Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 no.8 Pretoria ago. 2011
FORUM
ISSUES IN PUBLIC HEALTH
South Africa's cataract surgery rates - why are we not meeting our targets?
Karin Lecuona; Colin Cook
Cataract is the leading cause of blindness in South Africa, responsible for about 50% of the prevalence of blindness1 and identified as a national health priority. The cataract surgery rate (CSR) should be at least 2 000 per million population per year for elimination of cataract blindness.2 The national CSR target was planned to increase from 1 000 in 2005 to 2 000 in 2010, but since CSRs have failed to reach targets each year, the national target for 2010 was reduced from 2 000 to 1 500. We reviewed data from a situational analysis in 2007 of cataract surgery services to ascertain the obstacles to achieving CSR targets.
Methods
Quantitative data on the 2006 cataract surgery figures, human resources and the facilities available for cataract surgery were obtained from all public sector units offering cataract surgery. Provincial eye care co-ordinators provided a list of the provincial and mission hospitals providing cataract surgery to indigent patients. Pre-tested questionnaires were sent electronically to the ophthalmologist or ophthalmic medical officer working in each of the hospitals, and those who failed to respond were telephoned. The cataract surgery numbers provided were checked against the numbers submitted to the Department of Health (DoH) by each of the provincial eye care co-ordinators. Population data for each health district were obtained from the DoH.
Qualitative data on the perceived barriers to achieving higher cataract surgery numbers were obtained from surgeons and managers involved with planning of eye care services and provincial eye care co-ordinators by semi-structured in-depth telephone interviews. They were asked to identify the main causes for the low CSR in their province. At least 3 persons from each province were interviewed to obtain different perspectives and corroboration of the information. One province was excluded because permission for the interviews was not obtained from the provincial health department.
The national cataract surgery rates between 2005 and 2010 and the CSR targets for the period 2005 -2010 were obtained from the DoH.
Results
Human resources
The human resources available for eye care and cataract surgery in 2006 in the indigent population of South Africa are far below the number recommended for the public sector (number available in South Africa followed by recommended number in brackets): ophthalmologist 70 and ophthalmic medical officer 55 (160); ophthalmic nurse 65 (380); optometrist 74 (152).
Cataract surgery units
Cataract surgery in 2006 was performed in 44 of 53 districts; 34 districts had at least one hospital performing at least weekly cataract surgery, and 10 districts relied on regular outreach cataract surgery services. Sixty-two hospitals were equipped for cataract surgery: 41 were Level 1 + 2 hospitals, and 21 were Level 3 hospitals. An additional 19 hospitals were used for regular outreach services. Twenty-seven (66%) of the 41 Level 1+2 hospitals equipped for cataract surgery had a cataract surgery list on only one day each week. All the hospitals had surgery waiting lists.
Cataract surgeries
A total of 40 024 cataract surgical procedures were done in 2006 by 125 surgeons (mean: 320 per surgeon). The most done per surgeon in a district was 770 (in a rural district receiving non-government organisation support for eye care services by a single ophthalmologist with 4 ophthalmic nurses trained and equipped to run eye clinics in the district).
Provincial CSRs
The 2006 provincial CSRs positively correlated with the proportion of the population who live in urban areas (Pearson correlation co-efficient 0.80, p value 0.017) (Table I).
Reported barriers to increasing CSRs
In 24 telephone interviews, the main reported barriers to increasing CSRs were (in terms of number of provinces) (i) inadequate commitment by hospital or provincial managers to increase surgery numbers (7); (ii) insufficient access to theatre (7); (iii) theatre staff unfamiliar with high-volume cataract surgery (5); (iv) erratic supply of surgery consumables (5); (v) shortage of ophthalmic nurses (5); (vi) shortage of surgeons (4); and (vii) surgeons performing other non-surgical work (screening, refractions, administration) (4). In most provinces, a lack of commitment by management to increase numbers, and insufficient theatre time, were felt to hamper the number of cataract surgeries performed.
National cataract surgery rates
Fig. 1 shows CSR targets and CSRs actually achieved in the period 2005 - 2010. CSRs have increased by only 20% over 5 years, and failed to reach set targets each year.
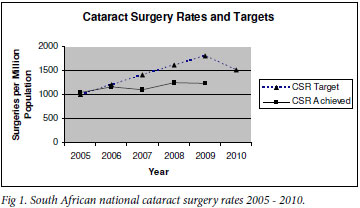
Discussion
The national CSR target in 2009 was 1 800, but the actual figure achieved was 1 226. The target for 2010 was set at 2 000 by the DoH, but was subsequently reduced to 1 500. It seems improbable that even this lower target will be met.
In most African countries, the barrier to increasing CSRs is an inadequate demand for surgery i.e. there is spare surgical capacity, but barriers in the community limit or preclude surgery uptake.5 In South Africa, the problem is inadequate surgery capacity, with waiting lists at all the hospitals where cataract surgery is done.
Despite inadequate surgical capacity in South Africa, the provincial CSRs correlate with the proportions of the urban population in each province. Urbanisation seems to drive demand for surgery and push up the CSR. With ongoing urbanisation, this demand for surgery will probably grow, and so will our waiting lists unless we increase our surgery capacity.
Of 53 districts in South Africa, 34 have at least one surgical unit providing cataract surgery at least once a week, and an additional 10 districts have outreach cataract surgery. While each of the 53 districts should ideally have its own unit providing regular surgery, 34 surgical units for a population of 38 million who are dependent on public sector services is close to the Vision 2020 target of one surgical unit per million population.6 Surgical unit numbers in South Africa do not seem to be the major problem.
The cataract services survey in 2007 identified primarily management problems in all the provinces as reasons for our low surgery capacity. A lack of commitment to increase cataract surgery numbers seems to be the underlying cause. Insufficient theatre time, erratic supplies of surgery consumables, and inefficiencies in theatre are cited as causes. Several eye hospitals in India and Nepal have systems that produce high levels of efficiency, high-volume delivery, and high-quality, low-cost cataract surgery.7-9 These systems have been adopted in some hospitals in Africa, allowing high cataract surgery numbers and district CSRs above 2 000.10 South Africa is falling behind.
A shortage of surgeons and inappropriate use of surgeons' time on performing other non-surgical work are also cited as causes. There are 125 cataract surgeons in provincial hospitals in South Africa (the recommended minimum number for our indigent population of 38 million is 160).3 The cataract surgeons comprise ophthalmologists and ophthalmic medical officer cataract surgeons. The latter are general medical officers trained in cataract surgery and who might spend one or more days a week doing cataract surgery, usually working in Levels 1 and 2 hospitals. The minimum number of cataract surgeons, optometrists and ophthalmic nurses recommended for Vision 2020 programmes in sub-Saharan Africa are 1 per 250 000, 1 per 250 000, and 1 per 100 000 population respectively - a ratio of 4:4:10.3 The ratio in South Africa is 2.5:1.5:1.3 which implies that some of the surgeons' time is spent doing non-surgical work such as patient screening and refractions. The highest number of 770 surgeries performed by a single surgeon in one year was achieved in a rural Level 1 hospital by a single medical officer cataract surgeon, supported by 4 ophthalmic nurses who screened and selected the patients for surgery, examined them after surgery, and managed the clinics and surgery lists. More posts for ophthalmologists, optometrists and ophthalmic nurses, and more training for medical officer surgeons, to achieve the recommended figures and proportions clearly should be provided.
The average number of surgeries done by a cataract surgeon in South Africa in 2006 was only 320.11 The 2007 survey did not evaluate the quality or the cost of cataract surgery in South Africa, but these are inextricably linked. Surgeons' complication rates decrease with higher surgery numbers - practice makes perfect.12 South Africa's cataract burden requires 500 - 1 000 cataract surgeries per surgeon per year to ensure high-quality surgery. Higher surgery numbers and fixed overhead costs decrease the unit costs of cataract surgery.13 Low surgery numbers by individual cataract surgeons make for a poor-quality service, and the low surgery numbers in individual surgery units make for an expensive service. These figures would be unacceptable to South Africa's private hospital managers and to India's high-volume eye hospitals - and should be unacceptable to South Africa's provincial hospital managers.
Conclusion
Cataract surgery is one of the most cost-effective of all health interventions, and the most cost-effective surgery.14 A target CSR of 2 000 per million population per year is realistic and achievable in South Africa. Increasing our cataract surgery rate should improve the quality of our surgery and reduce unit costs. Several recommendations may increase our cataract surgery rate to this level. In existing surgical units, systems developed in India and Nepal to generate efficiency and high-volume, high-quality, low-cost surgery should be introduced. Additional posts for ophthalmologists, optometrists and ophthalmic nurses should be provided and more medical officer cataract surgeons trained. Surgeries done each year by individual surgeons should be monitored, with a recommended minimum of 500 - 1 000 cataract surgeries per year.
This study was performed as part of a dissertation for MSC Community Eye Health (LSHTM) and was made possible by grants from the MRC, Nuffield Foundation and Commonwealth Shared Scholarship Scheme.
1. Cook CD, Stulting AA. Prevalence and incidence of blindness due to age-related cataract in the rural areas of South Africa. S Afr Med J 1995;85(1):26-27. [ Links ]
2. Foster A. VISION 2020: The Cataract Challenge J Comm Eye Health 2000;13(34):17-19. [ Links ]
3. World Health Organization. Global Initiative for the Elimination of Avoidable Blindness. 1997. whqlibdoc.who.int/hq/1997/WHO_PBL_97.61_Rev.1.pdf (accessed 20 July 2010). [ Links ]
4. StatsOnLine. http://www.statssa.gov.za/publications/P0302/P03022006.pdf (accessed 24 April 2011). [ Links ]
5. Lewallen S, Courtright P. Recognising and reducing barriers to cataract surgery. Community Eye Health 2000;13(34):20-21. [ Links ]
6. Department of Health. National guideline: Prevention of Blindness in South Africa - Fact Sheets/Guidelines 2002 www.doh.gov.za/docs/factsheets/guidelines/blindness.pdf (accessed 23 May 2008). [ Links ]
7. Thulasiraj RD, Priya R, Saravanan S. High volume, high quality cataract surgery. Indian Journal of Community Health 1997;3(2):32. http://laico.org/v2020resource/files/hightvol_catsurg.pdf (accessed 4 October 2010). [ Links ]
8. Gogate PM, Kulkarni SR, Krishnaiah S, et al. Safety and efficacy of phacoemulsification compared with manual small-incision cataract surgery by a randomized controlled clinical trial: six-week results. Ophthalmology 2005;112(5):869-874. [ Links ]
9. Hennig A, Kumar J, Yorston D, Foster A. Sutureless cataract surgery with nucleus extraction: outcome of a prospective study in Nepal. Br J Ophthalmol 2003;87(3):266-270. [ Links ]
10. Faal H, Minassian DC, Dolin PJ, Mohamed AA, Ajewole J, Johnson GJ. Evaluation of a national eye care programme: re-survey after 10 years. Br J Ophthalmol 2000;84(9):948-951. [ Links ]
11. Lewallen S, Kello AB. The need for management capacity to achieve VISION 2020 in Sub-Saharan Africa. PLoS Med 2009;6(12):e1000184. [ Links ]
12. Bell CM, Hatch WV, Cernat G, Urbach DR. Surgeon volumes and selected patient outcomes in cataract surgery: a population-based analysis. Ophthalmology 2007;114(3):405-410. [ Links ]
13. Yorston D. High-volume surgery in developing countries. Eye 2005;19(10):1083-1089. [ Links ]
14. Marseille E. Cost-effectiveness of cataract surgery in a public health eye care programme in Nepal. Bull World Health Organ1996;74(3):319-324. [ Links ]
15. South African Health Systems Trust. Health Statistics (2006). http://www.healthlink.org.za/healthstats/10/data (accessed 24 April 2011). [ Links ]
Karin Lecuona is an ophthalmologist, and Colin Cook is Professor and Head of Department, of the Division of Ophthalmology, University of Cape Town and Groote Schuur Hospital.
Corresponding author: K Lecuona (karin.lecuona@uct.ac.za)














