Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SAMJ: South African Medical Journal
versão On-line ISSN 2078-5135
versão impressa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.101 no.1 Pretoria Jan. 2011
ORIGINAL ARTICLES
Ecological determinants of blindness in Nigeria: the Nigeria national blindness and visual impairment survey
M M RabiuI; Murthy V S GudlavalletiII; C E GilbertIII; Selvaraj SivasubramaniamIV; Fatima KyariI; Tafida AbubakarV; on behalf of the Nigeria National Blindness and Visual Impairment Study Group*
IFMCOphth, MSc. National Eye Centre, Kaduna, Nigeria
IIMB BS, MD, MSc. International Centre for Eye Health, London School of Hygiene and Tropical Medicine, Keppel Street, London, UK
IIIFRCOphth, MD. International Centre for Eye Health, London School of Hygiene and Tropical Medicine, Keppel Street, London, UK
IVVBSc, MSc. International Centre for Eye Health, London School of Hygiene and Tropical Medicine, Keppel Street, London, UK
VFMCOphth. Ministry of Health, Dutse, Jigawa State, Nigeria
ABSTRACT
OBJECTIVE: To determine the prevalence and causes of visual loss in different ecological zones across Nigeria.
METHODS: A population-based survey using multi-stage, stratified, cluster random sampling with probability proportional to size comprising a nationally representative sample of adults aged >40 years from six ecological zones.
OUTCOME MEASURES: Distance vision was measured using reduced logMAR charts. Clinical examination included basic eye examination for all respondents and a detailed examination including visual fields, gonioscopy and fundus photography for those who were visually impaired or blind (i.e. presenting vision <20/40 in the better eye). A principal cause of visual loss was assigned to all respondents with presenting vision <20/40 in the better eye.
RESULTS: A total of 15 122 persons aged >40 years were enumerated, 13 599 (89.9%) of whom were examined. The prevalence of blindness varied according to ecological zone, being highest in the Sahel region (6.6%; 95% confidence interval (CI) 4.2 - 10.4) and lowest in the rain forest region (3.23%; 95% CI 2.6 - 3.9). Age/gender-adjusted analyses showed that risk of blindness was highest in Sahel (odds ratio (OR) 3.4; 95% CI 2.1 - 5.8). More than 80% of blindness in all ecological regions was avoidable. Trachoma was a significant cause only in the Sudan savannah belt. The prevalence of all major blinding conditions was highest in the Sahel.
CONCLUSIONS: The findings of this national survey may be applicable to other countries in West and Central Africa that share similar ecological zones. Onchocerciasis and trachoma are not major causes of blindness in Nigeria, possibly reflecting successful control efforts for both these neglected tropical diseases.
Ecological factors such as rainfall, temperature, vegetation, humidity, topography and altitude are associated with eye diseases, particularly those caused by infectious agents.1 Cataract, glaucoma, trachoma and onchocerciasis account for a significant proportion of blindness, especially in developing countries,2 and evidence links many of them directly or indirectly to ecological factors. For example, trachoma is endemic in communities in dry, dusty environments where water is scarce and the local environment often unhygienic,3 whereas onchocerciasis occurs mainly in communities close to rivers with characteristic topography that provides suitable breeding sites for the vector - the simulium species of black fly.4 It is also well recognised that the pattern of onchocercal disease in rain forest areas differs from that in savannah regions.5,6
Evidence for the role of ecological factors for non-communicable eye diseases is less robust, and the findings are more open to interpretation. The prevalence of lens opacities is clearly higher among people living in areas with high temperatures, low rainfall and lower altitudes,7,8 but these areas are often relatively poor and individuals are exposed to other factors, such as nutritional deficiencies and smoke from burning biomass fuels.9 Ultraviolet (UV) radiation has been postulated to be a risk factor for cataract, and the intensity of UV radiation varies in different latitudes and altitudes.10 Temperature and relative humidity are also associated with a higher prevalence of glaucoma,11-12 but this may reflect the geographical distribution of different ethnic groups known to have varying risk and access to services.12
Nigeria, the most populous country in Africa, has five ecological zones (river delta (fresh water swamps/mangroves), rain forest, Guinean forest savannah (woodland tall-grass savannah), Sudan savannah (short-grass savannah) and Sahel (marginal savannah)). These are shared by 19 other countries with a total population of 345 million people in West and Central Africa. These ecological zones are characterised by dry, arid conditions in the north (Sahel) and mangrove forest in the southern river delta area, with the rain forest, Guinean forest savannah, and Sudan savannah zones occupying most of the central regions of the country.
The National Blindness and Visual Impairment Survey was conducted over a 30-month period between 2005 and 2007.13 This paper explores associations between blindness/visual impairment and residence in Nigeria's different ecological zones.
Material and methods
A description of the sampling, enumeration, visual acuity (VA) and ocular examination procedures has been published.13 Ethical approval for the study was provided by the London School of Hygiene and Tropical Medicine and the Federal Government of Nigeria. The study adhered to the tenets of the Declaration of Helsinki. Informed consent was obtained from the participants after explanation of the nature of the study.
Ecological zones
The geographical coordinates (latitude and longitude bearings to the last second), and altitude (in metres) were recorded at the geographical centre of each cluster using a Thuraya satellite phone.
In a few situations where there was no satellite signal because of bad weather or the satellite phone was not available, the geographical coordinates of the closest urban area to the cluster were obtained from the Internet.
Sampling
Details of the sample size calculations have been reported.13 Multi-stage, stratified, cluster random sampling with probability proportional to size procedures were used to identify a cross-sectional nationally representative sample of 15 027 persons >40 years of age. The sample covered all the 36 states and the federal capital territory of Abuja and the 5 ecological zones in Nigeria. A total of 310 clusters across the country were identified, of which 5 could not be visited because of civil unrest (Fig. 1).
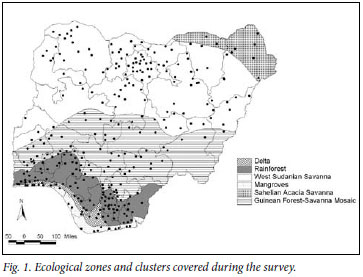
Personal and demographic data of eligible participants were collected at the time of enumeration and participants were invited to attend a location within the cluster for clinical examination. Enumerated individuals not reporting to the examination site were followed up three times and offered an examination at their house before being deemed non-respondents. Non-respondents were not replaced.
Examination procedures
All participants were interviewed to obtain socio-demographic data including age, sex, ethnicity, literacy level, occupation, and relevant past medical and ocular history. Blood pressure, height and weight were measured. The presenting distance VA was measured (i.e. with correction if usually worn) by an ophthalmic nurse, initially at 4 m and then at 1 m if required, using a reduced logMAR E chart. Each eye was tested separately and then testing was repeated with both eyes open. Individuals who could not be tested were assessed by an ophthalmologist who designated them as 'believed blind' or 'believed not blind'. All participants underwent auto-refraction, ocular axial length measurement, keratometry and visual field screening using frequency-doubling technology. Corrected VA was also assessed when indicated. Participants then had a basic eye examination by an ophthalmologist which included optic disc assessment. Detailed examination by a second ophthalmologist, including examination after dilation, was done on all those with presenting vision <20/40 in one or both eyes or who were believed to be blind; those with abnormal optic discs; and a 1 in 8 sample regardless of VA or findings during the basic eye examination. The examination consisted of slit-lamp anterior segment examination with applanation tonometry; gonioscopy; lens grading after dilation, using the World Health Organization (WHO)'s simplified grading system; and bi-microscopic fundus examination. Digital images were taken of all fundi wherever possible. A cause of visual loss was determined for all participants with presenting VA <20/40 in one or both eyes or who were believed to be blind, following WHO guidelines. All participants requiring further investigation or treatment were referred accordingly.
Definitions
Blindness/visual impairment
Blindness: Presenting VA (with glasses for distance if normally worn or unaided if glasses for distance not worn) of <20/400 in the better eye.
Severe visual impairment (SVI): Presenting VA of <20/200 - 20/400 in the better eye. Moderate visual impairment: Presenting VA of <20/63 -20/200 in the better eye. Mild visual impairment: Presenting VA <20/40 -20/63 in the better eye.
Normal/near normal: Presenting VA >20/40 in the better eye.
Cataract: Significant cataract was defined as grade 2B or 3 based on the Mehra-Minassian grading scheme and/or a score of 2 -3 based on the WHO lens grading system. These have been described in an earlier paper.14
Refractive errors/uncorrected aphakia: Significant refractive error and uncorrected aphakia were defined as a presenting visual acuity of <0/63, improving to >20/63 after refraction.
Glaucoma: Glaucoma was defined as a cup/disc ratio of >0.7 and/or intra-ocular pressure of >21 mmHg, with characteristic changes in the optic disc or visual fields adjudged to be consistent with glaucoma.
Identification of causes of visual loss
All individuals with a VA of <20/40 in either eye were assigned a cause for their visual loss. The algorithm to identify the principal cause for vision loss in an individual has been described earlier.13
As per the WHO procedure, refractive error was considered more amenable to treatment than cataract.14 If refractive error and cataract co-existed in the same eye, cataract was therefore selected as the main cause if the refraction did not improve visual acuity to >20/63.
Statistical analysis
A customised database was created in Microsoft Access and data were entered by two trained data entry clerks. Data entered by one operator were checked by the second operator and corrected if necessary. Quality assurance procedures included a random verification of filled forms in the field and at the project office. Data were transferred to the International Centre for Eye Health for cleaning and analysis.
Conditions were classified as preventable or treatable (i.e. avoidable) or unavoidable. Cause-specific prevalences of blindness and visual impairment were determined by age, gender, literacy, residence and ecological zone. Univariate and age/gender-adjusted logistic regression modelling was used to explore associations of the major causes. Design effects due to cluster sampling were taken into account in the calculation of confidence intervals (CIs) for prevalence estimates and for odds ratios (ORs) in the regression modelling. Stata 10.0 (Stata Corp, Texas, USA) was used for all the statistical analyses.
Results
Study population
A total of 15 122 persons aged >40 years were enumerated, 13 599 (89.9%) of who were examined in 305 clusters. The overall response rate was 89.9%, ranging from 87.9% in the delta region to 93.8% in the Sahel (Table I). The Sahel region had the smallest number of clusters, reflecting the population living in this ecological zone. Significant differences in age structure, gender, literacy and place of residence were observed across the ecological zones. Overall there was a higher proportion of females (54%).
Prevalence of blindness and visual impairment
The overall prevalence of blindness (presenting VA <20/400) was 4.2% (95% CI 3.8 -4.6). The prevalence varied by ecological zone, being highest in the Sahel region (6.6%; 95% CI 4.2 - 10.4) and lowest in the rain forest region (3.23%; 95% CI 2.6 -3.9) (Table II). There was no overlap in the CIs in these zones, indicating that these are statistically significant differences. The prevalence of SVI ranged from 1.1% (rain forest) to 1.8% (Guinean forest savannah). Adjusting for age and gender, those living in the Sahel had a 3.4 times higher risk of being blind (95% CI 2.1 - 5.8; p=0.001) than those in the rain forest. Residents in the Sudan savannah belt (adjusted OR 2.0; 95% CI 1.6 - 2.7; p=0.001) also had a higher risk of blindness. However, populations in the Guinean forest savannah (adjusted OR 1.2; 95% CI 0.9 - 1.7; p=0.183) and delta (adjusted OR 1.2; 95% CI 0.8 - 1.8; p=0.292) did not have a significantly higher risk compared with those in the rain forest region.
Causes of blindness
More than 80% of blindness in all ecological regions was avoidable (Table III). Cataract was the commonest cause of blindness in all zones and glaucoma was the second-commonest cause. Trachoma was an important cause only in the Sudan savannah belt, where 8.3% of blindness was attributable to trachoma. Onchocerciasis was only seen in the Guinean forest savannah and rain forest belt. Corneal scars were the most important preventable cause of blindness across all the ecological zones. The cause-specific prevalence of the major blinding conditions is shown in Table IV. Cataract blindness was the most prevalent in all ecological zones and was highest in the Sahel.
Age- and gender-adjusted association analyses showed that residents of the Sahel had a 3.8 times higher risk and residents of the Sudan savannah a 2.1 times higher risk of cataract blindness compared with residents of the rain forest region (Table V). A 3.4 times higher risk of glaucoma blindness was seen among Sahel residents and a 5.1 times higher risk of corneal pathology among residents of the Sudan savannah region.
Discussion
The high response rate across the country minimises non-response bias in the study. The number of persons examined in the Sahel was much lower than in the other regions, as this ecological zone is small in area and sparsely populated. Because significant demographic differences were observed between ecological regions, analyses were adjusted for age and gender.
Climatic conditions across Nigeria's ecological zones vary significantly: mean monthly temperatures range from 25 -28ºC in the delta region to 22 -33ºC in the Sahel/Sudan savannah regions,15 and the rainfall pattern also differs. The delta region has a bimodal pattern of rainfall as opposed to a unimodal pattern in the Sahel and Sudan savannah regions. The mean annual rainfall exceeds 2 000 mm in the delta region, while the rain forest area has 1 200 -2 000 mm annually, the Sudan savannah and the Guinean forest savannah 600 -1 400 mm, and the Sahel region 400 -600 mm.15 Living in regions with high rainfall in Pakistan was found to be associated with significantly lower odds of lens opacities compared with residence in the hot and dry regions.16 Residence in hotter regions may mean greater exposure to UV radiation, which may increase the risk of lens opacities. Most ecological studies suggest that there is an increased risk of cataract in areas of greater ambient UVB radiation,17 as do studies that have measured person-level exposure to UVB.
The gradient in blindness prevalence across the country, from high in the dry Sahel in the north to relatively low in the rain forest and delta zones in the south, has several possible explanations. Access to eye care services may be an important determinant, as the Sahel and Sudan savannah regions have fewer eye care services than the rain forest region (U Onyebuchi, national blindness co-ordinator, personal communication). Secondly, differences in climate and vegetation influence the distribution of trachoma and onchocerciasis, and in this survey trachoma blindness was higher in the Sahel and savannah regions while onchocerciasis-related blindness was seen mostly in the rain forest and Guinean forest savannah regions.
The overall prevalence of blindness among those aged >40 in Nigeria was much higher than reported from rapid assessments in Western Rwanda,18 Cameroon19 and Kenya,20 although lower than reported from Ethiopia for the older population (>60 years).21 The prevalence of blindness in the Sahel region was 3 times higher than reported in Western Rwanda18 or Kenya,19 even though these two studies were limited to individuals aged >50 years. The prevalence in the dry, poorly served population of the Sahel region of Nigeria was nearly 6 times higher than in populations of similar ages surveyed in neighbouring Cameroon.19,22 The proportion of avoidable causes of blindness in this study was much higher than reported from Rwanda,18 Kenya20 and Cameroon.19,22 In the Sahel region, 100% of blindness observed was avoidable. This highlights the need for priority action to eliminate avoidable blindness in Nigeria by augmenting service delivery and increasing access to needy populations in remote and under-served regions of Nigeria, if the goal of VISION2020: The Right to Sight initiative is to be achieved.
These findings from Nigeria can be used to estimate the need for eye care services for populations in similar ecological zones in West and Central Africa, provided that access to services is similar. The only exception may be glaucoma, where there may be ethnic differences in risk.
Ecological studies, such as this report, explore associations and make inferences about levels of disease in different populations (or subgroups within a population) compared with levels of exposure at the person level. However, ecological studies have two major limitations: firstly, not all those who develop the disease of interest will necessarily have been exposed to the risk factor being investigated,Discussion which is called the ecological fallacy; and secondly, confounding The high response rate across the country minimises non-response cannot always be taken into account, which can give misleading bias in the study. The number of persons examined in the Sahel was results. However, researchers have also stated that population-level much lower than in the other regions, as this ecological zone is small exposure may act as an 'effect modifier' as the risk to individuals would not have occurred if they were not living in an area of specific exposure.23 Despite these weaknesses, ecological studies can add to existing knowledge about risk factors for disease.
The authors thank Mrs Oye Quaye for managing the finances for the study, Mr Auwal Shehu and Mr Dania Charles for data entry, and the teams of ophthalmic nurses, enumerators and interviewers in the six geopolitical zones who assisted in data collection.
References
1. Johnson GJ. The environment and the eye. Eye 2004; 18: 1235-1250. [ Links ]
2. Resnikoff S, Pascolini D, Etya'ale D, et al. Global data on visual impairment in the year 2002. Bull World Health Organ 2004; 82: 844-851. [ Links ]
3. Webb SG, Prehistoric eye disease (trachoma?) in Australian aborigines. Am J Phys Anthropol 1990; 81: 91-100. [ Links ]
4. Botto C, Escalona E, Vivas-Martinez S, Behm V, Delgado L, Coronel P. Geographical patterns of onchocerciasis in southern Venezuela: relationships between environment and infection prevalence. Parassitologia 2005; 47: 145-150 [ Links ]
5. Picq JJ, Albert JP. Sudan-savannah and rain-forest onchocerciasis in West Africa: an epidemiological problem. Rev Epidemiol Sante Publique 1979; 27: 483-498. [ Links ]
6. Umeh RE, Chijioke CP, Okonkwo PO. Eye disease in an onchocerciasis-endemic area of the forest-savannah mosaic region of Nigeria. Bull World Health Organ 1996; 74: 95-100. [ Links ]
7. Sasaki H, Kawakami Y, Ono M, et al. Localization of cortical cataract in participants of diverse races and latitude. Invest Ophth Vis Sci 2003; 44: 4210-4214. [ Links ]
8. Sasaki H, Jonasson F, Shui YB, et al. High prevalence of nuclear cataract in the population of tropical and subtropical areas. Dev Ophthalmol 2002; 35: 60-69. [ Links ]
9. Fullerton DG, Bruce N, Gordon SB. Indoor air pollution from biomass fuel smoke is a major health concern in the developing world. Trans R Soc Trop Med Hyg 2008; 102: 843-851. [ Links ]
10. Seckmeyer G, Pissulla D, Glandorf M, et al. Variability of UV irradiance in Europe. Photochem Photobiol 2008: 84: 172-179. [ Links ]
11. Hu CC, Lin HC, Chen CS. A 7-year population study of primary angle closure glaucoma admissions and climate in Taiwan. Ophthalmic Epidemiol 2008; 15: 66-72. [ Links ]
12. Weale RA. Ethnicity and glaucoma: higher environmental temperatures may accelerate the onset, and increase the prevalence of primary open-angle glaucoma. Med Hypotheses 2007; 69: 432-437. [ Links ]
13. Dineen B, Gilbert CE, Rabiu MM, et al. The Nigerian national blindness and visual impairment survey: rationale, objectives and detailed methodology. BMC Ophthalmol 2008; 8: 17 [ [ Links ]epub].
14. Kyari F, Gudlavalleti MV, Sivasubramaniam S, et al. Prevalence of blindness and visual impairment in Nigeria: The national blindness and visual impairment survey. Invest Ophthalmol Vis Sci 2009, 50: 2033-2039. [ Links ]
15. Food and Agriculture Organization. http://www.fao.org/ag/agl/swlwpnr/reports/y_sf/z_ng/ngtb131.htm (accessed 9 February 2009). [ Links ]
16. Shah SP, Dineen B, Jadoon Z, et al. Lens opacities among adults in Pakistan: prevalence and risk factors. Ophthalmic Epidemiol 2007; 14: 381-389. [ Links ]
17. West S. Ocular ultraviolet B exposure and lens opacities: a review. J Epidemiol 1999; 9: Suppl, S97-101. [ Links ]
18. Mathenge W, Nkurikiye J, Limburg H, Kuper H. Rapid assessment of avoidable blindness in Western Rwanda: blindness in a postconflict setting. PLoS Med 2007; 4: e217 [ Links ]
19. Oye JE, Kuper H. Prevalence and causes of blindness and visual impairment in Limbe urban area, South West Province, Cameroon. Br J Ophthalmol. 2007; 91(11): 1435-1439. [ Links ]
20. Mathenge W, Kuper H, Limburg H, et al. Rapid assessment of avoidable blindness in Nakuru district, Kenya. Ophthalmology 2007; 114: 599-605. [ Links ]
21. Berhane Y, Worku A, Bejiga A, et al. Prevalence and causes of blindness and low vision in Ethiopia. Ethiopian J Health Development 2007; 21: 204-210. [ Links ]
22. Oye JE, Kuper H, Dineen B, Befidi-Mengue R, Foster A. Prevalence and causes of blindness and visual impairment in Muyuka: a rural health district in South West Province, Cameroon. Br J Ophthalmol 2006; 90(5): 538-542. [ Links ]
23. Bobak M, Marmot M. East-West mortality divide and its potential explanations: proposed research agenda. BMJ 1996; 312: 421-425. [ Links ]
Accepted 9 July 2010.
Declaration of interest: There is no conflicting or competing interest among all the authors.
Corresponding author: M V S Gudlavalleti (Gvs.Murthy@lshtm.ac.uk)
* The Nigeria National Blindness and Visual Impairment Study Group: Abdullahi U Imam, Adenike Abiose, Abdull M Mahdi, Bankole Olufunmilayo, Christian Ezelum, Elizabeth Elhassan, Gabriel Entekume, Hannah Faal and Pak Sang Lee, in addition to the other authors listed in the paper.














