Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 n.9 Pretoria Sep. 2011
ORIGINAL ARTICLES
Nevirapine plasma concentrations in premature infants exposed to single-dose nevirapine for prevention of mother-to-child transmission of HIV-1
Pierre MugaboI; Ilse ElsII; Johan SmithIII; Helena RabieIV; Peter SmithVI; Mark MirochnickVII; Wilhelm SteynVIII; David HallIX; Richard MadsenX; Mark F CottonV
IMB ChB, MMed, PhD. School of Pharmacy, University of the Western Cape
IIIlse Els, MB ChB, FCP, MMed. Neonatal Services, Tygerberg Children's Hospital and Stellenbosch University, Tygerberg, W Cape
IIIMB ChB, MMed, FCP, PhD. Neonatal Services, Tygerberg Children's Hospital and Stellenbosch University, Tygerberg, W Cape
IVMB ChB, MMed, FCP, PGDipID. Children's Infectious Diseases Clinical Research Unit, Stellenbosch University
VMB ChB, MMed, PhD, FCPaed, DTM&H, DCH. Children's Infectious Diseases Clinical Research Unit, Stellenbosch University
VIBSc, BSc Hons, PhD. Department of Pharmacology, University of Cape Town
VIIMirochnick, MD. Department of Pediatrics, Boston University School of Medicine, Boston, Mass, USA
VIIIMB ChB, MMed, FCOG, MD. Department of Obstetrics and Gynaecology, Stellenbosch University and Tygerberg Hospital
IXMB ChB, DObst, FCOG, MMed, MD. Department of Obstetrics and Gynaecology, Stellenbosch University and Tygerberg Hospital
XAB, MS, PhD. Department of Statistics, University of Missouri, Columbia, Mo., USA
ABSTRACT
BACKGROUND: No pharmacokinetic data exist for premature infants receiving single-dose nevirapine (sd NVP) for prevention of mother-to-child transmission (MTCT) of HIV. Aim. To describe NVP decay pharmacokinetics in two groups of premature infants - those whose mothers either received or did not receive NVP during labour.
METHODS: Infants less than 37 weeks' gestation were prospectively enrolled. Mothers received sd NVP during labour if time allowed. Infants received sd NVP and zidovudine. Blood was collected on specified days after birth and NVP concentrations were determined by liquid chromatography-mass spectrometry.
RESULTS: Data were obtained from 81 infants, 58 born to mothers who received sd NVP during labour (group I) and 23 to mothers who did not receive NVP (group II). Of the infants 29.6% were small for gestational age (SGA). Median (range) maximum concentration (Cmax), time to reach maximum concentration (Tmax), area under the plasma concentration-time curve (AUC) and halflife (T½) were 1 438 (350 - 3 832) ng/ml, 25h50 (9h40 - 83h45), 174 134 (22 308 - 546 408) ng×h/ml and 59.0 (15.4 - 532.6) hours for group I and 1 535 (635 - 4 218) ng/ml, 17h35 (7h40 - 29h), 168 576 (20 268 - 476 712) ng×h/ml and 69.0 (22.12 - 172.3) hours for group II. For group II, the median (range) volume of distribution (Vd) and body clearance (Cl) were 1 702.6 (623.7 - 6 189.8) ml and 34.9 (6.2 - 163.8) ml/h. The AUC was higher (p=0.006) and Cl lower (p<0.0001) in SGA infants. Plasma concentrations exceeding 100 ng/ml were achieved over 8 days in 78% infants in group I and 70.0% in group II. The MTCT rate was 4.8%.
CONCLUSION: Women in preterm labour often deliver with little advance warning. Our study suggests that NVP dosing of preterm infants as soon as possible after birth without maternal intrapartum dosing may be as effective as combined maternal and infant dosing.
The mother-to-child transmission (MTCT) rate for HIV-1 is 15 - 40% in the absence of intervention, with most of the transmission occurring late in pregnancy or during labour and delivery.1,2 Treating HIV-infected pregnant women with combination regimens of potent antiretrovirals can reduce the rate of transmission to 1%.3 In resource-poor areas where antiretrovirals are not readily available, less intensive regimens, although less effective, still significantly reduce transmission.4
Nevirapine (NVP) is a non-nucleoside reverse transcriptase inhibitor that has a potent antiviral effect (inhibitory concentration (IC)50 of 10 ng/ml), rapid oral absorption, good bio-availability and a long half-life after an initial dose (46 hours following a single 200 mg tablet in adults), and crosses the placenta.5-8 Administering a single dose (sd) to the mother during labour and to the infant after birth reduces HIV transmission by around 40%.9,10 In term infants, this regimen maintained infant plasma NVP concentrations above 100 ng/ml (10 times the in vitro IC50) throughout the first week of life.11,12 While approximately 18% of births in lower income settings are premature, there are no data describing NVP pharmacokinetics in premature infants.12
Our aim was to describe NVP decay pharmacokinetics in two groups of premature infants: those whose mothers either received or did not receive NVP during labour.
Material and methods
Site and population
The study was conducted in the Neonatology Department at Tygerberg Children's Hospital from February 2005 to April 2009. Premature infants whose mothers were admitted during labour were eligible. Infant growth was classified as small (SGA), appropriate (AGA) or large for gestational age (LGA) using the Fenton chart.13 All infants were fed with either formula milk or pasteurised expressed breastmilk.
Inclusion criteria. Infants born to HIV-infected women before 37 weeks' gestation were eligible. The new Ballard score14 was primarily used to determine gestational age, and when it was not available, data from abdominal ultrasound scans or the date of the last menstrual period were used. Maternal HIV infection status was determined according to South African Department of Health programme guidelines, which are based on guidance from the World Health Organization.15 HIV-1 antibodies were detected by a rapid test and positive results were confirmed on a second assay from a different manufacturer. Informed consent was obtained from the women enrolled and, when available, from the fathers.
Exclusion criteria. Infants were excluded if their mothers were on long-term NVP or other antiretrovirals, or receiving any drug known to interfere with NVP absorption, metabolism and distribution; on request by the mother; or if the infant's haematocrit was below 30%. If the haematocrit fell below 24% during the study, blood sampling was deferred until the haematocrit was higher than 24%.
Procedures
Mothers received 200 mg NVP during labour if time allowed. All babies received sd NVP as soon as possible after birth. The infant NVP dose was 6 mg if birth weight (BW) was above 2 000 g and 2 mg/kg if it was below 2 000 g. Infants also received zidovudine (AZT) for 7 days, 12 mg twice daily if the BW was above 2 000 g and 4 mg/kg twice daily if it was below 2 000 g. Infant blood samples (0.2 ml) were collected on days 1, 2, 4, 6, 8, 14 and 21 after birth. After sampling, blood was immediately centrifuged and the plasma was separated from the centrifugate and stored in a -80ºC deep freeze until the assays were performed.
Plasma concentrations of NVP were determined by liquid chromatography-mass spectrometry using a Waters Alliance 2690 HPLC coupled to a Waters/Micromass ZMD single quadrapole mass spectrometer.16 The mobile phase consisted of 50% acetonitrile in 4 mM ammonium acetate, 0.1% trifluoroacetic acid. A 20×2.1 mm Hypersil Gold C18 column (Thermo) was used at a flow rate of 0.3 ml/min. Neostigmine served as internal standard. Detection in positive ionisation mode of nevirapine was at 276.2 (m/z) and neostigmine at 223.2 (m/z). To precipitate protein, 50 µl of acetonitrile containing 1 µg/ml internal standard was added to 20 µl of each sample or control. Samples were vortexed for 30 seconds, and centrifuged for 5 minutes at 750 g. After this 2 µl of the supernatant was injected onto the column. The standard curve was linear to 0.1 µg/ml. The lower limit of quantification (LLQ) was set at 100 ng/ml. Quality control samples of 0.8, 3 and 9 µg/ml were included with each run. Inter- and intra-day percentage coefficients of variation were less than 10% for all controls. An HIV-DNA-PCR test was done 28 days after birth.
Determination of pharmacokinetic parameters
After determining NVP plasma concentrations, the plasma concentration-time profile for each patient was plotted using GraphPad Prism 4 (GraphPad Software Inc., USA). NVP pharmacokinetic parameters were calculated using a non-compartmental analysis. The maximum concentration (Cmax) and time to reach the maximum concentration (Tmax) were obtained directly from the plasma concentration-time profile. The area under the plasma concentrationtime curve from zero to 21 days (AUC0-504) was calculated by the trapezoidal method. The AUC from zero to infinity (AUC0-∞) was calculated using the following formula: AUC0-504 + Cplast/ Ke, where Cplast is the last measurable plasma concentration. The following formula was used to determine the volume of distribution: Vd = dose/ (AUC0-∞ × Ke). The total body clearance (Cltot) was calculated using the following formula: Cltot = dose/AUC0-∞. The elimination rate constant (Ke) was calculated as the slope of terminal log-linear phase of the plasma concentration-time profile multiplied by -2.303. The half-life (T½) was calculated using the formula: T½ = 0.639/Ke.
Statistical analysis
Patient data were organised and coded onto data collection forms and captured into Microsoft Excel spreadsheets. NVP concentrations and pharmacokinetic parameters were analysed using descriptive statistics. The proportion of infants with NVP plasma levels >100 ng/ ml on day 8 in groups 1 and 2 were compared using the chi-square test with the null hypothesis that the proportions for the two groups were equal. The statistical software used was SAS version 9.2 (SAS Institute Inc., Cary, NC, USA).
Ethical considerations
The study was approved the ethics committees of the universities of the Western Cape (Reference Nb 04/7/10) and Stellenbosch (Reference Nb 04/10/183).
Results
Of 100 mothers, 68 received NVP during labour. Of their infants, 2 were withdrawn before enough blood samples could be collected, 1 died before the study was completed, and the volume of blood collected was insufficient for 7. Of the 32 infants whose mothers did not receive NVP, 2 were withdrawn, 1 died, and the volume of blood collected was insufficient for 6. Gestational age was determined with the new Ballard score in 59 cases (72.8%) and antenatal ultrasonography in 19 (23.5%).
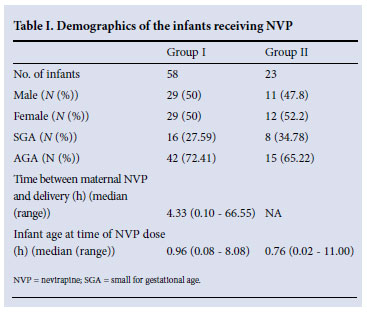
Table I sets out the demographic data for the 81 evaluable infants. The median gestational age was 34 weeks (range 28 - 37 weeks) and the median birth weight 2 052 g (range 950 - 3 400 g) for group I and 36 (28 - 37) weeks and 2 100 (1 028 - 3 460) g for group II. Twentyfour (29.6%) of the infants were SGA. Sixty-three received formula milk and 18 pasteurised expressed breastmilk.
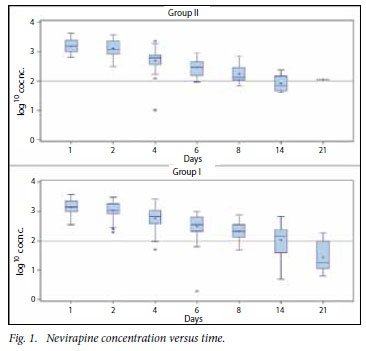
NVP concentrations over time
NVP plasma concentrations are presented in Table II and as box plots in Fig. 1. In the box plots the mean is denoted by +. The lower, middle and upper edges of the box represent the first quartile, the median and the third quartile, respectively. Extreme values are denoted by *. At 8 days after birth, 78% of infants whose mothers had received NVP had a NVP plasma concentration above 100 ng/ml compared with 70% of infants whose mothers had not received NVP (p=0.49).
Nevirapine pharmacokinetics
The median (range) Cmax, Tmax, AUC and T½ were 1 438.00 (350 -3 832) ng/ml, 25h50 (9h40 - 83h45), 174 134 (22 308 - 546 408) ng×h/ml and 59.00 (15.40 - 532.60) hours, respectively, for group I and 1 535 (635 - 4 218) ng/ml, 17h35 (7h40 - 29h), 168 576 (20 268 -476 712) ng×h/ml and 69.00 (22.12 -172.26) hours for group II. The median (range) Vd and Cl were 1 702.56 (623.74 - 6 189.77) ml and 34.91 (6.20 - 163.79) ml/h in group II (they could not be calculated in group I). The AUC was significantly higher and Cl significantly lower in SGA than AGA infants (Wilcoxon rank sum test p=0.006 and p<0.0001, respectively).
MTCT rate
Four infants (3 from group I and 1 from group II) were infected (transmission rate 4.8%) (95% confidence interval 1.3 - 11.9%).
Discussion
This study presents the first pharmacokinetic data for NVP in premature infants, a group comprising nearly 20% of deliveries in South Africa. The NVP concentration on day 8 exceeded our target of 100 ng/ml in 78% of infants whose mothers had received sd NVP and 70% of infants whose mothers had not received it. In previous studies of full-term infants, all had NVP concentrations over 100 ng/ ml at 7 days of life if both mother and infant received sd NVP.11,13,17,18
In our study, NVP exposure was not appreciably greater in infants whose mothers received intrapartum NVP compared with those who did not. Our median age at infant NVP dosing was less than 1 hour, compared with 3 - 5 hours in previous studies of the pharmacokinetics of single-dose NVP in term infants.11,12 Women in preterm labour often deliver with little advance warning, and our study suggests that NVP dosing of preterm infants as soon as possible after birth without maternal intrapartum dosing may be as effective as combined maternal and infant dosing. Avoiding maternal intrapartum NVP dosing eliminates the risk of maternal NVP exposure and subsequent maternal NVP resistance.19-21
The median NVP elimination T½ in the preterm infants in our study was prolonged compared with that of 48.5 hours seen after initial doses in adults, but was not markedly different from the 64.5 hours previously observed in term infants.16 The primary elimination pathway for nevirapine is oxidative metabolism by cytochrome P-450 enzymes of the CYP3A family, although CYP2B6 enzymes contribute as well.11 The major CYP3A isoform in adults is CYP 3A4, while fetuses express predominantly CYP3A7. After birth, CYP3A4 activity increases and CYP3A7 decreases over the first weeks and months of life.22 Clearance of midazolam, a known substrate for CYP3A metabolism, is reduced in newborns compared with older children and adults but not in premature neonates compared with term neonates.23,24 The lack of further prolongation of NVP and midazolam elimination in preterm infants compared with term infants is probably due to CYP3A7 activity. Our data suggest that the 2 mg/kg dose recommended for use in term infants is also appropriate for use in premature infants.9
Our study was the first to look at NVP elimination in both SGA and AGA preterm infants. The NVP AUC was significantly higher and Cl significantly lower in the SGA infants. We postulate that placental insufficiency could impair the levels of activity and maturation of CYP enzyme systems.
Conclusion
Our data support an NVP dosage of 2 mg/kg for infants born before 37 weeks' gestation. In term infants whose mothers do not receive intrapartum NVP, we recommend giving two doses of NVP, one immediately after birth and a second 48 - 72 hours later. Our data suggest that this may not be necessary in premature infants.
Acknowledgement. The South African Medical Research Council (MRC) supported the study. We thank the mothers and babies who participated, personnel from the labour ward, Department of Neonatology and Children's Infectious Diseases Clinical Research Unit (especially Sr B Hill, T Wahl and Mr G Fourie), Dr J L van Zyl of the High-Risk Neurodevelopmental Follow-up Clinic, Tygerberg Children's Hospital, and colleagues from the Pharmacokinetic Laboratory at UCT and the School of Pharmacy at UWC.
References
1. Rouzioux C, Costagliola D. Burgard M, et al. Estimated timing of mother-to-child human immunodeficiency virus type 1 transmission by use of a Markov model: The HIV Infection in Newborns French Collaborative Study Group. Am J Epidemiol 1995;142:1330-1337. [ Links ]
2. Bertolli J, St Louis ME, Simonds RJ, et al. Estimating the timing of mother-to-child transmission of human immunodeficiency virus in a breast feeding population in Kinshasa, Zaire. J Infect Dis 1996;174:722-726. [ Links ]
3. Townsend CL, Cortina-Borja M, Peckham CS, de Ruiter A, Lyall H, Tookey PA. Low rates of motherto-child transmission of HIV following effective pregnancy interventions in the United Kingdom and Ireland, 2000-2006. AIDS 2008;22(8):973-981. [ Links ]
4. Fowler MG, Lampe MA, Jamieson DJ, Kourtis AP, Rogers MF. Reducing the risk of mother-to-child human immunodeficiency virus transmission: past successes, current progress and challenges, and future directions. Am J Obstet Gynecol 2007;197(3 Suppl):S3-9. [ Links ]
5. Merluzzi V, Hargrave K, Grozinger K, et al. Inhibition of HIV-1 replication by a non-nucleoside reverse transcriptase inhibitor. Science 1990;250:1411-1413. [ Links ]
6. Cheeseman S, Havlir D, McLaughlin M, et al. Phase I/II evaluation of nevirapine alone and in combination with zidovudine for infection with human immunodeficiency virus. J AIDS 1995;8:141-151. [ Links ]
7. Havlir D, Cheeseman S, McLaughlin M, et al. High-dose nevirapine: safety, pharmacokinetics, and antiviral effect in patients with human immunodeficiency virus infection. J Infect Dis 1995;171:537-545. [ Links ]
8. Cheeseman S, Haltox S, McLaughlin M, et al. Pharmacokinetics of nevirapine: initial single-rising-dose study in humans. Antimicrob Agents Chemother 1993;37:178-182. [ Links ]
9. Guay LA, Musoke P, Fleming T, et al. Intrapartum and neonatal single-dose nevirapine compared with zidovudine for prevention of mother-to-child transmission of HIV-1 in Kampala, Uganda: HIVNET 012 randomised trial. Lancet 1999;354:795-802. [ Links ]
10. Jackson JB, Musoke P, Fleming T, et al. Intrapartum and neonatal single-dose nevirapine compared with zidovudine for prevention of mother-to-child transmission of HIV-1 in Kampala, Uganda: 18-month follow-up of the HIVNET 012 randomised trial. Lancet 2003;362:859-868. [ Links ]
11. Mirochnick M, Fenton T, Gagnier P, et al. Pharmacokinetics of nevirapine in human immunodeficiency virus type 1-infected pregnant women and their neonates. J Infect Dis 1998;178:368-374. [ Links ]
12. Musoke P, Guay LA, Bagenda D, et al. A phase I/II study of the safety and pharmacokinetics of nevirapine in HIV-1-infected pregnant Ugandan women and their neonates (HIVNET 006). AIDS 1999;13(4):479-486. [ Links ]
13. Barros FC, Bhutta ZA, Batra M, Hansen TN, Victora CG, Rubens CE; the GAPPS Review Group. Global report on preterm birth and stillbirth (3 of 7): evidence for effectiveness of interventions. BMC Pregnancy and Childbirth 2010;10(Suppl 1):S3. [ Links ]
14. Ballard JL, Khoury JC, Wedig K, Wang L, Eilers-Walsman BL, Lipp R. New Ballard score, expanded to include extremely premature infants. J Pediatr 1991;119(3):417-423. [ Links ]
15. World Health Organization. Rapid HIV Tests: Guidelines for Use in HIV Testing and Counseling Services in Resource-constrained Settings. Geneva: WHO, 2004:1-48. [ Links ]
16. Mirochnick M, Clarke DF, Dorenbaum A. Nevirapine considerations in children and pregnant women. Clin Pharmacokinet 2000;39(4):281-293. [ Links ]
17. Mirochnick M, Siminski S, Fenton T, et al. Pharmacokinetics of nevirapine in pregnant women and in their infants following in utero exposure. Presented at the 7th Conference on Retroviruses and Opportunistic Infections, 30 January - 2 February 2000, San Francisco. Abstract No. 716. [ Links ]
18. Warner A. Drug use in neonates: Interrelationship of pharmacokinetics, toxicity, and biochemical maturity. Clin Chem 1986;32/5:721-727. [ Links ]
19. Jourdain G, Ngo-Giang-Huong N, Le Coeur S, et al. Intrapartum exposure to nevirapine and subsequent maternal responses to nevirapine-based antiretroviral therapy. N Engl J Med 2004;351(3):229-240. [ Links ]
20. Lockman S, Shapiro RL, Smeaton LM, et al. Response to antiretroviral therapy after a single, peripartum dose of nevirapine. N Engl J Med 2007;356(2):135-147. [ Links ]
21. Palumbo P, Violari A, Lindsey J, et al. Nevirapine (NVP) vs lopinavir-ritonavir (LPV/r)-based antiretroviral therapy (ART) in single dose nevirapine (sdNVP)-exposed HIV-infected infants: preliminary results from the IMPAACT P1060 trial. Presented at the 5th IAS Conference on HIV Pathogenesis, Treatment and Prevention, 19-22 July 2009, Cape Town. [ Links ]
22. Shapiro RL, Thior I, Gilbert PB, et al. Maternal single-dose nevirapine versus placebo as part of an antiretroviral strategy to prevent mother-to-child HIV transmission in Botswana. AIDS 2006;20(9):1281-1288. [ Links ]
23. De Wildt SN, Kearns GL, Hop WC, Murry DJ, Abdel-Rahman SM, van den Anker JN. Pharmacokinetics and metabolism of intravenous midazolam in preterm infants. Clin Pharmacol Ther 2001;70:525-531. [ Links ]
24. Lee TC, Charles BG, Harte GJ, Gray PH, Steer PA, Flenady VJ. Population pharmacokinetic modeling in very premature infants receiving midazolam during mechanical ventilation: midazolam neonatal pharmacokinetics. Anesthesiology 1999;90:451-457. [ Links ]
Accepted 4 March 2011.
Corresponding author: P Mugabo (pmugabo@uwc.ac.za)














