Serviços Personalizados
Artigo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares em Google
Similares em Google
Compartilhar
SAMJ: South African Medical Journal
versão On-line ISSN 2078-5135
versão impressa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.100 no.7 Pretoria Jul. 2010
SCIENTIFIC LETTERS
Emergency centres lack defibrillator knowledge
Pauline LouwI; David MaritzII; Lee WallisIII
IMB ChB, MMed (EM). Division of Emergency Medicine, University of Cape Town and Stellenbosch University, Tygerberg, W Cape
IIMB ChB. Division of Emergency Medicine, University of Cape Town and Stellenbosch University, Tygerberg, W Cape
IIIMB ChB, MD, Dip Sport Med, FRCS Edin (A&E), FCEM, FCEM (SA). Division of Emergency Medicine, University of Cape Town and Stellenbosch University, Tygerberg, W Cape
To the Editor: In the emergency centre (EC), a number of essential items of equipment are needed to manage a wide variety of acute life-threatening emergencies. Their correct use depends heavily on the training and experience of personnel.
The defibrillator is part of this essential equipment and should be available in all ECs. Although defibrillators are widely available in Western Cape ECs, it is not known whether public sector EC personnel have the knowledge and skills necessary to use them safely and effectively.
Most cardiac arrests in adult patients are due to ventricular fibrillation (VF) or cardiac-related causes, and early defibrillation improves survival of such patients1,2 and is therefore an important part of their immediate treatment (combined with the other links of the chain of survival for both in- and out-of-hospital cardiac arrest).1
Aims
We aimed to assess the availability of defibrillators, and the current level of the correct and effective use of defibrillators among health care personnel in Western Cape public sector ECs, by means of a questionnaire (reproduced in an appendix to the web version of this article).
Methods
This was a prospective, cross-sectional study including all public hospitals with an EC in the Western Cape. Private hospitals and primary health care facilities (including community day centres and community health centres) and hospitals that refused to participate or failed to provide fully completed questionnaires were excluded.
Ethical approval was obtained from the University of Cape Town Research Ethics Committee.
Following agreement to participate, all full-time personnel in the hospital's EC were approached with a questionnaire comprising various questions including job description of personnel member completing the questionnaire, questions specific to defibrillators and pacing in the EC, and questions on defibrillators and pacing in general.
Data were collected on a Microsoft Excel database (Redmond, Va, 2007), on a password-protected work computer. Data analysis was performed using SAS Version 9.1.3.
Results
In the public health sector of the Western Cape, 3 central, 4 regional and 33 district hospitals (7 in the city, 26 rural) provide ECs. All 40 public sector hospitals with an EC in the Western Cape were approached; 2 refused to participate and 11 did not return the questionnaire forms in time, so 27 hospitals (67.5%) were analysed.
Of the 378 forms retrieved, 12 (3.2%) were excluded owing to lack of signed consent and 366 were analysed. The response rate varied by institution from 11.5% to 100%; 68% of forms were completed by nursing personnel.
Of the hospitals that participated in the study, 22 (81.5%) were district level, 3 (11.1%) regional and 2 (7.4%) central hospitals. All 27 hospitals had a defibrillator present in the EC, the number varying from 1 (16 hospitals, 59.3%) to more than 3 (1 hospital, 3.7%). Defibrillator specification varied between facilities: 67% had biphasic, 15% monophasic and 18% both mono- and biphasic defibrillators in the EC. Thirty-seven per cent of hospitals had pacing capabilities in the EC - all the hospitals without pacing were district level.
Defibrillator tests occur in 67% of ECs, but frequency of testing varied widely. Although 52% of defibrillators were tested daily, only 26% of these tests were documented in a dedicated log.
Of the participants, 58% had no previous training in using a defibrillator. Only 13% of nurses and 30% of sisters had received training, compared with 88% of doctors. Of the participants 96% knew that a defibrillator was present in their EC; however, only 42% knew which type of defibrillator it was, and only 58% were correctly aware that their EC had pacing capabilities. An alarming 58% of personnel had not used a defibrillator before, although 88% had witnessed its use. Only 17% of personnel had paced a patient before.
Areas of knowledge tested were correct use of Joule settings, indications for defibrillation, and indications for synchronised cardioversion. Only 14% of EC personnel were aware of the correct Joule setting for their defibrillator, only 18% knew all the indications for defibrillation, and only 6% were aware of the correct indications for synchronised cardioversion. Fig. 1 shows the differences in defibrillator knowledge according to level of seniority of personnel.
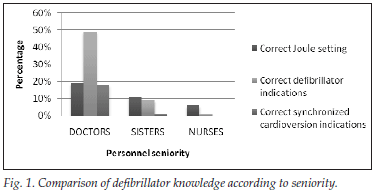
Doctors had the best knowledge with regard to the indications for both defibrillation (49%) and synchronised cardioversion (18%).
Discussion
Early defibrillation improves the outcome of patients presenting in cardiac arrest - for every minute's delay in defibrillation, survival decreases by 7 - 15%.1,3 The defibrillator plays a central role in patients presenting with shockable arrest rhythms (VF and pulseless VT); however, to have the maximum impact on patient outcomes, defibrillation must be done quickly and correctly.1 Selecting the correct Joule setting is an essential component of this process. Worryingly, in this study only 14% of personnel knew the correct Joule setting for their EC's defibrillator. This may lead to unnecessary delays or incorrect dosages and adversely affect survival.
All EC resuscitation equipment should be regularly checked to ensure its good working condition; this is especially applicable to defibrillators.4 The Emergency Medical Society of South Africa (EMSSA) recommends daily defibrillator testing as a national standard.5 The outcome of the testing should also be documented to ensure that it is working when it is required. In the absence of documentation of testing, the facility would be defenceless in a medicolegal case.
Anecdotally, in Western Cape ECs the main responsibility for the use of defibrillators lies with doctors. Comments on the questionnaires indicated that most nurses perceived that the use of defibrillators falls outside their scope of practice, although no formal documentation was found to validate this.
Defibrillators are most likely to be used in an EC or intensive care setting, or by cardiac arrest teams. In the vast majority of Western Cape hospitals, this means that EC personnel will most often make use of defibrillators, suggesting that their use of and knowledge of defibrillators should be better than their colleagues in a non-emergency environment.6 Only 18% knew the correct indications for defibrillation: even allowing for the argument that defibrillation is outside of a nurse's scope of practice, all doctors working in an EC should know these indications, but only 49% did so. This is despite 88% having received training, and indicates a serious problem with skill retention. Although training is important,7,8 retention of knowledge is more important: regular updates should occur to improve retention of knowledge and skills.9,10
There are two other standard emergency indications for defibrillator use: pacing and synchronised cardioversion. Both form part of the Western Cape Packages of Care11 at all levels, and the skills and knowledge should therefore be present.
Limitations
As this was a self-reported survey, the results may not exactly represent current practices. However, it is probable that it reflects the best-case scenario, as respondents tend to overstate their answers in anonymous questionnaires. If this is the case, the results may be even more concerning, adding to the urgency for intervention.
Conclusion
Defibrillators are life-saving and their early use improves survival of patients presenting with sudden cardiac arrest due to shockable rhythms if they are used safely and correctly. However, adequate knowledge and skills are of paramount importance to prevent unnecessary delays that may impact on patient outcome. Most EC personnel in the Western Cape do not have adequate levels of defibrillator knowledge.
Nurse-initiated defibrillation can be life-saving, and nursing personnel must be encouraged to add defibrillation to their scope of practice as an expected rather than an extended skill. This will need a change in mind-set on the part of many nurses in the provincial setting.
To ensure maximum patient benefit from defibrillator use, hospitals should aim to standardise equipment (this needs to be driven from Government level), ensure daily testing that is logged in a dedicated log, and mandate regular updates and training in defibrillator skills for staff.
References
1. Bossaert L, Callanan V, Cummins RO. Early defibrillation: An advisory statement by the Advanced Life Support Working Group of the International Liaison Committee on Resuscitation. Resuscitation 1997; 34: 113-114. [ Links ]
2. Peberby MA, Kaye W, Ornato JP. Cardiopulmonary resuscitation of adults in the hospital: a report of 14720 cardiac arrests from the National Registry of Cardiopulmonary Resuscitation. Resuscitation 2003; 58: 297-308. [ Links ]
3. Chan PS, Krumholz HM, Nichol G, et al. Delayed time to defibrillation after in-hospital cardiac arrest. N Engl J Med 2008; 358: 9-17. [ Links ]
4. Cummins RO, Chesemore K, White RD. Defibrillator failures. Causes of problems and recommendations for improvement. Defibrillator Working Group. JAMA 1990; 264(8): 1019-1025. [ Links ]
5. Emergency Medical Society of South Africa (EMSSA). Emergency Centre Defibrillation. Practice guideline EM008. January 2009. http://www.emssa.org.za (accessed 15 January 2010). [ Links ]
6. Hou S, Chern C, How C, Wang L, Huang C, Lee C. Is ward experience in resuscitation effort related to the prognosis of unexpected cardiac arrest? J Chin Med Assoc 2007; 70(9): 385-390. [ Links ]
7. Joint statement from the Royal College of Anaesthetists, Royal College of Physicians of London, Intensive Care Society and Resuscitation Council (UK). Cardiopulmonary Resuscitation: Standards for clinical practice and training. October 2004. www.resus.org.uk (accessed 23 January 2010). [ Links ]
8. Stross JK. Maintaining competency in advanced cardiac life support skills. JAMA 1983; 249:3339-3341. [ Links ]
9. Hamilton R. Nurses' knowledge and skill retention following cardiopulmonary resuscitation training: a review of literature. J Adv Nurs 2005; 51(3): 288-297. [ Links ]
10. Semeraro F, Signore L, Cerchiari EL. Retention of CPR performance in anaesthetists. Resuscitation 2006; 68(1): 101-108. [ Links ]
11. Western Cape Department of Health Hospital Package of Care. Cape Town: Provincial Government of the Western Cape, February 2009. [ Links ]
Accepted 23 March 2010.
Conflicts of interest: None.
Corresponding author: P Louw (paulinelouw@yahoo.com)














