Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 n.6 Pretoria Jun. 2011
FORUM
CLINICAL IMAGES
Tuberculous lymphadenitis and Horner's syndrome
Robert Freercks; Mark W Sonderup
Given the significant disease burden of tuberculosis (TB) and TB/ HIV co-infection in South Africa, disseminated TB and tuberculous lymphadenitis are common and important causes of morbidity. Despite this relationship, Horner's syndrome secondary to tuberculous lymph node compression of sympathetic nerves is rare.
Case report
A 20-year-old HIV-positive woman, not on antiretroviral therapy, was admitted to Groote Schuur Hospital following a short history of headache, lethargy and night sweats. She had previously started a 6-month course of TB treatment, but defaulted after 2 months.
She had significant meningism and bilateral enlarged, non-tender cervical lymph nodes in the anterior and posterior triangles, but no focal neurological deficit at this point.
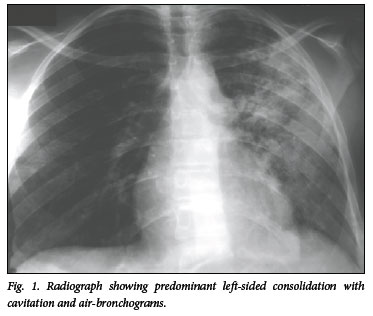
Chest radiography revealed confluent opacification of the left upper lobe with areas of cavitation and air-bronchograms (Fig. 1). The working diagnosis was disseminated TB with meningitis owing to incomplete TB treatment, for which she was admitted and treated. A subsequent TB blood culture was positive for drug-sensitive TB.
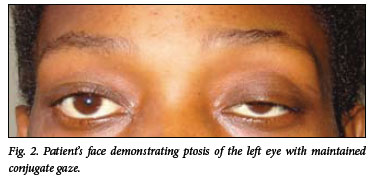
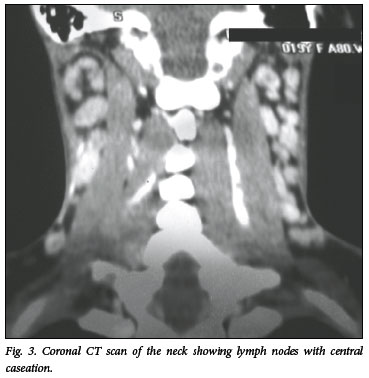
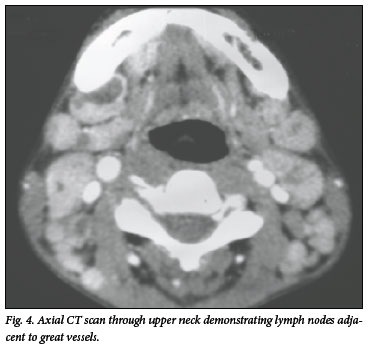
Within 36 hours of admission she developed left-sided ptosis and miosis with anisocoria (Fig. 2). Facial sweating was preserved and ocular movements were intact with no diplopia or other cranial nerve or long tract deficit, in keeping with a left postganglionic Horner's syndrome. A computed tomography (CT) scan demonstrated enlarged, centrally necrotic lymph nodes bilaterally in the neck (Fig. 3), adjacent to and displacing the carotid artery bifurcation on the left (Fig. 4). Three months after further TB care, her Horner's syndrome had resolved.
Discussion
Two case series1,2 identified neoplastic disease as the most common cause of Horner's syndrome. Only two case reports in the English literature describe TB as a cause for Horner's syndrome.3,4 Notably, the first-ever published case was in the SAMJ and was thought to be a pre-ganglionic lesion.
Horner's syndrome has many possible aetiologies that can involve a lesion anywhere in the course of the sympathetic tract from hypothalamus to brainstem and upper thoracic cord, sympathetic trunk, stellate ganglion, carotid artery and, finally, long ciliary nerve to the eye. The lack of other focal neurological deficits in our patient vitiates the possibility of a central lesion such as brainstem tuberculoma or tuberculous endarteritis. The preservation of facial sweating, which implies a post-ganglionic lesion as facial sweat gland tracts run along the external carotid artery, localises the lesion to the upper neck and/or internal carotid artery. A neoplastic cause is excluded by the lack of mediastinal or apical lung lesions on the CT scan, the presence of central lymph node necrosis, and the good response to TB treatment.
1. Giles CL, Henderson JW. Horner's syndrome: an analysis of 216 cases. Am J Ophthalmol 1958;46:289-296. [ Links ]
2. Keane JR. Oculosympathetic paresis. Analysis of 100 hospitalized patients. Arch Neurol 1979;36:13-15. [ Links ]
3. Ismail MH, Hodkinson HJ, Tuling B. Horner's syndrome and tuberculosis. A case report. S Afr Med J 1988;74:586-587. [ Links ]
4. Norhaya MR, Kuppusamy I, Aziah AM. Tuberculosis and Horner's syndrome. Int J Tuberc Lung Dis 1998;2:1049. [ Links ]
Robert Freercks and Mark Sonderup are affiliated to the Department of Medicine, University of Cape Town, and Groote Schuur Hospital.
Corresponding author: M Sonderup (msonderup@samedical.co.za)














