Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 n.8 Pretoria Aug. 2011
ORIGINAL ARTICLES
The effectiveness of the South African Triage Score (SATS) in a rural emergency department
K RosedaleI; Z A SmithII; H DaviesIII; D WoodIV
IMB BCh (Hons), BSc. Ngwelezane Hospital Emergency Department, Empangeni, KwaZulu-Natal
IIMB BCh (Hons), BSc, DTM&H. Ngwelezane Hospital Emergency Department, Empangeni, KwaZulu-Natal
IIIMB BCh, BSc, DipPEC, DA. Ngwelezane Hospital Emergency Department, Empangeni, KwaZulu-Natal
IVMB BCh, BPharm, MPhil, FCEM (UK), DipPEC, DA. Ngwelezane Hospital Emergency Department, Empangeni, KwaZulu-Natal
ABSTRACT
BACKGROUND: The Modified Early Warning Score (MEWS) is used to monitor medical inpatients in hospitals in the developed world. The South African Triage Score (SATS) was developed from the MEWS, and its use throughout South Africa has been proposed.
OBJECTIVES: We aimed to assess the effectiveness of the SATS in an emergency department (ED) in a rural setting in KwaZulu-Natal (KZN).
METHODS: A prospective cross-sectional study undertaken over a 1-month period in June 2009 of patients in the ED of a government hospital in rural KZN, the referral centre for 22 peripheral hospitals. Data capture included physiological parameters, mobility and trauma scores, a list of selected clinical conditions (physician discriminator list), MEWS and SATS scores, final clinical diagnosis, and outcome in the ED (death, hospital admission or discharge). Outcome measures were under- and over-triage rates according to both systems.
RESULTS: Over the study period, 589 patients were triaged and their data analysed. The MEWS under-triaged 15.1% (over-triaged 8.3%) of cases that needed admission, compared with an undertriage rate of 4.4% (over-triage rate 4.3%) when the SATS was used.
CONCLUSION: Our study supports use of the SATS as a primary triage score in South African urban and rural hospitals. The SATS is superior to the MEWS as a triage scoring system in a rural hospital ED in KZN, its rates of under- and over-triage falling within the limits of the American College of Surgeons Committee on Trauma (ACSCOT) guidelines.
South African government hospitals are poorly resourced, overcrowded, understaffed and underfunded, contributing to the pressure under which emergency departments (EDs) operate. The trauma load is one of the highest in the world.1 EDs deal firsthand with South Africa's so-called 'quadruple burden of disease':2 communicable diseases, non-communicable chronic diseases, injuries and HIV/AIDS (considered separately). The result is prolonged ED waiting times. An effective triage system to ensure early recognition of sick patients and prioritisation for treatment is essential.
'Triage' originates from the French meaning 'to select or sort'. The many triage scoring systems worldwide3-5 all require extensive training to implement, are labour intensive, and have a high failure rate. Many limitations also surround triage scale validation, and those used in developed countries are often inappropriate for developing countries.6 The Modified Early Warning Score (MEWS) has not been formally validated as a triage tool but has been used as a rapid, simple triage method to identify medical patients needing hospital admission and those at increased risk of in-hospital death.7 It is a successful indicator of condition severity, originally identifying physiological deterioration of inpatients.8 However, the MEWS encompasses only physiological parameters, which leads to medical bias in the ED.
Trauma patients are generally healthy and have good physiological reserve, so injuries may be severe with apparently normal physiological markers. Adding a 'mobility score' led to the development of the Trauma Early Warning Score (TEWS). Further, the Cape Triage Score (CTS) used triage discriminators that allow appropriate triage in cases with normal physiology (e.g. keto-acidosis, burns). It effectively increases triage scores for trauma cases and provides a more robust system that can easily be taught to inexperienced staff. Designed in 2006 to encompass trauma and medical patients in the ED and prehospital setting, it was the first national triage system implemented in South Africa.9,10 It dramatically reduced the waiting time of patients attending the ED.11 The scoring has been adapted to include a 'trauma score' as part of the TEWS component and is known as the South African Triage Score (SATS) (Table I).12
South Africa's extremely high burden of HIV and tuberculosis (TB), particularly in KwaZulu-Natal (KZN),13 means that a large proportion of chronically unwell patients attend EDs. Their baseline physiological parameters may be grossly abnormal, e.g. patients with pulmonary TB may present with symptoms of weakness and associated immobility. They may be hypoxic with a fever, and have altered vital signs such as increased respiratory and pulse rates.14 Such patients therefore score very highly in the SATS, despite not necessarily requiring 'immediate' treatment. In an ED in KZN, we hypothesised that a disadvantage of the SATS would be that these chronically ill patients would often be prioritised, to the detriment of more urgent acutely sick or injured patients. This study aimed to evaluate the use of the SATS and to compare the effectiveness of the MEWS versus the SATS in a rural hospital ED in KZN.
Methods
Ngwelezane Hospital is a 554-bed government referral hospital for 22 peripheral hospitals serving an estimated population of 3 million; only 28.2% of this population are formally employed, and only 39.2% have piped water to their houses.15 The ED deals with approximately 5 000 consultations per month, about 20% of these patients requiring inpatient treatment.
Data were collected prospectively from patients admitted to the casualty area in the ED from 1 to 31 June 2009 on weekdays between the hours of 08h00 and 16h00. They included patients referred from clinics or brought by ambulance. Exclusion criteria included children under 12 years (for whom a child/infant SATS system exists), those 'seen and treated' rather than formally triaged, and those admitted directly to the resuscitation bay or high-dependency unit (HDU) areas. Incomplete data sets were excluded.
On a patient's arrival, according to the generic flowchart for the SATS,12 nursing staff took a brief history and documented the main complaint, recorded vital signs, assessed mobility and level of consciousness according to the AVPU scale (A = alert, V = responds to voice, P = responds to pain, U = unresponsive), and calculated a TEWS. Pulse rate and blood pressure were measured by an automated Dynamap machine and temperature recorded by an automated tympanic thermometer. The TEWS score was then matched to the SATS discriminator list and an appropriate triage score allocated. Data capture was performed by the attending clinician on a standardised data collection sheet which incorporated age, gender, presenting complaint, MEWS and TEWS parameters, and outcome.
Outcomes
Primary endpoints were admission to the ward or HDU, or death in the ED. The hypothesis was that patients with a MEWS score of 4 or more or a SATS colour code of red/orange would have a higher likelihood of admission or death (endpoint reached). Conversely, patients scoring 0 - 2 on the MEWS or having a SATS colour code of green would be likely to be discharged home (endpoint not reached).
We also considered patients in our subset who were inappropriately triaged by each triage tool. Over-triage assumed that an endpoint was indicated according to the score (MEWS >4 or SATS orange/red) but not reached, i.e. the patient was discharged from the ED. Conversely, under-triage assumed that an endpoint was not indicated (score 0 - 2 or SATS colour code green) but was reached (i.e. patient admitted). The American College of Surgeons Committee on Trauma (ACSCOT) guideline suggests that threshold indicators for overtriage would be acceptable up to 50%, and 10% for under-triage.16
Data analysis
Data were entered into a Microsoft Excel 2007 spreadsheet and MEWS, TEWS and SATS scores calculated according to measured parameters and the physician discriminator list (Table I).
Results
Of the 640 patients entered into the trial, 589 (92.0%) had complete datasets; the mean age was 38.2 years (standard deviation 17.3), and 49.6% were women; 47.5% of consultations were medical, 17.0% surgical, 33.0% for trauma, and 1.5% psychiatric.
Outcomes
A total of 257 patients (43.6%) reached an endpoint. Of these, 253 required admission and 4 died (0.7% departmental mortality rate). Fig. 1 shows the distribution of scores across the different triage categories for each system. A higher proportion was seen with MEWS scores 0 - 2 than in the SATS green category.
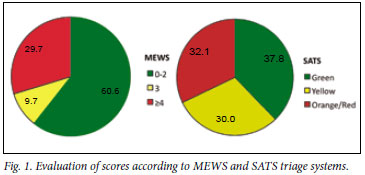
Fig. 2 shows that a greater percentage of patients in the higher categories scored by the SATS than those scored by the MEWS reached an endpoint. In the lowest-scoring category the reverse was true.
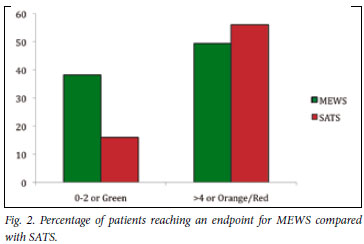
Triage
MEWS under-triaged 15.1% of patients (45 medicine, 11 surgery, 28 trauma and 5 psychiatry) and over-triaged 8.3% (39 medicine, 4 surgery and 6 trauma). In comparison, SATS under-triaged 4.4% of patients (19 medicine, 3 surgery and 4 trauma) and over-triaged 4.3% (19 medicine, 5 trauma and 1 surgical) (Fig. 3).
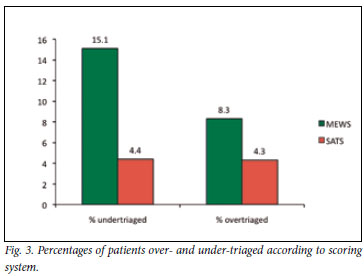
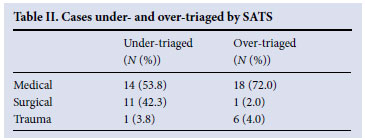
Under-triaged cases were mainly surgical patients requiring minor interventions, infections requiring intravenous antibiotics, or medical cases with normal physiological parameters. In the case of over-triage, most were medical cases (Table II). Patients with TB accounted for 24.0% of all SATS over-triaged cases.
Discussion
An argument for using the SATS in South Africa was that it would avoid the extensive training required to implement other triage systems such as the Manchester Triage, Canadian Triage Assessment Scale and Australian Triage Score. The SATS was in use in 75% of Western Cape hospitals in 2006.17 Accepting a training period, it was thought that even inexperienced staff could learn the new system following brief teaching, and there was hope for rolling this out throughout South Africa.9 In our experience, once the system worked well, using the SATS was safe and efficient. However, nursing staff initially resisted these changes because they found the tool Table II. Cases under- and over-triaged by SATS cumbersome to use at first. Owing to understaffing, the difficulties were more pronounced during busy periods.
Medical patients comprised 48% of those attending the ED. Many chronically unwell patients attend in wheelchairs or on stretchers Medical 14 (53.8) 18 (72.0) because of weakness or loss of energy. Adding the mobility score Surgical 11 (42.3) 1 (2.0) to medical patients who were otherwise relatively stable resulted in Trauma 1 (3.8) 6 (4.0) their over-triage and inappropriate resource allocation. The inverse of this effect were relatively stable patients who presented with more serious features that increased their MEWS according to the SATS physician discriminator list, i.e. seizures, hyperglycaemia, shortness of breath. This accounted for the higher proportion of SATS scores on the upper end of the spectrum compared with the MEWS. In these cases early medical resource allocation was appropriate. For trauma patients, the mobility discriminator appears to be more reflective of severity of injury.
The SATS has certain pitfalls. In KZN the quadruple burden of disease exerts greater pressure than in the Western Cape, where the SATS was founded. This is reflected in the higher proportion of MEWS score of 4 or more, or SATS orange/red coded patients, in our study (32.1%) than reported previously (27.1%).18 In our ED, chronically unwell patients frequently overwhelmed the triage system and prevented it from functioning effectively due to high numbers of 'orange' patients who were more stable than their score indicated (usually due to poor mobility), and did not require immediate attention. This was reflected by the high proportion of over-triaged patients in the medical category and suffering from TB. We had an over-triage rate of 4.3%, which is well within the acceptable range of 50% indicated by the ACSCOT guidelines.16 Although over-triage is preferable, because it protects patients who require treatment, it adds to the resource burden in poorly equipped and under-staffed South African hospitals.
When considering under-triage, the study clearly shows that the SATS is more effective in this setting than the MEWS. Under-triage rates were 15.1% for the MEWS and only 4.4% for the SATS. The acceptable rate for under-triage is <10%.16 Using the SATS rather than the MEWS therefore takes this proportion from unacceptable to acceptable. The patients who were under-triaged were medical, surgical and trauma patients (Table II). Most of these patients were not suffering from presenting conditions that caused haemodynamic instability, but rather required further intervention beyond what is provided in casualty, e.g. intravenous antibiotics or minor orthopaedic intervention. It therefore seems probable that the under-triage rate in this study is falsely high.
Perhaps one of the most important aspects of the SATS is the 'senior health care professional's discretion' tool. In our ED, we noted a vast anecdotal improvement in the functioning of the triage system when one experienced clinician was placed in charge of triage for the unit. Although nursing staff still documented the SATS score, this doctor consistently ensured adherence and correct use of the tool. Triage scores may therefore be amenable to downgrading when deemed appropriate, e.g. patients with high scores due to chronic disease who are considered not to require urgent resuscitative intervention. This clearly relies on senior clinician input and is dependent on staffing levels. However, we recommend this practice in units where staffing is adequate to provide such a service.
Conclusion
The variety, severity and numbers of cases in this study reflect the burden of disease in South Africa. In developed countries chronically ill medical patients usually attend the ED earlier, before their physiological parameters deteriorate to such life-threatening levels. A much higher proportion of our patients than those in the developed world fall into the higher triage categories, due to delays in reaching the ED. The SATS is more effective than the MEWS in triaging both medical and trauma patients correctly in a rural ED setting. Using the SATS reduces under-triage, which improves patient safety in terms of inappropriate discharge from hospital. However, the SATS is a more complex system than the MEWS, and correct implementation is more difficult. There are issues with adherence to the system, training, and the constant need for a senior health care professional's involvement. The 'senior health care professional's discretion' is essential, not only to ensure adherence but also to oversee correct patient endpoints, particularly to downgrade priority levels in chronic disease.
References
1. Matzopoulos RG, Prinsloo M, Butchart A, et al. Estimating the South African trauma caseload. Int J Inj Contr Saf Promot 2006;13:49-51. [ Links ]
2. Bradshaw D, Groenewald P, Laubscher R, et al. Initial burden of disease estimates for South Africa, 2000. S Afr Med J 2003;93:682-688. [ Links ]
3. Beveridge R, Ducharme J, Janes L, et al. Reliability of the Canadian emergency department triage and acuity scale: interrater agreement. Ann Emerg Med 1999;34:155-159. [ Links ]
4. Australian College of Emergency Medicine. G24 Guidelines on the Implementation of the Australasian Triage Scale in Emergency Departments. Melboune: Australian College of Emergency Medicine, 2005. [ Links ]
5. Manchester Triage Group. Emergency Triage. Manchester: BMJ Publishing Group, 1997. [ Links ]
6. Twomey M, Wallis LA, Myers JE. Limitations in validating emergency department triage scales. Emerg Med J 2007;24:477-479. [ Links ]
7. Burch VC, Tarr G, Morroni C. Modified early warning score predicts the need for hospital admission and inhospital mortality. Emerg Med J 2008;25:674-678. [ Links ]
8. Subbe CP, Kruger M, Rutherford P, et al. Validation of a modified Early Warning Score in medical admissions. QJM 2001;94:521-526. [ Links ]
9. Gottschalk SB, Wood D, DeVries S, et al. The Cape Triage Score: a new triage system in South Africa. Proposal from the Cape Triage Group. Emerg Med J 2006;23:149-153. [ Links ]
10. Wallis PA, Gottschalk SB, Wood D, et al. The Cape Triage Score - a triage system for South Africa. S Afr Med J 2006;96:53-56. [ Links ]
11. Bruijns SR, Wallis LA, Burch VC. Effect of introduction of nurse triage on waiting times in a South African emergency department. Emerg Med J 2008;25:395-397. [ Links ]
12. South African Triage Group, a division of the Emergency Medicine Society of South Africa. South African Triage Score (SATS), 2008. http://www.triagesa.co.za (accessed 30 November 2010). [ Links ]
13. Bradshaw D, Nannan N, Groenewald P, et al. Provincial mortality in South Africa, 2000: priority-setting for now and a benchmark for the future. S Afr Med J 2005;95:496-503. [ Links ]
14. Gibson W. The tachycardia of early pulmonary tuberculosis. Trans Am Climatol Assoc 1906;22:96-101. [ Links ]
15. Statistics South Africa. Census 2001: Primary Tables KwaZulu-Natal - '96 and 2001 Compared. Pretoria: Statistics South Africa, 2004. [ Links ]
16. American College of Surgeons Committee on Trauma (ASCOT). Resources for Optimal Care of the Injured Patient. Chicago: American College of Surgeons, 1999. [ Links ]
17. Bateman C. New triage system halves mortalities. S Afr Med J 2006;96:770-772. [ Links ]
18. Bruijns SR, Wallis LA, Burch VC. A prospective evaluation of the Cape triage score in the emergency department of an urban public hospital in South Africa. Emerg Med J 2008;25:398-402. [ Links ]
Accepted 15 February 2011.
Conflicting interests. None.
Corresponding author: D Wood (darryl.wood@kznhealth.gov.za)














