hearing screening was offered, to find out what the nature of the service was (i.e. universal, parental or paediatrician request only, targeted or high-risk screening) and (iv) to identify the most significant challenges towards implementation of newborn hearing screening programmes.
Questionnaire
A self-administered questionnaire was sent out by e-mail or fax. The questionnaire consisted of several sections. The first section surveyed biographical information and the second information on work context and hearing screening practices. Subsequent sections covered data management and quality control, diagnostic protocols and intervention services and are not reported here.
Data analysis
Data collected from the telephonic survey with private hospitals and subsequent maternity wards were integrated with data collected from the questionnaire completed by audiologists at the specific institutions. The data were analysed to yield percentages and frequency distributions nationally and across provinces.
Results
Screening coverage
Of the 286 eligible private health care institutions, 120 (42%) did not render obstetric services. The remaining 166 institutions with obstetric units were surveyed, and 53% (87/166) reported some form of newborn hearing screening service. Questionnaires were subsequently sent to audiologists managing the screening programmes at these institutions to ascertain the nature of the services. A return rate of 89% (77/87) was achieved.
Reported estimates by the private health care institutions with obstetric units indicated that approximately 136 934 babies were born each year across these units in South Africa. Audiologists managing hearing screening at the units (87/166) were asked to indicate the number of babies screened monthly at the respective institutions. Reportedly, an estimated 39 564 babies are screened annually (3 297 per month) at the institutions for which responses were obtained (N=70). Compared with the reported number of estimated births at all private institutions with obstetric units, at least 29% of newborns born at private health care institutions are screened for hearing loss. Seven (9%) of the respondents did not complete this question because regular statistics of screenings were not documented.
Table I provides a breakdown of the estimated number of births and the reported availability and nature of newborn hearing screening services. The highest screening coverage was in the Western Cape and Gauteng provinces, where 72% and 66% of obstetric units respectively offered some form of hearing screening. In the Eastern Cape, the Free State, Mpumalanga and the Northern Cape, more than two-thirds of obstetric units do not offer any form of hearing screening.
Screening approaches
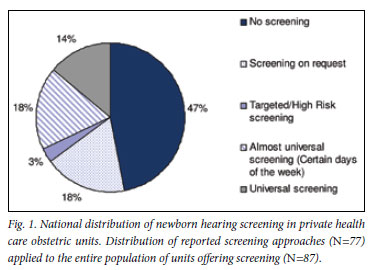
Applying the distribution of reported screening approaches (N=77) to the entire population sampled, i.e. including those who did not return the questionnaires (N=10), indicates that nationally only 14% of private health obstetric units offer universal hearing screening (Fig. 1). The two most common screening approaches are universal screening offered on certain days of the week only (18%) and screening on request (18%). A small number of units employed riskbased screening (3%) and reported a combination of methods to determine risk and subsequent need for screening. These included neonatal intensive care unit (NICU) admittance only, and risk factors listed by the Joint Committee of Infant Hearing (2007) and/ or the HPCSA Position Statement on Newborn and Infant Hearing Screening (2007).5,6
Challenges to implementation of newborn hearing screening
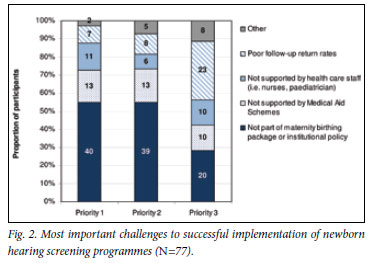
The three most important perceived challenges to successful implementation of newborn hearing screening in the private health care sector were prioritised by participants as illustrated in Fig. 2. Most prominently prioritised as the first (40%) and second (39%) most significant challenge was the apparent omission of newborn hearing screening from maternity birthing packages and institutional policy at the health care institutions. The small percentage of challenges listed under 'other' related mainly to test environment and procedural issues.
Discussion
This survey was the first to report the national status of newborn hearing screening services in the private health care sector of South Africa, which serves approximately 15% of the population.11 A similar survey in the public health sector of South Africa indicated that 7.5% of public birthing hospitals provide some form of newborn hearing screening and less than 1% offer universal newborn hearing screening.12 Screening in the private sector is more comprehensive, with 53% institutions with obstetric units offering some form of newborn hearing screening but only 14% offering true universal hearing screening. Being born in a unit that offers screening does not guarantee that a baby will be screened, since parents must indicate whether they agree to the service. Hearing screening is not included as an integrated part of maternity birthing services and is not covered by all medical aid schemes. The best practice recommendation for newborn hearing screening programmes is universal screening with coverage exceeding 95%.4,5,7 The current study demonstrates coverage rates for hearing screening in the private health sector that are significantly less than 50%.
Considering both the public and private health sectors, approximately 90% of newborns in South Africa will not be screened for hearing loss.12 Almost half of private health obstetric units nationally do not offer any form of hearing screening despite apparent world-class neonatal care. The estimated prevalence rate of permanent bilateral infant hearing loss in the private health care sector of South Africa is 3 in every 1 000 births.2 Based on the reported figures in this study, an estimated 411 babies will present with permanent bilateral congenital hearing loss annually in the private health care sector, of which 193 will be born in units without any hearing screening. The remaining babies, born in units where some form of screening is offered, may or may not be screened. The lack of systematic screening programmes means that the vast majority of babies with hearing loss go undetected until 2 - 3 years of age, as demonstrated by the initial age of diagnoses.2,10 By this stage critical developmental periods for language acquisition have passed, resulting in irreversible delays as opposed to developmental trajectories within normal ranges that are possible through early detection.2,4,7,14
The recommended hearing screening tests, which measure the integrity of the cochlea (oto-acoustic emissions) or of the auditory nerve and brainstem (auditory brainstem response), are simple, safe, inexpensive and can be completed within minutes.1,4,5,7 The screening can be conducted by trained nursing personnel with oversight and programme management by audiologists.4,14 Early identification of hearing loss is feasible, and its developmental, academic, vocational and economic benefits have been convincingly demonstrated over the past two decades.3,4,5,7,14 Newborn hearing screening should be part of neonatal standard of care, as is the case in the majority of developed countries of the world.2,4,8
The most frequently reported challenge to successful implementation of hearing screening in the private health care sector was the omission of newborn hearing screening from maternity birthing packages and institutional policy. As a result newborn hearing screening is not implemented or monitored systematically, but is dependent on individual initiatives without being an integrated part of routine neonatal care.2,8 Hospital management and paediatric services must prioritise hearing screening to include newborn screening as part of the birthing package services as opposed to being an optional extra, if available at all. Other secondary challenges to address include improving awareness among health care personnel regarding the importance of early identification and the comprehensive reimbursement of hearing screening services by medical aid schemes.
Conclusion
All children with hearing loss have the basic human right of access to human communication.14 The overwhelming majority of babies with hearing loss in South Africa will not be screened at birth, which leads to late identification and restricted developmental outcomes. Current screening programmes in private health care are not sufficiently systematic and integrated with birthing services to ensure adequate coverage. The successful implementation of these programmes is the first step towards optimal outcomes for affected individuals and lifelong savings for the family and the economy.1,2,4,7,8,9 Achieving this goal requires support from health care management and neonatal health providers.
References
1. Olusanya BO. Priorities for early hearing detection and intervention in sub-Saharan Africa. Int J Audiol 2008;47(Suppl. 1):S3-S13. [ Links ]
2. Swanepoel D, Störbeck C, Friedland P. Early hearing detection and intervention in South Africa. Int J Pediatr Otorhinolaryngol 2009;73:783-786. [ Links ]
3. Korver AMH, Konings S, Dekker FW, et al. Newborn hearing screening vs later hearing screening and developmental outcomes in children with permanent childhood hearing impairment. JAMA 2010;304(15):1701-1708. [ Links ]
4. Morton CC, Nance WE. Newborn hearing screening - a silent revolution. N Engl J Med 2006;354(20):2151-2164. [ Links ]
5. Joint Committee on Infant Hearing (JCIH). Year 2007 Position Statement: Principles and guidelines for early hearing detection and intervention programs. Pediatrics 2007;120:899-921. [ Links ]
6. Health Professions Council of South Africa. Professional Board for Speech, Language and Hearing Profession: Early Hearing Detection and Intervention Programmes in South Africa, Position Statement Year 2007: 1-42. http://www.hpcsa.co.za/downloads/speech_education/early_hearing_detection_statement.pdf (accessed 1 June 2011). [ Links ]
7. World Health Organization. Newborn and Infant Hearing Screening: current issues and guiding principles for action. Geneva: WHO Press, 2010:1-40. [ Links ]
8. Swanepoel D. Early detection of infant hearing loss in South Africa. S Afr Med J 2009;99(3):158-159. [ Links ]
9. Smith RJH, Bale JF, White KR. Sensorineural hearing loss in children. Lancet 2005;365:879-890. [ Links ]
10. Van der Spuy T, Pottas L. Infant hearing loss in South Africa: Age of intervention and parental needs for support. Int J Audiol 2008;47:S30-S35. [ Links ]
11. Blecher M, Harrison S. Healthcare financing. In: Ijumba P, Padarath A, eds. South African Health Review 2006. Durban: Health Systems Trust, 2006. www.healthlink.org.za/uploads/files/chap3_06.pdf (accessed 1 June 2011). [ Links ]
12. Theunissen M, Swanepoel D. Early hearing detection and intervention services in the public health sector in South Africa. Int J Audiol 2008;47(Suppl. 1):S23-S29. [ Links ]
13. Medpages (online): South African Health professionals directory. http://www.medpages.co.za/index.php?module=products&category=directory (accessed 30 August 2009).
14. Yoshinaga-Itano C, Thomson V. The work of the Village: Creating a new world for children with hearing loss and their families. Int J Audiol 2008;47(Suppl. 1):S14-S22. [ Links ]
Accepted 24 May 2011.
Corresponding author: D Swanepoel (dewet.swanepoel@up.ac.za)














