Services on Demand
Article
Indicators
Related links
-
 Cited by Google
Cited by Google -
 Similars in Google
Similars in Google
Share
SAMJ: South African Medical Journal
On-line version ISSN 2078-5135
Print version ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.100 n.11 Pretoria Nov. 2010
ORIGINAL ARTICLES
Heliotherapy: a South African perspective
Y MoosaI; D J EsterhuyseII
IDepartment of Dermatology, Steve Biko Academic Hospital and University of Pretoria
IIMB BCh, FC Derm (SA), DTM&H. South African Weather Service, Pretoria
ABSTRACT
The research objective was to gather and collate data that will enable dermatologists to quantify exposure to solar radiation so that they can give accurate advice to patients using heliotherapy, thereby minimising harm from sun exposure. Other patients can also be advised regarding ultraviolet index (UVI) and sun safety. The concept of minimal erythema dose per hour (MED/h) may be useful in future research into solar radiation and its effects on skin cancer.
In South Africa, dermatologists are often faced with a patient who requires phototherapy but, for financial or practical reasons (distance to a specialist centre, disruption of schooling, etc.), is unable to attend phototherapy clinics. Heliotherapy (the medicinal use of natural sunlight) has been practised for centuries. The main indication for heliotherapy is psoriasis, but it has also been used for treating atopic dermatitis and vitiligo; theoretically, it could be adapted to treat the pruritus from renal failure and HIV.1-3
Current approaches
Several approaches to using sunlight to treat skin eruptions have been described. In the Dead Sea basin, physicians have advocated 10 -20 minutes' sun exposure twice daily, followed by daily increments of 10 minutes until a maximum of 3 -6 hours per day is reached. The recommended period of treatment ranges from 3 to 4 weeks.4 This method is largely generic, with daily adjustments based on individual responses to ultraviolet radiation (UVR) and the season.5,6 Its disadvantage is that variations in solar ultraviolet type B (UVB) due to changes in the thickness of the ozone layer, daily variations in cloud cover, rain, aerosol content of the air, precipitable water and season are not accounted for.7,8 Exposure to ultraviolet type A (UVA) is also not considered for the same reasons.
An alternative approach is to determine the minimal erythema dose (MED) of the patient in the phototherapy unit. Heliotherapy is then started at 70% of the MED, with increases of 10 -15% of MED for skin types I to III and 15 -20% of MED for skin types IV and V with each treatment. Patients undergo 3 -5 treatments per week; the duration of treatment is at the doctor's discretion.8,9
Avraham Kushelevsky et al.10 devised the concept of MED per hour (MED/h) to overcome these issues when using heliotherapy in the Dead Sea basin. The concept differs from MED (energy per unit area); the latter varies according to skin type, and is the minimum single dose of UVR required to produce erythema after 24 hours at an exposed site.11 In contrast, MED/h is defined as the dose causing minimal redness of the average Fitzpatrick skin type 2 after 1 hour of irradiation.
In South Africa, although dermatologists advise suitable patients to expose themselves to sunlight, there is no scientific consensus regarding time and duration of exposure, which can be misleading and vague for patients. We aimed not to replace the controlled environment of the phototherapy unit but to provide less-privileged patients with more specific, evidence-based advice on the therapeutic use of sunlight, using the concept of MED/h.
Research setting
UVB data were collected at different times of the day throughout the year from meteorological stations in three major South African cities: east coast of South Africa in Durban, latitude 29.9 S, longitude 31.0 E, sea level; west coast of South Africa in Cape Town (latitude 34.0 S, longitude 18.6 E, sea level); and inland at the headquarters of the South African Weather Service (SAWS) in Pretoria (latitude 25.8 S, longitude 28.3 E, altitude 1 541 m).
The instrumentation to measure UVB radiation at all three sites was identical, consisting of a Model 501A UV-Biometer (Solar Light Co., Glenside, PA, USA). All UVR meters are positioned to monitor UVR intensity on a horizontal surface. The Biometer measures the biological effectiveness of UVB radiation in units of MED/h. Data were collected from readings taken over 11 years in Cape Town and Pretoria, and 6 years in Durban. The average hourly UVB values for times from 07h00 -18h00 were calculated for each week of the year.
Results and applications
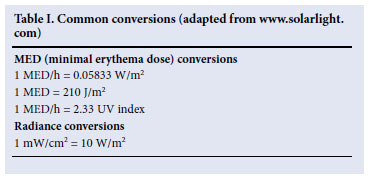
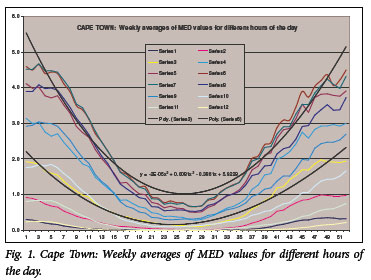
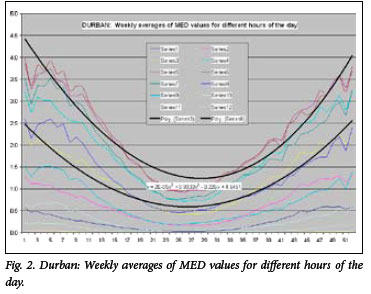
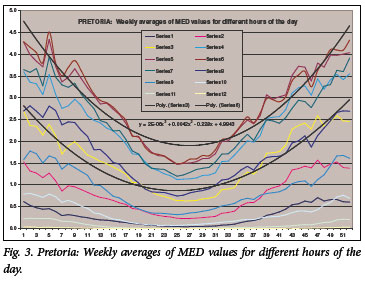
The average MED/h between 07h00 and 18h00 throughout the 52 weeks of the year for the three cities is shown in Tables I -III and Figs 1 -3. In the figures, series 1 is the average of the values between 07h00 and 08h00, series 2 represents the values between 08h00 and 09h00, etc. All values in Tables I -III are expressed in MED/h. This information can be used to give precise instructions to the patient regarding therapeutic exposure to sunlight, depending on skin type. For skin type I, a starting dose of 0.02 J/cm2 is recommended, while for skin types II -III, skin type IV and for skin type VI the starting doses are 0.03 J/cm2, 0.05 J/cm2 and 0.06 J/cm2, respectively. The following equation is then used to calculate the exact exposure time required at different times of the day and year using the data from Tables I - III, bearing in mind that 1 MED/h is the equivalent of an irradiance of 0.05833 W/m2, or 0.00583 mW/cm2 (Table I):

Irradiation time (seconds) = starting dose (J/cm2) × 1 000/ irradiance (mW/cm2)12
For example, consider a patient with psoriasis and Fitzpatrick skin type III skin seen in the 3rd week of January in Pretoria, for whom daily exposure at 10h00 is convenient. The starting dose for this skin type is 0.03 J/cm2. The MED/h for 10h00 - 11h00 on the 3rd week of January is 3.32 (UVB data Table III), which is equivalent to 0.019 mW/cm2. Therefore, the exposure time at 10h00 is calculated as follows:
Irradiation time (seconds) = 0.03 × 1 000/0.019 = 1 578 seconds = 26.3 minutes.
This patient can be advised to expose himself for 26.3 minutes a day at 10h00 in week 3 of January. The exposure times for subsequent weeks can be calculated in a similar manner, and the patient be given a written regimen. The doctor prescribing the heliotherapy can therefore quantify and adjust exposure to sunlight.
The UV data presented are also valuable in calculating the UV index (UVI), a concept with which the general public is familiar in preventing overexposure to solar radiation during outdoor activities. One MED/h equates to a UVI of 2.33, so in the example given above, the psoriatic patient will be exposed to a UVI of 3.32 × 2.33 = 7.7.
Discussion
The logistical limitation of carrying out phototherapy in South Africa, where much of the population live in isolated rural areas and lack the means for regular travel, led to this study. We aimed to assist dermatologists in employing a more scientific approach in the use of sunlight - a free, widely available, natural therapeutic resource. Heliotherapy (or climatotherapy) has been used extensively to treat thousands of patients in the Dead Sea basin, Switzerland and Sweden for many decades.12-14 Adapting this experience for use in South Africa, where many patients have little therapeutic alternative, is entirely possible and can be done in a controlled and quantifiable manner, taking into account seasonal and even hourly variations in UVR.
As with conventional phototherapy, heliotherapy requires precautions. A thorough history and physical examination should precede any consideration for heliotherapy, and should only be considered if the patient is unable to attend specialist phototherapy centres. Any potentially photosensitising drugs should be noted, as should a history of skin cancer, previous exposure to ionising radiation and skin type. A test for serum antinuclear antibodies may be indicated if there is a suggestion of an underlying photosensitive connective tissue disorder. The patient should be advised that the development of erythema is an integral part of the treatment. Strict compliance with treatment protocol should be emphasised, and solar exposure should be limited to the early morning and late afternoon hours.5 Avoidance of unnecessary sun exposure should be stressed, and patients should be advised to report any adverse events immediately, wear sunglasses, apply sunscreen to face and hands, and cover the genitalia during exposure to natural sunlight.10,13
Absolute contraindications to heliotherapy include xeroderma pigmentosum and other disorders predisposing to sun-induced cancers. Caution is appropriate if there is a past history of non-melanoma skin cancer, immunosuppression, pemphigus, pemphigoid, cataracts, aphakia or photo-sensitivity.2,10 A family history of melanoma is also reason for caution.
Acute side-effects of heliotherapy include sunburn, pruritus and a polymorphous light eruption-like response, which is usually transient and affects mainly patients with skin types II and III.14
Little is known about the chronic side-effects of long-term sun exposure and in particular the cumulative dose of solar UVR predisposing to the development of cutaneous malignancies.15 An important aspect of this work is that exposure to sunlight can be quantified, paving the way for further research into this area. Another useful application of this work is the ability to calculate UVI, which is of value to dermatologists in advising their patients about 'safe sun-exposure'. The World Health Organization classifies UVI values >9 as extreme risk, 9 -7 as high risk, 7 -4 as moderate risk, <4 as low risk, and <2 as negligible.16
UVB values across the three cities in South Africa are quite similar, possibly making it acceptable to combine and extrapolate these data for other cities in South Africa. Alternatively, region-specific values can be used, with the Cape provinces using values for Cape Town, Gauteng, Free State, North-West province and Limpopo the values for Pretoria, and KwaZulu-Natal the values for Durban. We thank Dr H Carman (consultant dermatologist in private practice in Johannesburg) for initially reviewing the paper; Professor G Todd (University of Cape Town) for reviewing the article; and Dr V Akhras (St George's University Hospital, London) for reviewing and editing the article.
References
1. Gilchrest BA, Rowe JW, Brown RS, et al. Relief of uremic pruritus by UV therapy. N Engl J Med 1997;297: 36-138. [ Links ]
2. Mentor A, Korman NJ, Elmets CA, et al. Guidelines of care for phototherapy and photochemotherapy. J Am Acad Dermatol 2010;62(1):114-135. [ Links ]
3. Abel JD, Kattan-Byron J. Psoriasis treatment at the Dead Sea: A natural selective ultraviolet phototherapy. J Am Acad Dermatol 1985;12:639-643. [ Links ]
4. Abel JD, Kipnis V. Bioclimatology and balneology in dermatology: A Dead Sea perspective. Clin Dermatol 1998;16:695-698. [ Links ]
5. Even-Paz Z, Gumon R, Kipnis V, et al. How much Dead Sea sun for psoriasis? J Dermatolog Treat 1996;7:17-19. [ Links ]
6. Diffey BL, Larko O, Swanbeck G. UV-B doses received during different outdoor activities and UV-B treatment of psoriasis. Br J Dermatol 1982;106:33-41. [ Links ]
7. Kudish AI, Abels D, Harari M. Ultraviolet radiation properties as applied to photoclimatherapy at the Dead Sea. Int J Dermatol 2003;42:359-365. [ Links ]
8. Walters IB, Burack LH, Coven TR, Gilleaudeau P, Krueger JG. Suberythemogenic narrow-band UVB is markedly more effective than conventional UVB in treatment of psoriasis vulgaris. J Am Acad Dermatol 1999;6:893-900. [ Links ]
9. Zanoli M. Phototherapy arsenal in the treatment of psoriasis. Dermatol Clin 2004;22:397-406. [ Links ]
10. Kushelevsky AP, Harari M, Kudish AI, Hristakieva E, Ingber A, Shani J. Safety of solar phototherapy at the Dead Sea. J Am Acad Dermatol 1998;3:447-452. [ Links ]
11. Freedberg IM, Eisen AZ, Wolff K, et al., eds. Fitzpatrick's Dermatology in General Medicine, 6th ed. New York: McGraw-Hill, 2003: 1275-1282. [ Links ]
12. Kudish AI, Evseev E, Kushelevsky P. The analysis of ultraviolet radiation in the Dead Sea basin. Int J Climatol 1997;17:1697-1704. [ Links ]
13. Larko O, Swanbeck G. Is UVB treatment of psoriasis safe? A study of UVB treated psoriatics compared with a matched control group. Arch Derm Venereol 1982;62:507-512. [ Links ]
14. Larko O. Phototherapy of psoriasis: clinical aspects and risk evaluation. Acta Derm Venereol 1982;103:1-42. [ Links ]
15. Abel JD, Even-Paz Z, Efron D. Bioclimatology at the Dead Sea. Clin Dermatol 1996;14:653-658. [ Links ]
16. Kudish AI, Lyubansky V, Evseev EG, Ianetz A. Inter-comparison of the solar UVB, UVA, and global radiation clearness and UV indices for Beer Sheva and Neve Zohar. Energy 2005;30:1623-1641. [ Links ]
Accepted 29 March 2010.
Corresponding author: Y Moosa (ymoosa75@gmail.com)














