Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.100 n.12 Pretoria Dec. 2010
IZINDABA
NHI fund to be vetted along SARS lines

A sophisticated 'risk management engine' will be set up to reduce fraud and corruption when the massive R128 billion National Health Insurance (NHI) fund rolls into gear in 2012.
This assurance was given to several worried delegates to the South African Medical Association (SAMA) conference addressing the impending system by Dr Olive Shisana, chairperson of the NHI Ministerial Advisory Task Team. Some delegates pointed to endemic corruption and financial mismanagement in several provincial health departments, some of it involving Health MECs or their Directors General and asked what the plan was to prevent the NHI fund (rising to R375.5 billion in 2025) from being similarly affected. Others alluded to Cosatu president Zwelinzima Vavi's reference to 'the predator state' in describing the current status quo, in spite of President Jacob Zuma's belated attempt to crack down on all forms of fraud and corruption.
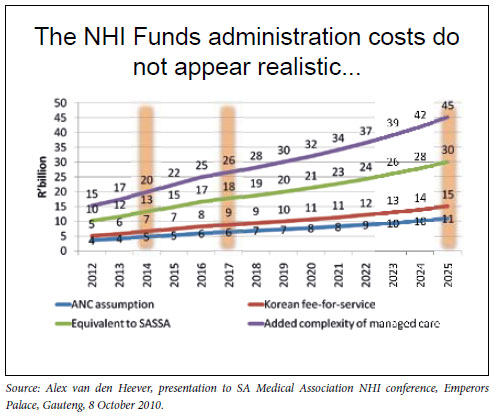
Economist Alex van den Heever cited the red flag waved by the International Labour Organisation (ILO), over the governance of social security agencies in which managers were either under-qualified or political appointees, or both. He also said the ANC projections for the administration costs of the fund (R4 billion in 2012 rising to R11 billion in 2025) did not appear realistic when compared with peer country costs or when the added complexity of managed care (R10 billion in 2012 to R45 billion in 2025) was included.

'Cheetah-like' NHI will pounce on cheaters
Shisana acknowledged that 'many of you are concerned that too many hands will be getting into this huge kitty', but said work had already begun on a risk management engine to prevent fraud and leakage. The NHI fund would report directly to the minister of health and be constructed along the lines of the South African Revenue Service (SARS), 'acting like a cheetah and not an elephant, with all the bureaucracy'. 'We must be able to act swiftly and pay quickly as a single-payer. We'll have a specialist committee to provide advisory support,' she said. She rebuffed the implication that fraud was predominantly located in the public sector, pointing to endemic fraud in the private medical aid system. However, she said a SWAT analysis was being conducted to identify just where the risks could be in the administration of an NHI fund. 'I think the transactional risk will probably be the greatest, wherever funds are moved around, so it's important to have a set of data bases set up immediately to enable someone to, in real time, monitor each transaction and see that it's legitimate.' One of the first steps would be to 'bump up' the Home Affairs data base. After this, monitors could check whether a person being claimed for was registered at the correct health facility and whether the right protocol was being followed. The data inspectors would also need an understanding of any medication the claimant was supposed to be getting and the services they were supposed to be receiving.
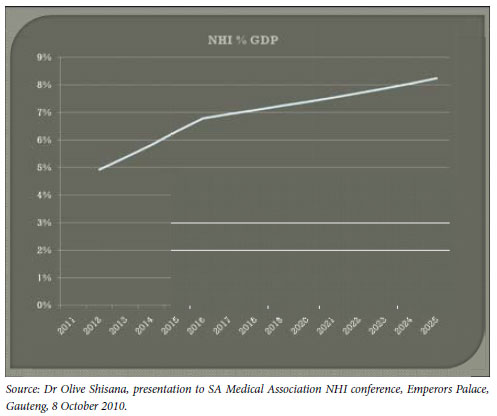
'All of this will have to be lumped together in the risk management engine so we can find anomalies in the data. We can then see, this and this is happening and ask why. In that way you don't wait for problems to occur but solve them immediately. You catch them as they occur. South Africa has a lot of expertise in this area,' she added, a probable reference to existing systems in the SARS and the private Board of Healthcare Funders (BHF).
Chris Bateman














