Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.100 n.12 Pretoria Dec. 2010
CORRESPONDENCE
GP remuneration compared with non-health care costs
To the Editor: While working for the National Pathology Group (NPG) to help them understand the pathology cost trends in medical schemes from publicly available data, we came across two interesting relationships between costs in the private industry.
Medical schemes have lamented the inflation increase in pathology costs over the past 5 years. This gave rise to a Discovery Health advertisement in a medical publication, 'Working together we can ensure a strong, sustainable health care system', where the increase in pathology costs was raised as a problem and doctors were requested to assist Discovery Medical Scheme manage these costs. In reviewing pathology trends against other trends within Discovery, using data obtained from the Council for Medical Schemes, we established the following.
Fig. 1 clearly shows that Discovery Medical Scheme experienced greater pressure in average beneficiary per annum (pabpa) trends for medical specialists (this measure excludes all radiology, pathology and anesthesiology) and general practitioners in the 5-year period than the scheme experienced in pathology costs. This graph supports the Lifechoice view that it is the increase in members accessing specialist care that drives pathology, radiology, hospital and other benefit expenditure areas.
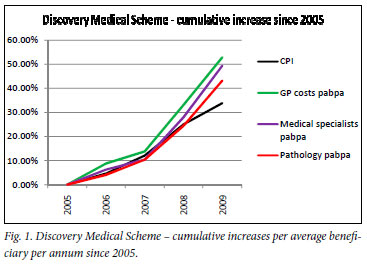
Comparing Discovery Medical Scheme's non-health care costs (NHCs) against the other South African medical schemes reveals the other interesting cost relationship.
Fig. 2. shows that the NHCs of Discovery Medical Scheme, the biggest scheme in South Africa, are significantly higher than the rest of the industry excluding Discovery. The difference shown is more than the amount Discovery Medical Scheme pays the general practitioners who look after its members and what it spends on pathology. This cost comparison cannot be ignored.
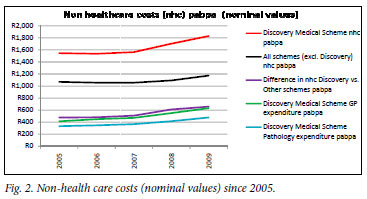
This difference may also be seen in some other open medical schemes, and some argue that open medical scheme and closed medical scheme NHCs are not comparable (we are not convinced that consumers would see this argument as relevant).
Lifechoice, together with one of South Africa's most respected independent health actuaries, have researched the cost drivers in South African health going back to 1980. The costs of belonging to medical schemes have increased over 400% in real terms since 1980. The five most significant cost drivers seen over this period are:
1. A lack of focus by medical schemes on primary health care.
2. A focus on specialist curative care and the costs associated with this.
3. The hospital admission and other costs that result from the focus on specialist care.
4. NHCs.
5. Missing medical scheme legislation - the current legislation is only sustainable if all working South Africans are compelled to belong to a medical scheme (so-called mandatory cover), prescribed minimum benefits include primary health care benefits, and clarity is provided regarding exactly what is covered by prescribed.
We must indeed start working together to ensure sustainable health care. It is critical that as we do this, we focus on all of the above areas. Until we move towards models that support primary health care and fund primary health care properly, we will continue to see costs escalate.
Andrew Good
MD, Lifechoice
agood@lifechoice.co.za














