Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 n.6 Pretoria Jun. 2011
ORIGINAL ARTICLES
Staphylococcus aureus skin and soft-tissue infections at a tertiary hospital in Botswana
Hong TruongI; Samir S ShahII; Jonathan LudmirIII; Ephraim O TawananaIV; Margaret BafanaV; Sarah M WoodVI; Howard MoffatVII; Andrew P SteenhoffVIII
IMS. Jefferson Medical College, Philadelphia, PA, USA
IIMD, MSCE. University of Pennsylvania School of Medicine and Children's Hospital of Philadelphia
IIIMD. University of Pennsylvania School of Medicine
IVBA. National Health Laboratory, Gaborone, Botswana
VMS. National Health Laboratory, Gaborone, Botswana
VIMD. Children's Hospital of Philadelphia
VIIMB ChB, FRCP. Botswana Ministry of Health, Gaborone
VIIIMB BCh, DCH, FCPaed (SA). University of Pennsylvania School of Medicine, Botswana-UPenn Partnership, Gaborone, and Children's Hospital of Philadelphia
ABSTRACT
OBJECTIVES: To study the epidemiology of Staphylococcus aureus skin and soft-tissue infections (SSTIs) in hospitalised children and adults in Gaborone, Botswana, and to describe the changes in antimicrobial susceptibilities of S. aureus isolates over time.
METHODS: A retrospective cohort study evaluated SSTI isolates from January 2000 to December 2007 at Princess Marina Hospital (PMH), a large tertiary referral centre in Gaborone. Eligible subjects were those hospitalised at PMH during the study period who had a skin or soft-tissue culture yielding a bacterial or fungal pathogen. The primary outcome measure was a skin or soft-tissue culture yielding S. aureus. Secondary outcomes were the organism's antimicrobial susceptibilities.
RESULTS: S. aureus was detected in 857 (35.8%) of single-organism SSTI cultures, and 194 (22.6%) of these isolates were methicillin resistant (MRSA). The proportion of MRSA isolates increased over time (linear test of trend: p=0.03 from 2000 to 2003), and MRSA isolates were more likely than methicillin-susceptible isolates to be resistant to commonly used antimicrobials recommended by the national SSTI treatment guideline.
CONCLUSIONS: We report a high and increasing proportion of MRSA SSTIs in Gaborone. This high rate of MRSA resistance to currently recommended empiric antibiotics for SSTIs dictates the need for revising national guidelines and ongoing prospective surveillance of SSTIs in this setting.
Over the past decades, methicillin-resistant Staphylococcus aureus (MRSA) has become a key pathogen in skin and soft-tissue infections (SSTIs). The emergence of MRSA in 1961 occurred predominantly in patients exposed to health care facilities;1,2 community-acquired MRSA (CA-MRSA) isolates were identified in the 1990s.3,4 From 1993 to 2005, the impact of CA-MRSA nearly tripled emergency department SSTI visits in the USA.4 However, there are limited data on the incidence and characteristics of SSTIs in sub-Saharan Africa, and knowledge of pathogen-specific attributable morbidity is lacking.
HIV-infected patients are at markedly increased risk for CA-MRSA SSTI. In Chicago the incidence of CA-MRSA SSTIs was 6-fold higher among HIV-infected patients than among HIV-negative patients.5 Given the region's high HIV seroprevalence rate, the impact of MRSA may be particularly pronounced in sub-Saharan Africa.6 A multinational surveillance project in eight African hospitals and Malta found that 14.8% of clinically significant S. aureus strains isolated from patients were resistant to methicillin.7 The prevalence of MRSA isolates was even higher in sub-Saharan countries, ranging from 16.8% in CÔte d'Ivoire to 29.6% in Nigeria.7 The prevalence of HIV in Botswana's general population is estimated to be 17% and reaches nearly 35% among individuals aged 15 -49 years, the highest infection rate after Swaziland.8 An S. aureus colonisation rate of 57.5% has been reported among food handlers in Gaborone, and 11.2% of bacteraemias in this setting are caused by MRSA, with neither study stratifying results by HIV status.9,10 Owing to the high prevalence of HIV in Botswana and the emergence of MRSA in blood isolates, we hypothesise that MRSA plays a significant role in SSTIs in this setting. However, the actual incidence and characteristics of SSTIs in this population remain unknown.
Knowledge of regional antimicrobial susceptibility patterns of SSTI pathogens influences treatment decisions and has broad public health implications. However, no data describing the antimicrobial susceptibility patterns of bacteria causing SSTIs in Botswana are available. In 2007 the Botswana Ministry of Health published national treatment guidelines for SSTIs, recommending doxycycline or penicillin for treatment of skin breaks with clinical signs of bacterial infections in adults, and co-trimoxazole, erythromycin or penicillin in children.11 These treatment guidelines and the lack of epidemiological and antimicrobial susceptibility data on SSTIs set the stage for this study. The primary objective was to determine the epidemiology of S. aureus SSTIs in hospitalised children and adults in Botswana's capital city of Gaborone over an 8-year period. The secondary objective was to describe temporal changes in antimicrobial susceptibilities of S. aureus isolates over this period.
Methods
This retrospective cohort study evaluated SSTI isolates from January 2000 to December 2007 at Princess Marina Hospital (PMH) in Gaborone, Botswana. PMH is the largest tertiary care referral centre in Botswana, with 530 beds and 20 000 -30 000 admissions annually. PMH provides virtually free health care to citizens of Botswana and charges a subsidised fee to non-citizens. Since January 2002, Botswana as a whole, and PMH in particular, have provided free highly active antiretroviral therapy (HAART) to citizens who are HIV positive and who meet specified clinical criteria.8 All patients hospitalised at PMH during the study period who had a skin or soft-tissue culture yielding a bacterial or fungal pathogen were included.
SSTI was defined as a culture of non-blood, non-stool or non-cerebrospinal fluid specimens that yielded a single bacterial or fungal pathogen. Most specimens were collected from pus, wound sites, eye, ear, throat, vaginal swabs, pleural fluid, pericardial fluid, joint fluid or brain abscesses. Polymicrobial skin and soft-tissue cultures were considered contaminants and were not included. Multiple cultures from an individual patient within 7 days of the original culture were considered part of the same episode of SSTI and therefore excluded. Clinical wards at PMH were categorised by three parameters: the clinical nature of the ward (medical, surgical, intensive care unit, accident and emergency, orthopaedic, oncology, ophthalmology, radiology); gender (male v. female medical or orthopaedic wards); and age of patients (neonatal, paediatric or adult).
Skin and soft-tissue cultures were subjected to microscopy, culture and sensitivity testing. Antimicrobial susceptibility patterns of isolates were determined by disc-diffusion methods according to Clinical Laboratory Standards Institute guidelines.12 Antimicrobial agents used were amikacin, ampicillin, amoxicillin-clavulanate, cefotaxime, ceftazidime,cephradine,chloramphenicol,ciprofloxacin,clindamycin, erythromycin, gentamicin, methicillin, penicillin G, piperacillin, tetracycline, trimethoprim, trimethoprim-sulfamethoxazole (TMP-SMX) and vancomycin. The D test for inducible clindamycin resistance was not available. Organisms that were resistant to all of the following were classified as multidrug-resistant organisms: ampicillin, amoxicillin-clavulanate, cefotaxime, gentamicin, tetracycline, trimethoprim and TMP-SMX. The proportion of resistance among S. aureus isolates was calculated by dividing the number of resistant isolates by the total number of isolates.
Electronic and manual records of the Botswana National Health Laboratory were reviewed to identify skin and soft-tissue samples that met the study criteria. Demographic data were abstracted from the records, including anatomical site of sample, age, gender, and the hospital ward at the time of specimen collection. Results of antimicrobial susceptibility testing were recorded. Owing to laboratory personnel changes, transition from manual to electronic medical records and periodic shortages of antibiotics, there were missing laboratory records in 39 of the 96 months (41%) of the study period - May 2000 -July 2001, December 2002 -June 2003, April 2004 -February 2005, June 2005 -September 2005, and November 2005 -December 2005.
Data were analysed using STATA version 11.0 (Stata Corp., College Station, TX). Continuous variables such as age were described using mean, median, and range or interquartile range (IQR) values and compared using the Wilcoxon rank-sum test. Categorical variables were described using counts and percentages and compared using the chi-square test. We used univariable logistic regression to determine the association of individual covariates with MRSA infection and a linear test of trend to identify changes in MRSA prevalence over time.
Results
During the study period, 2 979 (31.6%) of 9 428 cultures from SSTIs were positive. A single organism was isolated from 2 404 (80.7%) of the positive cultures. S. aureus was detected in 857 (35.8%) of the single-organism cultures.
Table I describes the demographic characteristics of patients with S. aureus infections. MRSA accounted for 194 (22.6%) of S. aureus isolates. Of patients with an MRSA SSTI, 55.1% were male. Patients 13 -49 years of age accounted for almost two-thirds of cases (Table I). The most common sites of S. aureus infection or colonisation were vaginal swabs (N=53), wounds (N=42) and eyes (N=36). However, in the vast majority of S. aureus isolates the anatomical site was unspecified 'pus' and 'unspecified fluid', yielding 2 083 (86.6%) and 60 (2.5%) of isolates, respectively.
The male orthopaedic ward had the highest rate of MRSA (42 cases - 20.6% of MRSA SSTIs). Patients in the male medical ward (odds ratio (OR) 4.5, 95% confidence interval (CI) 1.8 -18.2, p=0.01) were at increased odds of having a MRSA SSTI compared with SSTIs in the neonatal unit. Fig. 1 displays the annual prevalence of MRSA. The lowest proportion of MRSA SSTIs was in 2000 (15.9%) and the highest proportion was in 2003 (27%; linear regression p=0.03 from 2000 to 2003). Although there was an increase in the proportion of MRSA from 2000 to 2003, there were no further increases from 2003 to 2007 (p=0.48).

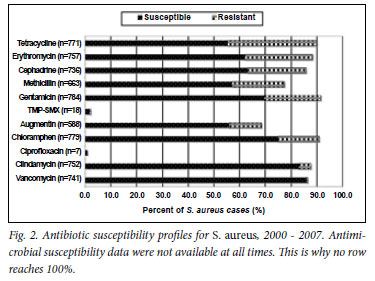
S. aureus isolates were routinely tested for susceptibility to amoxicillin-clavulanate, cephradine, chloramphenicol, clindamycin, erythromycin, gentamicin, methicillin, penicillin, tetracycline and vancomycin. Susceptibility to TMP-SMX was not routinely tested; results were available for only 18 isolates (Fig. 2). S. aureus was most susceptible to vancomycin, clindamycin and chloramphenicol, with susceptibility rates of 99.5%, 94.5% and 82.5%, respectively. No chloramphenicol susceptibility data were available for 2000.
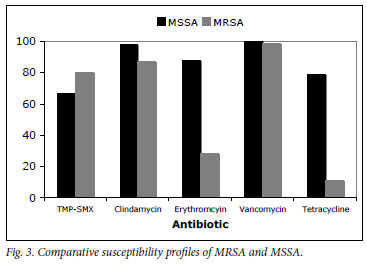
The antibiotic susceptibilities of MRSA and MSSA are compared in Fig. 3. MRSA isolates were more likely to be resistant to clindamycin (OR 26.1, 95% CI 15.1 -46.2, p<0.001), erythromycin (OR 25.5, CI 15.8 -41.3, p<0.001) and tetracycline (OR 31.0, 95% CI 17.8 -55.9, p<0.001), compared with MSSA isolates.
Discussion
The epidemiology and drug susceptibility of S. aureus SSTIs in Botswana are described. There is a high proportion of S. aureus SSTIs, particularly MRSA, at the tertiary hospital that serves the population of southern Botswana. Significant factors that increase the odds of MRSA infection among our cohort include age group 13 -49 years, and hospitalisation in the intensive care unit, male orthopaedic and male medical wards.
An increasing proportion of MRSA SSTIs in Botswana between 2000 and 2003 and high levels of MRSA resistance to commonly used antibiotics are revealed. There is considerable variation in MRSA resistance profiles between regions and countries. In Australia, Singapore and Taiwan, MRSA is predominantly resistant to ciprofloxacin, clindamycin, erythromycin, gentamicin, TMP/ SMX and tetracycline.13 In KwaZulu-Natal, South Africa, MRSA is resistant to clindamycin, erythromycin and TMP/SMX. Similarly, MRSA cases in this Botswana study displayed high resistance rates to clindamycin, erythromycin and tetracycline. This susceptibility pattern is of concern because patients with SSTIs in Botswana are routinely treated with one of these medications or penicillin. The empiric prescription of penicillin is probably targeting infection by Streptococcus group A, but our findings suggest that S. aureus is an under-recognised cause of SSTIs in Botswana.
Despite the Botswana Ministry of Health's recommendation to administer co-trimoxazole as the drug of choice for cutaneous bacterial infections, which is supported by current US guidelines advocating TMP-SMX as the first-line therapy against communityacquired MRSA, S. aureus isolate susceptibilities to TMP-SMX were not routinely tested. Additionally, we found that vancomycin, the most effective antibiotic against MRSA, is not readily available at health centres other than the main hospital. Hence, we propose four improvements in managing SSTIs in Botswana: (i) revision of Botswana's national SSTI guidelines, including discontinuing advocating penicillin as empiric treatment for SSTIs in a setting where S. aureusaccounts for more than a third of culture-positive SSTIs and virtually all of these S. aureus isolates are resistant to this class of antibiotics (this has been achieved, as Botswana's national antibiotic guidelines, informed by information from this study, were revised in July 2010); (ii) TMP-SMX susceptibility testing of all S. aureus SSTI isolates; (iii) improved hospital infection control guidelines and practices to prevent MRSA transmission in the hospital setting; and (iv) vancomycin availability in district hospitals with strict guidelines governing its use.
Limitations of this study include: (i) missing laboratory data from our study period may have contributed to an underestimate of SSTI prevalence; (ii) the anatomical site was not known for most S. aureus isolates, making it impossible to define the exact nature of each SSTI; (iii) owing to the retrospective study design, standard laboratory techniques may have shifted over the 8-year study period; and (iv) our retrospective design makes our results susceptible to potential biases of studies of similar design.
In summary, we found a high and increasing proportion of MRSA SSTIs in Gaborone. Additionally, the high rate of MRSA resistance to currently recommended empiric antibiotics for SSTIs dictates the need for revising national guidelines and ongoing prospective surveillance of SSTIs in this setting.
We thank the Botswana Ministry of Health, Dr Harvey Friedman, Dr Rameshwari Thakur, Jack Rowe, the staff of the microbiology lab in the Botswana National Health Laboratory, Rudo Nthobatsang, Katherine Steele, Gill Jones and Nikki Jones, who made this project possible by providing invaluable guidance and/or assisting with the logistics.
References
1. Deurenberg RH, Stobberingh EE. The evolution of Staphylococcus aureus. Infect Genet Evol 2008;8:747-763. [ Links ]
2. Shittu AO, Lin J. Antimicrobial susceptibility patterns and characterization of clinical isolates of Staphylococcus aureus in KwaZulu-Natal province, South Africa. BMC Infect Dis 2006;6:125. [ Links ].
3. Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med 2006;355:666-674. [ Links ]
4. Pallin DJ, Egan DJ, Pelletier AJ, Espinola JA, Hooper DC, Camargo CA Jr. Increased US emergency department visits for skin and soft tissue infections, and changes in antibiotic choices, during the emergence of community-associated methicillin-resistant Staphylococcus aureus. Ann Emerg Med 2008;51:291-298. [ Links ]
5. Popovich KJ, Weinstein RA, Aroutcheva A, et al. Community-associated methicillin-resistant Staphylococcus aureus and HIV: intersecting epidemics. Clin Infect Dis 2010;50(7):979-987. [ Links ]
6. Babirekere-Iriso E, Musoke P, Kekitiinwa A. Bacteraemia in severely malnourished children in an HIVendemic setting. Ann Trop Paediatr 2006;26(4):319-328. [ Links ]
7. Kesah C, Ben Redjeb S, Odugbemi TO, et al. Prevalence of methicillin-resistant Staphylococcus aureus in eight African hospitals and Malta. Clin Microbiol Infect 2003;9:153-156. [ Links ]
8. Agency NAC. Botswana AIDS Impact Survey II: Popular Report. Gaborone: National AIDS Coordinating Agency, 2005. [ Links ]
9. Loeto D, Matsheka MI, Gashe BA. Enterotoxigenic and antibiotic resistance determination of Staph aureus strains isolated from food handlers in Gaborone, Botswana. J Food Prot 2007;70(12):2764-2768. [ Links ]
10. Wood SM, Shah SS, Bafana M, et al. Epidemiology of methicillin-resistant Staphylococcus aureus bacteremia in Gaborone, Botswana. Infect Control Hosp Epidemiol 2009;30(8):728-725. [ Links ]
11. Kennedy I. Botswana Treatment Guide 2007. Botswana: Ministry of Health National Standing Committee on Drugs, 2007. [ Links ]
12 Clinical and Laboratory Standards Institute. Performance Standards for Antimicrobial Disk Susceptibility Tests: Approved Standard. 10th ed. Wayne, Penn.: CLSI, 2009. [ Links ]
13. Bell JM, Turnidge JD, SENTRY APAC. High prevalence of oxacillin-resistant Staphylococcus aureus isolates from hospitalized patients in Asia-Pacific and South Africa: results from SENTRY antimicrobial surveillance program, 1998-1999. Antimicrob Agents Chemother 2002;46(3):879-881. [ Links ]
Accepted 8 February 2011.
Financial support. This project was supported in part by the University of Pennsylvania Center for AIDS Research IP30AI45008-01 to APS.
Conflict of interest. The contributing authors of this publication have no relationship or support that may constitute a conflict of interest.
Corresponding author: J Ludmir (ludmir@mail.med.upenn.edu)














