Servicios Personalizados
Articulo
Indicadores
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en Google
Similares en Google
Compartir
SAMJ: South African Medical Journal
versión On-line ISSN 2078-5135
versión impresa ISSN 0256-9574
SAMJ, S. Afr. med. j. vol.100 no.7 Pretoria jul. 2010
FORUM
CLINICAL IMAGES
Reversible nephrotic syndrome secondary to pulmonary hydatid disease
Tahar Gargah; Rim Goucha-Louzir; Youssef Gharbi; Rachid Mohamed Lakhoua
Most patients with pulmonary hydatidosis are children. The disease may be asymptomatic or revealed by unusual events such as a glomerulopathy.1
Case report
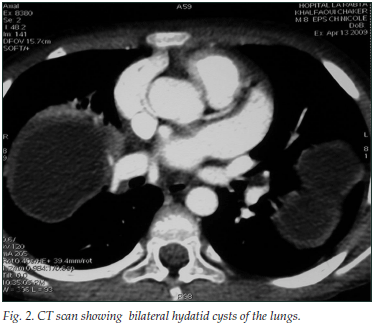
An 8-year-old boy from a rural part of Tunisia presented with generalised oedema and macroscopic haematuria. There was no familial history of renal disease. He had a normal blood pressure (100/60 mmHg), and a pleural effusion was detected. Urinalysis showed nephrotic range proteinuria (375 mg/kg/d) and microscopic haematuria. His serum total protein concentration was 40 g/l and his serum albumin was 10 g/l. Renal biopsy showed capillary wall thickening and duplication, and mesangial cell proliferation in the glomeruli, characteristic of mesangiocapillary glomerulonephritis. Renal and abdominal ultrasound images showed increased echogenicity of the kidneys and mild ascites. Radiology revealed three large pulmonary hydatid cysts (Figs 1 and 2). The largest cyst occupied the entire right upper lobe and compressed the superior vena cava. Hydatid disease was confirmed by a strongly positive serum enzyme-linked immunosorbent assay (ELISA) for echinococcus.

The patient was treated with high protein intake, dipyramidol and captopril; both right lung cysts were resected, followed by the left pulmonary cyst 4 weeks later. Hydatid cyst was confirmed histopathologically. He recovered well, the serum ELISA for echinococcus became negative, and follow-up urine examination and thoracic computerised tomography were normal 6 months after surgery, confirming good renal recovery and absence of pulmonary hydatid disease.
Discussion
Renal involvement during hydatid disease is well recognised.1 The most common manifestation is proteinuria, with or without nephrotic syndrome. Several histopathological types have been demonstrated.1-3 The pathogenesis of glomerular disease in patients with hydatid disease is not well understood, with most supporting an immune complex-mediated mechanism. Echinococcal antigen and corresponding antibody in the glomeruli have been demonstrated by immunoperoxidase studies.4 The site of the hydatid cyst appears to be crucial in the development of glomerular damage, since all reported cases are of either hepatic or pulmonary location. However, this deduction may be unfounded as hydatids occur most frequently in these locations.
Renal involvement during hydatid disease is not confined to the glomeruli. A case of predominantly chronic tubulo-interstitial nephritis with mesangioproliferative glomerulonephritis in a patient with hepatic hydatid cyst which responded to cyst resection was reported.5 In our patient, the lesions were confined to the glomeruli which have the typical features of a mesangiocapillary glomerulonephritis. Most cases of glomerular lesions associated with hydatid disease, including ours, are reversible by medical or surgical treatment of the hydatid;3 this demonstrates the causal relationship between hydatid disease and glomerulopathy. Our observation is believed to be the first in a child in the first decade, with renal histological confirmation.
1. Velthuysen V, Florquin S. Glomerulopathy associated with parasitic infections. Clin Microbiol Rev 2000; 13: 55-66. [ Links ]
2. Gelman R, Brook G, Green J, Ben-Itzhak O, Nakhoul F. Minimal change glomerulonephritis associated with hydatid disease. Clin Nephrol 2000; 53: 152-155. [ Links ]
3. Covic A, Mititiuc I, Caruntu L, Goldsmith DJA. Reversible nephrotic syndrome due to mesangiocapillary glomerulonephritis secondary to hepatic hydatid disease. Nephrol Dial Transplant 1996; 11: 2074-2076. [ Links ]
4. Edelweiss MI, Daudt HM, Goldstein HF, Garcia C. Hepatic hydatosis with glomerular involvement: report of a case. Rev Assoc Med Bras 1992; 38: 31-32. [ Links ]
5. Aziz F, Panday T, Patel H, et al. Nephrotic presentation in hydatid cyst disease with predominant tubulointerstital disease. Int J Nephrol Renovasc Dis 2000; 2: 23-26. [ Links ]
Tahar Gargah, Rim Goucha-Louzir and Rachid Mohamed Lakhoua are based at the Charles Nicolle Hospital in Tunis, Tunisia, and Youssef Gharbi in the Department of Paediatric Surgery at the Habib Thameur Hospital in Tunis.
Corresponding author: Tahar Gargah (kitomora@yahoo.fr)














